Abstract
Objective
To quantify the incidence and degree of endotracheal tube intraluminal obstruction after mechanical ventilation and its relation to time of intubation.
Design
Prospective observational study.
Setting
A 14-bed medical-surgical intensive care unit at a university-affiliated teaching hospital.
Patients
Ninety-four endotracheal tubes used in 80 patients requiring mechanical ventilation for more than 12 h.
Interventions and results
Acoustic reflectometry was performed in every endotracheal tube after patient extubation to measure its volume reduction. The intraluminal volumes of used endotracheal tubes in mechanically ventilated patients were significantly lower than those of unused tubes of the same size (5.52±0.92 ml3 versus 6.54±0.79 ml3, p<0.05). The mean difference in endotracheal tube segment volumes was 15.2% (range 0–66%). Volume reduction was above 10% in 60.8% of the tubes. In 22% of endotracheal tubes the remaining inner diameter was less than 7 mm. Reduction below this figure was less frequent (9.3%) in tubes 8 mm or more (p<0.05). The percentage of endotracheal tube volume reduction was not associated with the duration of intubation (r=−0.09, p= n.s.) Peak pressure measured before extubation did not predict obstruction (r=0.11, p= n.s.)
Conclusions
Inadvertent endotracheal tube obstruction was common in patients requiring mechanical ventilation and may be significant as early as at 24 h. Moderate obstruction in endotracheal tube lumens should be suspected in cases of difficulties in weaning, even in patients who were ventilated for less than 1 day.
Similar content being viewed by others
Introduction
The obstruction of endotracheal tubes (ETTs) is associated with extra work of breathing and is a well known emergency if it becomes complete. In addition, it may interfere in certain forms of mechanical ventilation [1–6]. But the question is when to suspect obstruction and how to detect it. The study by Wright [7] shows that in vitro measurements of resistances may be underestimated compared with measurements in vivo, due to the accumulation of secretions on the tube walls. Induced resistance is also substantially increased in tubes with an internal diameter of more than 7 mm [8, 9].
Acoustic reflectometry was designed to determine the airway cross-sectional area as a function of axial distance and has also been used to detect esophageal intubation in anesthesia patients [10] and to study the pharyngeal regions in patients with obstructive sleep apnea [11]. The method can be used to detect and quantify decreases in ETT volume [6, 10, 12]. Recently, Shah and Kollef [13] reported that ETT inner diameter decreased with time of use, but that the occlusion was also determined by a number of other factors such as the patient’s condition, the humidification system used and method of measurement.
The ETT inner diameter is used by respiratory modes such as automated tube compensation [14] or pressure support [15, 16] to estimate the force needed to compensate ETT resistance and, thus, to diminish respiratory workload. The inner diameter used by mechanical ventilators with these ventilatory modes is not the real diameter at the time of weaning, because occlusion occurs during intubation.
Our study objectives were: first, to quantify ETT volume loss during mechanical ventilation using acoustic reflectometry and, second, to assess whether this obstruction can be anticipated by intubation duration or peak pressure determination before extubation. Specifically, we aimed to identify what initial diameter would protect patients from complications (e.g. increased work of breathing), maintaining a final measurement more than 7 mm [4, 13]. Our hypothesis was that silent ETT obstruction may be a frequent problem and may contribute to ventilation difficulties in certain patients.
Material and methods
Demography, inclusion and exclusion criteria
The study was conducted in a 14-bed medical-surgical ICU of a university hospital, during a 5-month period (October 2002-February 2003). All adult patients requiring mechanical ventilation longer than 12 h were enrolled. The study was approved by the institutional research board. Exclusion criteria were: ETT other than Hi-Lo Mallinckrodt, age below 14, severe hemoptysis, tracheotomy, nasal intubation, enrolment in a clinical trial or use of special silver-coating devices.
Method
Patients were enrolled in the study trial without any change in routine airway management: that is, all available ventilators were used (Puritan-Benett, Servo 900 C, Evita-Dragger). ETTs were standard high-volume low-pressure cuffed endotracheal tubes (Hi-Lo Mallinckrodt Medical, Ireland). All tubes were placed orotracheally. There were no differences in the ventilator circuits between patients and the same ventilator circuit tubing was used throughout each patient’s course of mechanical ventilation, except in the case of mechanical problems.
