Abstract
Introduction
Hypertension is one of the major risk factors for cardiovascular disease and the leading cause of death worldwide. Hypertension was defined as systolic or diastolic blood pressure according to Joint National Committee 7 (JNC7) and 2017 American College of Cardiology/American Hypertension Association (ACC/AHA) rules.
Aim
The aims of this study was to determine the difference in hypertension prevalence and its risk factors using ACC/AHA rule, and compared its result with JNC7 rule.
Methods
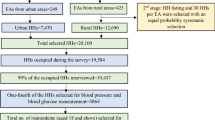
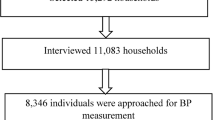
Data were collected using two-stage stratified cluster sample of households from 2017/18 Albanian Demographic and Health Survey. Data were analyzed using the descriptive and multivariate logistic regression model.
Results
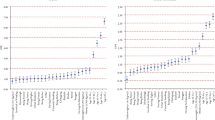
Among 15,003 respondents aged 15–49 years, the overall prevalence of hypertension was 63.48% and 16.24%, as per ACC/AHA and JNC7 rules, respectively with an absolute increase of prevalence by 47.3% (CI 46.4–48.2%). According to the ACC/AHA rule, in most of the categories of the respondents, the prevalence of hypertension was 40% higher compared with the JNC7 rule. In multivariate analysis, age, education, richest respondents, number of living children (≥ 3), health insurance and gender had significant (p < 0.05) impact on hypertension for both rules. Besides, the middle and richer wealth index, religion, and physically active work had also significant (p < 0.05) impact on hypertension for JNC7 rules.
Conclusions
Newly established ACC/AHA rule led to a significant increase in the proportion of hypertension among the Albanian populations. Similarly, there was a significant difference in the impact of some socioeconomic factors on hypertension as per both rules. Implementation of the prevention and control programs of hypertension are required to increase the awareness of the bad impact of hypertension.
Similar content being viewed by others
References
Kassebaum NJ, Arora M, Barber RM, Bhutta ZA, Brown J, Carter A, Casey DC, Charlson FJ, Coates MM, Coggeshall M, Cornaby L. Global, regional, and national disability-adjusted life-years (DALYs) for 315 diseases and injuries and healthy life expectancy (HALE), 1990–2015: a systematic analysis for the Global Burden of Disease Study 2015. Lancet. 2016;388(10053):1603–58.
Mills KT, Bundy JD, Kelly TN, Reed JE, Kearney PM, Reynolds K, Chen J, He J. Global disparities of hypertension prevalence and control: a systematic analysis of population-based studies from 90 countries. Circulation. 2016;134(6):441–50.
Kayima J, Nankabirwa J, Sinabulya I, Nakibuuka J, Zhu X, Rahman M, Longenecker CT, Katamba A, Mayanja-Kizza H, Kamya MR. Determinants of hypertension in a young adult Ugandan population in epidemiological transition—the MEPI-CVD survey. BMC Public Health. 2015;15(1):830.
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo JL Jr, Jones DW, Materson BJ, Oparil S, Wright JT Jr, Roccella EJ. The seventh report of the joint national committee on prevention, detection, evaluation, and treatment of high blood pressure: the JNC 7 report. JAMA. 2003;289(19):2560–71.
Roth GA, Johnson C, Abajobir A, Abd-Allah F, Abera SF, Abyu G, Ahmed M, Aksut B, Alam T, Alam K, Alla F. Global, regional, and national burden of cardiovascular diseases for 10 causes, 1990 to 2015. J Am Coll Cardiol. 2017;70(1):1–25.
Thawornchaisit P, de Looze F, Reid CM, Seubsman A, Sleigh AC. Health risk factors and the incidence of hypertension: 4-year prospective findings from a national cohort of 60 569 Thai Open University students. BMJ Open. 2013;3(6):e002826.
Whitworth JA. International Society of Hypertension Writing Group: 2003 World Health Organization (WHO)/International Society of Hypertension (ISH) statement on management of hypertension. J Hypertens. 2003;21:1983–92.
Kearney PM, Whelton M, Reynolds K, Muntner P, Whelton PK, He J. Global burden of hypertension: analysis of worldwide data. Lancet. 2005;365(9455):217–23.
