Abstract
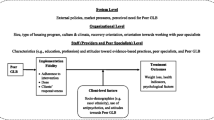
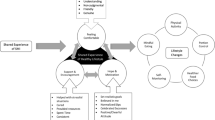
Overweight and obesity disproportionally impact people with serious mental illness (SMI). Healthy lifestyle interventions can improve the health of people with SMI but may need to be adapted for this population. The aims of this study were: to (1) examine the feasibility and acceptability of delivering the Peer-based Group Lifestyle Balance (PGLB) intervention and (2) describe intervention adaptations for people with SMI in supportive housing. Peer specialists and social workers co-facilitated 12 weekly PGLB sessions for 14 supportive housing clients. We conducted structured interviews and collected qualitative data through field notes and two focus groups. Frequencies and measures of central tendencies were used to describe participant characteristics and PGLB feasibility and acceptability measures. Qualitative data was analyzed using directed content analysis. Participants on average attended 8 of 12 sessions, and reported that services were satisfactory and helpful. Intervention adaptations, ongoing throughout the study, focused on adding peer-specialists as co-facilitators, increasing individualized support and developing strategies to address socioeconomic barriers impacting participants’ ability to engage in healthy lifestyle changes. Study findings suggest that participants with SMI in supportive housing perceived PGLB as feasible and acceptable. Expanding the relevance and reach of peer-based healthy lifestyle interventions in community settings serving people with SMI requires careful adaptations to the socioeconomic realities of this population and the complexities of living with co-morbid health and mental health conditions.
Similar content being viewed by others
References
Allison, D. B., Newcomer, J. W., Dunn, A. L., et al. (2009). Obesity among those with mental disorders: a National Institute of Mental Health meeting report. Am J Prev Med, 36(4), 341–350.
Daumit, G. L., Goldberg, R. W., Anthony, C., et al. (2005). Physical activity patterns in adults with severe mental illness. J Nerv Ment Dis, 193(10), 641–646.
Newcomer, J. W., & Hennekens, C. H. (2007). Severe mental illness and risk of cardiovascular disease. J Am Med Assoc, 298(15), 1794–1796.
Knowler, W. C., Barrett-Connor, E., & Fowler, S. E. (2002). Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med, 346(6), 393–403.
Cabassa, L. J., Ezell, J. M., & Lewis-Fernandez, R. (2010). Lifestyle interventions for adults with serious mental illness: a systematic literature review. Psychiatr Serv, 61(8), 774–782. doi:10.1176/appi.ps.61.8.774.
Cabassa, L. J., Stefancic, A., O’Hara, K., et al. (2015). Peer-led healthy lifestyle program in supportive housing: study protocol for a randomized controlled trial. Trials, 16, 388. doi:10.1186/s13063-015-0902-z.
Davidson, L., Chinman, M., Sells, D., & Rowe, M. (2006). Peer support among adults with serious mental illness: a report from the field. Schizophr Bull, 32(3), 443–450. doi:10.1093/schbul/sbj043.
Lorig, K., Ritter, P. L., Villa, F. J., & Armas, J. (2009). Community-based peer-led diabetes self-management: a randomized trial. Diabetes Education, 35(4), 641–651.
Chinman, M., George, P., Dougherty, R. H., et al. (2014). Peer support services for individuals with serious mental illnesses: assessing the evidence. Psychiatr Serv, 65(4), 429–441.
Peer Providers. SAMHSA-HRSA Center for Integrated Health Solutions Web Site.http://www.integration.samhsa.gov/workforce/team-members/peer-providers. Accessed September 7, 2016
Rosenthal, E. L., Brownstein, J. N., Rush, C. H., et al. (2010). Community health workers: part of the solution. Health Aff, 29(7), 1338–1342. doi:10.1377/hlthaff.2010.0081.
Campbell, M., Fitzpatrick, R., Haines, A., et al. (2000). Framework for design and evaluation of complex interventions to improve health. Br Med J, 321(7262), 694–696.
