Abstract
Background
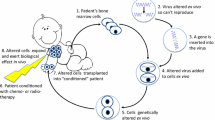
X-linked inhibitor of apoptosis protein (XIAP) deficiency is a severe immunodeficiency with clinical features including hemophagocytic lymphohistiocytosis (HLH) and inflammatory bowel disease (IBD) due to defective NOD2 responses. Management includes immunomodulatory therapies and hematopoietic stem cell transplant (HSCT). However, this cohort is particularly susceptible to the chemotherapeutic regimens and acutely affected by graft-vs-host disease (GvHD), driving poor long-term survival in transplanted patients. Autologous HSC gene therapy could offer an alternative treatment option and would abrogate the risks of alloreactivity.
Methods
Hematopoietic progenitor (Lin−ve) cells from XIAPy/− mice were transduced with a lentiviral vector encoding human XIAP cDNA before transplantation into irradiated XIAP y/− recipients. After 12 weeks animals were challenged with the dectin-1 ligand curdlan and recovery of innate immune function was evaluated though analysis of inflammatory cytokines, body weight, and splenomegaly. XIAP patient-derived CD14+ monocytes were transduced with the same vector and functional recovery was demonstrated using in vitro L18-MDP/NOD2 assays.
Results
In treated XIAPy/− mice, ~40% engraftment of gene-corrected Lin−ve cells led to significant recovery of weight loss, splenomegaly, and inflammatory cytokine responses to curdlan, comparable to wild-type mice. Serum IL-6, IL-10, MCP-1, and TNF were significantly reduced 2-h post-curdlan administration in non-corrected XIAPy/− mice compared to wild-type and gene-corrected animals. Appropriate reduction of inflammatory responses was observed in gene-corrected mice, whereas non-corrected mice developed an inflammatory profile 9 days post-curdlan challenge. In gene-corrected patient CD14+ monocytes, TNF responses were restored following NOD2 activation with L18-MDP.
Conclusion
Gene correction of HSCs recovers XIAP-dependent immune defects and could offer a treatment option for patients with XIAP deficiency.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
X-linked inhibitor of apoptosis protein (XIAP) deficiency is a primary immunodeficiency caused by mutations in the XIAP gene, and is estimated to occur in 1–2 per million live births [1, 2]. XIAP deficiency was first described in 2006 in association with recurrent hemophagocytic lymphohistiocytosis (HLH), now additional manifestations are being frequently recognized including inflammatory bowel disease (IBD), hypogammaglobulinemia, severe recurrent infections, autoimmunity, cytopenias, and other inflammatory complications [1, 3,4,5,6].
Given the range of clinical symptoms and disease course, there are no standardized treatment guidelines, and thus therapeutic intervention is primarily guided by clinical manifestations and includes immunosuppression and immunomodulatory drugs [7]. Currently, the only curative treatment option for XIAP deficiency is allogeneic hematopoietic stem cell transplantation (HSCT). In patients with severe disease, including HLH and severe refractory IBD, HSCT is often considered. However, early reports demonstrated poor transplant outcomes in this disease, with long-term survival below 50% [8]. Myeloablative conditioning (MAC) regimens were associated with poor long-term survival, (43% 5-year overall survival) particularly in the context of HLA-mismatched donors or ongoing HLH at time of transplantation [8]. More recent reports of reduced-intensity conditioning (RIC) regimens suggest these approaches are better tolerated with improved survival [8,9,10]. However, HSCT is associated with graft-versus-host disease (GvHD), which significantly increases the risk of mortality in patients with XIAP deficiency [9]. Autologous hematopoietic stem cell (HSC) gene therapy abrogates any risk of alloreactivity due to GvHD making it an extremely attractive potential therapy. For over 20 years, autologous HSC gene therapy has been a promising treatment option for specific immune disorders [11,12,13,14,15,16], and this success continues to promote the development of new gene therapy approaches for other monogenic immune disorders including several forms of familial HLH [17,18,19,20].
