Abstract
Objectives
Research is lacking on the impacts of exposure to particulate matter (PM) and air pollution on patients with chronic obstructive pulmonary disease (COPD) or asthma. Therefore, we investigate the effects of various air pollution factors on hospitalization for asthma and COPD.
Methods
We obtained data on pollutants—PM10, PM2.5, carbon monoxide (CO), ozone (O3), nitrogen dioxide (NO2), and sulfur dioxide (SO2)—in Gyeonggi-do, South Korea. We also extracted data from Korean National Health Insurance records and investigated asthma and COPD attacks that required hospitalization from January 2007 through February 2018. We used generalized additive models with Poisson distribution and log transformation to calculate adjusted risk. A time-stratified case-crossover design was used, and conditional logistic regression was performed to analyze these data.
Results
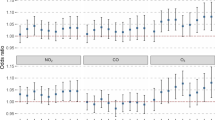
Per-unit increases in concentrations of PM10, PM2.5, SO2, NO2, CO, and O3 on different best lag days were associated with increased risks for hospital admission for COPD and asthma. SO2 had the strongest effect on hospital admission for asthma (odds ratio [OR], 1.535; 95 % confidence interval [CI], 1.450–1.619). SO2 also had the strongest effect on hospital admission for COPD (OR, 1.659; 95 % CI, 1.541–1.786). Subgroup analyses showed that these relationships were stronger in seniors (≥ 65 years old) and women with asthma than in men and nonseniors with COPD.
Conclusions
Short-term exposure to PM10, PM2.5, CO, O3, NO2, and SO2 may result in hospitalization for asthma and COPD. Of these pollutants, SO2 has the strongest effects. Therefore, patients with COPD and asthma should be cautioned against performing outdoor activities when SO2 levels are high.
Similar content being viewed by others
References
Dominici F, Peng RD, Bell ML, et al. Fine particulate air pollution and hospital admission for cardiovascular and respiratory diseases. JAMA. 2006;295:1127–34.
Künzli N, Kaiser R, Medina S, et al. Public-health impact of outdoor and traffic-related air pollution: a European assessment. Lancet. 2000;356:795–801.
Lim SS, Vos T, Flaxman AD, et al. A comparative risk assessment of burden of disease and injury attributable to 67 risk factors and risk factor clusters in 21 regions, 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet. 2012;380:2224–60.
Oudin A, Strömberg U, Jakobsson K, et al. Estimation of short-term effects of air pollution on stroke hospital admissions in southern Sweden. Neuroepidemiology. 2010;34:131–42.
Wellenius GA, Schwartz J, Mittleman MA. Particulate air pollution and hospital admissions for congestive heart failure in seven United States cities. Am J Cardiol. 2006;97:404–8.
Ni L, Chuang CC, Zuo L. Fine particulate matter in acute exacerbation of COPD. Front Physiol. 2015;6:294.
Jo YS, Lim MN, Han YJ, et al. Epidemiological study of PM(2.5) and risk of COPD-related hospital visits in association with particle constituents in Chuncheon, Korea. Int J Chron Obstruct Pulmon Dis. 2018;13:299–307.
Lee JT, Son JY, Cho YS. Benefits of mitigated ambient air quality due to transportation control on childhood asthma hospitalization during the 2002 summer Asian games in Busan, Korea. J Air Waste Manag Assoc. 2007;57:968–73.
Lee JT, Kim H, Song H, et al. Air pollution and asthma among children in Seoul Korea. Epidemiology. 2002;13:481–4.
Kim SY, O’Neill MS, Lee JT, et al. Air pollution, socioeconomic position, and emergency hospital visits for asthma in Seoul, Korea. Int Arch Occup Environ Health. 2007;80:701–10.
Jo EJ, Lee WS, Jo HY, et al. Effects of particulate matter on respiratory disease and the impact of meteorological factors in Busan, Korea. Respir Med. 2017;124:79–87.
Lee JT, Kim H, Cho YS, et al. Air pollution and hospital admissions for ischemic heart diseases among individuals 64 + years of age residing in Seoul, Korea. Arch Environ Health. 2003;58:617–23.
