Abstract
Objective
To evaluate the effect of tai chi exercise on cardiac and static lung function for older community-dwelling adults at risk of ischemic stroke.
Methods
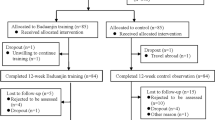
A total of 170 older community-dwelling adults (aged 55–75 years old) at risk of ischemic stroke were allocated to either tai chi training group (85 cases, five 60-min sessions of tai chi training per week for 12 weeks) or control group (85 cases, usual pbysical activity for 12 weeks) using a computer-generated randomization. The echocardiographic parameters of cardiac structure, cardiac function and static lung function were measured at baseline, after 12 weeks of intervention and additional 12-week follow-up period by a blinded professional staffmember using a color Doppler ultrasound imaging device or a cardiopulmonary function instrument. The t test and linear mixed model based on the intentionto-treat analysis principle was used to calculate the effect. The adverse effect was observed.
Results
Most of echocardiographic parameters on the cardiac structure, cardiac function and static lung function between the tai chi group and control group did not have a significant difference either post 12-week intervention or additional 12-week follow-up period. Only three parameters involving in right ventricular diameter (P=0.024), main pulmonary artery diameter (P=0.002) and vital capacity maximum (P=0.036) were beneficial to be improved in the tai chi group compared to the control group by the analysis of mixed linear model. No adverse effects were found during the intervention period.
Conclusion
The 12-week tai chi exercise did not have an obvious beneficial effect on cardiac structure, cardiac function and static lung function in older community-dwelling adults at risk of ischemic stroke. The study with a longer duration of intervention should be necessary. (Trial registration No. ChiCTR-TRC-13003601)
Similar content being viewed by others
References
Ferrari AU, Radaelli A, Centola M. Invited review: aging and the cardiovascular system. J Appl Physiol (1985) 2003;95:2591–2597.
Masugata H, Senda S, Goda F, Yoshihara Y, Yoshikawa K, Fujita N, et al. Cardiac function as assessed by echocardiography in the oldest old > or = 90 years of age. Int Heart J 2007;48:497–504.
Kwak HB. Aging, exercise, and extracellular matrix in the heart. J Exerc Rehabil 2013;9:338–347.
Fleg JL, Strait J. Age-associated changes in cardiovascular structure and function: a fertile milieu for future disease. Heart Fail Rev 2012;17:545–554.
Chambless LE, Folsom AR, Clegg LX, Sharrett AR, Shahar E, Nieto FJ, et al. Carotid wall thickness is predictive of incident clinical stroke: the Atherosclerosis Risk in Communities (ARIC) study. Am J Epidemiol 2000;151:478–487.
Yang EY, Chambless L, Sharrett AR, Virani SS, Liu X, Tang Z, et al. Carotid arterial wall characteristics are associated with incident ischemic stroke but not coronary heart disease in the Atherosclerosis Risk in Communities (ARIC) study. Stroke 2012;43:103–108.
Koren-Morag N, Goldbourt U, Tanne D. Relation between the metabolic syndrome and ischemic stroke or transient ischemic attack: a prospective cohort study in patients with atherosclerotic cardiovascular disease. Stroke 2005;36:1366–1371.
Lee CD, Blair SN. Cardiorespiratory fitness and stroke mortality in men. Med Sci Sport Exerc 2002;34:592–595.
Hooker SP, Sui X, Colabianchi N, Vena J, Laditka J, LaMonte MJ, et al. Cardiorespiratory fitness as a predictor of fatal and nonfatal stroke in asymptomatic woman and men. Stroke 2008;39:2950–2957.
Booher MA, Smith BW. Physiological effects of exercise on the cardiopulmonary system. Clin Sports Med 2003;22:1–21.
Thijssen DH, Maiorana AJ, O'Driscoll G, Cable NT, Hopman MT, Green DJ. Impact of inactivity and exercise on the vasculature in humans. Eur J Appl Physiol 2010;108:845–875.
van de Laar RJ, Ferreira I, van Mechelen W, Prins MH, Twisk JW, Stehouwer CD. Lifetime vigorous but not light-to-moderate habitual physical activity impacts favorably on carotid stiffness in young adults: the Amsterdam growth and health longitudinal study. Hypertension 2010;55:33–39.
Sacre JW, Jennings GL, Kingwell BA. Exercise and dietary influences on arterial stiffness in cardiometabolic disease. Hypertension 2014;63:888–893.
Mahdiabadi J, Gaeini AA, Kazemi T, Mahdiabadi MA. The effect of aerobic continuous and interval training on left ventricular structure and function in male non-athletes. Biol Sport 2013;30:207–211.
Aksakal E, Kurt M, Oztürk ME, Tanboga IH, Kaya A, Nacar T, et al. The effect of incremental endurance exercise training on left ventricular mechanics: a prospective observational deformation imaging study. Anadolu Kardiyol Derg 2013;13:432–438.
Iskander A, Thompson PD. A meta-analysis of aortic root size in elite athletes. Circulation 2013;127:791–798.
Oxborough D, Sharma S, Shave R, Whyte G, Birch K, Artis N, et al. The right ventricle of the endurance athlete: the relationship between morphology and deformation. J Am Soc Echocardiogr 2012;25:263–271.
Pelliccia A, Maron BJ, Di Paolo FM, BiffiA, Quattrini FM, Pisicchio C, et al. Prevalence and clinical significance of left atrial remodeling in competitive athletes. J Am Coll Cardiol 2005;46:690–696.