XIAP is an antiapoptotic protein that regulates cell death in response to apoptotic stimuli by directly inhibiting caspase-3, caspase-7, and caspase-9 via its N-terminal baculoviral IAP repeat (BIR) domains [21,22,23,24]. As such, T cells from XIAP deficient patients, including invariant natural killer T cells (iNKT) and mucosal-associated invariant T (MAIT) cells which express elevated levels of caspases that are inhibited by XIAP, have an increased sensitivity to activation-induced cell death (AICD) [1, 5, 6, 25]. Although blood lymphocyte cell numbers may be within normal ranges [2], it is thought that suboptimal expansion of virus-specific T cells occurs following infection in XIAP deficient patients [2, 5,6,7]. XIAP is also involved in other immune signaling pathways essential for innate immune responses. The RING and BIR2 domains of XIAP are required for nuclear factor-κB (NF-κB) and mitogen-activated protein kinase (MAPK) signaling in response to activation of nucleotide-binding oligomerization domain 1 (NOD1) and NOD2 [26, 27]. Several studies have shown that peripheral monocytes from XIAP-deficient patients have compromized cytokine production, including TNF and IL-8, in response to NOD2 ligands, while TLR-2 and TLR-4 receptor stimulation is unaffected [3, 28, 29]. Impaired NOD2 signaling is implicated in the development of IBD in XIAP deficiency. In addition, serum levels of pro-inflammatory cytokines, including IL-6, IL-2, IFN-γ, and TNF are elevated in XIAP-deficient patients with HLH [30]. IL-18 levels are significantly elevated during HLH in XIAP deficiency and remain chronically elevated during remission [30, 31].
XIAP is known to play a role in dectin-1 signaling, a transmembrane pattern recognition receptor (PRR) involved in antifungal immunity through β-glucan recognition [32, 33]. The observations by Hsieh et al. demonstrate that XIAP-deficient mice have impaired innate immune responses following dectin-1 priming, which result in XIAP deficiency-like features [32]. XIAP is also an important regulator of the NLRP3 inflammasome. Studies show loss of XIAP result in dysregulated caspase-1/NLRP3 inflammasome activation, which is associated with overproduction of pro-inflammatory cytokines and cell death [25, 34,35,36]. Furthermore, XIAP prevents TNF-mediated, receptor-interacting protein 3 (RIPK3)-dependent cell death, by regulating RIPK1 ubiquitylation, and inhibiting inflammatory cell death [34].
Due to the role of XIAP in preventing cell death, over-expression of XIAP can enhance cell tolerance to external and internal apoptotic stimuli [37], and dysregulation of XIAP has been shown to contribute toward the progression of multiple cancers, including bladder [38,39,40], breast [41,42,43], ovarian [44,45,46], lung [47,48,49], colon [50,51,52], and prostate [53,54,55,56]. Therefore, the expression profile of XIAP is thought to be part of a system of regulatory loops that balance a cell’s response to environmental stimuli [37, 57]. In addition to its anti-apoptotic function, extensive studies suggests that XIAP is important for both the clearance of pathogens and the regulation of inflammatory responses.
To address the treatment challenges in this condition, we generated a self-inactivating lentiviral vector containing human XIAP cDNA under the control of a spleen focus forming virus (SFFV) promoter, as well as a GFP reporter gene (LV-SFFV-XIAP-GFP) and investigated whether gene transfer could correct immune abnormalities and phenotype in a murine model of the disease and XIAP-deficient patient cells. Here for the first time, we show that lentiviral mediated gene correction can recover immune defects associated with XIAP deficiency, providing proof of principle for an autologous HSC gene therapy treatment approach.
Methods
Mice
All animal studies were approved by the Institutional Research Ethics Committee (Great Ormond Street Institute of Child Health, University College London [UCL], UK) and licensed under the Animals (Scientific Procedures) Act 1986 (Home Office, London, United Kingdom). XIAP-deficient mice (XIAPy/−) have been previously described [58]. Mice were housed in single ventilated cages, in pathogen-free conditions, and given ad libitum access to food and water. XIAPy/− mice were bred as heterozygous, and littermates were genotyped to identify homozygous and wild-type control mice.