Khanam R, Ahmed S, Rahman S, Al Kibria GM, Syed JR, Khan AM, Moin SM, Ram M, Gibson DG, Pariyo G, Baqui AH. Prevalence and factors associated with hypertension among adults in rural Sylhet district of Bangladesh: a cross-sectional study. BMJ Open. 2019;9:e026722. https://doi.org/10.1136/bmjopen-2018-026722.
O’Brien E. The Lancet Commission on hypertension: addressing the global burden of raised blood pressure on current and future generations. J Clin Hypertens. 2017;19(6):564–8.
Ali J, Gul AM, Irfan M, Querishi MS, Faheem M, Hussain C, Khan SB, Shah SF, Hafizullah M. How frequent are cardiovascular risk factors in lawyers? Pak Heart J. 2012;45(2):91–6.
Ghose B, Yaya S. Blood pressure-controlling behavior in relation to educational level and economic status among hypertensive women in Ghana. Fam Med Community Health. 2018;6(3):114–23.
Chow CK, Teo KK, Rangarajan S, Islam S, Gupta R, Avezum A, Bahonar A, Chifamba J, Dagenais G, Diaz R, Kazmi K. Prevalence, awareness, treatment, and control of hypertension in rural and urban communities in high-, middle-, and low-income countries. JAMA. 2013;310(9):959–68.
Pirkle CM, Ylli A, Burazeri G, Sentell TL. Social and community factors associated with hypertension awareness and control among older adults in Tirana, Albania. Eur J Public Health. 2018;28(6):1163–8.
Petrela E, Burazeri G, Pupuleku F, Zaimi E, Rahman M. Prevalence and correlates of hypertension in a transitional southeastern European population: results from the Albanian Demographic and Health Survey. Arch Ind Hyg Toxicol. 2013;64(4):479–87.
Mackenbach J, and McKee M. Successes and failures of health policy in Europe: Four decades of divergent trends and converging challenges: Four decades of divergent trends and converging challenges. McGraw-Hill Education (UK), 2013.
Whelton PK, Carey RM, Aronow WS, Casey DE, Collins KJ, Himmelfarb CD, DePalma SM, Gidding S, Jamerson KA, Jones DW, MacLaughlin EJ. 2017ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol. 2018;71(19):127–248.
Rahman M, Zaman MM, Islam JY, Chowdhury J, Ahsan HN, Rahman R, Hassan M, Hossain Z, Alam B, Yasmin R. Prevalence, treatment patterns, and risk factors of hypertension and pre-hypertension among Bangladeshi adults. J Hum Hypertens. 2018;32(5):334–48.
Tocci G, Presta V, Figliuzzi I, Miceli F, Citoni B, Coluccia R, Paini A, Salvetti M, Ferrucci A, Muiesan ML, Volpe M. Reclassification of hypertensive outpatients according to new US guidelines on high blood pressure. Am J Hypertens. 2019;32(1):77–87.
Shapo L, Pomerleau J, McKee M. Epidemiology of hypertension and associated cardiovascular risk factors in a country in transition: a population-based survey in Tirana City, Albania. J Epidemiol Community Health. 2003;57(9):734–9.
Gelber RP, Gaziano JM, Manson JE, Buring JE, Sesso HD. A prospective study of body mass index and the risk of developing hypertension in men. Am J Hypertens. 2007;20(4):370–7.
Burazeri G, Goda A, Sulo G, Stefa J, Roshi E, Kark JD. Conventional risk factors and acute coronary syndrome during a period of socioeconomic transition: population-based case-control study in Tirana, Albania. Croatian Med J. 2007;48(2):225–33.
Shurdha O, Hasimi E, Petrela E, Goda A. Prevalence of major cardiovascular risk factors among adults in Albania. Int J Sci Res. 2015;4(12):604–7.
Abariga SA, Khachan H, Al Kibria GM. Prevalence and determinants of hypertension in India based on the 2017 ACC/AHA guideline: evidence from the India national family health survey. Am J Hypertens. 2020;33(3):252–60.
Al Kibria GM, Swasey K, Angela KC, Mirbolouk M, Sakib MN, Sharmeen A, Chadni MJ, Stafford KA. Estimated change in prevalence of hypertension in Nepal following application of the 2017 ACC/AHA guideline. JAMA Netw Open. 2018;1(3):e180606.
