Abstract
Objectives
Substance misuse during pregnancy can be harmful to the health of both mothers and infants. Existing recovery services or prenatal care for pregnant women with substance use disorders (SUD) in the U.S. and other countries typically fall short in providing the necessary specialized care women with SUDs need. Disclosure of substance misuse is one key factor in gaining access to specialized prenatal care; yet, barriers such as social stigma and internal shame and guilt lead many women to under-report any substance misuse during their pregnancy. This study sought to understand the process of how and why pregnant women with SUDs choose to disclose or not disclose their substance misuse to their providers when seeking prenatal care.
Methods
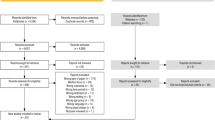
Data were collected through interviews with N = 21 women with SUDs in the northeast U.S. whose young children had been exposed to opioids, cocaine, or MAT in utero. Thematic, inductive analysis using line-by-line coding was conducted to understand the perspectives of the women.
Results
The women’s narratives suggested a clear tension regarding whether to disclose their substance misuse to any providers during their pregnancy. Four themes describing the process of disclosure or non-disclosure were found, including reasons for and ways of being secret or choosing to disclose their substance misuse during pregnancy.
Conclusions for Practice
The centrality of shame, guilt, and stigma regarding substance misuse must be addressed by medical and mental health providers in order to increase disclosure and improve access to care for women with SUDs.
Similar content being viewed by others
References
American College of Obstetricians and Gynecologists. (2017). Opioid use and opioid use disorder in pregnancy. https://www.acog.org/clinical/clinical-guidance/committee-opinion/articles/2017/08/opioid-use-and-opioid-use-disorder-in-pregnancy.
Amnesty International. (2017). Criminalizing pregnancy: Policing pregnant women who use drugs in the USA.https://www.amnesty.org/download/Documents/AMR5162032017ENGLISH.pdf.
Bishop, D., Borkowski, L., Couillard, M., Allina, A., Baruch, S., & Wood, S. (2017). Bridging the divide white paper: Pregnant women and substance use: Overview of research and policy in the United States. Jacobs Institute of Women’s Health. Paper 5. https://pdfs.semanticscholar.org/62f8/175426c9db6ecccba2183bff6799537daaf9.pdf.
Braun, V., & Clarke, V. (2006). Using thematic analysis in psychology. Qualitative Research in Psychology, 3(2), 77–101. https://doi.org/10.1191/1478088706qp063oa.
Child Welfare Information Gateway. (2019). About CAPTA: A legislative history. Children’s Bureau, U.S. Department of Health and Human Services. https://www.childwelfare.gov/pubPDFs/about.pdf.
Forray, A. (2016). Substance use during pregnancy. F1000Research, 5, 887. https://doi.org/10.12688/f1000research.7645.1.
Goel, N., Beasley, D., Rajkumar, V., & Banerjee, S. (2010). Perinatal outcome of illicit substance use in pregnancy—Comparative and contemporary socio-clinical profile in the UK. European Journal of Pediatrics, 170(2), 199–205. https://doi.org/10.1007/s00431-010-1284-6.
Goodman, D. J., Saunders, E. C., & Wolff, K. B. (2020). In their own words: a qualitative study of factors promoting resilience and recovery among postpartum women with opioid use disorders. BMC Pregnancy and Childbirth, 20(1), 1–10.
Harris, J., & McElrath, K. (2012). Methadone as social control: Institutionalized stigma and the prospect of recovery. Qualitative Health Research, 22(6), 810–824. https://doi.org/10.1177/1049732311432718.
Howard, H. (2015). Reducing stigma: Lessons from opioid-dependent women. Journal of Social Work Practice in the Addictions, 15(4), 418–438. https://doi.org/10.1080/1533256x.2015.1091003.
Jackson, A., & Shannon, L. (2012). Barriers to receiving substance abuse treatment among Rural pregnant women in Kentucky. Maternal and Child Health Journal, 16(9), 1762–1770. https://doi.org/10.1007/s10995-011-0923-5.
Jones, H. E., Deppen, K., Hudak, M. L., Leffert, L., McClelland, C., Sahin, L., et al. (2014). Clinical care for opioid-using pregnant and postpartum women: The role of obstetric providers. American Journal of Obstetrics and Gynecology, 210(4), 302–310. https://doi.org/10.1016/j.ajog.2013.10.010.
Kaltenbach, K. (2013). Bio-psychosocial characteristics of parenting women with substance use disorders. In N. Suchman, M. Pajulo, & L. Mayes (Eds.), Parenting and substance abuse: Developmental approaches to interventio (pp. 185–194). Oxford: Oxford University Press.
Kuo, C., Schonbrun, Y. C., Zlotnick, C., Bates, N., Todorova, R., Kao, J. C.-W., et al. (2013). A qualitative study of treatment needs among pregnant and postpartum women with substance use and depression. Substance Use & Misuse, 48(14), 1498–1508. https://doi.org/10.3109/10826084.2013.800116.
