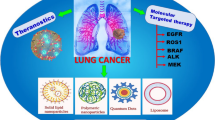
Summary
Lung cancer is still one of the most common cancer entities worldwide and the leading cause of cancer mortality. Despite significant advances in the diagnosis and therapy of lung cancer, many patients do not respond to existing therapies, indicating an urgent need for the development of novel treatment strategies. In recent years, nanotechnology has led to significant progress in modern medicine. Especially lipid nanoparticles (LNPs) evoked substantial interest, due to their broad application as coronavirus disease 2019 (COVID-19) vaccines. In the future of lung cancer treatment, lipid nanoparticles hold the potential to provide specific, safe, and well-tolerated treatments by incorporating multiple drugs and targeting agents and enabling their trafficking to tissues or cell types of interest. This review briefly summarizes the application of LNPs in lung cancer treatment as well as their future possibilities.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lung cancer is the second most common cancer worldwide and the leading cause of cancer-related deaths [1]. Despite numerous improvements in lung cancer therapy, such as targeted therapy or immunotherapy, drug resistance leading to tumor progression and disease recurrence is an enormous clinical challenge [2]. Apart from that, the tumor microenvironment, including abnormal blood vessel formation, tumor hypoxia and tumor acidity, makes it difficult for therapeutics to reach their target and thus reduces their effectiveness [3]. As most of the systemic therapeutic approaches are not cancer cell selective and therefore induce side effects on healthy tissue and the patient’s general condition, more targeted and personalized therapies are urgently needed [4].
Due to their properties and possible applications, the use of nanoparticles (NPs) in the treatment of lung cancer could be one way to achieve this goal and overcome the restrictions of conventional therapy approaches. NPs, covering a size range of 1 to 100 nm, are used as drug carriers transporting anticancer agents directly to the tumor. They hold the potential to improve the bioavailability of encapsulated drugs and also reduce the toxicity of these compounds to healthy tissues [5, 6]. Following systemic injection, nanoparticles can be eliminated from the bloodstream by the mononuclear phagocyte system (MPS), hepatobiliary elimination or urinary excretion [7].
At present, lipid nanoparticles (LNPs) are considered one of the best drug carriers for cancer therapeutics [8]. Thus, this review aims to highlight the application of LNPs in the treatment of lung cancer and discuss their future potential.
Application of lipid nanoparticles in lung cancer treatment
One nanoparticle that has already been approved for the first-line treatment of advanced non-small-cell lung cancer, is the nanoparticle albumin-bound paclitaxel (nab-paclitaxel) [9]. Nab-paclitaxel has been confirmed as a safe and effective therapy in combination with carboplatin for patients with advanced non-small-cell lung cancer [10]. Although nab-paclitaxel is superior to conventional chemotherapies in terms of toxicity, there are still some safety concerns related to albumin-based nanoparticles [11, 12].
Lipid nanoparticles, in contrast, have a quite high biocompatibility and are less toxic and immunogenic compared to other nanoparticles [13]. This results from the fact that LNPs are very small particles, mainly built by lipids and other biochemical compounds [8]. Administration routes are usually either systemic (intravenous injection) or local (e.g., intramuscular, intradermal, and subcutaneous injection), mainly depending on the therapeutic indication. For lung cancer, another possible application route of LNP-based agents is added: topical administration by direct inhalation into the lungs [14]. Current research suggests that LNPs hold the potential to serve as a safe and effective pulmonary drug delivery platform, allowing high concentrations at the desired site with less systemic toxicity [15].
The current relevance of LNPs in the therapy of solid tumors, including lung cancer, also becomes evident when looking at the accepted and published abstracts at the ASCO (American Society of Clinical Oncology) Annual Meeting and the AACR (American Association for Cancer Research) Annual Meeting this year. It’s not only the high number of ongoing areas of research concerning first-in-human studies on the efficacy, safety, and dosing of different LNP-associated anticancer agents that is remarkable [16, 17], but also the forward-looking nature of the projects [18, 19].
Further clinical trials of lipid nanoparticles in the treatment of lung cancer are shown in Table 1 (search terms: lipid nanoparticles; lipid nanoparticles, cancer; lipid nanoparticles, tumor). Two of nine trials are solely focusing on non-small-cell lung cancer and one trial exclusively includes small-cell lung cancer patients in extensive stages [20].
Considering the above aspects, LNPs open up tremendous potential for future therapies and therefore may lead to a new era of lung cancer treatment.
Current advances and future directions
LNPs as drug delivery platforms are actively explored in various medical applications, including cancer immunotherapy, protein replacement therapy, vaccination, and gene editing. They are characterized by high potency, biocompatibility and the possibility of repeated administration, which facilitates clinical translation [14]. In the following, an overview of potential future applications of LNP-based cancer therapy is given. A selection of these promising treatments is illustrated in Fig. 1.