Humidification and air care management
Heat and moisture exchangers (HMEs) (Higroster, DAR Breathing system, Mallinckrodt Medical, Italy) were routinely used. HMEs were changed daily and placed behind the medication delivery device, so they did not have to be removed during the bronchodilator administration. Suctioning was performed by the nurse in charge of the patient using a standardized open technique as often as required according to the presence of secretions in the ETT or increased ventilator airway pressures. No heated-water humidification devices were used.
Acoustic reflectometry
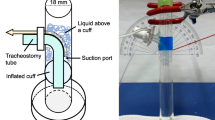
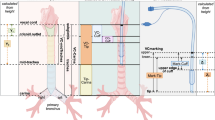
The acoustic reflectometry technique was performed within the first hour after the tube was removed from the patient. The result was the mean of the three measurements from the same tube. A plastic mold was used to cut the distal (carinal) portion of endotracheal tubes to a uniform length (17 cm) with a blade. The proximal portion was discarded and reflectometry was performed to measure the occlusion of the distal portion. The operating principle of the acoustic reflection device [17–21] is that sound pulses emitted by a horn are transmitted through a wave-tube into the airway device. Expansions and constrictions along the airway reflect incident sound waves. A microphone mounted within the wave-tube records reflected waves.
Acoustic reflectometry profiles were obtained using a customized, computer-based acoustic reflectometer (Eccovision Rhinometer, Hoods Labs, Pembroke, MA). The instrument measured the cross-sectional area to a maximum measurement distance of 13 cm from the distal end of the wave-tube (the instrument’s integration window was set between 2 and 15 cm, to avoid errors in the calculation induced by the connector and the distal portion of the Murphy eye). This technique has been used before to assess the position and patency of infant endotracheal tubes and to measure cross-sectional areas of the upper airway in certain laryngological diseases, as well as to verify proper endotracheal tube placement [22, 23].
The cross-sectional area can be converted into an effective diameter though the area may not be circular. The total volume of accretions over a specified length is calculated, as well as the minimum cross-sectional area over the study length. The minimum cross-sectional area can be converted into an effective diameter and the estimated maximum mucus thickness can be used to compare groups. The theoretical volume of unused ETT was calculated by obtaining the mean value of serial measurements on five ETTs of the same size. For each diameter (6.0 mmID, etc), the volumes of three different, unused tubes were each measured 20 times. These data show the precision of repeated measurements of the same tube [24]. The relative standard deviations ranged from 1.0 to 3.3%.
Evaluation criteria
Data were obtained from the ETT after removal from the patient. The variables recorded for all the study patients were: age, gender, indication for mechanical ventilation and peak pressures recorded from the ventilator just before removing the endotracheal tube. Each intubation episode was considered a separate case regardless of the number of intubations performed in each patient. The main criterion was to determine the ETT occlusion level after its use and the secondary end point was to analyze the association between occlusion level and intubation time.
Statistical analysis
The data are reported as means ± SD. Calculations of sample size: the minimum number of subjects to obtain a correlation of 50% or more between days of mechanical ventilation and the reduction of the intraluminal volume is 45, accepting an alpha risk of 5% and a power of 95%. Due to the need to analyze other parameters and to stratify, the sample was increased to 100. Analysis of variance (ANOVA) was performed to compare the mean values between groups. To compare the mean values of obstruction of all ETTs with mean values of equivalent sizes of unused ETTs, analysis of variance (MANOVA) with repeated measures of one factor was used. Spearman rank test was used to correlate the time of intubation and ETT volume reduction. A significance level of p of 0.05 or less was accepted. Data analysis was performed with the CIA program version 1.2 (Statistics with confidence, Martin J Gardner and Douglas G Altman, BMJ 1989) and SPSS 6.1.