Al Kibria GM, Swasey K, Choudhury A, Burrowes V, Stafford KA, Uddin SI, Mirbolouk M, Sharmeen A, Angela KC, Mitra DK. The new 2017 ACC/AHA guideline for classification of hypertension: changes in prevalence of hypertension among adults in Bangladesh. J Hum Hypertens. 2018;32(8):608–16.
Verdecchia P, Angeli F. The seventh report of the joint national committee on the prevention, detection, evaluation and treatment of high blood pressure: the weapons are ready. Rev Esp Cardiol. 2003;56(9):843–7.
Al Kibria GM, Swasey K, Hasan MZ, Choudhury A, Gupta RD, Abariga SA, Sharmeen A, Burrowes V. Determinants of hypertension among adults in Bangladesh as per the Joint National Committee 7 and 2017 American College of Cardiology/American Hypertension Association hypertension guidelines. J Am Soc Hypertens. 2018;12(11):e45–55.
Kario K. Global impact of 2017 American Heart Association/American College of Cardiology hypertension guidelines: a perspective from Japan. Circulation. 2018;137:543–5.
Schiffrin EL. Global impact of the 2017 American College of Cardiology/American Heart Association hypertension guidelines: a perspective from Canada. Circulation. 2018;137:883–5.
Pinto E. Blood pressure and ageing. Postgrad Med J. 2007;83(976):109–14.
Chowdhury MAB, Uddin, MJ, Haque MR, Ibrahimou, B. Hypertension among adults in Bangladesh: evidence from a national cross-sectional survey. BMC Cardiovasc Disord. 2016;16(1):22.
Lewington S, Clarke R, Qizilbash N, Peto R, Collins R. Prospective Studies Collaboration. Age-specific relevance of usual blood pressure to vascular mortality: a meta-analysis of individual data for one million adults in 61 prospective studies. Lancet 2002; 360:1903–13.
Sun Z. Aging, arterial stiffness, and hypertension. Hypertension. 2014;65(2):252–6.
AlGhatrif M, Strait JB, Morrell CH, Canepa M, Wright J, Elango P, Scuteri A, Najjar SS, Ferrucci L, Lakatta EG. Longitudinal trajectories of arterial stiffness and the role of blood pressure: the Baltimore Longitudinal Study of Aging. Hypertension. 2013;62(5):934–41.
Ong KL, Cheung BM, Man YB, Lau CP, Lam KS. Prevalence, awareness, treatment, and control of hypertension among United States adults 1999–2004. Hypertension. 2007;49(1):69–75.
Hasan M, Sutradhar I, Akter T, Gupta RD, Joshi H, Haider MR, Sarker M. Prevalence and determinants of hypertension among adult population in Nepal: data from Nepal Demographic and Health Survey 2016. PLoS One. 2018;13(5):e0198028.
Basu S, Millett C. Social epidemiology of hypertension in middle-income countries: determinants of prevalence, diagnosis, treatment, and control in the WHO SAGE study. Hypertension. 2013;62(1):18–26.
Keetile M, Navaneetham K, Letamo G. Patterns and determinants of hypertension in Botswana. J Public Health. 2014;23(5):311–8.
Laxmaiah A, Meshram II, Arlappa N, Balakrishna N, Rao KM, Reddy CG, Ravindranath M, Kumar S, Kumar H, Brahmam GN. Socio-economic & demographic determinants of hypertension & knowledge, practices & risk behaviour of tribals in India. Indian J Med Res. 2014;141(5):697.
Singh S, Shankar R, Singh GP. Prevalence and associated risk factors of hypertension: a cross-sectional study in urban Varanasi. Int J Hypertens. 2017. https://doi.org/10.1155/2017/5491838.
Cuschieri S, Vassallo J, Calleja N, Pace N, Mamo J. The effects of socioeconomic determinants on hypertension in a cardiometabolic at-risk European country. Int J Hypertens. 2017. https://doi.org/10.1155/2017/7107385.
Peltzer K, Pengpid S. The prevalence and social determinants of hypertension among adults in Indonesia: a cross-sectional population-based national survey. Int J Hypertens. 2018. https://doi.org/10.1155/2018/5610725.
