Abstract
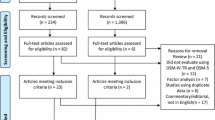
We conducted a systematic review and meta-analysis to determine the effect of changes to the Diagnostic and Statistical Manual (DSM)-5 on autism spectrum disorder (ASD) and explore policy implications. We identified 418 studies; 14 met inclusion criteria. Studies consistently reported decreases in ASD diagnosis (range 7.3–68.4 %) using DSM-5 criteria. There were statistically significant pooled decreases in ASD [31 % (20–44), p = 0.006] and DSM-IV-TR subgroups of Autistic disorder [22 % (16–29), p < 0.001] and pervasive developmental disorder-not otherwise specified (PDD-NOS) [70 % (55–82), p = 0.01]; however, Asperger’s disorder pooled decrease was not significant [70 % (26–94), p = 0.38]. DSM-5 will likely decrease the number of individuals diagnosed with ASD, particularly the PDD-NOS subgroup. Research is needed on policies regarding services for individuals lacking diagnosis but requiring assistance.





Similar content being viewed by others
References
APA. (2012a). DSM-5 Autism Spectrum Disorder Fact Sheet. http://dsmfacts.org/wp-content/uploads/2012/11/Autism-spectrum-disorder-fact-sheet.pdf.
APA. (2012b). Recent updates to proposed revisions for DSM-5. http://www.dsm5.org/Pages/RecentUpdates.aspx.
APA. (2013a). Diagnostic and statistical manual of mental disorders (5th ed.). Washington, DC: American Psychiatric Publishing.
APA. (2013b). Social (pragmatic) communication disorder. http://www.dsm5.org/Documents/Social%20Communication%20Disorder%20Fact%20Sheet.pdf.
Autism Speaks. (May 31, 2013). CT legislature passes DSM-V bill. http://www.autismspeaks.org/advocacy/advocacy-news/ct-legislature-passes-dsm-v-bill.
Barton, M. L., Robins, D. L., Jashar, D., Brennan, L., & Fein, D. (2013). Sensitivity and specificity of proposed DSM-5 criteria for autism spectrum disorder in toddlers. Journal of Autism and Developmental Disorders. doi:10.1007/s10803-013-1817-8.
Beighley, J. S., Matson, J. L., Rieske, R. D., Jang, J., Cervantes, P. E., & Goldin, R. L. (2013). Comparing challenging behavior in children diagnosed with autism spectrum disorders according to the DSM-IV-TR and the proposed DSM-5. Developmental Neurorehabilitation. doi:10.3109/17518423.2012.760119.
Centers for Disease Control and Prevention. (2012). Prevalence of autism spectrum disorders–autism and developmental disabilities monitoring network, 14 sites, United States, 2008. Morbidity and Mortality Weekly Report, 61(3), 1–19.
Dickerson Mayes, S., Black, A., & Tierney, C. D. (2013). DSM-5 under-identifies PDDNOS: diagnostic agreement between the DSM-5, DSM-IV, and checklist for autism spectrum disorder. Research in Autism Spectrum Disorders, 7, 298–306.
Falkmer, T., Anderson, K., Falkmer, M., & Horlin, C. (2013). Diagnostic procedures in autism spectrum disorders: A systematic literature review. European Child and Adolescent Psychiatry. doi:10.1007/s00787-013-0375-0.
Gibbs, V., Aldridge, F., Chandler, F., Witzlsperger, E., & Smith, K. (2012). Brief report: an exploratory study comparing diagnostic outcomes for autism spectrum disorders under DSM-IV-TR with the proposed DSM-5 revision. Journal of Autism and Developmental Disorders, 42(8), 1750–1756. doi:10.1007/s10803-012-1560-6.
Glasson, E. J., MacDermott, S., Dixon, G., Cook, H., Chauvel, P., Maley-Berg, A., et al. (2008). Management of assessments and diagnoses for children with autism spectrum disorders: The Western Australian model. Medical Journal of Australia, 188(5), 288–291.
Greaves-Lord, K., Eussen, M. L., Verhulst, F. C., Minderaa, R. B., Mandy, W., Hudziak, J. J., et al. (2013). Empirically based phenotypic profiles of children with pervasive developmental disorders: Interpretation in the light of the DSM-5. Journal of Autism and Developmental Disorders, 43(8), 1784–1797.
Hemp, R., Catherine Rizzolo, M., & Braddock, D. (2002). Selected trends in public spending for MR/DD services and the state economies. Mental Retardation, 40(5), 418–422. doi:10.1352/0047-6765(2002)040<0418:stipsf>2.0.co;2.
