Abstract
Introduction
Structural and functional properties of the left ventricle (LV) wall have been reported to be altered in hypertension, even at early stages of the disease. Abnormal adipokine levels affect blood pressure regulation. Hypo-adiponectinaemia and hyper-leptinaemia were reported in hypertension.
Aim
To evaluate the effects of valsartan versus amlodipine on LV deformation also, on plasma adiponectin and leptin levels in hypertensive individuals.
Methods
LV strain was measured by two-dimensional speckle tracking echocardiography, plasma levels of adiponectin and leptin was determined in 30 healthy individuals served as control group and in 200 hypertensive patients before and after treatment for 6 months with either valsartan 160 mg or amlodipine 10 mg.
Results
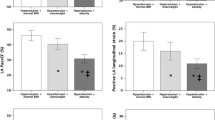
Compared to control group longitudinal strain was significantly affected in hypertensive patients, adiponectin was significantly lower while TNF-α, hs-CRP and leptin levels were significantly higher in hypertensive group. A significant improvement in LV functions, along with a decrease in leptin and increase in adiponectin levels in valsartan group compared to amlodipine group.
Conclusions
Our results indicate that valsartan is superior to amlodipine when it comes to affecting the hormonal function of human adipose tissue. Valsartan has a beneficial effect on LV deformation and function presented in GLS.

Similar content being viewed by others
References
Kannel WB. Incidence and epidemiology of heart failure. Heart Fail Rev. 2000;5(2):67–73. https://doi.org/10.1023/A:1009884820941.
Rusconi C, Sabatini T, Faggiano P, Ghizzoni G, Oneglia C, Simoncelli U, Gualeni A, Sorgato A, Marchetti A. Prevalence of isolated left ventricular diastolic dysfunction in hypertension as assessed by combined transmitral and pulmonary vein flow Doppler study. Am J Cardiol. 2001;87(3):357–60. https://doi.org/10.1016/s0002-9149(00)01378-3.
García EH, Perna ER, Farías EF, Obregón RO, Macin SM, Parras JI, Agüero MA, Moratorio DA, Pitzus AE, Tassano EA, Rodriguez L. Reduced systolic performance by tissue Doppler in patients with preserved and abnormal ejection fraction: new insights in chronic heart failure. Int J Cardiol. 2006;108(2):181–8. https://doi.org/10.1016/j.ijcard.2005.04.026.
Sanderson JE. Heart failure with a normal ejection fraction. Heart. 2007;93(2):155–8. https://doi.org/10.1136/hrt.2005.074187.
Kraigher-Krainer E, Shah AM, Gupta DK, Santos A, Claggett B, Pieske B, Zile MR, Voors AA, Lefkowitz MP, Packer M, McMurray JJ, Solomon SD, PARAMOUNT Investigators (2014) Impaired systolic function by strain imaging in heart failure with preserved ejection fraction. J Am Coll Cardiol 63(5):447–456. https://doi.org/10.1016/j.jacc.2013.09.052
Sabbatini AR, Fontana V, Laurent S, Moreno H. An update on the role of adipokines in arterial stiffness and hypertension. J Hypertens. 2015;33(3):435–44. https://doi.org/10.1097/HJH.0000000000000444.
Fontana V, de Faria AP, Oliveira-Paula GH, Silva PS, Biagi C, Tanus-Santos JE, Moreno H. Effects of angiotensin-converting enzyme inhibition on leptin and adiponectin levels in essential hypertension. Basic Clin Pharmacol Toxicol. 2014;114(6):472–5. https://doi.org/10.1111/bcpt.12195.
Kim DH, Kim C, Ding EL, Townsend MK, Lipsitz LA. Adiponectin levels and the risk of hypertension: a systematic review and meta-analysis. Hypertension. 2013;62(1):27–322. https://doi.org/10.1161/HYPERTENSIONAHA.113.01453.
Scotece M, Conde J, López V, Lago F, Pino J, Gómez-Reino JJ, Gualillo O. Adiponectin and leptin: new targets in inflammation. Basic Clin Pharmacol Toxicol. 2014;114(1):97–102. https://doi.org/10.1111/bcpt.12109.
Galletti F, D'Elia L, Barba G, Siani A, Cappuccio FP, Farinaro E, Iacone R, Russo O, De Palma D, Ippolito R, Strazzullo P. High-circulating leptin levels are associated with greater risk of hypertension in men independently of body mass and insulin resistance: results of an eight-year follow-up study. J Clin Endocrinol Metab. 2008;93(10):3922–6. https://doi.org/10.1210/jc.2008-1280.
