Abstract
Purpose
It is unclear if there is a consistent signature in breath patterns prior to an impending obstructive apneic event in patients with sleep-disordered breathing (SDB).
Objective
To use continuous recordings of ambient sound in sleep using a smartphone to track auditory signatures of breaths and measure their regularity preceding apneic events.
Methods
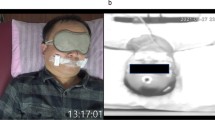
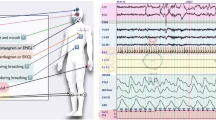
We studied 50 patients evaluated for SDB in whom sound was recorded using smartphones concurrently with polysomnography (PSG). Whole-night sound files were analyzed for time and frequency domain analyses of breath periodicity during periods of normal and sleep-disordered breathing.
Results
Fifty patients (44% women, 42.0 ± 9.4 years old, BMI 32.8 ± 10.8 kg/m2) recorded sound, of whom 30 were diagnosed with OSA and 20 were not. We analyzed a total of 497 apneic (≥10 s) and 481 non-apneic intervals, confirmed by PSG. Interbreath intervals were 3.75 ± 0.62 s for 1 min in quiet breathing, with SD 1.11 ± 0.48 s that increased to 4.16 ± 3.06 s in successive 60-s epochs up to apnea (p < 0.001). Interbreath SD in the 60 s immediately preceding apnea was higher than the SD in random non-apneic periods (p < 0.01, ANOVA). Interbreath SD ≥1.49 s gave 87.3% sensitivity and 86.5% specificity for predicting apnea in the next minute (c-statistic 0.94).
Conclusions
Breaths increase in variability minutes before proven obstructive apnea in patients with suspected SDB. These results suggest that it may be possible to predict and thus potentially avert apneic events and provide insights into events leading to SDB.
Trial registration
NCT03288376, clinicaltrials.org






Similar content being viewed by others
Abbreviations
- AASM:
-
American Academy of Sleep Medicine
- AHI:
-
Apnea Hypopnea Index
- BMI:
-
body mass index (kg/m2)
- CPAP:
-
continuous positive airway pressure
- dB:
-
decibel
- ECG:
-
electrocardiogram
- EEG:
-
electroencephalogram
- Epoch:
-
one-minute audio segment
- HST:
-
home sleep testing
- IRB:
-
Institutional Review Board
- PSG:
-
polysomnography
- OSA:
-
obstructive sleep apnea
- SD:
-
standard deviation
- SDB:
-
sleep-disordered breathing
References
Mysliwiec V, Martin JL, Ulmer CS, Chowdhuri S, Brock MS, Spevak C and Sall J (2020) The management of chronic insomnia disorder and obstructive sleep apnea: synopsis of the 2019 U.S. Department of Veterans Affairs and U.S. Department of Defense Clinical Practice Guidelines. Ann Intern Med
Pack A, Maislin G, Staley B, Pack F, Rogers W, George C, Dinges D (2006) Impaired performance in commercial drivers—role of sleep apnea and short sleep duration. American Journal of Respiratory and Critical Care Medicine 174:446–454
Siedlecka J, Rybacki M, Plywaczewski R, Czajkowska-Malinowska M, Radlinski J, Kania A, Sliwinski P (2020) The management of obstructive sleep apnea syndrome in drivers—recommendations of the Polish Society Of Occupational Medicine, the Polish Respiratory Society, the Nofer Institute of Occupational Medicine in Lodz and the Polish Sleep Research Society. Med Pr 71:233–243
Linz D, McEvoy RD, Cowie MR, Somers VK, Nattel S, Levy P, Kalman JM, Sanders P (2018) Associations of obstructive sleep apnea with atrial fibrillation and continuous positive airway pressure treatment: a review. JAMA Cardiol 3:532–540
Freedman N (2015) Counterpoint: Does laboratory polysomnography yield better outcomes than home sleep testing? No. Chest; 148:308–10
Pack AI (2015) Point: Does laboratory polysomnography yield better outcomes than home sleep testing? Yes. Chest;148:306–8
Friedman M, Shnowske K, Hamilton C, Samuelson CG, Hirsch M, Pott TR, Yalamanchali S (2014) Mandibular advancement for obstructive sleep apnea: relating outcomes to anatomy. JAMA otolaryngology-- head & neck surgery 140:46–51
Koo SK, Kwon SB, Kim YJ, Moon JI, Kim YJ and Jung SH. (2016) Acoustic analysis of snoring sounds recorded with a smartphone according to obstruction site in OSAS patients. Eur Arch Otorhinolaryngol
