Abstract
Introduction
Intracerebral haemorrhage (ICH) is associated with high morbidity and mortality. Blood pressure (BP) control is one of the main management strategies in acute ICH. Limited data currently exist regarding intracranial pressure (ICP) in acute ICH. The relationship between BP lowering and ICP is yet to be fully elucidated.
Methods
We conducted a systematic review to investigate the effects of BP lowering on ICP in acute ICH. The study protocol was registered on PROSPERO (CRD42019134470).
Results
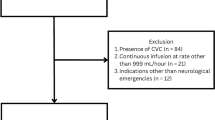
Following PRISMA guidelines, MEDLINE, EMBASE and CENTRAL were searched for studies on ICH with BP and ICP or surrogate measures. 1096 articles were identified after duplicates were removed; 18 studies meeting the inclusion criteria. Dihydropyridine calcium channel blockers (CCBs) were the most common agent used to lower BP, but had a varying effect on ICP. Other BP-lowering agents used also had a varying effect on ICP.
Discussion and Conclusion
Further work, including large observational or randomized interventional studies, is needed to develop a better understanding of the effect of BP lowering on ICP in acute ICH, which will assist the development of more effective management strategies.
Trial Registration
The study protocol was registered on PROSPERO (CRD42019134470) on 29/05/2019.




Similar content being viewed by others
References
Feigin VL, Lawes CM, Bennett DA, et al. Worldwide stroke incidence and early case fatality reported in 56 population-based studies: a systematic review. Lancet Neurol. 2009;8:355–69.
Feigin VL, Krishnamurthi RV, Parmar P, et al. Update on the global burden of ischemic and hemorrhagic stroke in 1990–2013: the GBD 2013 study. Neuroepidemiology. 2015;45:161–76.
Van Asch CJ, Luitse MJ, Rinkel GJ, et al. Incidence, case fatality, and functional outcome of intracerebral haemorrhage over time, according to age, sex, and ethnic origin: a systematic review and meta-analysis. Lancet Neurol. 2010;9:167–76.
Lovelock CE, Molyneux AJ, Rothwell PM. Oxford Vascular Study. Change in incidence and aetiology of intracerebral haemorrhage in Oxfordshire, UK, between 1981 and 2006: a population-based study. Lancet Neurol. 2007;6:487–93.
Hemphill JC, Greenberg SM, Anderson CS, et al. Guidelines for the management of spontaneous intracerebral haemorrhage: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2015;46:2032–60.
Kazui S, Minematsu K, Yamamoto H, et al. Predisposing factors to enlargement of spontaneous intracerebral hematoma. Stroke. 1997;28:2370–5.
Zhang Y, Reilly KH, Tong W, et al. Blood pressure and clinical outcome among patients with acute stroke in Inner Mongolia, China. J Hypertens. 2008;26:1446–52.
Anderson CS, Heeley E, Huang Y, et al. Rapid blood-pressure lowering in patients with acute intracerebral hemorrhage. N Engl J Med. 2013;368:2355–65.
Qureshi AI, Palesch YY, Barsan WG, et al. Intensive blood-pressure lowering in patients with acute cerebral hemorrhage. N Engl J Med. 2016;375:1033–43.
Moullaali TJ, Wang X, Martin RH, et al. Blood pressure control and clinical outcomes in acute intracerebral haemorrhage: a preplanned pooled analysis of individual participant data. Lancet Neurol. 2019;18:857–64.
Parry-Jones AR, Sammut-Powell C, Paroutoglou K, et al. An intracerebral hemorrhage care bundle is associated with lower case fatality. Ann Neurol. 2019;86:495–503.
Minhas JS, Panerai RB, Ghaly G, et al. Cerebral autoregulation in hemorrhagic stroke: a systematic review and meta-analysis of transcranial Doppler ultrasonography studies. J Clin Ultrasound. 2019;47:14–21.
Balami JS, Buchan AM. Complications of intracerebral haemorrhage. Lancet Neurol. 2012;11:101–18.
Tameem A, Krovvidi H. Cerebral physiology. BJA Educ. 2013;13:113–8.
Kamel H, Hemphill JC. Characteristics and sequelae of intracranial hypertension after intracerebral hemorrhage. Neurocrit Care. 2012;17:172–6.
Willmot M, Ghadami A, Whysall B, et al. Transdermal glyceryl trinitrate lowers blood pressure and maintains cerebral blood flow in recent stroke. Hypertension. 2006;47:1209–15.
Moher D, Liberati A, Tetzlaff J, Altman DG. PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med. 2009;6:e1000097.
Li Y, Fang W, Tao L, et al. Efficacy and safety of intravenous nimodipine administration for treatment of hypertension in patients with intracerebral hemorrhage. Neuropsychiatr Dis Treat. 2015;11:1231–8.
Gavito-Higuera J, Khatri R, Qureshi IA, et al. Aggressive blood pressure treatment of hypertensive intracerebral hemorrhage may lead to global cerebral hypoperfusion: case report and imaging perspective. World J Radiol. 2017;9:448–53.
Tamm AS, McCourt R, Gould B, et al. Cerebral perfusion pressure is maintained in acute intracerebral hemorrhage: a CT perfusion study. AJNR Am J Neuroradiol. 2016;37:244–51.