The future of lipid nanoparticles in lung cancer treatment. Lipid nanoparticles have the potential to become an essential drug delivery system in the treatment of lung cancer and may pave the way towards novel therapeutic approaches, e.g., CAR (chimeric antigen receptor) therapy, mRNA (messenger ribonucleic acid) cancer vaccines, or CRISPR/Cas9 (clustered regularly interspaced short palindromic repeats, Cas9-protein) genome editing. (Figure created in BioRender.com)
LNP-based mRNA vaccines in lung cancer
Since the coronavirus disease 2019 (COVID-19) pandemic, lipid nanoparticles are no longer a rare novelty. After their safe and effective application as LNP-based mRNA vaccines in severe acute respiratory syndrome coronavirus type 2 (SARS-CoV-2) treatment, they are an area of great promise for mRNA (messenger ribonucleic acid) cancer vaccines with the potential of broad future applications [21, 22].
Although viral-vector-based mRNA delivery has led to successful clinical outcomes, there are many restrictions such as immune responses to the virus, unwanted integration into the host genome, or the impossibility of repeated administration, all of which could be overcome by using LNP-based delivery systems [23].
LNP-based mRNA vaccines are among the leading candidates for therapeutic cancer vaccines of various solid tumors, including lung cancer. Encapsulating mRNA in LNPs protects the loaded mRNA from degradation and enables the trafficking to the cytoplasm of the targeted tumor cells [24].
At present, only few preclinical studies of LNP-based mRNA vaccines in lung cancer treatment have been carried out. However, these trials suggest the relevance of LNP-based mRNA vaccines in combination with immune checkpoint inhibitors in the treatment of non-small-cell lung cancer [22].
Recently, the approach to develop personalized neoantigen vaccines gained significant interest. Neoantigens from patient-specific tumor mutations are mostly unique to the individual patient, entirely absent from healthy tissue and induce a specific anti-tumor immune response [25]. Therefore, they are emerging targets for personalized cancer treatment, especially for patients resistant to conventional therapies.
A further promising approach is the delivery of immunostimulatory RNA molecules via LNP-based vaccine formulations. The combination of these two therapies has the potential to improve therapeutic efficacy by abrogating the immunosuppressive tumor microenvironment, leading to a next generation of cancer immunotherapy [26].
LNP-based delivery of CRISPR/Cas9 genome editing components
CRISPR/Cas (clustered regularly interspaced short palindromic repeats/Cas-protein) gene editing offers new possibilities in cancer treatment, such as the permanent inactivation of PD-L1 (programmed death-ligand 1) on tumor cells. However, tumor characteristics, like the high density of the tumor microenvironment, hamper this approach [27]. Zhang et al. overcame this obstacle by developing multiplexed LNPs loaded with tools that facilitate tumor penetration on the one hand and enable gene editing of cancer cells on the other hand, enhancing overall gene editing by greater than 10-fold in vitro [27].
Another challenge that must be addressed before the clinical implementation of LNP-based CRISPR therapies for solid tumors is the ability of specific tissue targeting. Since the liver is the primary organ of LNP accumulation, there is a need for new targets enabling the LNP delivery to therapeutically relevant cell types [28, 29].
Recently, researchers reported a strategy called selective organ targeting (SORT), in which lipid nanoparticles are systematically engineered to target specific tissues or cell types by adding an additional molecule, termed SORT. This approach is compatible with various gene editing techniques allowing tissue-specific gene delivery and editing [29]. These findings indicate that LNP-based delivery of CRIPS/Cas9 genome editing components offers enormous potential for the future of lung cancer treatment.
In vivo mRNA-LNP-based CAR therapy for solid tumors
Chimeric antigen receptor (CAR) T cell therapy is a modern and innovative cancer treatment currently used for certain blood cancers. During a complex manufacturing process, a patient’s T cells are genetically modified ex vivo to form CAR, targeting cancer-specific surface proteins. CAR‑T therapies using in vivo LNP-based mRNA delivery to T cells may provide not only time and cost savings, but also therapeutic and safety benefits for future CAR therapies. Recently, the development of CAR therapy beyond T cells tremendously evolved. Using immune cells that are more abundant in solid tumors than T cells, for instance monocytes/macrophages, may pave the way towards CAR therapies for solid malignancies, including lung cancer [26]. Combining these technologies, in vivo LNP-based CAR therapy for solid tumors might be conceivable in the future.
Conclusion and outlook
Lipid nanoparticle (LNP)-based drug delivery is a promising strategy with tremendous potential to refine the lung cancer treatment landscape and approaches. Recently, they have gained significant interest, mainly due to the widespread use of COVID-19 mRNA vaccines, which would not have been possible without LNP-based mRNA delivery. While many challenges remain in the development of safe and effective LNP-based drug delivery systems, further studies are needed to deepen our understanding of biological and chemical factors prior to broad clinical application. However, researchers assume that targeted delivery systems, such as LNPs, are likely to increase the efficacy and reduce side effects of existing therapies, e.g., immunotherapy, mRNA-based cancer vaccines or CAR therapy [22, 26].
