Abstract
Purpose
Inborn errors of immunity (IEI) are typically monogenic. Data from the Indian subcontinent are relatively scarce. This paper evaluates IEI diagnosed in Sri Lanka.
Methods
Data of patients diagnosed with IEI from 2010 to 2022 at the Department of Immunology, Medical Research Institute, Colombo, Sri Lanka, were retrospectively analyzed.
Results
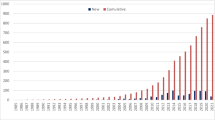
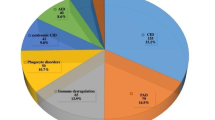
Two hundred and six patients were diagnosed with IEI, with a prevalence of 0.94 per 100,000. The onset of disease was below 12 years in 84.9%, whereas in 10.9%, it was after 18 years. The male: female ratio was 1.78:1. Consanguinity was identified in 26.6%. IEI were found in all but one (bone marrow failure) of the 10 IUIS categories. Predominantly antibody deficiencies were the most common category among the nine identified (30.1%), followed by combined immune deficiencies with syndromic features (21.3%), immunodeficiencies affecting cellular and humoral immunity (19.9%), congenital defects of phagocyte number or function (13.1%), and defects in intrinsic and innate immunity (8.2%). Severe combined immune deficiency (SCID) was the commonest disease (14.6%), followed by chronic granulomatous disease (CGD) (10.6%) and X linked agammaglobulinemia (8.7%). Of the patients with a known outcome (n = 184), 51 died (27.7%). Mortality rates were high in SCID (83.3%), Omenn syndrome (OS) (100%), and CGD (31.8%) patients.
Conclusion
IEI in Sri Lanka are diagnosed mainly in childhood. The low diagnosis rates suggest a need for educating clinicians regarding IEI in adulthood. The high mortality rates associated with some IEI indicate the need of transplant services in the country.


Similar content being viewed by others
Data Availability
The original contributions presented in the study are included in the article/supplementary material. Further inquiries can be directed to the corresponding author.
References
Tangye SG, Al-Herz W, Bousfiha A, Cunningham-Rundles C, Franco JL, Holland SM, Klein C, et al. Human inborn errors of immunity: 2022 update on the classification from the International Union of Immunological Societies Expert Committee. J Clin Immunol. 2022;42(7):1473–507. https://doi.org/10.1007/s10875-022-01289-3.
Notarangelo LD, Bacchetta R, Casanova JL, Su HC. Human inborn errors of immunity: an expanding universe. Sci Immunol. 2020;5(49):eabb1662. https://doi.org/10.1126/sciimmunol.abb1662.
Spaan AN, Neehus AL, Laplantine E, Staels F, Ogishi M, Seeleuthner Y, et al. Human OTULIN haploinsufficiency impairs cell-intrinsic immunity to staphylococcal α-toxin. Science. 2022;376(6599):eabm6380. https://doi.org/10.1126/science.abm6380.
Quinn J, Modell V, Orange JS, Modell F. Growth in diagnosis and treatment of primary immunodeficiency within the global Jeffrey Modell Centers Network. Allergy Asthma Clin Immunol. 2022;18(1):19. https://doi.org/10.1186/s13223-022-00662-6.
de Silva NR, Gunawardena S, Rathnayake D, Wickramasingha GD. Spectrum of primary immunodeficiency disorders in Sri Lanka. Allergy Asthma Clin Immunol. 2013;9(1):50. https://doi.org/10.1186/1710-1492-9-50.
Pan-Hammarstrom Q, Hammarstrom L. Antibody deficiency diseases. Eur J Immunol. 2008;38(2):327–33. https://doi.org/10.1002/eji.200737927.
Bousfiha AA, Jeddane L, Ailal F, et al. Primary immunodeficiency diseases worldwide: more common than generally thought. J Clin Immunol. 2013;33(1):1–7. https://doi.org/10.1007/s10875-012-9751-7.
Aluri J, Desai M, Gupta M, Dalvi A, Terance A, Rosenzweig SD, et al. Clinical, immunological, and molecular findings in 57 patients with severe combined immunodeficiency (SCID) from India. Front Immunol. 2019;10:23. https://doi.org/10.3389/fimmu.2019.00023.
