Abstract
Summary
Angiotensin-converting enzyme inhibitor use in women was associated with lower femoral neck and lumbar spine bone mineral density as well as trabecular bone score compared to non-users. No differences were identified for men or for those who used ARB medications.
Purpose
Many individuals at high fracture risk use medications such as angiotensin-converting enzyme inhibitors (ACEI) or angiotensin II receptor blockers (ARB) that could affect bone; thus, this study aimed to investigate whether there are any differences in bone mineral density (BMD) and trabecular bone score (TBS) between ACEI users, ARB users, and non-users.
Methods
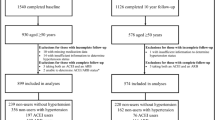
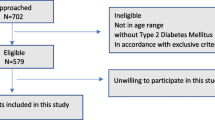
Participants (685 men, 573 women) were from the Geelong Osteoporosis Study. Current medication use was self-reported. BMD at the femoral neck (FNBMD) and lumbar spine (LSBMD) were measured using DXA. TBS was calculated using TBS iNsight software. Linear regression models were used to investigate associations between ACEI or ARB use and bone measures, adjusting for other potential confounders. Due to interaction terms, data were stratified by age.
Results
There were 88 (12.8%) men and 41 (7.2%) women taking an ACEI medication, and 71 (10.4%) men and 76 (13.3%) women taking an ARB medication. Compared to non-users, ACEI use was associated with lower FNBMD (− 7.2%), LSBMD (− 12.2%), and TBS (− 9.0%) for women aged < 65 years. Lower TBS was also observed for women aged ≥ 65 years (− 17.3%). No differences were identified for ARB use.
Conclusions
Women who used an ACEI medication had lower values for FNBMD, LSBMD and TBS compared to non-users. No differences were identified for men or for those who used ARB medications.

Similar content being viewed by others
Data availability
Data are available upon reasonable request.
References
Ghosh M, Majumdar SR (2014) Antihypertensive medications, bone mineral density, and fractures: a review of old cardiac drugs that provides new insights into osteoporosis. Endocrine 46:397–405. https://doi.org/10.1007/s12020-014-0167-4
Bislev LS, Sikjær T, Rolighed L, Rejnmark L (2015) Relationship between aldosterone and parathyroid hormone, and the effect of angiotensin and aldosterone inhibition on bone health. Clin Rev Bone Miner Metab 13:194–205. https://doi.org/10.1007/s12018-015-9182-0
Unger T, Stoppelhaar M (2007) Rationale for double renin-angiotensin-aldosterone system blockade. Am J Cardiol 100:S25–S31. https://doi.org/10.1016/j.amjcard.2007.05.011
National Heart Foundation of Australia (2016) Guideline for the diagnosis and management of hypertension in adults - 2016. Melbourne: National Heart Foundation of Australia
Tamargo J, Caballero R, Delpón E (2015) The renin–angiotensin system and bone. Clin Rev Bone Miner Metab 13:125–148. https://doi.org/10.1007/s12018-015-9189-6
Kwok T, Leung J, Zhang YF et al (2012) Does the use of ACE inhibitors or angiotensin receptor blockers affect bone loss in older men? Osteoporos Int 23:2159–2167. https://doi.org/10.1007/s00198-011-1831-7
Krieger NS, Frick KK, Bushinsky DA (2004) Mechanism of acid-induced bone resorption. Curr Opin Nephrol Hypertens 13:423–436
Asaba Y, Ito M, Fumoto T et al (2009) Activation of renin-angiotensin system induces osteoporosis independently of hypertension. J Bone Miner Res 24:241–250. https://doi.org/10.1359/jbmr.081006
Shimizu H, Nakagami H, Osako MK et al (2009) Prevention of osteoporosis by angiotensin-converting enzyme inhibitor in spontaneous hypertensive rats. Hypertens Res 32:786–790. https://doi.org/10.1038/hr.2009.99
Kang KY, Kang Y, Kim M et al (2013) The effects of antihypertensive drugs on bone mineral density in ovariectomized mice. J Korean Med Sci 28:1139–1144. https://doi.org/10.3346/jkms.2013.28.8.1139
Donmez BO, Ozdemir S, Sarikanat M et al (2012) Effect of angiotensin II type 1 receptor blocker on osteoporotic rat femurs. Pharmacol Reports 64:878–888. https://doi.org/10.1016/S1734-1140(12)70882-4
