Abstract
Purpose
This study aimed to explore the feasibility of [68 Ga]pentixafor positron emission tomography/computed tomography (PET/CT) in patients with nasopharyngeal carcinoma (NPC).
Procedures
This prospective study included patients with NPC who underwent [68 Ga]pentixafor PET/CT and 2-[18F]fuoro-2-deoxy-D-glucose ([18F]FDG) PET/CT within one week between November 2022 and March 2023. The [68 Ga]pentixafor and [18F]FDG uptakes in primary and metastatic lesions were measured and compared.
Results
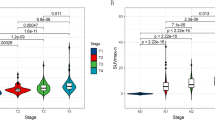
Twenty-five participants (21 patients for initial stage and four patients for recurrence detection) were enrolled in our study. The participants underwent [18F]FDG PET/CT and [68 Ga]pentixafor PET/CT. [68 Ga]pentixafor PET/CT had the same detection rate as [18F]FDG for primary tumor (96% vs. 96%). The [68 Ga]pentixafor maximum standard uptake value (SUVmax) and target-to-background ratio (TBR) of primary tumors were lower than those of [18F]FDG (SUVmax: 8.13 ± 2.78 vs. 14.25 ± 6.45; P < 0.01; TBR: 5.17 ± 2.14 vs. 9.81 ± 5.30, P < 0.01). The difference between tumor volume of [68 Ga]pentixafor (TVpentixafor) and tumor volume of [18F]FDG (TVFDG) showed no significance (median: 16.01 vs. 9.56, P = 0.332). In the detection of suspected metastatic cervical lymph nodes (CLNs), [68 Ga]pentixafor PET possessed a lower SUVmax than [18F]FDG PET/CT (SUVmax: 6.86 ± 2.63 vs. 10.39 ± 5.28, P < 0.01), but there was no significant difference in the detection rate between [68 Ga]pentixafor and [18F]FDG PET/CT (96 vs. 98, P = 0.613).
Conclusions
[68 Ga]pentixafor is a promising imaging tracer for detecting primary and metastatic NPC. [68 Ga]pentixafor PET/CT is comparable to [18F]FDG PET/CT in the detection rate of primary tumors and metastatic cervical lymph nodes in nasopharyngeal carcinoma, but [68 Ga]pentixafor uptake was heterogeneous. [68 Ga]pentixafor PET/CT may help select patients most likely to benefit from CXCR4-directed endoradiotherapy.
Clinical trial registration No.: ChiCTR2200065902




Similar content being viewed by others
References
Chen YP, Chan ATC, Le QT, Blanchard P, Sun Y, Ma J (2019) Nasopharyngeal carcinoma. Lancet 394:64–80
Li WF, Sun Y, Chen M et al (2012) Locoregional extension patterns of nasopharyngeal carcinoma and suggestions for clinical target volume delineation. Chin J Cancer 31:579–587
Tang LL, Chen WQ, Xue WQ et al (2016) Global trends in incidence and mortality of nasopharyngeal carcinoma. Cancer Lett 374:22–30
Wei KR, Zheng RS, Zhang SW, Liang ZH, Ou ZX, Chen WQ (2014) Nasopharyngeal carcinoma incidence and mortality in China in 2010. Chin J Cancer 33:381–387
King AD, Vlantis AC, Bhatia KS et al (2011) Primary nasopharyngeal carcinoma: diagnostic accuracy of MR imaging versus that of endoscopy and endoscopic biopsy. Radiology 258:531–537
Yen TC, Chang YC, Chan SC et al (2005) Are dual-phase 18F-FDG PET scans necessary in nasopharyngeal carcinoma to assess the primary tumour and loco-regional nodes? Eur J Nucl Med Mol Imaging 32:541–548
Chua ML, Ong SC, Wee JT et al (2009) Comparison of 4 modalities for distant metastasis staging in endemic nasopharyngeal carcinoma. Head Neck 31:346–354