Results
Ninety-four ETTs were collected from 80 consecutive patients requiring mechanical ventilation for more than 12 h. Patients with two tubes were considered as independent cases. Two of the tubes collected were rejected due to technical problems with the reflectometry procedure. Data analysis was performed in the ninety-two remaining tubes. The mean age of the patients was 53.1±20.5 years. Fifty-four were men (58.7%) and 38 (41.3%) were women. The indications for mechanical ventilation are displayed in Table 1. Causes of extubation were: 21 tracheostomies, 3 cuff ruptures, 2 self-extubation, 13 deaths and clinical improvement in the rest of the patients. Seven of the extubated patients were reintubated due to respiratory failure (all within 48 h after extubation).
Patients were intubated for a mean of 7.2±5.8 days (range 12 h–24 days). Fifteen of them (16.3%) were intubated between 12–24 h. For tubes removed from the patient airways, we found a statistically significant volume reduction when compared to the theoretical volume of the unused tubes of the same size (5.52±0.92 ml3 versus 6.54±0.79 ml3, p<0.01). The mean reduction in ETT volume was 15.2±12.4% (range 0–66%) and in 60.6% the volume loss was higher than 10%. The effective inner diameter mean reduction was 7.9±0.4 to 7.3±0.6 mm. Twenty ETTs (21.7%) eventually had an effective inner diameter of less than 7 mm. (Table 2, Fig. 1)
The inner diameter narrowing of the ETTs smaller than 8 mm was significantly less than in larger ones. Even though ETTs 8 mm or larger were associated with major occlusion, the mean effective inner diameter always remained larger than in ETTs less than 8 mm. There were no statistical differences in intubation times for any ETT size.
No significant association was documented between volume reduction and duration of tracheal intubation ( r=–0.09 p= n.s). This was true for the total number of ETTs and also when the analysis was performed according to ETT size. There were no statistical differences between the 15 tubes used for 24 h or less and those used in the 77 patients intubated for longer periods. Nor was there an association between endotracheal volume reduction and mean peak pressures measured from the ventilator before extubation (r=0.11, p= n.s.). Only in one patient was the ETT removed due to clinical suspicion of occlusion (indicated by increased peak pressure and difficulty on passing the aspiration probe), which was confirmed upon removal.
Discussion
Our study confirms the presence of ETT obstruction in mechanically ventilated patients which may represent an unsuspected difficulty in weaning. A particularly interesting finding was that this obstruction was documented within 24 h of intubation.
Prolongation of mechanical ventilation in these patients does not seem to increase the risk of major obstruction. The mean obstruction rate was 15.2%, but in two-thirds of the patients analyzed the volume loss was higher than 10%. Moreover, in one out of five patients the remaining effective inner diameter of the tube was less than 7.0 mm. In spite of this, only one patient had clinical suspicion of ETT obstruction. Similarly, we found no association between peak pressure values registered from the ventilator previous to extubation and the degree of intraluminal volume reduction. Peak airway pressure, which has been used as an index of respiratory resistance in ventilated patients, is unable to assess the contribution of the ETT resistance and is highly dependent upon flow pattern [25]. In addition, monitoring peak pressure, we cannot distinguish between the resistance caused by the ETT and the total resistance of the airway.
Loss of volume secondary to ETT narrowing has been associated with increases in breathing workload and prolongation of mechanical ventilation as well as failed weaning efforts [1, 4, 5]. The minimal ETT size that guarantees adequate work of breathing and prevents weaning failure is unknown. In the early 1980s, Shapiro et al. [8] reported that work of breathing increased when ventilating patients with high volumes through ETTs narrower than 7 mm in diameter. However, a study in newborns [15] and another study designed to determine the ideal pressure support to overcome ETT resistance [16] stressed the need to adjust this parameter according to the size of each ETT. The results of our study suggest that this parameter should be adjusted to the real ETT inner diameter due to the fact that the final ETT size was lower than 7 mm in more than 20% of intubated patients.