Lynn H, Kwok T, Wong SYS et al (2006) Angiotensin converting enzyme inhibitor use is associated with higher bone mineral density in elderly Chinese. Bone 38:584–588. https://doi.org/10.1016/j.bone.2005.09.011
Zhang Y, Qin L, Leung P, Kwok TCY (2012) The effect of angiotensin-converting enzyme inhibitor use on bone loss in elderly Chinese. J Bone Miner Metab 30:666–673. https://doi.org/10.1007/s00774-012-0363-3
Rianon N, Ambrose CG, Pervin H et al (2017) Long-term use of angiotensin-converting enzyme inhibitors protects against bone loss in African-American elderly men. Arch Osteoporos 12:94. https://doi.org/10.1007/s11657-017-0387-3
Pasco JA, Nicholson GC, Kotowicz MA (2012) Cohort Profile: Geelong Osteoporosis Study. Int J Epidemiol 41:1565–1575
Adverse Drug Reactions Advisory Committee (1999) Australian Adverse Drug Reactions Bulletin. 18:1–4
Martineau P, Silva BC, Leslie WD (2017) Utility of trabecular bone score in the evaluation of osteoporosis. Curr Opin Endocrinol Diabetes Obes 24:402–410. https://doi.org/10.1097/med.0000000000000365
Giles GG, Ireland PD (1996) Dietary Questionnaire for Epidemiological Studies (Version 2), Melbourne. Cancer Counc Victoria
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383
Henry MJ, Pasco JA, Korn S et al (2010) Bone mineral density reference ranges for Australian men: Geelong Osteoporosis Study. Osteoporos Int 21:909–917
Henry MJ, Pasco JA, Pocock NA et al (2004) Reference ranges for bone densitometers adopted Australia-wide: Geelong osteoporosis study. Australas Radiol 48:473–475
Anderson KB, Holloway-Kew KL, Hans D et al (2019) Reference ranges for trabecular bone score in Australian men and women: a cross-sectional study. JBMR Plus 3:e10133. https://doi.org/10.1002/jbm4.10133
Choi HJ, Park C, Lee Y-K et al (2015) Risk of fractures in subjects with antihypertensive medications: a nationwide claim study. Int J Cardiol 184:62–67. https://doi.org/10.1016/j.ijcard.2015.01.072
Solomon DH, Mogun H, Garneau K, Fischer MA (2011) Risk of fractures in older adults using antihypertensive medications. J Bone Miner Res 26:1561–1567. https://doi.org/10.1002/jbmr.356
Kwok T, Leung J, Barrett-Connor E, Group for the OF in M (MrOS) R (2017) ARB users exhibit a lower fracture incidence than ACE inhibitor users among older hypertensive men. Age Ageing 46:57–64. https://doi.org/10.1093/ageing/afw150
Bokrantz T, Schiöler L, Boström KB et al (2020) Antihypertensive Drug Classes and the Risk of Hip Fracture: Results From the Swedish Primary Care Cardiovascular Database. J Hypertens 38:167–175
Butt DA, Mamdani M, Gomes T et al (2014) Risk of osteoporotic fractures with angiotensin II receptor blockers versus angiotensin-converting enzyme inhibitors in hypertensive community-dwelling elderly. J Bone Miner Res 29:2483–2488. https://doi.org/10.1002/jbmr.2271
Rejnmark L, Vestergaard P, Mosekilde L (2006) Treatment with beta-blockers, ACE inhibitors, and calcium-channel blockers is associated with a reduced fracture risk: a nationwide case–control study. J Hypertens 24
Kao Y-T, Huang C-Y, Fang Y-A, Liu J-C (2020) The association between renin angiotensin aldosterone system blockers and future osteoporotic fractures in a hypertensive population - a population-based cohort study in Taiwan. Int J Cardiol 305:147–153. https://doi.org/10.1016/j.ijcard.2019.12.069
Carbone LD, Vasan S, Prentice RL et al (2019) The renin-angiotensin aldosterone system and osteoporosis: findings from the Women’s Health Initiative. Osteoporos Int 30:2039–2056. https://doi.org/10.1007/s00198-019-05041-3
Chen C-I, Yeh J-S, Tsao N-W et al (2017) Association between renin-angiotensin-aldosterone system blockade and future osteoporotic fracture risk in hypertensive population: a population-based cohort study in Taiwan. Medicine (Baltimore) 96:e8331–e8331. https://doi.org/10.1097/MD.0000000000008331