Liu, A. J., Jones, M. P., Murray, H., Cook, C.-M., & Nanan, R. (2010). Perinatal risk factors for the neonatal abstinence syndrome in infants born to women on methadone maintenance therapy. Australian and New Zealand Journal of Obstetrics and Gynaecology, 50(3), 253–258. https://doi.org/10.1111/j.1479-828x.2010.01168.x.
Marroun, H. E., Tiemeier, H., Jaddoe, V. W., Hofman, A., Mackenbach, J. P., Steegers, E. A., et al. (2008). Demographic, emotional and social determinants of cannabis use in early pregnancy: The Generation R study. Drug and Alcohol Dependence, 98(3), 218–226. https://doi.org/10.1016/j.drugalcdep.2008.05.010.
McCance-Katz, E. F. (2018). The national survey on drug use and health: 2017. Substance Abuse and Mental Health Services Administration. https://www.samhsa.gov/data/sites/default/files/nsduh-ppt-09-2018.pdf.
New York State Corrections and Community Supervision. (2019). Trauma, addictions, mental health and recovery (TAMAR) facilitators manual.
O'Donnell, F. T., & Jackson, D. L. (2017). Opioid use disorder and pregnancy. Missouri Medicine, 114(3), 181–186.
Pajulo, H., Pajulo, M., Jussila, H., & Ekholm, E. (2016). Substance-abusing pregnant women: Prenatal intervention using ultrasound consultation and mentalization to enhance the mother-child relationship and reduce substance use. Infant Mental Health Journal, 37(4), 317–334. https://doi.org/10.1002/imhj.21574.
Passey, M. E., Sanson-Fisher, R. W., D’Este, C. A., & Stirling, J. M. (2014). Tobacco, alcohol and cannabis use during pregnancy: Clustering of risks. Drug and Alcohol Dependence, 134, 44–50. https://doi.org/10.1016/j.drugalcdep.2013.09.008.
Roberts, S. C., & Nuru-Jeter, A. (2010). Women's Perspectives on screening for alcohol and drug use in prenatal care. Women's Health Issues, 20(3), 193–200. https://doi.org/10.1016/j.whi.2010.02.003.
Roberts, S. C. M., & Pies, C. (2010). Complex calculations: How drug use during pregnancy becomes a barrier to prenatal care. Maternal and Child Health Journal, 15(3), 333–341. https://doi.org/10.1007/s10995-010-0594-7.
Saia, K. A., Schiff, D., Wachman, E. M., Mehta, P., Vilkins, A., Sia, M., et al. (2016). Caring for pregnant women with opioid use disorder in the USA: expanding and improving treatment. Current Obstetrics and Gynecology Reports, 5(3), 257–263.
Schempf, A. H., & Strobino, D. M. (2008). Illicit drug use and adverse birth outcomes: Is it drugs or context? Journal of Urban Health, 85(6), 858–873. https://doi.org/10.1007/s11524-008-9315-6.
Smith, K., & Lipari, R. (2017, January). Women of childbearing age and opioids. Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration, U.S. Department of Health and Human Services. https://www.samhsa.gov/data/sites/default/files/report_2724/ShortReport-2724.html.
Stone, R. (2015). Pregnant women and substance use: Fear, stigma, and barriers to care. Health & Justice. https://doi.org/10.1186/s40352-015-0015-5.
Substance Abuse and Mental Health Services Administration. (2018a). Clinical guidance for treating pregnant and parenting women with opioid use disorder and their infants (HHS Publication Np. SMA18-5054).
Substance Abuse and Mental Health Services Administration. (2018b). Results from the 2017 national survey on drug use and health: Detailed tables.https://www.samhsa.gov/data/sites/default/files/report_2724/ShortReport-2724.html.
Substance Abuse and Mental Health Services Administration. (2019). Medication-assisted treatment (MAT). https://www.samhsa.gov/medication-assisted-treatment.
Terplan, M., Kennedy-Hendricks, A., & Chisolm, M. S. (2015). Article commentary: Prenatal substance use: Exploring assumptions of maternal unfitness. Substance Abuse: Research and Treatment, 9s2, 1–4. https://doi.org/10.4137/sart.s23328.
Tong, A., Sainsbury, P., & Craig, J. (2007). Consolidated criteria for reporting qualitative research (COREQ): A 32-item checklist for interviews and focus groups. International journal for Quality in Health Care, 19(6), 349–357.
Woo, J., Bhalerao, A., Bawor, M., Bhatt, M., Dennis, B., Mouravska, N., et al. (2017). “Don’t judge a book by its cover”: A qualitative study of methadone patients’ experiences of stigma. Substance Abuse: Research and Treatment, 11, 1–12. https://doi.org/10.1177/1178221816685087.
Acknowledgements
Support for this work was in part provided by the Hawk Foundation. The authors would like to thank Peggy Kaufman, Eda Spielman and the staff of the NESST program, Greater Boston Jewish Family and Children’s Service and study participants for their willingness to share their experiences.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Paris, R., Herriott, A.L., Maru, M. et al. Secrecy Versus Disclosure: Women with Substance Use Disorders Share Experiences in Help Seeking During Pregnancy. Matern Child Health J 24, 1396–1403 (2020). https://doi.org/10.1007/s10995-020-03006-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-020-03006-1