Abstract
Background
The indications for lymph node dissection (LND) for intrahepatic cholangiocarcinoma (ICC) are controversial.
Methods
Seventy patients with mass-forming dominant ICC underwent hepatectomy with systematic LND or lymph node sampling between 2003 and 2013. We defined the computed tomography (CT) ratio as the CT value (Hounsfield units) of the tumor divided by the CT value (Hounsfield units) of the liver parenchyma in the late arterial phase, and investigated the indications for LND with hepatectomy for ICC.
Results
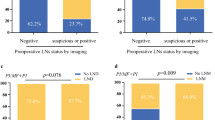
A multivariate analysis identified lymph node metastasis (LNM; n = 19, p = 0.012) and perineural invasion (p = 0.017) as independent predictors of survival. The median survival time and 5-year survival rate in patients exhibiting LNM were 31.1 months and 16.0 %, respectively. In a subgroup analysis of patients without LNM, overall survival was comparable between patients treated with LND and those treated without LND (p = 0.801). A multivariate analysis of the preoperatively measurable parameters revealed that a CT ratio <0.88 and macroscopic periductal infiltration were independently associated with LNM. We developed a score predicting LNM of mass-forming dominant ICC (LMIC score), assigning 1 point for each of these risk factors. The percentages of patients with LNM with an LMIC score of 0, 1, or 2 points were 0, 35, and 58 %, respectively.
Conclusions
The vascularity of ICC is associated with important prognostic factors, LNM, and perineural invasion. LN dissection would be conducted in patients with an LMIC score of one or two points but can be omitted in patients with an LMIC score of zero.


Similar content being viewed by others
References
Lang H, Sotiropoulos GC, Fruhauf NR, et al. Extended hepatectomy for intrahepatic cholangiocellular carcinoma (ICC): when is it worthwhile? Single center experience with 27 resections in 50 patients over a 5-year period. Ann Surg. 2005;241:134–43
Yamamoto M, Takasaki K, Yoshikawa T. Lymph node metastasis in intrahepatic cholangiocarcinoma. Jpn J Clin Oncol. 1999;29:147–50
Yamamoto Y, Shimada K, Sakamoto Y, et al. Clinicopathological characteristics of intrahepatic cholangiocellular carcinoma presenting intrahepatic bile duct growth. J Surg Oncol. 2009;99:161–5
Shimada K, Sano T, Sakamoto Y, et al. Surgical outcomes of the mass-forming plus periductal infiltrating types of intrahepatic cholangiocarcinoma: a comparative study with the typical mass-forming type of intrahepatic cholangiocarcinoma. World J Surg. 2007;31:2016–22
Inoue K, Makuuchi M, Takayama T, et al. Long-term survival and prognostic factors in the surgical treatment of mass-forming type cholangiocarcinoma. Surgery. 2000;127:498–505
Tsuji T, Hiraoka T, Kanemitsu K, et al. Lymphatic spreading pattern of intrahepatic cholangiocarcinoma. Surgery. 2001;129:401–7
Shimada M, Yamashita Y, Aishima S, et al. Value of lymph node dissection during resection of intrahepatic cholangiocarcinoma. Br J Surg. 2001;88:1463–6
Ohtsuka M, Ito H, Kimura F, et al. Results of surgical treatment for intrahepatic cholangiocarcinoma and clinicopathological factors influencing survival. Br J Surg. 2002;89:1525–31
Shirabe K, Shimada M, Harimoto N, et al. Intrahepatic cholangiocarcinoma: its mode of spreading and therapeutic modalities. Surgery. 2002;131:159–64
Shimada K, Sano T, Nara S, et al. Therapeutic value of lymph node dissection during hepatectomy in patients with intrahepatic cholangiocellular carcinoma with negative lymph node involvement. Surgery. 2009;145:411–6
Uenishi T, Yamazaki O, Horii K, et al. A long-term survivor of intrahepatic cholangiocarcinoma with paraaortic lymph node metastasis. J Gastroenterol. 2006;41:391–2
Akatsu T, Shimazu M, Kawachi S, et al. Long-term survival of intrahepatic cholangiocarcinoma with hilar lymph node metastasis and portal vein involvement. Hepatogastroenterology. 2005;52:603–5
Asakura H, Ohtsuka M, Ito H, et al. Long-term survival after extended surgical resection of intrahepatic cholangiocarcinoma with extensive lymph node metastasis. Hepatogastroenterology. 2005;52:722–4