Shea C, Witham MD (2020) Association between the use of angiotensin-blocking medications with hip fracture and death in older people. J Frailty Aging 9:107–110. https://doi.org/10.14283/jfa.2019.38
Kunutsor SK, Blom AW, Whitehouse MR et al (2017) Renin-angiotensin system inhibitors and risk of fractures: a prospective cohort study and meta-analysis of published observational cohort studies. Eur J Epidemiol 32:947–959. https://doi.org/10.1007/s10654-017-0285-4
Ruths S, Bakken MS, Ranhoff AH et al (2015) Risk of hip fracture among older people using antihypertensive drugs: a nationwide cohort study. BMC Geriatr 15:153. https://doi.org/10.1186/s12877-015-0154-5
Pérez-Castrillón JL, Silva J, Justo I et al (2003) Effect of quinapril, quinapril-hydrochlorothiazide, and enalapril on the bone mass of hypertensive subjects: relationship with angiotensin converting enzyme polymorphisms. Am J Hypertens 16:453–459. https://doi.org/10.1016/S0895-7061(03)00845-8
Steckelings UM, Kaschina E, Unger T (2005) The AT2 receptor—a matter of love and hate. Peptides 26:1401–1409. https://doi.org/10.1016/j.peptides.2005.03.010
Pasco JA, Kotowicz MA, Henry MJ, Nicholson GC, Spilsbury HJ, Box JDSH (2006) High sensitivity C-reactive protein and fracture risk in elderly women. JAMA 296:1353–1355
Quinn JMW, Gillespie MT (2005) Modulation of osteoclast formation. Biochem Biophys Res Commun 328:739–745. https://doi.org/10.1016/j.bbrc.2004.11.076
Tanabe N, Ito-Kato E, Suzuki N et al (2004) IL-1α affects mineralized nodule formation by rat osteoblasts. Life Sci 75:2317–2327. https://doi.org/10.1016/j.lfs.2004.04.026
Liao W-H, Suendermann C, Steuer AE et al (2018) Aldosterone deficiency in mice burdens respiration and accentuates diet-induced hyperinsulinemia and obesity. JCI Insight 3:e99015. https://doi.org/10.1172/jci.insight.99015
Yuan F-L, Xu M-H, Li X et al (2016) The roles of acidosis in osteoclast biology. Front Physiol 7:222
Butt DA, Alharty R, Leu R, Cheung AM (2015) Hypertension, antihypertensive drugs and the risk of fractures. Clin Rev Bone Miner Metab 13:160–172. https://doi.org/10.1007/s12018-015-9191-z
Hwang JK, Leu R, Butt DA (2015) Hypertension, antihypertensive drugs, and bone mineral density. Clin Rev Bone Miner Metab 13:149–159. https://doi.org/10.1007/s12018-015-9193-x
Ilić K, Obradović N, Vujasinović-Stupar N (2013) The relationship among hypertension, antihypertensive medications, and osteoporosis: a narrative review. Calcif Tissue Int 92:217–227. https://doi.org/10.1007/s00223-012-9671-9
Acknowledgements
The authors thank Professor Graham Giles of the Cancer Epidemiology Centre of The Cancer Council Victoria for permission to use the Dietary Questionnaire for Epidemiological Studies (Version 2), Melbourne: The Cancer Council Victoria 1996.
The authors also thank the Victorian Cancer Registry for data linkage.
Funding
The Geelong Osteoporosis Study was supported by grants from the National Health and Medical Research Council (NHMRC; projects 251638, 299831, 628582).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Barwon Health Human Research Ethics Committee approved the study (projects 92/01 and 00/56).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
For this type of study, formal consent is not required.
Conflict of interest
KLH-K is supported by an Alfred Deakin Postdoctoral Research Fellowship and KBA by an Australian Government Research Training Program Scholarship. AGB, JG, MAK, W-HL, MH, and JAP declare no competing interests.
Additional information
Publisher's Nnote
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Holloway-Kew, K.L., Betson, A.G., Anderson, K.B. et al. Association between bone measures and use of angiotensin-converting enzyme inhibitors or angiotensin II receptor blockers. Arch Osteoporos 16, 137 (2021). https://doi.org/10.1007/s11657-021-01004-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11657-021-01004-6