Vignesh P, Rawat A, Kumrah R, Singh A, Gummadi A, Sharma M, Kaur A, et al. Clinical, immunological, and molecular features of severe combined immune deficiency: a multi-institutional experience from India. Front Immunol. 2021;11:619146. https://doi.org/10.3389/fimmu.2020.619146.
Vorsteveld EE, Hoischen A, van der Made CI. Next-generation sequencing in the field of primary immunodeficiencies: current yield, challenges, and future perspectives. Clin Rev Allergy Immunol. 2021;61(2):212–25. https://doi.org/10.1007/s12016-021-08838-5.
ESID - European Society for immunodeficiencies. Available at: https://esid.rg/Education/Diagnostic-Criteria-PID. Accessed 13 Jun 2022.
Feinberg J, Fieschi C, Doffinger R, Feinberg M, Leclerc T, Boisson-Dupuis S, Picard C, et al. Bacillus Calmette Guerin triggers the IL-12/IFN-gamma axis by an IRAK-4- and NEMO-dependent, non-cognate interaction between monocytes, NK, and T lymphocytes. Eur J Immunol. 2004;34(11):3276–84. https://doi.org/10.1002/eji.200425221.
Fernando SJA, Faiz NM, Handunnetti SM, De Silva AD, Dasanayake WMDK, Wickramasinghe GD, Karunatilake RMCH, et al. Preliminary study on chronic granulomatous disease in Sri Lanka. Allergy Asthma Clin Immunol. 2018;14:37. https://doi.org/10.1186/s13223-018-0264-7.
de Silva R, Dasanayake D, Senanayake M, Ediriweera R, Dias S, Karunatilleke C, Brocas K, et al. Hyper IgE recurrent infection syndrome in South Asia: is there a different outcome? Allergy Asthma Clin Immunol. 2018;14:70. https://doi.org/10.1186/s13223-018-0292-3.
Bradley LA, Sweatman AK, Lovering RC, Jones AM, Morgan G, Levinsky RJ, Kinnon C. Mutation detection in the X-linked agammaglobulinemia gene, BTK, using single strand conformation polymorphism analysis. Hum Mol Genet. 1994;3(1):79–83. https://doi.org/10.1093/hmg/3.1.79.
McDonald-McGinn DM, Sullivan KE. Chromosome 22q11.2 deletion syndrome (DiGeorge syndrome/velocardiofacial syndrome). Medicine. 2011;90(1):1–18. https://doi.org/10.1097/MD.0b013e318206046.
Abd Hamid IJ, Azman NA, Gennery AR, Mangantig E, Hashim IF, Zainudeen ZT. Systematic review of primary immunodeficiency diseases in Malaysia: 1979–2020. Front Immunol. 2020;11:1923. https://doi.org/10.3389/fimmu.2020.0192.
Mukhina AA, Kuzmenko NB, Rodina YA, Kondratenko IV, Bologov AA, Latysheva TV, Prodeus AP, et al. Primary immunodeficiencies in Russia: data from the National Registry. Front Immunol. 2020;11:1491. https://doi.org/10.3389/fimmu.2020.01491.PMID:32849507.
Belaid B, Mahammed L, Drali O, Oussaid AM, Touri NS, Melzi S, Dehimi A, et al. Inborn errors of immunity in Algerian children and adults: a single-center experience over a period of 13 years (2008–2021). Front Immunol. 2022;13:900091. https://doi.org/10.3389/fimmu.2022.90009.
El-Helou SM, Biegner AK, Bode S, Ehl SR, Heeg M, Maccari ME, Ritterbusch H, et al. The German national registry of primary immunodeficiencies (2012–2017). Front Immunol. 2019;10:1272. https://doi.org/10.3389/fimmu.2019.01272.
The French national registry of primary immunodeficiency diseases. Clin Immunol. 2010;135:264–72. https://doi.org/10.1016/j.clim.2010.02.021).