D'Ascenzi F, Pelliccia A, Natali BM, Zacà V, Cameli M, Alvino F, et al. Morphological and functional adaptation of left and right atria induced by training in highly trained female athletes. Circ Cardiovasc Imag 2014;7:222–229.
World Health Organization. Global recommendations on physical activity for health. Available at https://doi.org/www.who.int/dietphysicalactivity/factsheet_recommendations/en/.2012.
Bauman A, Bull F, Chey T, Craig CL, Ainsworth BE, Sallis JF, et al. The international prevalence study on physical activity: results from 20 countries. Int J Behav Nutr Phys Act 2009;6:21.
Global recommendations on physical activity for health. Geneva, Switzerland, World Health Organization 2010. Available at: https://doi.org/whqlibdoc.who.int/publications/2010/9789241599979_eng.pdf.
Yeh GY. Commentary on the Cochrane review of Tai Chi for rheumatoid arthritis. Explore 2008;4:275–277.
Yan JH, Gu WJ, Sun J, Zhang WX, Li BW, Pan L. Efficacy of tai chi on pain, stiffness and function in patients with osteoarthritis: a meta-analysis. PLoS One 2013;8:e61672.
Zheng G, Li S, Huang M, Liu F, Tao J, Chen L. The effect of tai chi training on cardiorespiratory fitness in healthy adults: a systematic review and meta-analysis. PLoS One 2015;10:e0117360.
Zheng G, Huang M, Liu F, Li S, Tao J, Chen L. Tai chi chuan for the primary prevention of stroke in middle-aged and elderly adults: a systematic review. Evid Based Complement Altern Med 2015;2015:742152.
Zheng G, Zheng X, Li J, Duan T, Qi D, Ling K, et al. Design, methodology and baseline characteristics of tai chi and its protective effect against ischaemic stroke risk in an elderly community population with risk factors for ischaemic stroke: a randomised controlled trial. BMJ Open 2015;5:e009158.
Wang LD, ed. Screening of subjects at high risk for stroke. Beijing: Ministry of Public Health Press;2012:2–4.
Sheng JZ, Gu LX, Fu ZW, Tang H, eds. The comprehensive book of tai chi chuan. 2nd ed. Beijing: People Sports Press;2006:125.
Schafer JL. Multiple imputation: a primer. Stat Method Med Res 1999;8:3–15.
Kodama S, Saito K, Tanaka S, Maki M, Yachi Y, Asumi M, et al. Cardiorespiratory fitness as a quantitative predictor of all-cause mortality and cardiovascular events in healthy men and women: a meta-analysis. JAMA 2009;301:2024–2035.
Cheon SM, Chae BK, Sung HR, Lee GC, Kim JW. The efficacy of exercise programs for parkinson's disease: tai chi versus combined exercise. J Clin Neurol 2013;9:237–243.
Lan C, Chou SW, Chen SY, Lai JS, Wong MK. The aerobic capacity and ventilatory efficiency during exercise in Qigong and tai chi chuan practitioners. Am J Chin Med 2004;32:141–50.
Niu R, He R, Luo BL, Hu C. The effect of tai chi on chronic obstructive pulmonary disease: a pilot randomised study of lung function, exercise capacity and diaphragm strength. Heart Lung Circ 2014;23:347–352.
Lan C, Chen SY, Lai JS. Changes of aerobic capacity, fat ratio and flexibility in older TCC practitioners: a five-year follow-up. Am J Chin Med 2008;36:1041–1050.
Lan C, Chen SY, Lai JS, Wong MK. The effect of tai chi on cardiorespiratory function in patients with coronary artery bypass surgery. Med Sci Sports Exerc 1999;31:634–638.
Shi ZM, Wen HP, Liu FR, Yao CX. The effects of tai chi on the renal and cardiac functions of patients with chronic kidney and cardiovascular diseases. J Phys Ther Sci 2014;26:1733–1736.
Xiong KY, He H, Ni GX. Effect of skill level on cardiorespiratory and metabolic responses during tai chi training. Eur J Sport Sci 2013;13:386–391.
Tonelli AR, Johnson S, Alkukhun L, Yadav R, Dweik RA. Changes in main pulmonary artery diameter during follow-up have prognostic implications in pulmonary arterial hypertension. Respirology 2017;22:1649–1655.
Lee J, Kang T, Yeo Y, Han D. The change of lung capacity in elderly women caused by life span. J Phys Ther Sci 2017;29:658–661.
Wernstedt P, Sjöstedt C, Ekman I, Du H, Thuomas KA, Areskog NH, et al. Adaptation of cardiac morphology and function to endurance and strength training. A comparative study using MR imaging and echocardiography in males and females. Scand J Med Sci Sports 2002;12:17–25.
Acknowledgements
We thank the participants and staff in the communities and hospitals, including the Fujian University of Traditional Chinese Medicine Subsidiary Rehabilitation Hospital and Health Check Center of the Second People's Hospital of Fujian Province, for their work in this project.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by the Study of Traditional Chinese Mind-Body Exercise (No. X2012002-Cooperation) and the Social Development Guidance Project of Fujian Province (No. 2014Y0031)
Rights and permissions
About this article
Cite this article
Zheng, Gh., Zheng, X., Li, Jz. et al. Effect of Tai Chi on Cardiac and Static Pulmonary Function in Older Community-Dwelling Adults at Risk of Ischemic Stroke: A Randomized Controlled Trial. Chin. J. Integr. Med. 25, 582–589 (2019). https://doi.org/10.1007/s11655-018-3056-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11655-018-3056-5