Singhal A, Farooqi IS, Cole TJ, O'Rahilly S, Fewtrell M, Kattenhorn M, Lucas A, Deanfield J. Influence of leptin on arterial distensibility: a novel link between obesity and cardiovascular disease? Circulation. 2002;106(15):1919–24. https://doi.org/10.1161/01.cir.0000033219.24717.52.
Rahmouni K, Morgan DA. Hypothalamic arcuate nucleus mediates the sympathetic and arterial pressure responses to leptin. Hypertension. 2007;49(3):647–52. https://doi.org/10.1161/01.HYP.0000254827.59792.b2.
Black HR, Bailey J, Zappe D, Samuel R. Valsartan: more than a decade of experience. Drugs. 2009;69(17):2393–414. https://doi.org/10.2165/11319460-000000000-00000.
Jeffers BW, Robbins J, Bhambri R, Wajsbrot D. A Systematic review on the efficacy of amlodipine in the treatment of patients with hypertension with concomitant diabetes mellitus and/or renal dysfunction, when compared with other classes of antihypertensive medication. Am J Ther. 2015;22(5):322–41. https://doi.org/10.1097/MJT.0000000000000202.
Lang RM, Bierig M, Devereux RB, Flachskampf FA, Foster E, Pellikka PA, Picard MH, Roman MJ, Seward J, Shanewise J, Solomon S, Spencer KT, St John Sutton M, Stewart W. Recommendations for chamber quantification. Eur J Echocardiogr. 2006;7(2):79–108. https://doi.org/10.1016/j.euje.2005.12.014.
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L, Flachskampf FA, Foster E, Goldstein SA, Kuznetsova T, Lancellotti P, Muraru D, Picard MH, Rietzschel ER, Rudski L, Spencer KT, Tsang W, Voigt JU. Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr. 2015;28(1):1–39.e14. https://doi.org/10.1016/j.echo.2014.10.003.
Sun JP, Lee AP, Wu C, Lam YY, Hung MJ, Chen L, Hu Z, Fang F, Yang XS, Merlino JD, Yu CM. Quantification of left ventricular regional myocardial function using two-dimensional speckle tracking echocardiography in healthy volunteers–a multi-center study. Int J Cardiol. 2013;167(2):495–501. https://doi.org/10.1016/j.ijcard.2012.01.071.
Feigenbaum H, Mastouri R, Sawada S. A practical approach to using strain echocardiography to evaluate the left ventricle. Circ J. 2012;76(7):1550–5. https://doi.org/10.1253/circj.CJ-12-0665.
Dalen H, Thorstensen A, Aase SA, Ingul CB, Torp H, Vatten LJ, Stoylen A. Segmental and global longitudinal strain and strain rate based on echocardiography of 1266 healthy individuals: the HUNT study in Norway. Eur J Echocardiogr. 2010;11(12):176–83. https://doi.org/10.1093/ejechocard/jep194.
Wiesner G, Vaz M, Collier G, Seals D, Kaye D, Jennings G, Lambert G, Wilkinson D, Esler M. Leptin is released from the human brain: influence of adiposity and gender. J Clin Endocrinol Metab. 1999;84(7):2270–4. https://doi.org/10.1210/jcem.84.7.5854.
Tsao TS, Lodish HF, Fruebis J. ACRP30, a new hormone controlling fat and glucose metabolism. Eur J Pharmacol. 2002;440(2–3):213–21. https://doi.org/10.1016/s0014-2999(02)01430-9.
Brouckaert P, Libert C, Everaerdt B, Takahashi N, Cauwels A, Fiers W. Tumor necrosis factor, its receptors and the connection with interleukin 1 and interleukin 6. Immunobiology. 1993;187(3–5):317–29. https://doi.org/10.1016/S0171-2985(11)80347-5.
Avci E, Cakir E, Cevher SC, Yaman H, Agilli M, Bilgi C. Determination of oxidative stress and cellular inflammation in patients with diabetic nephropathy and non-diabetic nephropathy being administered hemodialysis treatment due to chronic renal failure. Ren Fail. 2014;36(5):767–73. https://doi.org/10.3109/0886022X.2014.890841.
Delles C, Klingbeil AU, Schneider MP, Handrock R, Weidinger G, Schmieder RE. Direct comparison of the effects of valsartan and amlodipine on renal hemodynamics in human essential hypertension. Am J Hypertens. 2003;16(12):1030–5. https://doi.org/10.1016/j.amjhyper.2003.07.017.
Fogari R, Derosa G, Zoppi A, Rinaldi A, Lazzari P, Fogari E, Mugellini A, Preti P. Comparison of the effects of valsartan and felodipine on plasma leptin and insulin sensitivity in hypertensive obese patients. Hypertens Res. 2005;28(3):209–14. https://doi.org/10.1291/hypres.28.209.