Studies performed to date using reflectometry [5, 26] have assessed only a small number of patients. Our trial and another carried out by Shah [13] enrolled around 100 patients. Both used reflectometry, though with certain differences: first, in the study performed by Shah [13] ETT tubes were refrigerated once removed from the patient and measurements were made within 5 days of extubation. We measured the ETT inner diameter immediately (within 1 h of extubation). Second, the humidification systems used in the two studies were different. Third, in contrast to Shah, we did not find a linear relationship between time of intubation and occlusion rate. Indeed, obstruction greater than 10% within the first 24 h of intubation was present in 9/15 patients, with no significant differences being found for longer periods of intubation. Other differences were case mix, mean ETT size and intubation period (mean 4.2 vs 7.2 days); all these variables may have contributed to the differences in the results.
Heat and moisture exchangers may play an important role in the decrease of inner tube diameter by impeding the adherence of mucus to the inner surface of the tube. The results of studies comparing different HME systems are controversial. Some authors reported higher occlusion rates with HME than with heated humidifiers [27, 28], but others reported differences in moisture level with different makes of the same type of HME [29–31]. A recent study by Jaber et al. [32] demonstrated a higher rate of ETT occlusion with HMEs than with modern heated humidifiers, but the study by Villefane [27] found no significant differences, perhaps because the ventilation times were shorter. In our study, the same HME system was used in all patients and throughout the study period. The HME system used has been validated by previous studies [31]. Recently published studies have reported that the continuous use of humidifying systems is safe as long as they are replaced every 48 h [33]; however, the safety they offer may not be adequate beyond 48 h. So one limitation of this study was the use of humidification systems unable to guarantee 100% moisture.
The reason why ETT occlusion occurs in the early phases of intubation remains unknown. It may be due to local inflammatory mechanisms [34] which are responsible for the increased secretion production within the first 24 h after intubation. When analyzing ETT occlusion in relation to intubation time, we did not find any significant differences according to diagnosis on admission (COPD, pneumonia or trauma). In any case, the number of patients is too small to be able to draw firm conclusions.
Our study has some limitations. First, tube narrowing is a dynamic rather than a static process, influenced by local inflammatory mechanisms that may vary over the period of intubation. This process can only be determined by measuring ETT inner occlusion while the patient is extubated. Several studies [5, 21, 32] determined ETT occlusion in vivo, using a complex technique with two microphones. These studies, conducted with different objectives in mind, show that reflectometry can be performed in situ with the patient, though the procedure is complex. Further studies should compare the current technique with other methods of measuring resistance (e.g. pressure drop with different flows). Second, the inner volume loss may also be influenced by techniques such as bronchoscopy and aspiration of secretions. Both procedures may remove a substantial amount of mucus adhering to the inner surface of the tube.
Trying to correlate the degree of tube occlusion with the number of times that the patient’s respiratory secretions are suctioned is a hard task, due to the difficulty in standardizing the indication for secretion aspiration and the subjective criteria used in determining the need to perform this procedure. Even though time between extubation and measurement did not exceed 60 min, it is possible, even likely, that significant changes occurred in the contents of the material occluding the tracheal tube as a result of drying, dripping etc. that would make it hard to extrapolate the in vitro data to the clinical situation. Specifically, we do not know how factors such as tube temperature, humidity or kinking might affect the generalization of our results in vivo. Third, the analysis did not take into account the use of bronchodilator therapy: the way it was delivered to the patient or the patient’s hydric balance. This study was not designed to evaluate ETT bacterial colonization, nor associations between ventilator-associated pneumonia and tube occlusion. Our findings cannot be generalized to populations with different case mixes, longer periods of ventilation or different humidification policies.
In summary, ETT narrowing due to secretion accumulation during mechanical ventilation is a frequent event. This occlusion was more than 10% in almost 60% of our patients and the residual tube inner-diameter reached critical values (≤7 mm) in 22% of them. The most important finding was that the obstruction of the ETT may appear during the first 24 h of mechanical ventilation; it may not be easy to detect and it may represent an unsuspected difficulty in respiratory weaning.
This study was presented in part at the 16th European Society Intensive Care Medicine Congress, Amsterdam, October 2003 [35].
