Abstract
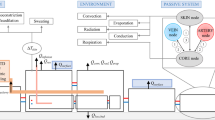
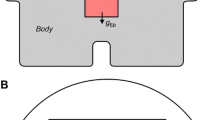
Ischaemic stroke is a major public health issue in both developed and developing nations. Hypothermia is believed to be neuroprotective in cerebral ischaemia. Conversely, elevated brain temperature is associated with poor outcome after ischaemic stroke. Mechanisms of heat exchange in normally-perfused brain are relatively well understood, but these mechanisms have not been studied as extensively during focal cerebral ischaemia. A finite element model (FEM) of heat exchange during focal ischaemia in the human brain was developed, based on the Pennes bioheat equation. This model incorporated healthy (normally-perfused) brain tissue, tissue that was mildly hypoperfused but not at risk of cell death (referred to as oligaemia), tissue that was hypoperfused and at risk of death but not dead (referred to as penumbra) and tissue that had died as a result of ischaemia (referred to as infarct core). The results of simulations using this model were found to match previous in-vivo temperature data for normally-perfused brain. However, the results did not match what limited data are available for hypoperfused brain tissue, in particular the penumbra, which is the focus of acute neuroprotective treatments such as hypothermia. These results suggest that the assumptions of the Pennes bioheat equation, while valid in the brain under normal circumstances, are not valid during focal ischaemia. Further investigation into the heat exchange profiles that do occur during focal ischaemia may yield results for clinical trials of therapeutic hypothermia.




Similar content being viewed by others
References
Bernard SA et al (2002) Treatment of comatose survivors of out-of-hospital cardiac arrest with induced hypothermia. New Engl J Med 346(8):557
van der Worp HB et al (2014) EuroHYP-1: European multicenter, randomized, phase III clinical trial of therapeutic hypothermia plus best medical treatment vs. best medical treatment alone for acute ischemic stroke. Int J Stroke 9(5):642–645
Childs C et al (2007) Determination of regional brain temperature using proton magnetic resonance spectroscopy to assess brain-body temperature differences in healthy human subjects. Magn Reson Med 57(1):59–66
Powers WJ (2008) Imaging preventable infarction in patients with acute ischemic stroke. AJNR: Am J Neuroradiol 29(10):1823–1825
Heiss WD, Sobesky J, Hesselmann V (2004) Identifying thresholds for penumbra and irreversible tissue damage. Stroke 35(11 Suppl 1):2671–2674
Hemmen T, Lyden P (2009) Hypothermia after Acute Ischemic Stroke. J Neurotrauma 26(3):387
Pennes HH (1948) Analysis of tissue and arterial blood temperatures in the resting human forearm. J Appl Physiol 85(1):5–34
Chen MM, Holmes KR (1980) MICROVASCULAR CONTRIBUTIONS IN TISSUE HEAT TRANSFER. Ann N Y Acad Sci 335(1):137–150
Dennis BH et al (2004) Finite-Element Simulation of Cooling of Realistic 3-D Human Head and Neck. J Biomech Eng 125(6):832–840
Collins CM et al (2004) Model of local temperature changes in brain upon functional activation. J Appl Physiol 97(6):2051–2055
Keller E et al (2009) Theoretical evaluations of therapeutic systemic and local cerebral hypothermia. J Neurosci Methods 178(2):345–349
Diao C, Zhu L, Wang H (2003) Cooling and Rewarming for Brain Ischemia or Injury: theoretical analysis. Ann Biomed Eng 31(3):346–353
Boller M et al (2010) Feasibility of intra-arrest hypothermia induction: a novel nasopharyngeal approach achieves preferential brain cooling. Resuscitation 81(8):1025–1030
Slotboom J et al (2004) Locally induced hypothermia for treatment of acute ischaemic stroke: a physical feasibility study. Neuroradiology 46(11):923–934
Konstas AA et al (2007) A theoretical model of selective cooling using intracarotid cold saline infusion in the human brain. J Appl Physiol 102(4):1329–1340
