Abstract
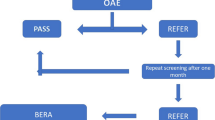
Objective to implement Universal Neonatal Hearing Screening (UNHS) in a tertiary academic hospital and identify associated risk factors. Prospective study. Screening tests with Otoacoustic Emissions (OAE) were done among newborns, prior to hospital discharge. In babies who fail OAE twice, Brain Response Audiometry (BERA) was done, failing which they were referred to higher ENT center for repeat testing and hearing rehabilitation. A total 2323 babies were admitted in the neonatal unit during the study period. Only 773 babies (a third) could be screened for the first OAE, two thirds being lost to study right at inception!! Among the 773 neonates, in the “at risk” group of 301 neonates, 31(10%) and in the “not at risk” group of 472 neonates, 30 (6%) were lost to follow up respectively. The occurrence of hearing loss in this study population was 1.3 per 1000. Risk factors were noted in 38.9% of this subgroup with occurrence of hearing loss in “at risk” group being 3.32 per 1000. The implementation of UNHS in a developing country like India, has multiple challenges including infrastructural and non-compliance to follow up. In the meantime, the possibility of compromising ‘at-risk” neonates, who are significantly more prone to hearing loss, both neonatal and delayed onset, is an additional grave reality which needs deep considerationin this Herculean task of attaining “universality”.



Similar content being viewed by others
References:
Garg S, Singh R, Khurana D (2015) Infant hearing screening in India: Current status and way forwards. Int J Prev Med 6:113
Kundu CL (2000). Status of Disability in India 2000 New Delhi: Rehabilitation Council of India, Ministry of Welfare, Government of India] In National Sample Survey Organization, Disabled Persons in India, NSS 58th Round. Report no. 485 (58/26/1), National Sample Survey Organization, Ministry of Statistics and Programme Implementation, Government of India, New Delhi 2003
DelaneyAM and Roland P.Newborn Hearing Screening: Overview, Prevalence of Hearing Loss, The High-Risk Register [Internet]. Emedicine.medscape.com. 2020 [cited 26 July 2016]. Available from: https://emedicine.medscape.com/article /836646-overview.
Sukumaran TU (2011) Newborn hearing screening program Indian paediatrics 48(5):351
Yoshinaga-Itano C, Sedey AL, Coulter DK, Mehl AL (1998) Language of early- and later-identified children with hearing loss. Pediatrics 102(5):1161–1171
Joint Committee on Infant Hearing (2007) Year 2007 position statement: principles and guidelines for early hearing detection and intervention programs. Pediatrics 120(4):898–921
Newborn and infant hearing screening: current issues and guiding principles for action. Geneva: World Health Organization; 2010. Available from: https://www.who.int/blindness/publications/Newborn_and_Infant_Hearing_Screenig. Report.pdf [cited 2018 Jul 3].
Suresh K, Arif Ali K, Mary K (2015) Challenges in the detection and intervention of childhood deafness: experience from a developing country. Int J Biomed Res 6(01):40–45
Gelfand S (2016) Audiological screening chapter 13. In: Sydor A (ed) Essentials of Audiology, 4th edn. Thieme, New York, pp 353–354
Jedrzejczak WW, Konopka W, Kochanek K, Skarzynski H (2015) Otoacoustic emissions in newborns evoked by 0.5 kHz tone bursts. Int J PediatrOtorhinolaryngol 79(9):1522–1526
Johnson LC, Toro M, Vishnja E et al (2018) Age and other factors affecting the outcome of aabr screening in neonates. HospPediatr 8(3):141–147
Directorate General of Health Services (2006) National Programme for Prevention and Control of Deafness. Project Proposal, Ministry of Health and Family Welfare, New Delhi
Kumar S, Mohapatra B (2011) Status of a newborn hearing screening program in India. Int J PediatrOtorhinolaryngol 75(1):20–26
Annual Data Early Hearing Detection and Intervention (EHDI) Program [internet]. Atlanta: Centers for Disease Control and Prevention; 2016. Available from: https://www.cdc.gov/ncbddd/hearingloss/ehdi-data2016.html [cited 2019 Jul 3].