Malekzadeh MM, Etemadi A, Kamangar F, Khademi H, Golozar A, Islami F, Pourshams A, Poustchi H, Navabakhsh B, Naemi M, Pharoah PD. Prevalence, awareness and risk factors of hypertension in a large cohort of Iranian adult population. J Hypertens. 2013;31(7):1364.
Scholes S, Bajekal M, Love H, Hawkins N, Raine R, O’Flaherty M, Capewell S. Persistent socioeconomic inequalities in cardiovascular risk factors in England over 1994-2008: a time-trend analysis of repeated cross-sectional data. BMC Public Health. 2012;12(1):129.
Reddy KS, Naik N, Prabhakaran D. Hypertension in the developing world: a consequence of progress. Curr Cardiol Rep. 2006;8(6):399–404.
Seedat YK. Impact of poverty on hypertension and cardiovascular disease in sub-Saharan Africa. Cardiovasc J Afr. 2007;18(5):316.
Lear SA, Teo K, Gasevic D, Zhang X, Poirier PP, Rangarajan S, Seron P, Kelishadi R, Tamil AM, Kruger A, Iqbal R. The association between ownership of common household devices and obesity and diabetes in high, middle- and low-income countries. CMAJ. 2014;186(4):258–66.
Magallanes, JM. Human nutrition: the impact of family size and income on dietary intake. Philippine Sociol Rev. 1984;69–79.
Mekonnen TT, Woldeyohannes SM, Yigzaw T. Contraceptive use in women with hypertension and diabetes: cross-sectional study in northwest Ethiopia. Int J Women’s Health. 2015;7:957–64.
Oso AA, Adefurin A, Benneman MM, Oso OO, Taiwo MA, Adebiyi OO, Oluwole O. Health insurance status affects hypertension control in a hospital based internal medicine clinic. Int J Cardiol Hypertens. 2019;1:100003.
Fang J, Zhao G, Wang G, Ayala C, Loustalot F. Insurance status among adults with hypertension—the impact of underinsurance. J Am Heart Assoc. 2016;5(12):e004313.
Keith C, Norris KC. Health insurance and blood pressure control. J Am Heart Assoc. 2016;5:e005130.
Sampson UK, Edwards TL, Jahangir E, Munro H, Wariboko M, Wassef MG, Fazio S, Mensah GA, Kabagambe EK, Blot WJ, Lipworth L. Factors associated with the prevalence of hypertension in the southeastern United States: insights from 69 211 blacks and whites in the southern community cohort study. Circ Cardiovasc Qual Outcomes. 2014;7(1):33–54.
Ghosh S, Mukhopadhyay S, Barik A. Sex differences in the risk profile of hypertension: a cross-sectional study. BMJ Open. 2016;6(7):e010085.
Tocci G, Presta V, Ferri C, Redon J, Volpe M. Blood Pressure Targets Achievement According to 2018 ESC/ESH guidelines in three european excellence centers for hypertension. High Blood Pressure Cardiovasc Prev. 2020;27(1):51–9.
Acknowledgements
Authors acknowledge the Demographic and Health Surveys (DHS) Program for providing data. The authors are grateful to the Statistics Discipline, Khulna University, Khulna-9208, Bangladesh, where this study is conducted. Authors are also thankful to authors of different articles are used in this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This research received no specific grant from any funding agency, commercial entity or not-for-profit organization.
Conflicts of interest/Competing interests
The authors have no conflicts of interest to declare.
Availability of data and material
The data is available at: https://dhsprogram.com/data/available-datasets.cfm.
Code availability
None.
Authors’ contributions
Benojir Ahammed designed the design of this study, after collecting and checking the data, performed the statistical analysis and write the manuscript; Md. Maniruzzaman checked the data and edited the manuscript; Ashis Talukder edited the manuscript; Farzana Ferdausi review relavent literature and write the manuscript. All authors have read and approved the final manuscript.
Rights and permissions
About this article
Cite this article
Ahammed, B., Maniruzzaman, M., Talukder, A. et al. Prevalence and Risk Factors of Hypertension Among Young Adults in Albania. High Blood Press Cardiovasc Prev 28, 35–48 (2021). https://doi.org/10.1007/s40292-020-00419-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40292-020-00419-5