From our perspective, major challenges regarding the clinical implementation of LNPs in lung cancer treatment are (1) identifying the target and determining druggability, (2) predicting the quality and stability of LNPs, and (3) enabling specific tissue targeting and tumor penetration.
Overall, however, we believe that LNPs have the potential to become an essential drug delivery system, overcome limitations of traditional therapeutic reagents and open new avenues for translational nanomedicine in lung cancer treatment.
References
Sung H, Ferlay J, Siegel RL, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71(3):209–49. https://doi.org/10.3322/caac.21660.
Sosa Iglesias V, Giuranno L, Dubois LJ, Theys J, Vooijs M. Drug resistance in non-small cell lung cancer: a potential for NOTCH targeting? Front Oncol. 2018;8:267. https://doi.org/10.3389/fonc.2018.00267.
Tan Q, Saggar JK, Yu M, Wang M, Tannock IF. Mechanisms of drug resistance related to the microenvironment of solid tumors and possible strategies to inhibit them. Cancer J. 2015;21(4):254–62. https://doi.org/10.1097/PPO.0000000000000131.
Maeda H, Khatami M. Analyses of repeated failures in cancer therapy for solid tumors: poor tumor-selective drug delivery, low therapeutic efficacy and unsustainable costs. Clin Transl Med. 2018;7(1):11. https://doi.org/10.1186/s40169-018-0185-6.
Miele E, Spinelli GP, Miele E, et al. Nanoparticle-based delivery of small interfering RNA: challenges for cancer therapy. Int J Nanomedicine. 2012;7:3637–57. https://doi.org/10.2147/IJN.S23696.
Pérez-Herrero E, Fernández-Medarde A. Advanced targeted therapies in cancer: drug nanocarriers, the future of chemotherapy. Eur J Pharm Biopharm. 2015;93:52–79. https://doi.org/10.1016/j.ejpb.2015.03.018.
Dilliard SA, Siegwart DJ. Passive, active and endogenous organ-targeted lipid and polymer nanoparticles for delivery of genetic drugs. Nat Rev Mater. 2023;8(4):282–300. https://doi.org/10.1038/s41578-022-00529-7.
Sheoran S, Arora S, Samsonraj R, Govindaiah P, Vuree S. Lipid-based nanoparticles for treatment of cancer. Heliyon. 2022;8(5):e9403. https://doi.org/10.1016/j.heliyon.2022.e09403.
Celgene Corporation. Abraxane® for injectable suspension (paclitaxel protein-bound particles for injectable suspension) [albumin-bound]: US prescribing information [Internet]. 2014 [cited 09 May 2023]. Available from: http://www.fda.gov/.
Socinski MA, Manikhas GM, Stroyakovsky DL, et al. A dose finding study of weekly and every-3-week nab-Paclitaxel followed by carboplatin as first-line therapy in patients with advanced non-small cell lung cancer. J Thorac Oncol. 2010;5(6):852–61. https://doi.org/10.1097/jto.0b013e3181d5e39e.
Hassanin I, Elzoghby A. Albumin-based nanoparticles: a promising strategy to overcome cancer drug resistance. Cancer Drug Resist. 2020;3(4):930–46. https://doi.org/10.20517/cdr.2020.68.
Tan H, Hu J, Liu S. Efficacy and safety of nanoparticle albumin-bound paclitaxel in non-small cell lung cancer: a systematic review and meta-analysis. Artif Cells Nanomed Biotechnol. 2019;47(1):268–77. https://doi.org/10.1080/21691401.2018.1552595.
Li Y, Lee RJ, Yu K, et al. Delivery of siRNA using lipid nanoparticles modified with cell penetrating peptide. ACS Appl Mater Interfaces. 2016;8(40):26613–21. https://doi.org/10.1021/acsami.6b09991.
Hou X, Zaks T, Langer R, Dong Y. Lipid nanoparticles for mRNA delivery. Nat Rev Mater. 2021;6(12):1078–94. https://doi.org/10.1038/s41578-021-00358-0.
Zhang H, Leal J, Soto MR, Smyth HDC, Ghosh D. Aerosolizable lipid nanoparticles for pulmonary delivery of mRNA through design of experiments. Pharmaceutics. 2020;12(11):1042. https://doi.org/10.3390/pharmaceutics12111042.
