Abstract
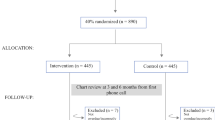
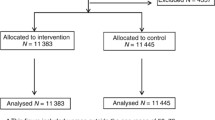
The optimal form of outreach to promote repeated, on time screening mammograms in primary care has not been established. The purpose of this study is to assess the implementation process and process outcomes for three interventions for promoting biannual screening mammography in a randomized trial. In a large urban primary care practice over a 4-year period, we randomized women aged 40–85 and eligible for mammograms to three interventions: reminder letter only (LO), reminder letter + reminder call (RC), and reminder letter + counseling call (CC). We tracked information system development, staff training, patient and provider recruitment, reach, dose delivered and received, fidelity, and context measures. Ninety-three of 95 providers approved participation by 80% (23,999) of age-eligible patients, of whom only 207 (0.9%) opted not to receive any intervention. Of 9161 initial reminder letters mailed to women coming due or overdue for mammograms, 0.8% were undeliverable. Of women in the RC and CC arms unresponsive to the first reminder letter (n = 3982), 71.4% were called and reached, and of those, 49.1% scheduled a mammogram. Only 33.4% of women reached in the CC arm received full counseling, and women in the CC arm were less likely to schedule a mammogram than those in the RC arm. Implementing mail and telephone mammography reminders is feasible and acceptable in a large urban practice and reaches a majority of patients. Many schedule a mammogram when reached. A reminder letter followed by a simple reminder call if needed may be the optimal approach to promoting screening mammograms.




Similar content being viewed by others
References
http://www.cancer.org/treatment/understandingyourdiagnosis/examsandtestdescriptions/mammogramsandotherbreastimagingprocedures/mammograms-and-other-breast-imaging-procedures-types-of-mammograms Accessed 30 July 2015.
https://www.cdc.gov/brfss/brfssprevalence/. Accessed 19 July 2015.
http://www.healthypeople.gov/2020/topics-objectives/topic/cancer/objectives Accessed 30 July 2015.
Halabi, S., Skinner, C. S., Samsa, G. P., Strigo, T. S., Crawford, Y. S., & Rimer, B. K. (2000). Factors associated with repeat mammography screening. The Journal of Family Practice , 49, 1104–1112.
Mandelblatt, J. S., Cronin, K. A., Bailey, S., Berry, D. A., et al. (2009). Breast Cancer Working Group of the Cancer Intervention and Surveillance Modeling Network (CISNET). Effects of mammography screening under different screening schedules: model estimates of potential benefits and harms. Annals of Internal Medicine, 151, 738–747.
Mandelblatt, J. S., Cronin, K. A., Berry, D. A., et al. (2011). Modeling the impact of population screening on breast cancer mortality in the United States. Breast , 20(Suppl 3), S75–S81. doi:10.1016/S0960-9776(11)70299-5.
van Ravesteyn, N. T., Heijnsdijk, E. A., Draisma, G., & de Koning, H. J. (2011). Prediction of higher mortality reduction for the UK Breast Screening Frequency Trial: a model-based approach on screening intervals. British Journal of Cancer, 105, 1082–1088.
Graham Moore, G., Audrey, S., Barker, M., Bond, L., et al. (2014). Process evaluation in complex public health intervention studies: the need for guidance. Journal of Epidemiology and Community Health, 68, 590.
Linnan, L., & Steckler, A. (2002). Process evaluation for public health interventions and research: an overview. In A. Steckler & L. Linnan (Eds.), Process evaluation for public health interventions and research (pp. 1–23). San Francisco: Published by Josey-Bass A Wiley Imprint.
Costanza, M.E., Luckmann, R., White, M.J., Rosal, M.C., Cranos, C., Reed, G., Clark, R., Sama, S., Yood, R. (2011). Design and methods for a randomized clinical trial comparing three outreach efforts to improve screening mammography adherence. BMC Health Services Research, 11, 145.
Weinstein, N. D., & Sandman, P. M. (1992). A model of the precaution adoption process: evidence from home radon testing. Health Psychology, 11, 170–180.
Costanza, M. E., Stoddard, A. M., Luckmann, R., White, M. J. P., Avrunin, J. S., & Clemow, L. (2000). Promoting mammography: a randomized trial of telephone counseling and a medical practice intervention. American Journal of Preventive Medicine, 19, 39–46.