Lougaris V, Pession A, Baronio M, Soresina A, Rondelli R, Gazzurelli L, Benvenuto A, et al. The Italian registry for primary immunodeficiencies (Italian Primary Immunodeficiency Network; IPINet): Twenty Years of Experience (1999–2019). J Clin Immunol. 2020;40(7):1026–37. https://doi.org/10.1007/s10875-020-00844-0.
Shillitoe B, Bangs C, Guzman D, Gennery AR, Longhurst HJ, Slatter M, Edgar DM. The United Kingdom primary immune deficiency (UKPID) registry 2012 to 2017. Clin Exp Immunol. 2018;192(3):284–91. https://doi.org/10.1111/cei.13125.
Waleed AH, Al-Ahmad M, Al-Khabaz A, Husain A, Sadek A, Othman Y. The Kuwait national primary immunodeficiency registry 2004–2018. Front Immunol. 2019;10:1754. https://doi.org/10.3389/fimmu.2019.01754).
USNET https://usidnet.org/registry-data/stats-registry-enrollment/. Accessed 4 Jan 2023.
Abolhassani H, Kiaee F, Tavakol M, Chavoshzadeh Z, Mahdaviani SA, Momen T, Yazdani R, et al. Fourth update on the Iranian national registry of primary immunodeficiencies: integration of molecular diagnosis. J Clin Immunol. 2018;38(7):816–32. https://doi.org/10.1007/s10875-.
Al-Saud B, Al-Mousa H, Al Gazlan S, Al-Ghonaium A, Arnaout R, Al-Seraihy A, Elshorbagi S, et al. Primary immunodeficiency diseases in Saudi Arabia: a tertiary care hospital experience over a period of three years (2010–2013). J Clin Immunol. 2015;35(7):651–60. https://doi.org/10.1007/s10875-015-0197-6.
Aghamohammadi A, Rezaei N, Yazdani R, Delavari S, Kutukculer N, Topyildiz E, et al. Consensus Middle East and North Africa registry on inborn errors of immunity. J Clin Immunol. 2021;41:1339–51. https://doi.org/10.1007/s10875-021-01053-z.
El Hawary RE, Meshaal SS, Abd Elaziz DS, Alkady R, Lotfy S, Eldash A, Erfan A, Chohayeb EA, Saad MM, Darwish RK, Boutros JA, Galal NM, Elmarsafy AM. Genetic testing in Egyptian patients with inborn errors of immunity: a single-center experience. J Clin Immunol. 2022;42(5):1051–70. https://doi.org/10.1007/s10875-022-01272-y.
Premawardhena AP, De Silva ST, Goonatilleke MDDC, Ediriweera DS, Mettananda S, Rexan BK, Rodrigo P, et al. Marriage patterns in Sri Lanka and the prevalence of parental consanguinity in patients with β-thalassemia: a cross-sectional descriptive analysis. J Biosoc Sci. 2020;52(4):573–84. https://doi.org/10.1017/S0021932019000658.
Gathmann B, Binder N, Ehl S, Kindle G. ESID Registry Working Party. The European internet-based patient and research database for primary immunodeficiencies: update 2011. Clin Exp Immunol. 2012;167(3):479–91. https://doi.org/10.1111/j.1365-2249.2011.04542.
Benhsaien I, Ailal F, El Bakkouri J, Jeddane L, Ouair H, Admou B, Bouskraoui M, et al. Clinical and immunological features of 96 Moroccan children with SCID phenotype: two decades’ experience. J Clin Immunol. 2021;41(3):631–8. https://doi.org/10.1007/s10875-020-00960-x.
Stephan JL, Vlekova V, Le Deist F, Blanche S, Donadieu J, De Saint-Basile G, Durandy A, et al. Severe combined immunodeficiency: a retrospective single-center study of clinical presentation and outcome in 117 patients. J Pediatr. 1993;123(4):564–72. https://doi.org/10.1016/s0022-3476(05)80951-5.
Michos A, Tzanoudaki M, Villa A, Giliani S, Chrousos G, Kanariou M. Severe combined immunodeficiency in Greek children over a 20-year period: rarity of γ cchain deficiency (X-Linked) type. J Clin Immunol. 2011;31(5):778–83. https://doi.org/10.1007/s10875-011-9564-0.