Bivard A et al (2011) Defining the extent of irreversible brain ischemia using perfusion computed tomography. Cerebrovasc Dis 31(3):238–245
Sukstanskii AL, Yablonskiy DA (2007) Theoretical limits on brain cooling by external head cooling devices. Eur J Appl Physiol 101(1):41–49
Kiyatkin EA (2010) Brain temperature homeostasis: physiological fluctuations and pathological shifts. Front Biosci 15:73–92
Zhu L, Diao C, Theoretical simulation of temperature distribution in the brain during mild hypothermia treatment for brain injury. Med Biol Eng Comput 39(6):681–687
Powers WJ et al (1985) Cerebral blood flow and cerebral metabolic rate of oxygen requirements for cerebral function and viability in humans. J Cereb Blood Flow Metab 5(4):600–608
Harukuni I et al (2006) Mechanisms of brain injury after global cerebral ischemia. Neurol Clin 24(1):1–21
Sun Z et al (2012) Differential temporal evolution patterns in brain temperature in different ischemic tissues in a monkey model of middle cerebral artery occlusion. J Biomed Biotechnol 2012:8
Shulman RG, Rothman DL (eds) (2004) Brain energetics and neuronal metabolism: applications to fMRI and medicine. Wiley, Chichester, p 334
Powers WJ, Zazulia AR (2003) The use of positron emission tomography in cerebrovascular disease. Neuroimaging Clin N Am 13(4):741–758
Karaszewski B et al (2013) Relationships between brain and body temperature, clinical and imaging outcomes after ischemic stroke. J Cereb Blood Flow Metab 33(7):1083–1089
Thrippleton MJ et al (2014) Reliability of MRSI brain temperature mapping at 1.5 and 3 T. NMR Biomed 27(2):183–190
Liebeskind DS (2003) Collateral circulation. Stroke 34(9):2279–2284
Liebeskind DS (2007) Understanding blood flow: the other side of an acute arterial occlusion. Int J Stroke 2(2):118–120
Bivard A et al (2014) Defining acute ischemic stroke tissue pathophysiology with whole brain CT perfusion. J Neuroradiol 41(5):307–315
Bivard A et al (2013) Perfusion CT in acute stroke: a comprehensive analysis of infarct and penumbra. Radiology 267(2):543–550
Liebeskind DS (2010) Recanalization and reperfusion in acute ischemic stroke. F1000 Med Rep 2:71
Dexter F, Hindman BJ (1994) Computer simulation of brain cooling during cardiopulmonary bypass. Ann Thorac Surg 57(5):1171–1178
Elwassif MM et al. (2006) Bio-heat transfer model of deep brain stimulation induced temperature changes. Conference Proceedings: Annual International Conference of the IEEE Engineering in Medicine & Biology Society 1:3580–3583
Neimark MA et al. (2007) The role of intracarotid cold saline infusion on a theoretical brain model incorporating the circle of willis and cerebral venous return. In: Conference proceedings: annual international conference of the IEEE engineering in medicine & biology society, vol 2007. pp 1140–1143
Neimark MA et al. (2007) Local control of temperature in a theoretical human model of selective brain cooling. In: Conference proceedings: annual international conference of the IEEE engineering in medicine biology society, vol 2007. pp 6349–6352
Nelson DA, Nunneley SA (1998) Brain temperature and limits on transcranial cooling in humans: quantitative modeling results. Eur J Appl Physiol Occup Physiol 78(4):353–359
Van Leeuwen G.M.J. et al (2000) Numerical modeling of temperature distributions within the neonatal head. Pediatr Res 48(3):351–356
Funding
This study did not receive any direct funding. Dr Lillicrap received an Australian Postgraduate Award PhD scholarship through the Australian National University during the conduction of this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This study does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Lillicrap, T., Tahtalı, M., Neely, A. et al. A model based on the Pennes bioheat transfer equation is valid in normal brain tissue but not brain tissue suffering focal ischaemia. Australas Phys Eng Sci Med 40, 841–850 (2017). https://doi.org/10.1007/s13246-017-0595-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13246-017-0595-6