U.S. Department of Housing and Urban Development. The 2013 Annual Homeless Assessment Report to Congress. https://www.hudexchange.info/resources/documents/ahar-2013-part1.pdf. Accessed September 7, 2016.
Henwood, B. F., Cabassa, L. J., Craig, C. M., & Padgett, D. K. (2013). Permanent supportive housing: addressing homelessness and health disparities? Am J Public Health, 103(S2), S188–S192.
Cabassa, L. J., Parcesepe, A., Nicasio, A., Baxter, E., Tsemberis, S., & Lewis-Fernandez, R. (2013). Health and wellness photovoice project: engaging consumers with serious mental illness in health care interventions. Qual Health Res, 23(5), 618–630. doi:10.1177/1049732312470872.
Tsemberis, S., Gulcur, L., & Nakae, M. (2004). Housing first, consumer choice, and harm reduction for homeless individuals with a dual diagnosis. Am J Public Health, 94(4), 651–656.
Zayas, L. H., Cabassa, L. J., & Pérez, M. C. (2005). Capacity-to-consent in psychiatric research: development and preliminary testing of a screening tool. Res Soc Work Pract, 15(16), 545–556.
Palmer, R. M., & Meldon, S. W. (2003). Acute care. In W. R. Hazzard (Ed.), Principles of Geriatric Medicine and Gerontology (5th ed., pp. 157–168). Boston, MA: McGraw-Hill.
Kramer, M. K., Kriska, A. M., Venditti, E. M., et al. (2009). Translating the diabetes prevention program: a comprehensive model for prevention training and program delivery. Am J Prev Med, 37(6), 505–511. doi:10.1016/j.amepre.2009.07.020.
Ali, M. K., Echouffo-Tcheugui, J., & Williamson, D. F. (2012). How effective were lifestyle interventions in real-world settings that were modeled on the diabetes prevention program? Health Aff, 31, 67–75.
Roberts, R., Atkinson, C., & Mendías, R. (1984). Assessing the client satisfaction questionnaire in English and Spanish. Hisp J Behav Sci, 6, 385–395.
Venditti, E. M., & Kramer, M. K. (2012). Necessary components for lifestyle modification interventions to reduce diabetes risk. Current Diabetes Report, 12(2), 138–146. doi:10.1007/s11892-012-0256-9.
Hsieh, H. F., & Shannon, S. E. (2005). Three approaches to qualitative content analysis. Qual Health Res, 15(9), 1277–1288.
Fereday, J., & Muir-Cochrane, E. (2006). Demonstrating rigor using thematic analysis: a hybrid approach of inductive and deductive coding and theme development. International Journal of Qualitative Methods, 5, 80–92.
Padgett, DK Qualitative Methods in Social Work Research: Challenges and Rewards. 2nd ed. Thousand Oaks, CA: Sage; 2008.
Kreyenbuhl, J., Nossel, I. R., & Dixon, L. B. (2009). Disengagement from mental health treatment among individuals with schizophrenia and strategies for facilitating connections to care: a review of the literature. Schizophr Bull, 35(4), 696–703. doi:10.1093/schbul/sbp046.
Aschbrenner, K. A., Naslund, J. A., Shevenell, M., Mueser, K. T., & Bartels, S. J. (2015). Feasibility of behavioral weight loss treatment enhanced with peer support and mobile health technology for individuals with serious mental illness. Psychiatry Q, 87, 401–415. doi:10.1007/s11126-015-9395-x.
Druss, B. G., Zhao, L., von Esenwein, S. A., et al. (2010). The Health and Recovery Peer (HARP) Program: a peer-led intervention to improve medical self-management for persons with serious mental illness. Schizophr Res, 118(1–3), 264–270. doi:10.1016/j.schres.2010.01.026.
Schneider, K. L., Sullivan, J. C., & Pagoto, S. L. (2011). Translation of the diabetes prevention program into a community mental health organization for individuals with severe mental illness: a case study. Translational Behavavioral Medicine, 1(3), 453–460. doi:10.1007/s13142-011-0053-z.