Liu FY, Chang JT, Wang HM et al (2006) [18F]fluorodeoxyglucose positron emission tomography is more sensitive than skeletal scintigraphy for detecting bone metastasis in endemic nasopharyngeal carcinoma at initial staging. J Clin Oncol 24:599–604
Liu FY, Lin CY, Chang JT et al (2007) 18F-FDG PET can replace conventional work-up in primary M staging of nonkeratinizing nasopharyngeal carcinoma. J Nucl Med 48:1614–1619
Xiao BB, Chen QY, Sun XS et al (2021) Low value of whole-body dual-modality [18f]fluorodeoxyglucose positron emission tomography/computed tomography in primary staging of stage I-II nasopharyngeal carcinoma: a nest case-control study. Eur Radiol 31:5222–5233
Ng SH, Chan SC, Yen TC et al (2009) Staging of untreated nasopharyngeal carcinoma with PET/CT: comparison with conventional imaging work-up. Eur J Nucl Med Mol Imaging 36:12–22
Chen WS, Li JJ, Hong L, Xing ZB, Wang F, Li CQ (2016) Comparison of MRI, CT and 18F-FDG PET/CT in the diagnosis of local and metastatic of nasopharyngeal carcinomas: an updated meta analysis of clinical studies. Am J Transl Res 8:4532–4547
Teicher BA, Fricker SP (2010) CXCL12 (SDF-1)/CXCR4 pathway in cancer. Clin Cancer Res 16:2927–2931
Derlin T, Hueper K (2018) CXCR4-targeted therapy in breast cancer. Lancet Oncol 19:e370
Zong G, Han J, Yue Z, Liu Y, Cui Z, Shi L (2020) Downregulation of miR-204 facilitates the progression of nasopharyngeal carcinoma by targeting CXCR4 through NF-kappaB signaling pathway. J BUON 25:1098–1104
Hadebe B, Sathekge MM, Aldous C, Vorster M (2022) Current status of (68)Ga-Pentixafor in solid tumours. Diagnostics (Basel) 12(9):2135
Ramachandran A, Krishnaraju VS, Kumar R, Shukla J, Laroya I (2022) Ga-68 chemokine Receptor-4 PET/CT imaging in Schminke type of nasopharyngeal carcinoma. Indian J Nucl Med 37:284–285
van den Brekel MW, Stel HV, Castelijns JA et al (1990) Cervical lymph node metastasis: assessment of radiologic criteria. Radiology 177:379–384
Zhang GY, Liu LZ, Wei WH, Deng YM, Li YZ, Liu XW (2010) Radiologic criteria of retropharyngeal lymph node metastasis in nasopharyngeal carcinoma treated with radiation therapy. Radiology 255:605–612
Buck AK, Haug A, Dreher N et al (2022) Imaging of C-X-C motif chemokine receptor 4 expression in 690 patients with solid or hematologic neoplasms using (68)Ga-Pentixafor PET. J Nucl Med 63:1687–1692
Dreher N, Hahner S, Fuss CT et al (2023) CXCR4-directed PET/CT with [(68) Ga]Ga-pentixafor in solid tumors-a comprehensive analysis of imaging findings and comparison with histopathology. Eur J Nucl Med Mol Imaging 51(5):1383–1394
Watts A, Singh B, Singh H et al (2023) [(68)Ga]Ga-Pentixafor PET/CT imaging for in vivo CXCR4 receptor mapping in different lung cancer histologic sub-types: correlation with quantitative receptors’ density by immunochemistry techniques. Eur J Nucl Med Mol Imaging 50:1216–1227
Werner RA, Kircher S, Higuchi T et al (2019) CXCR4-Directed imaging in solid tumors. Front Oncol 9:770
Zhi Y, Werner RA, Schirbel A et al (2023) Diagnostic efficacy of C-X-C motif chemokine receptor 4-directed PET/CT in newly diagnosed head and neck squamous cell carcinoma - a head-to-head comparison with [(18)F]FDG. Am J Nucl Med Mol Imaging 13:208–216
Qin N, Zhang Y, Xu L, Liu W, Luo B (2022) Maintenance of Epstein-Barr virus latency through interaction of LMP2A with CXCR4. Arch Virol 167:1947–1959