Luckmann, R., Savageau, J. A., Clemow, L., Stoddard, A. M., & Costanza, M. E. (2003). A randomized trial of telephone counseling to promote screening mammography in two HMOs. Cancer Detection and Prevention, 27, 442–450.
White, M. J., Stark, J. R., Luckmann, R., Rosal, M. C., Clemow, L., & Costanza, M. E. (2006). Implementing a computer-assisted telephone interview (CATI) system to increase colorectal cancer screening: a process evaluation. Patient Education and Counseling, 61, 419–428.
Costanza, M. E., Luckmann, R., Stoddard, A. M., White, M. J., Stark, J. R., Avrunin, J. S., Rosal, M. C., & Clemow, L. (2007). Using tailored telephone counseling to accelerate the adoption of colorectal cancer screening. Ca Detect Prev, 31(3), 191–198.
Rubak, S., Sandbek, A., Lauritzen, T., Christensen, B. (2005). Motivational interviewing: a systematic review and meta-analysis. The British Journal of General Practice, 55 305–312.
http://masshealthpolicyforum.brandeis.edu/forums/Documents/Issue%20Brief_ConnorCenter.pd Accessed 30 Jan 2015.
http://www.hhs.gov/healthcare/rights/ Accessed 30 Jan 2015.
Rakowski, W., Lipkus, I. M., Clark, M. A., Rimer, B. K., Ehrich, B., Lyna, P. R., & Kornguth, P. J. (2003). Reminder letter, tailored stepped-care, and self-choice comparison for repeat mammography. American Journal of Preventive Medicine, 25, 308–314.
Hegenscheid, K., Hoffmann, W., Fochler, S., Domin, M., Weiss, S., Hartmann, B., Bick, U., & Hosten, N. (2011). Telephone counseling and attendance in a national mammography-screening program a randomized controlled trial. American Journal of Preventive Medicine, 41, 421–427.
Gierisch, J. M., DeFrank, J. T., Bowling, J. M., Rimer, B. K., Matuszewski, J. M., Farrell, D., & Skinner, C. S. (2010). Finding the minimal intervention needed for sustained mammography adherence. American Journal of Preventive Medicine, 39, 334–344.
Page, A., Morrell, S., Chiu, C., Taylor, R., & Tewson, R. (2006). State Co-ordination Unit Recruitment to mammography screening: a randomized trial and meta-analysis of invitation letters and telephone calls. Australian and New Zealand Journal of Public Health, 30, 111–118.
Acknowledgements
We thank Devi Sundaresan for her data management support and Kathleen Allain, Ariel Berk, Meaghan Fair, Belinda James, Brenda Kniskem, and Kathleen Matthews for their assistance in implementing the intervention programs. We thank the RMG Information Services leadership and staff for their dedication to meeting our challenging IT needs and the RMG and FCHP administration for providing access to their systems and patients.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
• The findings reported have not been previously published and this manuscript is not being simultaneously submitted elsewhere.
• The authors have full control of all primary data and agree to allow the journal to review their data if requested.
• There are no actual or potential conflicts of interest with the organization that sponsored the research.
• This work was supported by Grant R01CA132935 from the National Cancer Institute.
• All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
• Informed consent was obtained from all individual participants included in the study. The informed consent process was involved passive consent as stated in the manuscript.
• The study was approved by the Reliant Medical Group/Fallon Health Institutional Review Board (IRB).
Additional information
Implications
Practice: In populations with high rates of mammography adherence, outreach calls that involve only the offer to schedule a mammogram may be as or more effective in scheduling patients than more complex counseling calls.
Policy: Policies are needed to incentivize the development of low-cost, interoperable information systems to support outreach in primary care.
Research: Research is needed to identify effective approaches for increasing patient response to primary care outreach efforts, such as publicizing and seeking patient buy-in to outreach programs.
About this article
Cite this article
Luckmann, R., White, M.J., Costanza, M.E. et al. Implementation and process evaluation of three interventions to promote screening mammograms delivered for 4 years in a large primary care population. Behav. Med. Pract. Policy Res. 7, 547–556 (2017). https://doi.org/10.1007/s13142-017-0497-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13142-017-0497-x