Castañón E, Zamarin D, Carneiro BA, et al. Intratumoral (IT) MEDI1191 + durvalumab (D): Update on the first-in-human study in advanced solid tumors [abstract]. In: Proceedings of the American Association for Cancer Research Annual Meeting 2023; Part 2 (Clinical Trials and Late-Breaking Research); 2023 Apr 14–19; Orlando, FL. Philadelphia (PA): AACR. Cancer Res. 2023;83(8_Suppl):Abstract nr CT4.
Tolcher A, Spira A, Nemunaitis J, et al. First-in-human dose-escalation study of NBF-006, a novel investigational siRNA targeting GSTP, in patients with non-small cell lung, pancreatic, or colorectal cancer. In: Proceedings of the American Society of Clinical Oncology Annual Meeting 2023; Poster Session (Developmental Therapeutics-Molecularly Targeted Agents and Tumor Biology; Sub Track: New Targets and New Technologies (non-IO)). 2023 June 2–6; Chicago. p. Abstract nr 3084.
Thomas A, Jain N, Nazaripour S, et al. Lipid nanoparticle library towards development next generation genomic medicines [abstract]. In: Proceedings of the American Association for Cancer Research Annual Meeting 2023; Part 1 (Regular and Invited Abstracts); 2023 Apr 14–19; Orlando, FL. Philadelphia (PA): AACR. Cancer Res. 2023;83(7_Suppl):Abstract nr 4066.
Prod’homme TE, Argueta S, Zhao H, et al. In vivo delivery of novel CD89 fusion receptor to myeloid cells by mRNA activates anti-tumor immunity [abstract]. In: Proceedings of the American Association for Cancer Research Annual Meeting 2023; Part 2 (Clinical Trials and Late-Breaking Research); 2023 Apr 14–19; Orlando, FL. Philadelphia (PA): AACR. Cancer Res. 2023;83(8_Suppl):Abstract nr LB27.
Data retrieved from US National Library of Medicine. http://clinicaltrials.gov/. Accessed 9 May 2023.
Xu K, Dai L, Gao GF. Humoral and cellular immunity and the safety of COVID-19 vaccines: a summary of data published by 21 May 2021. Int Immunol. 2021;33(10):529–40. https://doi.org/10.1093/intimm/dxab061.
Huang T, Peng L, Han Y, et al. Lipid nanoparticle-based mRNA vaccines in cancers: current advances and future prospects. Front Immunol. 2022;13:922301. https://doi.org/10.3389/fimmu.2022.922301.
Paunovska K, Loughrey D, Dahlman JE. Drug delivery systems for RNA therapeutics. Nat Rev Genet. 2022;23(5):265–80. https://doi.org/10.1038/s41576-021-00439-4.
Barbier AJ, Jiang AY, Zhang P, Wooster R, Anderson DG. The clinical progress of mRNA vaccines and immunotherapies. Nat Biotechnol. 2022;40(6):840–54. https://doi.org/10.1038/s41587-022-01294-2.
Lang F, Schrörs B, Löwer M, Türeci Ö, Sahin U. Identification of neoantigens for individualized therapeutic cancer vaccines. Nat Rev Drug Discov. 2022;21(4):261–82. https://doi.org/10.1038/s41573-021-00387-y.
Raimondo TM, Reed K, Shi D, Langer R, Anderson DG. Delivering the next generation of cancer immunotherapies with RNA. Cell. 2023;186(8):1535–40. https://doi.org/10.1016/j.cell.2023.02.031.
Zhang D, Wang G, Yu X, et al. Enhancing CRISPR/Cas gene editing through modulating cellular mechanical properties for cancer therapy. Nat Nanotechnol. 2022;17(7):777–87. https://doi.org/10.1038/s41565-022-01122-3.
Di J, Du Z, Wu K, et al. Biodistribution and non-linear gene expression of mRNA LNPs affected by delivery route and particle size. Pharm Res. 2022;39(1):105–14. https://doi.org/10.1007/s11095-022-03166-5.
Cheng Q, Wei T, Farbiak L, Johnson LT, Dilliard SA, Siegwart DJ. Selective organ targeting (SORT) nanoparticles for tissue-specific mRNA delivery and CRISPR-Cas gene editing. Nat Nanotechnol. 2020;15(4):313–20. https://doi.org/10.1038/s41565-020-0669-6.
Funding
Open access funding provided by University of Innsbruck and Medical University of Innsbruck.
Author information
Authors and Affiliations
Contributions
A. Mair and F. Nocera drafted the manuscript, A. Mair prepared the figure, A. Mair prepared the table, A. Pircher and D. Wolf critically revised the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
A. Mair, F. Nocera, D. Wolf and A. Pircher declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Mair, A., Nocera, F., Wolf, D. et al. Lipid nanoparticles in the treatment of lung cancer—hype or hope?. memo 16, 193–197 (2023). https://doi.org/10.1007/s12254-023-00904-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12254-023-00904-2