Hu, V. W. (2012). Subphenotype-dependent disease markers for diagnosis and personalized treatment of autism spectrum disorders. Disease Markers, 33(5), 277–288. doi:10.3233/dma-2012-0916.
Huerta, M., Bishop, S. L., Duncan, A., Hus, V., & Lord, C. (2012). Application of DSM-5 criteria for autism spectrum disorder to three samples of children with DSM-IV diagnoses of pervasive developmental disorders. American Journal of Psychiatry, 169(10), 1056–1064. doi:10.1176/appi.ajp.2012.12020276.
Johnson, C. P., & Myers, S. M. (2007). Identification and evaluation of children with autism spectrum disorders. Pediatrics, 120(5), 1183–1215. doi:10.1542/peds.2007-2361.
King, M., & Bearman, P. (2009). Diagnostic change and the increased prevalence of autism. International Journal of Epidemiology, 38(5), 1224–1234.
Lane, C. (May 4, 2013). The NIMH Withdraws Support for DSM-5. Psychology today. http://www.psychologytoday.com/blog/side-effects/201305/the-nimh-withdraws-support-dsm-5.
Lord, C., Rutter, M., DiLavore, P. C., & Risi, S. (1999). Autism diagnostic observation schedule (WPS ed.). Los Angeles: Western Psychological Services.
Lucas, N. P., Macaskill, P., Irwig, L., & Bogduk, N. (2010). The development of a quality appraisal tool for studies of diagnostic reliability (QAREL). Journal of Clinical Epidemiology, 63(8), 854–861. doi:10.1016/j.jclinepi.2009.10.002.
Mark, T. L., Buck, J. A., Dilonardo, J. D., Coffey, R. M., & Chalk, M. (2003). Medicaid expenditures on behavioral health care. Psychiatric Services (Washington, D. C.), 54(2), 188–194.
Matson, J. L., Beighley, J., & Turygin, N. (2012a). Autism diagnosis and screening: factors to consider in differential diagnosis. Research in Autism Spectrum Disorders, 6, 19–24.
Matson, J. L., Belva, B. C., Horovitz, M., Kozlowski, A. M., & Bamberg, J. W. (2012b). Comparing symptoms of autism spectrum disorders in a developmentally disabled adult population using the current DSM-IV-TR diagnostic criteria and the proposed DSM-5 diagnostic criteria. Journal of Developmental and Physical Disabilities, 24(4), 403–414.
Matson, J. L., Kozlowski, A. M., Hattier, M. A., Horovitz, M., & Sipes, M. (2012c). DSM-IV vs DSM-5 diagnostic criteria for toddlers with autism. Developmental Neurorehabilitation, 15(3), 185–190. doi:10.3109/17518423.2012.672341.
Matson, J. L., Wilkins, J., & Gonzalez, M. (2008). Early identification and diagnosis in autism spectrum disorders in young children and infants: How early is too early? Research in Autism Spectrum Disorders, 2, 75–84.
Mattila, M. L., Kielinen, M., Linna, S. L., Jussila, K., Ebeling, H., Bloigu, R., et al. (2011). Autism spectrum disorders according to DSM-IV-TR and comparison with DSM-5 draft criteria: An epidemiological study. Journal of the American Academy of Child and Adolescent Psychiatry, 50(6), 583–592. doi:10.1016/j.jaac.2011.04.001. e511.
Mazefsky, C. A., McPartland, J. C., Gastgeb, H. Z., & Minshew, N. J. (2013). Brief report: Comparability of DSM-IV and DSM-5 ASD research samples. Journal of Autism and Developmental Disorders, 43(5), 1236–1242.
McClure, I., Mackay, T., Mamdani, H., & McCaughey, R. (2010). A comparison of a specialist autism spectrum disorder assessment team with local assessment teams. Autism, 14(6), 589–603. doi:10.1177/1362361310373369.
McPartland, J. C., Reichow, B., & Volkmar, F. R. (2012). Sensitivity and specificity of proposed DSM-5 diagnostic criteria for autism spectrum disorder. Journal of the American Academy of Child and Adolescent Psychiatry, 51(4), 368–383. doi:10.1016/j.jaac.2012.01.007.
Moher, D., Liberati, A., Tetzlaff, J., & Altman, D. G. (2009). Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Annals of internal Medicine, 151(4), 264–269. W264.