Fazlollahi MR, Pourpak Z, Hamidieh AA, Movahedi M, Houshmand M, Badalzadeh M, Nourizadeh M, et al. Clinical, laboratory, and molecular findings for 63 patients with severe combined immunodeficiency:a decade’s experience. J Investig Allergol Clin Immunol. 2017;27(5):299–304. https://doi.org/10.18176/jiaci.0147.
van den Berg JM, van Koppen E, Ahlin A, Belohradsky BH, Bernatowska E, Corbeel L, Español T, Fischer A, Kurenko-Deptuch M, Mouy R, Petropoulou T, Roesler J, Seger R, Stasia MJ, Valerius NH, Weening RS, Wolach B, Roos D, Kuijpers TW. Chronic granulomatous disease: the European experience. PLoS One. 2009;4(4):e5234. https://doi.org/10.1371/journal.pone.0005234.
Blancas-Galicia L, Santos-Chávez E, Deswarte C, Mignac Q, Medina-Vera I, León-Lara X, Roynard M, et al. Genetic, immunological, and clinical features of the first Mexican cohort of patients with chronic granulomatous disease. J Clin Immunol. 2020;40(3):475–93. https://doi.org/10.1007/s10875-020-00750-5.
Rawat A, Vignesh P, Sudhakar M, Sharma M, Suri D, Jindal A, Gupta A, et al. Clinical, immunological, and molecular profile of chronic granulomatous disease: a multi-centric study of 236 patients from India. Front Immunol. 2021;12:625320. https://doi.org/10.3389/fimmu.2021.625320.
Cardenas-Morales M, Hernandez-Trujillo VP. Agammaglobulinemia: from X-linked to autosomal forms of disease. Clin Rev Allergy Immunol. 2021;9:1–14. https://doi.org/10.1007/s12016-021-08870-5.
de Beaucoudrey L, Samarina A, Bustamante J, Cobat A, Boisson-Dupuis S, Feinberg J, Al-Muhsen S, et al. Revisiting human IL-12Rβ1 deficiency: a survey of 141 patients from 30 countries. Medicine. 2010;89(6):381–402. https://doi.org/10.1097/MD.0b013e3181fdd832.
Taur PD, Gowri V, Pandrowala AA, Iyengar VV, Chougule A, Golwala Z, Chandak S, et al. Clinical and molecular findings in Mendelian susceptibility to mycobacterial diseases: experience from India. Front Immunol. 2021;12:631298. https://doi.org/10.3389/fimmu.2021.631298.
Errami A, Baghdadi JE, Ailal F, Benhsaien I, Bakkouri JE, Jeddane L, et al. Mendelian susceptibility to mycobacterial disease (MSMD): clinical, immunological, and genetic features of 22 patients from 15 Moroccan kindreds. J Clin Immunol. 2023;43:728–40. https://doi.org/10.1007/s10875-022-01419-x.
Peñafiel Vicuña AK, Yamazaki Nakashimada M, León Lara X, Mendieta Flores E, Nuñez Núñez ME, Lona-Reyes JC, Hernández Nieto L, et al. Mendelian susceptibility to mycobacterial disease: retrospective clinical and genetic study in Mexico. J Clin Immunol. 2023;43(1):123–35. https://doi.org/10.1007/s10875-022-01357-8.
Mahdaviani SA, Mansouri D, Jamee M, Zaki-Dizaji M, Aghdam KR, Mortaz E, Khorasanizadeh M, et al. Mendelian susceptibility to mycobacterial disease (MSMD): clinical and genetic features of 32 Iranian patients. J Clin Immunol. 2020;40(6):872–82. https://doi.org/10.1007/s10875-020-00813-7.
Depner M, Fuchs S, Raabe J, Frede N, Glocker C, Doffinger R, Gkrania-Klotsas E, et al. The extended clinical phenotype of 26 patients with chronic mucocutaneous candidiasis due to gain-of-function mutations in STAT1. J Clin Immunol. 2016;36:73e84. https://doi.org/10.1007/s10875-015-0214-9.