References
Stauffer JL, Olson DE, Petty TL (1981) Complications and consequences of endotracheal intubation and tracheostomy. A prospective study of 150 critically ill adult patients Am J Med 70:65–76
Bolder PM, Healy TE, Bolder AR, Beatty PC, Kay B (1986) The extra work of breathing through different sized endotracheal tubes. Anesth Analg 14:1028–1031
Esteban A, Frutos F, Tobin MJ, Alia I, Solsona JF, Valverdu I, Fernandez R, de la Cal MA, Benito S, Tomas R (1995) A comparison of four methods of weaning patients from mechanical ventilation. Spanish Lung Failure Collaborative Group. New Engl J Med 332:345–350
Rumbak MJ, Walsh FW, Anderson WM, Rolfe MW, Solomon DA (1999) Significant tracheal obstruction causing failure to wean in patients requiring prolonged mechanical ventilation: a forgotten complication of long-term mechanical ventilation. Chest 115:1092–1095
Heyer L, Louis B, Isabey D, Lofaso F, Brochard L, Fredberg JJ, Harf A (1996) Noninvasive estimate of work of breathing due to the endotracheal intubation. Anesthesiology 85:1324–1333
Strauss C, Louis B, Isabey D, Lemaire F, Harf A, Brochard L (1999) Contribution of endotracheal tube and upper airway to breathing workload. Am J Respir Crit Care Med 157:23–3l
Wright PE, Marini JJ, Bernard GR (1989) In vitro versus in vivo comparison of endotracheal tube airflow resistance. Am Rev Respir Dis 140:10–16
Shapiro M, Wilson RK, Casar G, Bloom K, Teague RB (1986) Work of breathing through different sized endotracheal tubes. Crit Care Med 14:1028–1031
Diehl JL, El Artrous S, Touchard D, Lemaire F, Brochard L (1999) Changes in the work of breathing induced by tracheotomy in ventilator-dependent patients. Am J Respir Crit Care Med 159:383–388
Eckmann D, Glassenberg R, Gavriely N (1996) Acoustic reflectometry and endotracheal intubation. Anesth Analg 83:1084–1089
Rivlain J, Hoffstein V, Kalbfleish J, McNicholas W, Zamel N, Bryan C (1984) Upper airway morphology in patient with idiopathic obstructive sleep apnea. Am Rev Respir Dis 129:355–360
Epstein SK, Ciubotaru RL (1996) Influence of gender and endotracheal tube size on preextubation breathing pattern. Am J Respir Crit Care Med 154:1647–1652
Shah Ch, Kollef M (2004) Endotracheal tube intraluminal volume loss among mechanically ventilated patients. Crit Care Med 32:120–124
Fabry B, Haberthur C, Zappe D, Guttmann J, Kuhlen R, Stocker R (1997) Breathing pattern and additional work of breathing in spontaneously breathing patients with different ventilatory demands during inspiratory pressure support and automatic tube compensation. Intensive Care Med 23:545–552
Bock KR, Silver P, Rom M, Sagy M (2000) Reduction in tracheal lumen due to endotracheal intubation and its calculated clinical significance. Chest 118:468–472
Fiastro JF, Habib MP, Quan SF(1988) Pressure support compensation for inspiratory work due to endotracheal tubes and demand continuous positive airway pressure. Chest 93:499–505
Hoffstein V, Fredberg JJ (1991) The acoustic reflection technique for non-invasive assessment of upper airway area. Eur Resp J 4:602–611
Mansfield JP, Wodicka GR (1995) Using reflectometry to determine tube position and patency. J Sound Vibration 188:167–188
Louis B, Fodil R, Jaber S, Pigeot J, Jarreau PH, Lofaso F, Isabey D (2001) Dual assessment of airway area profile and respiratory input impedance from a single transient wave. J Appl Physiol 90:630–637
Raphael D (2000) Acoustic reflectometry profiles of endotracheal intubation. Anesthesiology 92:1293–1299
Raphael D, Benbassat M, Arnaudov D, Bohorquez A, Nasseri B (2002) Validation study of two microphone acoustic reflectometry for determination of breathing tube placement in 200 adult patients. Anesthesiology 97:1371–1377