Kobayashi S, Tomokuni A, Gotoh K, et al. Evaluation of the safety and pathological effects of neoadjuvant full-dose gemcitabine combination radiation therapy in patients with biliary tract cancer. Cancer Chemother Pharmacol. 2015;76:1191–8
Park MS, Lee DK, Kim MJ, et al. Preoperative staging accuracy of multidetector row computed tomography for extrahepatic bile duct carcinoma. J Comput Assist Tomogr. 2006;30:362–7
Xu J, Sasaki M, Harada K, et al. Intrahepatic cholangiocarcinoma arising in chronic advanced liver disease and the cholangiocarcinomatous component of hepatocellular cholangiocarcinoma share common phenotypes and cholangiocarcinogenesis. Histopathology. 2011;59:1090–9
Nakanuma Y, Sasaki M, Ikeda H, et al. Pathology of peripheral intrahepatic cholangiocarcinoma with reference to tumorigenesis. Hepatol Res. 2008;38:325–34
Xu J, Igarashi S, Sasaki M, et al. Intrahepatic cholangiocarcinomas in cirrhosis are hypervascular in comparison with those in normal livers. Liver Int. 2012;32:1156–64
Yoshida Y, Imai Y, Murakami T, et al. Intrahepatic cholangiocarcinoma with marked hypervascularity. Abdom Imaging. 1999;24:66–8
Ariizumi S, Kotera Y, Takahashi Y, et al. Mass-forming intrahepatic cholangiocarcinoma with marked enhancement on arterial-phase computed tomography reflects favorable surgical outcomes. J Surg Oncol. 2011;104:130–9
Yamamoto M, Ariizumi S, Otsubo T, et al. Intrahepatic cholangiocarcinoma diagnosed preoperatively as hepatocellular carcinoma. J Surg Oncol. 2004;87:80–3
Asayama Y, Yoshimitsu K, Irie H, et al. Delayed-phase dynamic CT enhancement as a prognostic factor for mass-forming intrahepatic cholangiocarcinoma. Radiology. 2006;238:150–5
Nanashima A, Sumida Y, Abo T, et al. Relationship between pattern of tumor enhancement and clinicopathologic characteristics in intrahepatic cholangiocarcinoma. J Surg Oncol. 2008;98:535–9
Liver Cancer Study Group of Japan. General rules for the clinical and pathological study of primary liver cancer. 3rd English ed. Tokyo: Kanehara; 2010
Uno M, Shimada K, Yamamoto Y, et al. Periductal infiltrating type of intrahepatic cholangiocarcinoma: a rare macroscopic type without any apparent mass. Surg Today. 2012;42:1189–94
Ebata T, Kosuge T, Hirano S et al. Proposal to modify the International Union Against Cancer staging system for perihilar cholangiocarcinomas. Br J Surg. 2014;101:79–88
Compton CC, Byrd DR, Garcia-Aguilar J, et al.. American Joint Committee on Cancer. Cancer staging atlas: a companion to the seventh editions of the AJCC cancer staging manual and handbook. 2nd ed. Springer, New York; 2009
Grambsch PM, Therneau TM. Proportional hazards tests and diagnostics based on weighted residuals. Biometrics. 1994;81:515–9
Roche CJ, Hughes ML, Garvey CJ, et al. CT and pathologic assessment of prospective nodal staging in patients with ductal adenocarcinoma of the head of the pancreas. AJR Am J Roentgenol. 2003;180:475–80
Horgan AM, Amir E, Walter T et al. Adjuvant therapy in the treatment of biliary tract cancer: a systematic review and meta-analysis. J Clin Oncol. 2012;30:1934–40.
Nathan H, Aloia TA, Vauthey JN et al. A proposed staging system for intrahepatic cholangiocarcinoma. Ann Surg Oncol. 2009;16:14–22
DISCLOSURE
Yusuke Yamamoto, Mehmet Akif Türkoğlu, Takeshi Aramaki, Teiichi Sugiura, Yukiyasu Okamura, Takaaki Ito, Ryo Ashida, Sunao Uemura, Takashi Miyata, Yoshiyasu Kato, Yuko Kakuta, Yasuni Nakanuma, and Katsuhiko Uesaka declare no conflicts of interest in association with this study.
Author information
Authors and Affiliations
Corresponding author
Additional information
This paper is not based on a previous communication to a society or meeting.
Rights and permissions
About this article
Cite this article
Yamamoto, Y., Türkoğlu, M.A., Aramaki, T. et al. Vascularity of Intrahepatic Cholangiocarcinoma on Computed Tomography is Predictive of Lymph Node Metastasis. Ann Surg Oncol 23 (Suppl 4), 485–493 (2016). https://doi.org/10.1245/s10434-016-5382-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-016-5382-1