Vector Constructs and Copy Number Analysis
Murine and human cell experiments were carried out by using a third-generation lentiviral vector on a pCCL backbone containing codon-optimized human XIAP cDNA driven by the spleen focus-forming virus (SFFV) promoter, internal ribosomal entry site, and eGFP or eGFP alone (SFFV-XIAP-eGFP; SFFV-eGFP). Lentiviral particles were produced, vesicular stomatitis virus glycoprotein G (VSV-G) pseudotyped and titered in HEK293T cells as previously described [59]. Lentiviral integration were quantified using a TaqMan real-time PCR assay targeting the WPRE region in the lentiviral vector and murine titin or human β-actin genomic regions in cells. A stable XIAP knockdown THP-1 (human monocytic leukemia) cell line was generated by transducing wild-type THP-1 with a pGIPZ lentiviral vector containing either a miR-30 shRNA sequence targeting XIAP (Clone 302,102), or non-silencing random control shRNA sequence (Open Biosystems). In both constructs, a co-expressed GFP cassette allowed for FACSorting transduced cells. Genomic DNA was extracted from cell pellets using a DNeasy Blood and Tissue kit (QIAGEN, West Sussex, UK) following the manufacturer’s guidelines. Average vector copy number per cell was determined by multiplex qPCR using a gBLOCK standards curve (Integrated DNA Technologies).
Cell Cultures and Cytokine Assessments
The THP-1 (human monocytic leukemia) cell line was maintained in RPMI 1640 medium (Invitrogen, Paisley, UK) supplemented with 10% fetal bovine serum (FBS, Sigma-Aldrich, Poole, UK) and 10 μg/mL each of penicillin and streptomycin (pen/strep, Invitrogen), while HEK293T cells were maintained in 10% FBS and 1% pen/strep Dulbecco’s modified Eagle’s medium (DMEM, Invitrogen). THP-1 cells were seeded at a density of 1.0 × 106 cells/well in a 12-well plate and differentiated into macrophages in the presence of 10 ng/mL phorbol 12-myristate 13-acetate (PMA) for 48 h. Cells were then washed and cultured in complete RPMI media for a further 48 h prior to NOD2/TLR/dectin-1 stimulation (See Supplemental Information). XIAPy/− bone marrow-derived macrophages (BMDM) were generated as previously described [34, 60]. For BMDM stimulations, cells were harvested on day 7 and seeded at a density of 4.0 × 105 cells/well in a 24-well plate. All cells were cultured at 37 °C at 5% CO2. Cytokines were measured by ELISA Ready-SET-Go kit (eBioscience, Carlsbad, CA) and Cytometric Bead Array (BD Biosciences).
HSC Reconstitution and Curdlan Challenge
For murine reconstitution studies, lineage-negative (Lin−ve) cells were isolated from XIAPy/− bone marrow and purified by negative selection using MACS Lineage Cell Depletion Kits (Miltenyi Biotec). Lin−ve cells were transduced at a multiplicity of infection (MOI) of 75 using spinoculation (45 min at 1500 g) and cultured in StemSpam medium enriched with 100 ng/mL mSCF, 100 ng/mL mFlt3, 25 ng/mL hTPO (all PeproTech, Rocky Hill, NJ, USA), 2% FBS and 1% pen/strep. Seventy-two hours after transduction, cells were harvested and analyzed by flow cytometry (LSRII; BD, San Jose, CA) for transduction efficiency. A colony-forming unit (CFU) assay was performed in MethoCult GF M3434 (STEMCELL Technologies, Grenoble, France). Recipient XIAPy/− mice were lethally irradiated with 6 Gray (Gy) + 4 Gy in 2 consecutive days, and 5.0 × 105 gene-corrected Lin−ve cells/mouse was intravenously (i.v.) injected into pre-conditioned mice. Eight weeks after reconstitution, mice were challenged through intraperitoneal injections with the dectin-1 ligand curdlan as previously described [32].
Patient Samples
Consent was obtained to use samples from 3 unrelated patient donors. All patients had confirmed mutations in XIAP (P1, age 8, exon 3 and 4 deletion; P2, age 4, c.712 C > T pArg238 stop codon; and P3, age 39, c.1396 G > T).