Ohashi K, Ouchi N, Matsuzawa Y. Adiponectin and hypertension. Am J Hypertens. 2011;24(3):263–9. https://doi.org/10.1038/ajh.2010.216.
Iwashima Y, Katsuya T, Ishikawa K, Ouchi N, Ohishi M, Sugimoto K, Fu Y, Motone M, Yamamoto K, Matsuo A, Ohashi K, Kihara S, Funahashi T, Rakugi H, Matsuzawa Y, Ogihara T. Hypoadiponectinemia is an independent risk factor for hypertension. Hypertension. 2004;43(6):1318–23. https://doi.org/10.1161/01.HYP.0000129281.03801.4b.
Schillaci G, Verdecchia P, Porcellati C, Cuccurullo O, Cosco C, Perticone F. Continuous relation between left ventricular mass and cardiovascular risk in essential hypertension. Hypertension. 2000;35(2):580–6. https://doi.org/10.1161/01.hyp.35.2.580.
Ayoub AM, Keddeas VW, Ali YA, El Okl RA. Subclinical LV dysfunction detection using speckle tracking echocardiography in hypertensive patients with preserved LV ejection fraction. Clin Med Insights Cardiol. 2016;27(10):85–90. https://doi.org/10.4137/CMC.S38407.
Tadic M, Majstorovic A, Pencic B, Ivanovic B, Neskovic A, Badano L, Stanisavljevic D, Scepanovic R, Stevanovic P, Celic V. The impact of high-normal blood pressure on left ventricular mechanics: a three-dimensional and speckle tracking echocardiography study. Int J Cardiovasc Imaging. 2014;30(4):699–711. https://doi.org/10.1007/s10554-014-0382-3.
Kim SA, Park SM, Kim MN, Shim WJ. Assessment of left ventricular function by layer-specific strain and its relationship to structural remodelling in patients with hypertension. Can J Cardiol. 2016;32(2):211–6. https://doi.org/10.1016/j.cjca.2015.04.025.
Yilmaz MI, Sonmez A, Caglar K, Celik T, Yenicesu M, Eyileten T, Acikel C, Oguz Y, Yavuz I, Vural A. Effect of antihypertensive agents on plasma adiponectin levels in hypertensive patients with metabolic syndrome. Nephrology (Carlton). 2007;12(2):147–53. https://doi.org/10.1111/j.1440-1797.2007.00764.x.
Ohbayashi H, Minatoguchi S, Aoyama T, Fujiwara H. Open-label, randomized crossover study between telmisartan and valsartan on improving insulin resistance and adipocytokines in nondiabetic patients with mild hypertension. J Rural Med. 2010;5(2):165–74. https://doi.org/10.2185/jrm.5.165.
Fliser D, Buchholz K, Haller H. Antiinflammatory effects of angiotensin II subtype 1 receptor blockade in hypertensive patients with microinflammation. Circulation. 2004;110(9):1103–7. https://doi.org/10.1161/01.CIR.0000140265.21608.8E.
Pscherer S, Heemann U, Frank H. Effect of Renin-Angiotensin system blockade on insulin resistance and inflammatory parameters in patients with impaired glucose tolerance. Diabetes Care. 2010;33(4):914–9. https://doi.org/10.2337/dc09-1381.
Aksnes TA, Seljeflot I, Torjesen PA, Hoieggen A, Moan A, Kjeldsen SE. Improved insulin sensitivity by the angiotensin II-receptor blocker losartan is not explained by adipokines, inflammatory markers, or whole blood viscosity. Metabolism. 2007;56(11):1470–7. https://doi.org/10.1016/j.metabol.2007.06.012.
Goossens GH, Moors CC, van der Zijl NJ, Venteclef N, Alili R, Jocken JW, Essers Y, Cleutjens JP, Clément K, Diamant M, Blaak EE. Valsartan improves adipose tissue function in humans with impaired glucose metabolism: a randomized placebo-controlled double-blind trial. PLoS ONE. 2012;7(6):e39930. https://doi.org/10.1371/journal.pone.0039930.
Watanabe S, Okura T, Kurata M, Irita J, Manabe S, Miyoshi K, Fukuoka T, Murakami K, Higaki J. The effect of losartan and amlodipine on serum adiponectin in Japanese adults with essential hypertension. Clin Ther. 2006;28(10):1677–85. https://doi.org/10.1016/j.clinthera.2006.10.012.