Behbehani K, Lopez F, Yen FC, Lucas EA, Burk JR, Axe JP, Kamangar F (1997) Pharyngeal wall vibration detection using an artificial neural network. Medical & biological engineering & computing 35:193–198
Tan SK, Leung WK, Tang ATH, Zwahlen RA (2017) How does mandibular advancement with or without maxillary procedures affect pharyngeal airways? An overview of systematic reviews. PLoS One 12:e0181146
Narayan S, Shivdare P, Niranjan T, Williams K, Freudman J and Sehra R. (2018) Noncontact identification of sleep-disturbed breathing from smartphone-recorded sounds validated by polysomnography. Sleep Breath
Ben-Israel N, Tarasiuk A and Zigel Y. (2010) Nocturnal sound analysis for the diagnosis of obstructive sleep apnea. Conference proceedings: Annual International Conference of the IEEE Engineering in Medicine and Biology Society IEEE Engineering in Medicine and Biology Society Annual Conference;2010:6146–9
Force USPST, Bibbins-Domingo K, Grossman DC, Curry SJ, Davidson KW, Epling JW Jr, Garcia FA, Herzstein J, Kemper AR, Krist AH, Kurth AE, Landefeld CS, Mangione CM, Phillips WR, Phipps MG, Pignone MP, Silverstein M, Tseng CW (2017) Screening for obstructive sleep apnea in adults: US Preventive Services Task Force recommendation statement. JAMA. 317:407–414
Smith HA, Smith ML (2017) The role of dentists and primary care physicians in the care of patients with sleep-related breathing disorders. Front Public Health 5:137
Bailes S, Fichten CS, Rizzo D, Baltzan M, Grad R, Pavilanis A, Creti L, Amsel R, Libman E (2017) The challenge of identifying family medicine patients with obstructive sleep apnea: addressing the question of gender inequality. Fam Pract 34:467–472
Chiu HY, Chen PY, Chuang LP, Chen NH, Tu YK, Hsieh YJ, Wang YC, Guilleminault C (2017) Diagnostic accuracy of the Berlin questionnaire, STOP-BANG, STOP, and Epworth sleepiness scale in detecting obstructive sleep apnea: a bivariate meta-analysis. Sleep Med Rev 36:57–70
Younes M, Raneri J and Hanly P. (2016) Staging sleep in polysomnograms: analysis of inter-scorer variability. Journal of clinical sleep medicine : JCSM : official publication of the American Academy of Sleep Medicine
Majumder S, Mondal T and Deen MJ (2017) Wearable sensors for remote health monitoring. Sensors (Basel). 17
Thap T, Chung H, Jeong C, Hwang KE, Kim HR, Yoon KH and Lee J. (2016) High-resolution time-frequency spectrum-based lung function test from a smartphone microphone. Sensors (Basel). 16
Toy BC, Myung DJ, He L, Pan CK, Chang RT, Polkinhorne A, Merrell D, Foster D, Blumenkranz MS (2016) Smartphone-based dilated fundus photography and near visual acuity testing as inexpensive screening tools to detect referral warranted diabetic eye disease. Retina. 36:1000–1008
Cornet VP, Holden RJ (2018) Systematic review of smartphone-based passive sensing for health and wellbeing. J Biomed Inform 77:120–132
Agbana TE, Diehl JC, van Pul F, Khan SM, Patlan V, Verhaegen M, Vdovin G (2018) Imaging & identification of malaria parasites using cellphone microscope with a ball lens. PLoS One 13:e0205020
Shcherbina A and Ashley EA. (2017) Accuracy in wrist-worn, sensor-based measurements of heart rate and energy expenditure in a diverse cohort. J Pers Med 7(2):3
Nakano H, Hirayama K, Sadamitsu Y, Toshimitsu A, Fujita H, Shin S, Tanigawa T (2014) Monitoring sound to quantify snoring and sleep apnea severity using a smartphone: proof of concept. Journal of clinical sleep medicine : JCSM : official publication of the American Academy of Sleep Medicine 10:73–78
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Narayan, Dr. Sehra, and Mr. Niranjan are inventors of an intellectual property owned by Resonea Inc. Dr. Sehra and Mr. Niranjan are employees of Resonea Inc.
Informed consent
All participants involved in the study gave their informed consent.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 83 kb)
Rights and permissions
About this article
Cite this article
Pandian, T.N.G., Sehra, R. & Narayan, S. Breath variability increases in the minutes preceding obstructive sleep apneic events. Sleep Breath 25, 271–280 (2021). https://doi.org/10.1007/s11325-020-02094-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-020-02094-1