Flow Cytometry, XIAP Staining and L18-MDP Assay
Single-cell suspensions were prepared from murine peripheral blood and splenic tissue. Cells were freshly stained for 30 min at room temperature with various antibodies: hamster anti-mouse CD11c APC (HL3), hamster anti-mouse CD3 APC-Cy7 (45-2C11), mouse anti-mouse NK-1.1 BV421 (PK136), rat anti-mouse CD11b PE-Cy7 or BV421 (M1/70), rat anti-mouse CD4 PerCP-Cy5.5 (RM4-5), rat anti-mouse CD45R/B220 APC (RA3-6B2), rat anti-mouse CD8 V500 (53–6.7), rat anti-mouse F4/80 PE-Cy7 (T45-2343) and, rat anti-mouse Gr-1 BV421 (RB6-8C5). The dimension reduction algorithm tSNE was applied to flow cytometry data (~20,000 cells per sample) from total splenocytes of curdlan-challenged animals using default parameters (iterations: 1000, perplexity: 30 and KNN algorithm: vantage point tree) in FlowJo™ v10.8 Software (BD Life Sciences). For human peripheral blood mononuclear cells (PBMC) isolation, red blood cell (RBC) lysis was performed with RBC lysis buffer (BioLegend, San Diego, CA, USA), and CD14+ monocytes were purified by positive selection using CD14 MicroBeads (Miltenyi Biotec) as per manufacturer’s guidelines. For intracellular XIAP staining, after fixation and permeabilization (IntraPrep; Beckman Coulter, Fullerton, CA), cells were incubated either with a mouse anti-human/mouse XIAP (clone 48) or the corresponding isotype control mouse IgG1, κ (both from BD Biosciences, San Jose, CA, USA). Human PBMC-derived CD14+ were transduced at an MOI of 20 in the presence of virion-like particles carrying Vpx (kindly provided by Giorgia Santilli). Gene-modified CD14+ cells were cultured for 72 h with 50 ng/mL macrophage colony-stimulating factor and analyzed by flow cytometry for transduction efficiency, and XIAP protein reconstitution. The L18-MDP assay was then carried out to determine correction of NOD2 responses in patient cells as previously described [61].
Statistical Analysis
Statistical analysis was performed with GraphPad Prism 6.0 software (GraphPad Software, La Jolla, CA). Statistical significance for murine experiments was determine by using 2-way ANOVA. To determine statistical significance for in vitro assays, appropriate nonparametric testing was used, including Kruskal–Wallis multiple comparison tests, and Mann–Whitney 2-tailed Student t tests assuming non-Gaussian distribution. The significance level is shown as follows: ∗ P < 0.05, ∗ ∗ P < 0.01, ∗ ∗ ∗ P < 0.001, ∗ ∗ ∗ ∗ P < 0.0001.
Restoration of Cytokine Defects in XIAP-Deficient Myeloid Cells
We generated a self-inactivating lentiviral vector with a pCCL backbone that has been frequently used in gene therapy clinical trials [62, 63] containing codon-optimized human XIAP cDNA under the transcriptional control of the SFFV promoter and an eGFP reporter gene (LV-SFFV-XIAP-GFP). To investigate whether XIAP transgene expression can correct innate immune responses in myeloid cells, we transduced THP-1 XIAP knockdown cells (sh-XIAP) and XIAPy/− bone marrow-derived macrophages (BMDMs) using the LV-SFFV-XIAP-GFP vector alongside a GFP control vector (LV-SFFV-GFP) (Fig. 1A). NOD2- and dectin-1-mediated inflammatory responses were successfully restored by XIAP gene transfer (Fig. 1B, C). To study cytokine responses, knockdown THP-1 cells were differentiated into macrophages in the presence of PMA and stimulated with PRR agonists. A striking reduction in TNF secretion was observed in XIAP-deficient THP-1 cells (P < 0.001), which was restored to control levels following transduction with the LV-SFFV-XIAP-eGFP construct (Fig. 1B; left panel). Stimulation with TLR ligands as a positive control induced TNF secretion in XIAP-deficient THP-1 cells (Fig. 1B; right panel).