Strong J, Gatz JD, Al Rebh H, et al. 273 emergency providers did not adequately manage patients with spontaneous intracranial hemorrhage and suspected intracranial hypertension. Ann Emerg Med. 2017;70:S108.
Nishiyama T, Yokoyama T, Matsukawa T, et al. Continuous nicardipine infusion to control blood pressure after evacuation of acute cerebral hemorrhage. Can J Anaesth. 2000;47:1196–201.
Ko SB, Choi HA, Parikh G, et al. Multimodality monitoring for cerebral perfusion pressure optimization in comatose patients with intracerebral hemorrhage. Stroke. 2011;42:3087–92.
Ziai WC, Melnychuk E, Thompson CB, et al. Occurrence and impact of intracranial pressure elevation during treatment of severe intraventricular hemorrhage. Crit Care Med. 2012;40:1601–8.
Hamani C, Zanetti MV, Pinto FC, et al. Intraventricular pressure monitoring in patients with thalamic and ganglionic hemorrhages. Arq Neuropsiquiatr. 2003;61:376–80.
Tian Y, Wang Z, Jia Y, et al. Intracranial pressure variability predicts short-term outcome after intracerebral hemorrhage: a retrospective study. J Neurol Sci. 2013;330:38–44.
Hirayama T, Katayama Y, Kano T, et al. Control of systemic hypertension with Diltiazem, a calcium-antagonist, in patients with a mildly elevated intracranial pressure: a comparative study. Neurol Res. 1994;16:97–9.
Elwood KA, Lam TS, Rhodes HM, et al. P396 Impact of clevidipine on intracranial pressure in adults with intracranial haemorrhage. Crit Care. 2018;22(Suppl 1):82.
Tuteja G, Uppal A, Strong J, et al. Interventions affecting blood pressure variability and outcomes after intubating patients with spontaneous intracranial hemorrhage. Am J Emerg Med. 2019;37:1665–71.
Picetti E, De Angelis A, Villani F, et al. Intravenous paracetamol for fever control in acute brain injury patients: cerebral and hemodynamic effects. Acta Neurochir. 2014;156:1953–9.
Narotam PK, Puri V, Roberts JM, et al. Management of hypertensive emergencies in acute brain disease: evaluation of the treatment effects of intravenous nicardipine on cerebral oxygenation. J Neurosurg. 2008;109:1065–74.
Hayashi M, Kobayashi H, Kawano H, et al. Treatment of systemic hypertension and intracranial hypertension in cases of brain hemorrhage. Stroke. 1988;19:314–21.
Suarez JI, Qureshi AI, Bhardwaj A, et al. Treatment of refractory intracranial hypertension with 23.4% saline. Crit Care Med. 1998;26:1118–22.
Woodcock JO, Ropper AH, Kennedy SK. High dose barbiturates in non-traumatic brain swelling: ICP reduction and effect on outcome. Stroke. 1982;13:785–7.
Ankolekar S, Fuller M, Cross I, et al. Feasibility of an ambulance-based stroke trial, and safety of glyceryl trinitrate in ultra-acute stroke: the rapid intervention with glyceryl trinitrate in Hypertensive Stroke Trial (RIGHT, ISRCTN66434824). Stroke. 2013;44:3120–8.
Woodhouse L, Scutt P, Krishnan K, et al. Effect of hyperacute administration (within 6 hours) of transdermal glyceryl trinitrate, a nitric oxide donor, on outcome after stroke: subgroup analysis of the efficacy of Nitric Oxide in Stroke (ENOS) trial. Stroke. 2015;46:3194–201.
Bath PM, Scutt P, Anderson CS, et al. Prehospital transdermal glyceryl trinitrate in patients with ultra-acute presumed stroke (RIGHT-2): an ambulance-based, randomised, sham-controlled, blinded, phase 3 trial. Lancet. 2019;393:1009–20.
Bath PM, Woodhouse LJ, Krishnan K, et al. Prehospital transdermal glyceryl trinitrate for ultra-acute intracerebral hemorrhage: data from the RIGHT-2 trial. Stroke. 2019;50:3064–71.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
MK is an NIHR Academic Clinical Fellow. JSM is an NIHR Clinical Lecturer in Older People and Complex Health Needs. APJ is an NIHR Clinician Scientist. TGR is an NIHR Senior Investigator. The views expressed in this publication are those of the author(s) and not necessarily those of the NHS, the National Institute for Health Research, the Department of Health, or the authors’ respective institutions.
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Availability of data and material
Material and data included in manuscript.
Author contributions
MK, TGR, APJ and JSM conceived and designed the review. MK, PD and JSM searched and selected the studies. MK and JSM prepared the figures. All authors read and approved the final manuscript.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kadicheeni, M., Robinson, T.G., Divall, P. et al. Therapeutic Variation in Lowering Blood Pressure: Effects on Intracranial Pressure in Acute Intracerebral Haemorrhage. High Blood Press Cardiovasc Prev 28, 115–128 (2021). https://doi.org/10.1007/s40292-021-00435-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40292-021-00435-z