Özkan B, Açar G, Alıcı G, Alizade E, Tabakcı MM, Sahin M, Yazıcıoğlu MV, Ozkok A, Tanboğa IH, Coşkun C, Esen AM. Decreased plasma adiponectin is associated with impaired left ventricular longitudinal systolic function in hypertensive patients: a two-dimensional speckle tracking study. Clin Exp Hypertens. 2014;36(1):46–51. https://doi.org/10.3109/10641963.2013.783053.
Vitlyanova K, Naidenov S, Runev N, Manov E, Shabani R, Rangelov Y, Koshtikova K, Donova T. Effects of the angiotensin receptor blocker Valsartan (Valsacor®) on arterial pressure, indices of myocardial diastolic function and global longitudinal strain in patients with uncontrolled arterial hypertension. Vnitr Lek. 2013;59(12):1124–8 (PMID: 24466609).
Yamamoto K, Mano T, Yoshida J, Sakata Y, Nishikawa N, Nishio M, Ohtani T, Hori M, Miwa T, Masuyama T. ACE inhibitor and angiotensin II type 1 receptor blocker differently regulate ventricular fibrosis in hypertensive diastolic heart failure. J Hypertens. 2005;23(2):393–400. https://doi.org/10.1097/00004872-200502000-00022.
Uziębło-Życzkowska B, Krzesiński P, Gielerak G, Skrobowski A. Speckle tracking echocardiography and tissue Doppler imaging reveal beneficial effect of pharmacotherapy in hypertensives with asymptomatic left ventricular dysfunction. J Am Soc Hypertens. 2017;11(6):334–42. https://doi.org/10.1016/j.jash.2017.03.009.
Tzortzis S, Ikonomidis I, Triantafyllidi H, Trivilou P, Pavlidis G, Katsanos S, Katogiannis K, Birba D, Thymis J, Makavos G, Varoudi M, Frogoudaki A, Vrettou AR, Vlastos D, Parissis J, Lekakis J. Optimal blood pressure control improves left ventricular torsional deformation and vascular function in newly diagnosed hypertensives: a 3-year follow-up study. J Cardiovasc Transl Res. 2020. https://doi.org/10.1007/s12265-019-09951-9.
Kucukler N, Kurt IH, Topaloglu C, Gurbuz S, Yalcin F. The effect of valsartan on left ventricular myocardial functions in hypertensive patients with left ventricular hypertrophy. J Cardiovasc Med (Hagerstown). 2012;13(3):181–6. https://doi.org/10.2459/JCM.0b013e3283511f00.
Motoki H, Koyama J, Izawa A, Tomita T, Miyashita Y, Takahashi M, Ikeda U. Impact of azelnidipine and amlodipine on left ventricular mass and longitudinal function in hypertensive patients with left ventricular hypertrophy. Echocardiography. 2014;31(10):1230–8. https://doi.org/10.1111/echo.12548.
Bamaiyi AJ, Norton GR, Peterson V, Libhaber CD, Sareli P, Woodiwiss AJ. Limited contribution of left ventricular mass and remodelling to the impact of blood pressure on diastolic function in a community sample. J Hypertens. 2019;37(6):1191–9. https://doi.org/10.1097/HJH.0000000000002051.
Tadic M, Cuspidi C. The effect of antihypertensive therapy on left ventricular longitudinal strain: missing part of the puzzle. J Cardiovasc Transl Res. 2020. https://doi.org/10.1007/s12265-020-09970-x.
Acknowledgements
Authors thank Damanhour University and Tanta University for supporting our study. Authors also thank medical staff members of Cardiology Department, Tanta University Hospital, Egypt, for their help in collecting patient’s data and samples for analysis.
Author information
Authors and Affiliations
Contributions
IK and LK performed eligibility assessment, participant selection, enrolment, echocardiographic study and collection of clinical data. RW performed statistical analysis of collected data, performed biomarker laboratory investigation of collected samples. All authors shared in literature reviewing, study design construction, wrote and revised the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declares that there is no conflict of interest.
Ethical Approval
The study protocol was approved by Institutional Ethic Committee and was registered in ClinicalTrials.gov with Code No: NCT03990480. All procedures agreed with the Declaration of Helsinki.
Informed Consent
Written informed consent was obtained from all participants.
Rights and permissions
About this article
Cite this article
Khairat, I., Khedr, L. & Werida, R. Valsartan Versus Amlodipine Effect on Left Ventricular Multidirectional Deformation and Adipocytokines Levels in Hypertensive Patients: Speckle Tracking Echocardiography. High Blood Press Cardiovasc Prev 27, 379–388 (2020). https://doi.org/10.1007/s40292-020-00398-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40292-020-00398-7