Correction of NOD2 and dectin-1 innate immune responses in myeloid cells. A Schematic representation of LV vectors containing human XIAP cDNA driven by the SFFV promoter and eGFP or SFFV-eGFP only. B PMA-differentiated THP-1 cells were treated for 2 h with NOD2/TLR/dectin-1 ligands (See Supplemental Information). ctr, control. Secreted TNF in gene-correct THP-1 macrophages. C A stable XIAP knockdown human monocytic cell THP-1 was established and transduced using SFFV-XIAP-eGFP or SFFV-eGFP vectors at an MOI of 20. Transduction efficiency ranged between 65 to 77% (data not shown). D Recovery of NOD2- and dectin-1-indiced TNF, IL-6, and MCP-1 production in gene-corrected XIAPy/− BMDMs were quantified by Cytokine Bead Array. BMDMs were treated for 4 h with NOD2/TLR/dectin-1 ligands (See Supplemental Information). XIAPy/− BMDMs were transduced using SFFV-XIAP-eGFP or SFFV-eGFP vectors at an MOI of 20. Transduction efficiency ranged between 50 and 84% (see Supplemental Fig. 1B), with a vector copy number of 3 to 4 copies per cell. Data are shown as means ± SEM of three independent experiments (n = 3 mice per group) performed in triplicates
Other studies have shown attenuated inflammatory responses in XIAPy/− BMDMs in response to NOD2 [26, 34] and dectin-1 stimulation [32], so we next investigated whether gene-corrected BMDMs were able to efficiently regain their innate inflammatory responses in a XIAP-dependent manner. Since XIAP is important for NOD2- and dectin-1-mediated inflammatory responses, we observed reduced IL-6, MCP-1 and TNF secretion following NOD2 and dectin-1 stimulation (Fig. 1D, See Supplemental Information) but not TLR-4 stimulation in XIAPy/− BMDMs as expected. Following lentiviral-mediated XIAP gene transfer, cytokine responses in gene-corrected XIAPy/− BMDMs were restored to levels comparable to BMDMs from wild-type (WT) littermates. Transduction efficiency ranged between 50 and 84% (see Supplemental Fig. 1B), with a vector copy number of 3–4 copies per cell. Indeed, successful protein reconstitution in XIAPy/− BMDMs using our LV-SFFV-XIAP-eGFP vector was able to restore NOD2- and dectin-1-mediated secretion of IL-6, MCP-1 and TNF compared to XIAPy/− BMDMs transduced with SFFV-eGFP only (Fig. 1D, Supplemental Fig. 1A, B). These findings indicate that lentiviral gene transfer in myeloid cells can reconstitute specific innate immune responses associated with XIAP deficiency.
XIAP Gene Transfer to HSCs Restores Innate Immune Function in an In vivo Murine Model
Priming of XIAPy/− mice with the dectin-1 ligand curdlan induces features of XIAP deficiency, including compromized early innate responses to curdlan followed by elevated levels of proinflammatory cytokines which invariably result in splenomegaly and cachexia [32]. Following rescue of immune function in XIAP-deficient myeloid cells using our LV-SFFV-XIAP-eGFP vector, we next conducted in vivo studies to test the vector in an established murine model of XIAP deficiency (Fig. 2A). Bone marrow was isolated from XIAPy/− donor animals and enriched for Lin−ve cells, which were transduced with either the LV-SFFV-eGFP or LV-SFFV-XIAP-eGFP vector at an MOI of 75. 2 × 105 gene-corrected donor XIAPy/− Lin−ve cells were then transferred into lethally irradiated XIAPy/− recipients (transduction efficiency 51–81% for both XIAP and GFP control vectors, respectively; Supplemental Fig. 2A and B). Lentiviral-mediated gene transfer did not adversely affect colony formation (Fig. 2B).
Experimental design of the gene-corrected HSC transfer and curdlan challenge model in XIAPy/− mice. A Timeline of gene-corrected HSC transfer experiments following irradiation (6 Gy + 4 Gy in 2 consecutive days) on day 0 with intravenous infusion of murine Lin−ve cells transduced with SFFV-XIAP-eGFP or SFFV-eGFP vectors at an MOI of 75. B Transduced Lin−ve cells that were not used for transplants remained in culture for CFU assays. C Animals underwent tail vein bleeds at 8 weeks to assess peripheral donor cell engraftment before immunologic challenge at week 12 with the dectin-1 curdlan. Level of eGFP expression and (D), reconstitution of XIAP protein in PBMCs isolated from transplanted XIAPy/− animals at 8 weeks, with an average vector copy number of 3 copies per cell, for both vectors (n = 4 mice per group). Protein expression was analyzed by using intracellular fluorescence-activate cell sorting staining. Solid line, Control IgG1κ; dotted line, anti-XIAP antibody
After 8 weeks, engraftment was assessed (eGFP and XIAP expression, and vector copy number in peripheral blood) (Fig. 2C, D and Supplemental Fig. 2C) and recovery of different hematopoietic cell lineages in the periphery was similar in all irradiated animals (Supplemental Fig. 2D). The average vector copy number in PBMCs was 3 viral copies per cell, for both LV-SFFV-eGFP and LV-SFFV-XIAP-eGFP vectors. At 12 weeks after infusion of gene-corrected HSCs, XIAPy/− mice were challenged with the dectin-1 ligand curdlan and analyzed at 2-h post-challenge and again 9 days later to investigate immune responses, including serum cytokines, splenomegaly and myeloid cell infiltration, as well as loss of body mass. Mice were sacrificed after 9 days and engraftment was measured by eGFP expression in blood, bone marrow, spleen, liver, and thymus (Supplemental Fig. 2E).