Montes, G., Halterman, J. S., & Magyar, C. I. (2009). Access to and satisfaction with school and community health services for US children with ASD. Pediatrics, 124(Suppl 4), S407–S413. doi:10.1542/peds.2009-1255L.
National Conference of State Legislatures. (August 2012). Insurance coverage for autism. http://www.ncsl.org/issues-research/health/autism-and-insurance-coverage-state-laws.aspx.
Neal, D., Matson, J. L., & Hattier, M. A. (2012). A comparison of diagnostic criteria on the autism spectrum disorder observation for children (ASD-OC). Developmental Neurorehabilitation, 15(5), 329–335. doi:10.3109/17518423.2012.697492.
Newschaffer, C. J., & Curran, L. K. (2003). Autism: an emerging public health problem. Public Health Reports, 118(5), 393–399.
Peterson, K., & Barbel, P. (2013). On alert for autism spectrum disorders. Nursing, 43(4), 28–34. quiz 35.
Regier, D. A., Narrow, W. E., Clarke, D. E., Kraemer, H. C., Kuramoto, S. J., Kuhl, E. A., et al. (2013). DSM-5 field trials in the United States and Canada, Part II: Test-retest reliability of selected categorical diagnoses. American Journal of Psychiatry, 170(1), 59–70. doi:10.1176/appi.ajp.2012.12070999.
Robertson, K., Stafford, T., Benedicto, J., & Hocking, N. (2013). Autism assessment: The Melton health model. Journal of Paediatrics and Child Health. doi:10.1111/jpc.12303.
Robison, J.E. (January 17, 2013). Social Communication Disorder—is it “Autism Lite?”. Psychology Today. April 25, 2013, http://www.psychologytoday.com/blog/my-life-aspergers/201301/social-communication-disorder-is-it-autism-lite.
Rossi, J., Newschaffer, C., & Yudell, M. (2013). Autism spectrum disorders, risk communication, and the problem of inadvertent harm. Kennedy Institute of Ethics Journal, 23(2), 105–138.
Ruble, L. A., Heflinger, C. A., Renfrew, J. W., & Saunders, R. C. (2005). Access and service use by children with autism spectrum disorders in Medicaid Managed Care. Journal of Autism and Developmental Disorders, 35(1), 3–13.
Rutter, M., Le Couteur, A., & Lord, C. (2002). Autism diagnostic interview-revised (ADI-R). Los Angeles: Western Psychological Services.
State of Connecticut. (June 5, 2013). Senate Bill No. 1029, Public Act No. 13–84, “An act concerning health insurance coverage for autism spectrum disorders”. http://www.cga.ct.gov/2013/ACT/PA/2013PA-00084-R00SB-01029-PA.htm.
Taheri, A., & Perry, A. (2012). Exploring the proposed DSM-5 criteria in a clinical sample. Journal of Autism and Developmental Disorders, 42(9), 1810–1817. doi:10.1007/s10803-012-1599-4.
Wilson, C. E., Gillan, N., Spain, D., Robertson, D., Roberts, G., Murphy, C. M., et al. (2013). Comparison of ICD-10R, DSM-IV-TR and DSM-5 in an adult autism spectrum disorder diagnostic clinic. Journal of Autism and Developmental Disorders. doi:10.1007/s10803-013-1799-6.
Woolfenden, S., Sarkozy, V., Ridley, G., & Williams, K. (2012). A systematic review of the diagnostic stability of autism spectrum disorder. Research in Autism Spectrum Disorders, 6(1), 345–354.
Worley, J. A., & Matson, J. L. (2012). Comparing symptoms of autism spectrum disorders using the current DSM-IV-TR diagnostic criteria and the proposed DSM-V diagnostic criteria. Research in Autism Spectrum Disorders, 6(2), 965–970.
You, Y., Wu, B.-L., & Shen, Y. (2011). A pilot study on the diagnostic performance of DSM-IV and DSM-V for autism spectrum disorder. North American Journal of Medicine and Science, 4(3), 116–123.
Acknowledgements
Elizabeth G. Cohn’s work on this project was supported by the Robert Wood Johnson Foundation Nurse Faculty Scholars Program.
Conflict of interest
The authors declare they have no conflict of interest.
Ethical standards
This systematic literature review and meta-analysis did not involve any human subjects research.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kulage, K.M., Smaldone, A.M. & Cohn, E.G. How Will DSM-5 Affect Autism Diagnosis? A Systematic Literature Review and Meta-analysis. J Autism Dev Disord 44, 1918–1932 (2014). https://doi.org/10.1007/s10803-014-2065-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10803-014-2065-2