Scheepers L, Swanepoel D, Roux T (2014) why parents refuse newborn hearing screening and default on follow-up rescreening—a south African perspective. Int J PediatrOtorhinolaryngol 78(4):652–658
Hansashree YS, Bhatt SH, Nimbalkar S, Mishra G (2018) Non-compliance with neonatal hearing screening follow-up in rural western India. Indian Pediatr 55(6):482–484
Pitathawatchai P, Khaimook W, Kirtsreesakul V (2019) Pilot implementation of newborn hearing screening programme at four hospitals in southern Thailand. Bull World Health Organ 97(10):663–671
Ravi R, Gunjawate D, Yerraguntla K, Lewis L, Driscoll C, Rajashekhar B (2016) Follow-up in newborn hearing screening – a systematic review. Int J PediatrOtorhinolaryngol 90:29–36
Cunningham M, Thomson V, McKiever E, Dickinson LM, Furniss A, Allison MA (2018) Infant, maternal and hospital factors’ role in loss to follow-up after failed newborn hearing screening. AcadPediatr 18(2):188–195. https://doi.org/10.1016/j.acap.2017.05.005Epub 2017 May 23
Kolethekkat AA, Al Abri R, HIaiwah O, AI Harasi, Sulaiman AA, AI Bahlani H, AI Jaradi M, Mathew J. Limitations and drawbacks of the hospital-based universal neonatal hearing screening program: First report from the Arabian Peninsula and insights. Int J PediatrOtorhinolaryngol. 2020, 132:109926. https://doi.org/10.1016/j.ijporl.2020.109926
Kumar P, Adhisivam B, Bhat V, Bharathi B, Francis F, Mondal N (2016) Screening for hearing loss among high risk neonates– experience from a tertiary care center. CurrPediatr Res 20(1&2):43–46
Wroblewska-Seniuk K, Greczka G, Dabrowski P, Szyfter-Harris J, Mazela J (2017) Hearing impairment in premature newborns—analysis based on the national hearing screening database in Poland. PLoS ONE. https://doi.org/10.1371/journal.pone.0184359
Nair VS, Das P, Soundararajan P (2018) Prevalence and risk factors of hearing impairment among neonates admitted in NICU in a tertiary care center in South India. Int J ContempPediatr 5(4):1342–1347
Yilmazer R, ZahideYazici M, Erdim I, Kaya H, OzcanDalbudak S, Kayhan T (2016) Follow-up results of newborns after hearing screening at a training and research hospital in Turkey. J Intl AdvOtol 12(1):55–60
Nair M, Girish S, Nair SS, Sameer P (2018) Risk factors and prevalence of hearing impairment among neonates in a South Indian Tertiary Neonatal Centre. Journal of Medical Science and Clinical Research 6(02):665–675
Parab SR, Khan MM, Kulkarni S, Ghaisas V, Kulkarni P (2018) Neonatal screening for prevalance of hearing impairment in rural areas. Indian J Otolaryngol Head Neck Surg 70(3):380–386
Butcher E, Dezateux C, Knowles R (2020) Risk factors for permanent childhood hearing impairment. Arch Dis Child 105(2):187–189. https://doi.org/10.1136/archdischild-2018-315866
Kumar A, Gupta SC, Sinha VR (2017) Universal hearing screening in newborns using otoacoustic emissions and brainstem evoked response in Eastern Uttar Pradesh. Indian J Otolaryngol Head Neck Surg 69(3):296–299
Sachdeva K, Sao T (2017) Outcomes of newborn hearing screening program: a hospital based study. Indian J Otolaryngol Head Neck Surg 69(2):194–198
Butcher E, Dezateux C, Cortina-Borja M, Knowles R (2018) Prevalence of permanent childhood hearing impairment identified by universal newborn hearing screening: a systematic review and meta-analysis. Revue d'Épidémiologieet de Santé Publique. 66:S313
Mehar V, Somani P, Singh K, Munjal VR (2015) Targeted hearing screening in newborns. Int J ContempPediatrics 3(1):159–163
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jacob, J., Kurien, M., Sindhusha et al. Challenges of Universal Newborn Hearing Screening in a Developing Country-a Double-Edged Sword. Indian J Otolaryngol Head Neck Surg 74 (Suppl 1), 395–401 (2022). https://doi.org/10.1007/s12070-020-02170-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12070-020-02170-8