In XIAPy/− mice reconstituted with LV-SFFV-eGFP only vector, a single peritoneal administration of curdlan induced body mass loss that was not recovered by day 9 (Fig. 3A), consistent with data from Hsieh et al. [32]. WT and gene-corrected XIAPy/− animals regained their body weight within a week following curdlan administration. At 2-h blood sampling, serum levels of IL-6 (P = 0.03), IL-10 (P = 0.001), MCP-1 (P = 0.0002), and TNF (P = 0.002) were reduced in XIAP-deficient mice; however, we observed significantly higher cytokines responses in WT and gene-corrected animals compared with those receiving the eGFP control vector (Fig. 3B). Splenomegaly was observed in XIAPy/− mice reconstituted with the SFFV-eGFP only vector compared to WT and gene-corrected XIAPy/− animals, which was associated with infiltrating neutrophils and macrophages (Fig. 3D–G). Moreover, we were able to demonstrate appropriate cessation of inflammatory cytokines in gene-corrected mice, whereas XIAPy/− animals reconstituted with the SFFV-eGFP only vector developed an inflammatory cytokine profile 9 days after curdlan injection (Fig. 3C). XIAPy/− mice receiving HSCs transduced with LV-SFFV-XIAP-eGFP vector exhibited weight loss, spleen size and histology and cytokine profiles comparable to WT mice. Our findings indicate that lentiviral gene therapy can recover the major defects of innate immunity in XIAPy/− mice.
Intravenous infusion of gene-corrected HSCs from XIAP-deficient mice restores immune function in a dectin-1 ligand curdlan challenge model. A Recovery of body weight in XIAPy/− mice transplanted with SFFV-XIAP-eGFP-transduced HSCs. Male mice (12 weeks after reconstitution) were challenged with intraperitoneal administration of curdlan (5 mg/20 g body weight), and body weight was measured daily; n = 4 mice per group. B Restored inflammatory cytokine production in gene-corrected XIAPy/− animals following curdlan priming. Serum was collected via tail vein bleeding 2 h after curdlan administration, and the levels of IL-6, IL-10, MCP-1 and TNF-α was quantified and (C), repeated 9 days later. Increased inflammatory cytokine secretion in XIAPy/− mice transplanted with SFFV-eGFP-transduced HSCs (mock vector) 9 days after curdlan challenge; n = 4 mice per group. D Gene-correction rescues curdlan-induced splenomegaly in XIAPy/− mice. Spleens were harvested from all animals 9 days after intraperitoneal curdlan stimulation for size and (E), weight comparison. F Sections of spleen (4 μm) were stained with hematoxylin and eosin. One representative image from each group is shown; n = 4 mice per group. Bar indicates 50 μm. G Dimension reduction analysis showing macrophage and neutrophil infiltration 9 days after curdlan challenge. Representative analyses of WT, XIAPy/−, uncorrected XIAPy/− (eGFP), and gene-corrected XIAPy/− (XIAP-eGFP) animals are shown. Total splenocytes were prepared from the spleen in mice from D and stained with anti-F4/80 and anti-Gr-1. The population of macrophages (Gr-1−/int F4/80+) and neutrophils (Gr-1+F4/80−) was determined by flow cytometry
XIAP Gene Transfer Restores NOD2 Innate Immune Responses in Patient Monocytes
To investigate the human relevance of the data generated in the XIAP-deficient murine model, we tested whether restoration of XIAP expression in patient-derived CD14+ monocytes could reconstitute NOD-2-dependent innate immune function, using the functional assay previously described by Ammann et al. [61]. All patients, including two pediatric and one adult patient, were confirmed to have XIAP deficiency by Sanger sequencing and demonstrated abnormal intracellular XIAP expression. Patient CD14+ monocytes were isolated from PBMCs and transduced with either the LV-XIAP-SFFV-eGFP or LV-SFFV-eGFP control vector at an MOI of 20 (transduction efficiency 57–80%). Transduction with the LV-SFFV-XIAP-eGFP vector was able to restore XIAP protein expression in patient CD14+ monocytes, which was comparable to healthy donor monocytes as measured by intracellular staining (Fig. 4). Total XIAP-expressing monocytes in healthy donor and patient corrected cells were 56% and 69%, respectively (P = 0.14).