Yen RF, Chen TH, Ting LL, Tzen KY, Pan MH, Hong RL (2005) Early restaging whole-body (18)F-FDG PET during induction chemotherapy predicts clinical outcome in patients with locoregionally advanced nasopharyngeal carcinoma. Eur J Nucl Med Mol Imaging 32:1152–1159
King AD, Ma BB, Yau YY et al (2008) The impact of 18F-FDG PET/CT on assessment of nasopharyngeal carcinoma at diagnosis. Br J Radiol 81:291–298
Fischbein NJ, AAssar OS, Caputo GR et al (1998) Clinical utility of positron emission tomography with 18F-fluorodeoxyglucose in detecting residual/recurrent squamous cell carcinoma of the head and neck. AJNR Am J Neuroradiol 19:1189–1196
Tsai MC, Shu YC, Hsu CC et al (2016) False-positive finding of retropharyngeal lymph node recurrence in both fluorine (18)FDG PET and MRI in a patient with nasopharyngeal carcinoma. Head Neck 38:E84-86
Bouter C, Meller B, Sahlmann CO et al (2018) (68)Ga-Pentixafor PET/CT imaging of chemokine receptor CXCR4 in chronic infection of the bone: first insights. J Nucl Med 59:320–326
Kircher M, Tran-Gia J, Kemmer L et al (2020) Imaging inflammation in atherosclerosis with CXCR4-Directed (68)Ga-Pentixafor PET/CT: correlation with (18)F-FDG PET/CT. J Nucl Med 61:751–756
Derlin T, Jaeger B, Jonigk D et al (2021) Clinical molecular imaging of pulmonary CXCR4 expression to predict outcome of pirfenidone treatment in idiopathic pulmonary fibrosis. Chest 159:1094–1106
Lapa C, Hanscheid H, Kircher M et al (2019) Feasibility of CXCR4-Directed radioligand therapy in advanced diffuse large B-Cell Lymphoma. J Nucl Med 60:60–64
Lapa C, Herrmann K, Schirbel A et al (2017) CXCR4-directed endoradiotherapy induces high response rates in extramedullary relapsed Multiple Myeloma. Theranostics 7:1589–1597
Habringer S, Lapa C, Herhaus P et al (2018) Dual targeting of acute leukemia and supporting niche by CXCR4-Directed theranostics. Theranostics 8:369–383
Acknowledgements
We would like to thank Yue Feng, Department of Nuclear Medicine, the Affiliated Hospital of Southwest Medical University, for preparation of [68Ga]pentixafor.
Funding
This study was funded by Sichuan Provincial Science and Technology Department (Grant No.2022NSFSC0827), Luzhou Science and Technology Bureau (Grant No.2021CDLZ-9) and Sichuan Science and Technology Program (Grant No.2022YFS0608).
Author information
Authors and Affiliations
Contributions
ML, XC and HD contributed to the study conception and design. Material preparation and data collection were performed by ML, XC, HD, QS, YZ, YC and LC. ML and XC processed and analyzed the data. The first draft of the manuscript was written by ML and XC, and HD reviewed and revised the manuscript. All authors contributed to the article and approved the submitted version.
Corresponding authors
Ethics declarations
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Mengna Liu, Xi Chen and Haoyuan Ding contributed equally to this work and share first authorship.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Liu, M., Chen, X., Ding, H. et al. Comparison of [18F]FDG and [68 Ga]pentixafor PET/CT in Nasopharyngeal Carcinoma. Mol Imaging Biol (2024). https://doi.org/10.1007/s11307-024-01913-1
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s11307-024-01913-1