Mansfield JP, Shanon DC, Wodicka GR (1998) Acoustic method to quantitatively assess the position and patency of infant endotracheal tubes: preliminary results in rabbits. Pediatr Pulmonol 26:354–361
Jarreau PH, Louis B, Desfrere L, Blanchard PW, Isabey D, Harf A, Moriette G (2000) Detection of positional airway obstruction in neonates by acoustic reflection. Am J Respir Crit Care Med 161:1754–1756
Mathews JN, Altman DG, Campbell MJ, Royston P (1990) Analysis of serial measurements in medical research. BMJ 300:230–236
Tobin M, Van de Graaff (1994) Monitoring of lung mechanics and work of breathing. In: Tobin M (ed) Principles and practice of mechanical ventilation. McGraw-Hill, USA, pp 967–1004
Van Surell C, Louis B, Lofaso F, Beydon L, Brochard L, Harf A, Fredberg J, Isabey D (1994) Acoustic method to estimate the longitudinal area profile on endotracheal tube. Am J Respir Crit Care Med 149:28–33
Villafane MC, Cinnella G, Lofaso F Isabey D, Harf A, Lemaire F, Brochard L (1996) Gradual reduction of endotracheal tube during mechanical ventilation via different humidification devices. Anesthesiology 6:1341–1349
Unal N, Kanhai JK, Buijk SL, Pompe JC, Holland WP, Gultuna I, Ince C, Saygin B, Bruining HA (1998) A novel method of evaluation of three heat-moisture exchangers in six different ventilator settings. Intensive Care Med 24:138–146
Thomachot L, Leone M, Razzouk K, Antonini F, Vialet R, Martin C (2002) Randomized clinical trial of extended use of a hydrophobic condenser humidifier: 1 vs. 7 days. Crit Care Med 30:232–237
Markowicz P, Ricard JD, Dreyfuss D, Mier L, Brun P, Coste F, Boussougant Y, Djedaini K (2000) Safety, efficacy and cost-effectiveness of mechanical ventilation with humidifying filters changed every 48 hours: a prospective, randomized study. Crit Care Med 28:665–671
Thomachot L, Viand X, Arnaud S, Boisson C, Martin CD (1998) Comparing two heat and moisture exchangers, one hydrophobic and one hygroscopic, on humidifying efficacy and the rate of nosocomial pneumonia. Chest 114:1383–1389
Jaber S, Pigeot J, Fodil R, Maggiore S, Harf A, Isabey D, Brochard L, Louis B (2004) Long-term effects of difference humidification systems on endotracheal tube patency. Anesthesiology 100:782–788
Boyer A, Thiery G, Lasry S, Pigne E, Salah A, de Lassence A, Dreyfuss D, Ricard JD (2003) Long-term mechanical ventilation with hygroscopic heat and moisture exchangers used for 48 hours: a prospective clinical, hygrometric and bacteriologic study. Crit Care Med 31:823–829
Mohler J, Azoulay-Depuis E, Amory-Riviere C, Mazoit JX, Bedos JP, Rieux V, Moine P (2003) Streptococcus Pneumoniae strain-dependent lung inflammatory responses in a murine model of pneumococcal pneumonia. Intensive Care Med 29:808–816
(2003) Abstracts of the 16th Annual Congress oh the European Society of Intensive Care Medicine. 5–8 October 2003, Amsterdam, Netherlands. Intensive Care Med 29 (suppl 1):S149
Acknowledgements
We thank Will Waughan for his description of reflectometry techniques and advice with the measurements, Bard Incorporated for providing the hardware and software required and Michael Maudsley for editing the manuscript. We are indebted to Montse Olona for statistical advice.
Author information
Authors and Affiliations
Corresponding author
Additional information
Presented, in part, at the 16th European Society Intensive Care Medicine Congress, Amsterdam, October 2003.
Rights and permissions
About this article
Cite this article
Boqué, M.C., Gualis, B., Sandiumenge, A. et al. Endotracheal tube intraluminal diameter narrowing after mechanical ventilation: use of acoustic reflectometry. Intensive Care Med 30, 2204–2209 (2004). https://doi.org/10.1007/s00134-004-2465-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-004-2465-4