XIAP gene transfer restores NOD2 immune responses in CD14+ monocytes of patients with XIAP deficiency. A Representative flow cytometric contour plots of TNF-production in mock-transduced monocytes from healthy donors (HD) and patients (n = 3), and (B, C), TNF-producing monocytes from patients transduced with corrective lentiviral XIAP vector. Transduction efficiency was assessed by using flow cytometry; eGFP expression ranged from 57 to 80% (data not shown), with an average vector copy number of 1 copy per cell. Monocytes were cultured in the presence of medium only, L18-MDP (200 ng/mL) or LPS (200 ng/mL) for 2.5 h. TNF-producing monocytes were defined by forward-/side-scatter, surface expression of CD14 and human leucocyte antigen D-related (HLA-DR). The percentages indicate the fraction of TNF-positive cells of all HLA-DR+CD14+ monocytes. D XIAP expression in uncorrected and gene-corrected cells from patients, as analyzed by using intracellular fluorescence-activate cell sorting staining. Solid line, Control IgG1κ; dotted line, anti-XIAP antibody. E The Percentage (left) and mean fluorescence intensity (MFI) (right) of XIAP+ cells within the HLA-DR+CD14.+ monocyte population was assessed by flow cytometry in HD or patient monocytes transduced with corrective lentiviral XIAP vector (n = 3)
Following successful protein reconstitution, we next sought to determine if gene-corrected patient CD14+ monocytes regain their NOD2-dependent innate immune function in response to L18-MDP stimulations, an inflammatory response primary mediated by monocytes following NF-κB activation downstream of NOD2 [64]. TNF responses in patient-derived CD14+ monocytes transduced with LV-SFFV-eGFP were severely reduced in all patients (Fig. 4A), whereas gene-corrected patient monocytes transduced with LV-SFFV-XIAP-eGFP with an average vector copy number of 1 viral copy per cell demonstrated significantly higher levels of TNF+ cells in response to L18-MDP stimulation (P = 0.003) and are comparable to healthy controls (Fig. 4B–E). These data suggest gene-correction in CD14+ monocytes rescue innate inflammatory responses following NOD2 pathway stimulation. Moreover, our data supports the use of gene-correction strategies as an alternative treatment option for patient with XIAP deficiency.
Discussion
Hematopoietic stem cell gene therapy has been used successfully to treat a number of monogenic immunological, hematological and metabolic diseases [11,12,13,14,15,16, 65,66,67], and offers a curative treatment option for patients lacking a suitable donor for HSCT. XIAP deficiency is an inborn error of immunity with a range of severe manifestations, and even when diagnosed early, provision of prophylactic therapies and close monitoring may not prevent fatal complications such as HLH. Outcomes following HSCT are significantly worse in patients with XIAP deficiency than those with other familial forms of HLH and even low grade GvHD is associated with disproportionate mortality [8, 9, 68]. Studies by Marsh et al. [8] and Varghese et al. [68] show high levels of toxicity following conventional myeloablative conditioning, likely due to loss of XIAP. A high incidence of GvHD, mixed donor chimerism (< 95%) and relapsed HLH post-HSCT have been observed when using RIC-HSCT [9]. As such, development of autologous gene therapy strategies can offer patients lacking suitable donors an alternative clinical option which removes any risk of alloreactivity and allows the use of reduced toxicity conditioning.
Here, we provide evidence that transfer of gene-corrected hematopoietic progenitors can correct innate immune responses associated with XIAP deficiency in a murine model, which could translate to therapeutic benefit. Further proof of concept is shown by correction of impaired immune function in CD14+ patient monocytes with normalization of cytokine responses following XIAP gene transfer with an average copy number of 1 viral copy per cell. This is supported by in vitro studies of XIAP-deficient THP-1 cells and BMDMs from the established XIAPy/− murine model showing that gene-correction leads to rescue of both NOD2- and dectin-1-mediated cytokine responses.