Park JW, Lim YH, Kyung SY, et al. Effects of ambient particulate matter on peak expiratory flow rates and respiratory symptoms of asthmatics during Asian dust periods in Korea. Respirology. 2005;10:470–6.
Hwang SH, Lee JY, Yi SM, et al. Associations of particulate matter and its components with emergency room visits for cardiovascular and respiratory diseases. PLoS One. 2017;12:e0183224.
Stanek LW, Brown JS, Stanek J, et al. Air pollution toxicology–a brief review of the role of the science in shaping the current understanding of air pollution health risks. Toxicol Sci. 2011;120(Suppl 1):8–27.
Falcon-Rodriguez CI, Osornio-Vargas AR, Sada-Ovalle I, et al. Aeroparticles, composition, and lung diseases. Front Immunol. 2016;7:3.
Guarnieri M, Balmes JR. Outdoor air pollution and asthma. Lancet. 2014;383:1581–92.
Amâncio CT, Nascimento LF. Asthma and ambient pollutants: a time series study. Rev Assoc Med Bras (1992) 2012;58:302-7.
Park M, Luo S, Kwon J, et al. Effects of air pollution on asthma hospitalization rates in different age groups in metropolitan cities of Korea. Air Qual Atmos Health. 2013;6:559–65.
Masiol M, Agostinelli C, Formenton G, et al. Thirteen years of air pollution hourly monitoring in a large city: potential sources, trends, cycles and effects of car-free days. Sci Total Environ. 2014;494–495:84–96.
Auerbach A, Hernandez ML. The effect of environmental oxidative stress on airway inflammation. Curr Opin Allergy Clin Immunol. 2012;12:133–9.
Brugha R, Grigg J. Urban air pollution and respiratory infections. Paediatr Respir Rev. 2014;15:194–9.
Esposito S, Tenconi R, Lelii M, et al. Possible molecular mechanisms linking air pollution and asthma in children. BMC Pulm Med. 2014;14:31.
Bowatte G, Lodge C, Lowe AJ, et al. The influence of childhood traffic-related air pollution exposure on asthma, allergy and sensitization: a systematic review and a meta-analysis of birth cohort studies. Allergy. 2015;70:245–56.
Samet JM, Zeger SL, Dominici F, et al. The national morbidity, mortality, and air pollution study. Part II: Morbidity and mortality from air pollution in the United States. Res Rep Health Eff Inst. 2000;94:5–70 discussion 1–9.
Gasana J, Dillikar D, Mendy A, et al. Motor vehicle air pollution and asthma in children: a meta-analysis. Environ Res. 2012;117:36–45.
Barone-Adesi F, Dent JE, Dajnak D, et al. Long-term exposure to primary traffic pollutants and lung function in children: cross-sectional study and meta-analysis. PLoS One. 2015;10:e0142565.
Zheng XY, Ding H, Jiang LN, et al. Association between air pollutants and asthma emergency room visits and hospital admissions in time series studies: a systematic review and meta-analysis. PLoS One. 2015;10:e0138146.
Zhang S, Li G, Tian L, et al. Short-term exposure to air pollution and morbidity of COPD and asthma in East Asian area: A systematic review and meta-analysis. Environ Res. 2016;148:15–23.
Sunyer J, Spix C, Quénel P, et al. Urban air pollution and emergency admissions for asthma in four European cities: the APHEA Project. Thorax. 1997;52:760–5.
Author information
Authors and Affiliations
Contributions
All authors contributed conception, analysis, interpretation, revising, and final approval of the manuscript. CH Han served as a principal investigator and had full access to all of the data in the study. JH Chung take responsibility for the integrity of the data and the accuracy of the data analysis.
Corresponding author
Ethics declarations
Conflict of interest
This work was supported by the National Health Insurance Ilsan Hospital grant (NHIMC-2019-11-019).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Chang Hoon Han and Haeyong Pak contributed equally to this work as co-first authors.
Rights and permissions
About this article
Cite this article
Han, C.H., Pak, H. & Chung, J.H. Short-term effects of exposure to particulate matter and air pollution on hospital admissions for asthma and chronic obstructive pulmonary disease in Gyeonggi-do, South Korea, 2007–2018. J Environ Health Sci Engineer 19, 1535–1541 (2021). https://doi.org/10.1007/s40201-021-00709-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40201-021-00709-7