Jindal AK, Pilania RK, Rawat A, Singh S. Primary immunodeficiency disorders in India-a situational review. Front Immunol. 2017;19(8):714. https://doi.org/10.3389/fimmu.2017.00714.
Gupta S, Sehgal S. Editorial: advances in primary immunodeficiencies in India. Front Immunol. 2021;24(12):701335. https://doi.org/10.3389/fimmu.2021.701335.
Taur PD, Gowri V, Pandrowala AA, Iyengar VV, Chougule A, Golwala Z, Chandak S, et al. Clinical and molecular findings in Mendelian susceptibility to mycobacterial diseases: experience from India. Front Immunol. 2021;12:631298. https://doi.org/10.3389/fimmu.2021.631298.
Boisson-Dupuis S, Bustamante J. Mycobacterial diseases in patients with inborn errors of immunity. Curr Opin Immunol. 2021;72:262–71. https://doi.org/10.1016/j.coi.2021.07.001.
Mellouli F, Mustapha IB, Khaled MB, Besbes H, Ouederni M, Mekki N, Ali MB, et al. Report of the Tunisian registry of primary immunodeficiencies:25-years of experience (1988–2012). J Clin Immunol. 2015;35(8):745–53. https://doi.org/10.1007/s10875-015-0206-950.
Abolhassani H, Azizi G, Sharifi L, Yazdani R, Mohsenzadegan M, Delavari S, Sohani M, et al. Global systematic review of primary immunodeficiency registries. Expert Rev Clin Immunol. 2020;16(7):717–32. https://doi.org/10.1080/1744666X.2020.1801422.
Ismaili-Jaha V, Kuli-Lito G, Spahiu-Konjusha S, Baloku A, Maródi L. Through education and collaboration to better care for primary imunodeficiencies in Albania and Kosovo. J Clin Immunol. 2022;1–5. https://doi.org/10.1007/s10875-022-01409-z
Acknowledgements
We thank the Jeffrey Modell Foundation for providing next generation sequencing for some patients, The Binding Site, Birmingham, UK, for providing typhoid VI antibody testing kits, and Dr. Nalini Withana for providing DNA extraction kits.
Funding
The Laboratory of Human Genetics of Infectious Diseases is supported in part by institutional grants from INSERM, the University of Paris Cité, the St. Giles Foundation, and The Rockefeller University, the Center for Clinical and Translational Science grant number UL1TR001866 from the National Center for Research Resources and the National Center for Advancing Sciences (NCATS), National Institutes of Health (NIH), the National Institute of Allergy and Infectious Diseases, NIH (R01AI095983), a grant from the French Foundation for Medical Research (FRM) and grants from the French National Research Agency (ANR) under the “Investments for the future” program (ANR-10-IAHU-01) and GENMSMD (ANR-16-CE17-0005-01). Y-L L is supported by the Hong Kong Society for the Relief of Disabled Children for his research in inborn error of immunity. The Jeffrey Modell Foundation has sponsored next generation sequencing for some patients.
Author information
Authors and Affiliations
Contributions
RdS and DD conceptualized the study and performed data analysis. JB, S B-D, AP, J-LC, K-WC, and Y-LL performed genetic studies. RD and DSK did cytokine assays. RdS drafted the manuscript. CK provided the data. JT helped in genetic diagnosis. All authors critically reviewed the manuscript and approved the submitted version.
Corresponding author
Ethics declarations
Ethics Approval
The study was reviewed and approved by the Ethics Committee of the Medical Research Institute (28/2020 and extended in January 2023).
Consent to Participate
This is a retrospective study of existing data. Written informed consent to participate in genetic testing and publishing the results was provided by the participant or parent/legal guardian.
Consent for Publication
Consent for publication is given.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dasanayake, D., Bustamante, J., Boisson–Dupuis, S. et al. Inborn Errors of Immunity—the Sri Lankan Experience 2010–2022. J Clin Immunol 43, 1858–1872 (2023). https://doi.org/10.1007/s10875-023-01542-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10875-023-01542-3