McGinty, E. E., Baller, J., Azrin, S. T., Juliano-Bult, D., & Daumit, G. L. (2015). Interventions to address medical conditions and health-risk behaviors among persons with serious mental illness: a comprehensive review. Schizophr Bull, 42(1), 96–124. doi:10.1093/schbul/sbv101.
Burke, L. E., Wang, J., & Sevick, M. A. (2011). Self-monitoring in weight loss: a systematic review of the literature. J Am Diet Assoc, 111(1), 92–102. doi:10.1016/j.jada.2010.10.008.
McKibbin, C. L., Folsom, D., Meyer, J., Sirkin, A., Loh, C., & Lindamer, L. (2008). Behavioral interventions to improve management of overweight, obesity, and diabetes in patients with schizophrenia. In D. Gallagher-Thompson, A. M. Steffen, & L. W. Thompson (Eds.), Handbook of Behavioral and Cognitive Therapies with Older Adults (pp. 171–186). New York: NY: Springer.
Daumit, G. L., Dickerson, F. B., Wang, N. Y., et al. (2013). A behavioral weight-loss intervention in persons with serious mental illness. N Engl J Med, 368(17), 1594–1602.
Drewnowski, A. (2009). Obesity, diets, and social inequalities. Nutrion Reviews, 67(Supplement 1), S36–S39. doi:10.1111/j.1753-4887.2009.00157.x.
Walker, R. E., Keane, C. R., & Burke, J. G. (2010). Disparities and access to healthy food in the United States: a review of food deserts literature. Health & Place, 16(5), 876–884. doi:10.1016/j.healthplace.2010.04.013.
Cabassa, L. J., Siantz, E., Nicasio, A., Guarnaccia, P., & Lewis-Fernandez, R. (2014). Contextual factors in the health of people with serious mental illness. Qual Health Res, 24(8), 1126–1137. doi:10.1177/1049732314541681.
Druss, B. G., von Esenwein, S. A., Compton, M. T., Rask, K. J., Zhao, L., & Parker, R. M. (2010). A randomized trial of medical care management for community mental health settings: the Primary Care Access, Referral, and Evaluation (PCARE) study. Am J Psychiatr, 167(2), 151–159.
Acknowledgements
This study was supported in part by pilot funds from the Columbia University Provost Office and a grant from the National Institute of Mental Health (R01MH104574). The content of this article is solely the responsibility of the authors and does not represent the official views of the National Institutes of Health. The authors wish to thank all of the people who participated in this study and Paola Volquez for her assistance with this project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. This study was approved by the Columbia University Institutional Review Board.
Informed consent
Informed consent was obtained from all individual participants included in the study.
The findings reported here have not been previously published nor is the manuscript being simultaneously submitted elsewhere. The authors have full control of all primary data and will agree to allow the journal to review de-identified data if requested.
Funding
This study was supported in part by pilot funds from the Columbia University Provost Office and a grant from the National Institute of Mental Health (R01MH104574).
Conflict of interest
The authors declare that they have no conflict of interest.
Statement on the welfare of animals
Not applicable since no animals were in involved this study.
Additional information
Implications
Policy: Healthy lifestyle intervention policies and programming should be responsive to cultural, geographic, and socioeconomic factors, as well as mental health concerns that may influence the engagement of people with SMI.
Research: The results of our pilot study suggest that future work should prioritize efforts to test the effectiveness of peer-based healthy lifestyle interventions that combine group and individual sessions, tailor and simplify self-monitoring strategies, and adapt intervention content and activities to the socioeconomic realities of people with SMI.
Practice: Healthy lifestyle interventions represent a promising component of a holistic approach to improve the physical health of people with SMI.
About this article
Cite this article
O’Hara, K., Stefancic, A. & Cabassa, L.J. Developing a peer-based healthy lifestyle program for people with serious mental illness in supportive housing. Behav. Med. Pract. Policy Res. 7, 793–803 (2017). https://doi.org/10.1007/s13142-016-0457-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13142-016-0457-x