Using a previously described curdlan challenge model [32], we have shown in vivo transfer of XIAP gene-corrected HSCs results in recovery of dectin-1-dependent innate immunity through specific cytokine responses, which are dysregulated in XIAP-deficient mice following curdlan administration. Early production of proinflammatory cytokines (IL-6, MCP-1 and TNF) following dectin-1 stimulation suggest the initial inability of XIAPy/− mice to mount an effective innate immune response to curdlan but this was restored in gene-corrected animals. Moreover, gene-corrected animals did not demonstrate continued stimulation accompanied by accumulation of proinflammatory cytokines leading to cachexia and splenomegaly, which were markedly infiltrated by macrophages and neutrophils, unlike their non-corrected littermates. Restoration was achievable at levels of engraftment close to 40%; a clinically feasible level of correction in patients from our experience with other lentiviral gene therapy trials for inborn errors of immunity (IEI). Together, these data suggest that HSC gene therapy could be of considerable clinical benefit to XIAP-deficient patients presenting with severe inflammatory conditions such and HLH and IBD.
Our data also confirm that lentiviral-mediated XIAP gene transfer can correct innate immune defects in CD14+ monocytes from patients in the context of NOD2 signaling. We reliably show that gene-corrected CD14+ monocytes from patients can induce NOD2-mediated immune responses through ex vivo functional assays where L18-MDP-induced TNF production can be restored to healthy donor levels in patient-corrected cells (60% vs 56%, respectively) compared to only 6% response in uncorrected patient cells.
The murine model has some limitations but is still a valuable preclinical model. XIAP-deficient mice have not been shown to have a susceptibility to develop IBD or HLH like their human counterparts, but instead have compromized immunity leading to decreased survival under certain infectious conditions [2, 7]. Defects in NOD2- and dectin-1-mediated cytokine production by XIAP-deficient myeloid cells has been associated with compromized innate immunity to L. monocytogenes and C. albicans, respectively [32, 69]. Interestingly, XIAP-deficient mice challenged with MHV-68 as a surrogate for EBV infection, or C. albicans developed splenomegaly with increased levels of proinflammatory cytokines [32, 34]. In these models, splenomegaly occurs secondarily to the innate immune defect, which could be dependent of high levels of inflammation due to the persistence of pathogens [2].
The robust data presented here demonstrates correction of the inflammatory phenotype following gene transfer into HSCs. The cytokine profile reported in XIAPy/− mice recapitulates those observed in patients [32, 34, 60], and therefore our data suggests that we could improve the pro-inflammatory status and clinical manifestations of XIAP deficiency. Although the majority of HLH in patients reported in earlier series were triggered by EBV infections [70,71,72], the exact mechanism for the development of HLH in XIAP deficiency is currently poorly understood but is it likely that dysregulated innate immune responses and cytokine production play a role.
For these studies, we used a lentiviral vector with the XIAP transgene under transcriptional control of the SFFV promoter, which is a viral promoter and not suitable for clinical use given the increased risk of insertional mutagenesis and clonal events with viral regulatory elements [73,74,75,76]. We investigated numerous promoter elements currently in clinical use (including MND, EFS and PGK promoters) but were unable to achieve sufficient XIAP expression levels to correct the immune defects described here. Reassuringly, we did not observe any detrimental effects of XIAP ‘overexpression’ in murine HSC function and hematopoietic development, but experiments were not specifically designed to assess tumorgenicity. While this data serves as proof of concept that corrective gene transfer ameliorates the immune abnormalities seen in this condition, with the highly regulated expression profile of XIAP in immune lineages, achieving as close to a physiological expression profile will be crucial. Thus, we are now focusing our efforts on targeted gene editing platforms to precisely correct the XIAP gene in situ, allowing expression from endogenous regulatory elements which should improve the safety and efficacy of gene therapy for this disease. The level of correction required to ameliorate disease phenotype will only truly be understood through clinical studies. There are reports describing female carriers with random X inactivation experiencing mild inflammatory symptoms [3, 77]; however, we are encouraged that the high levels of correction (> 50%) resulted in restoration of NOD2 signaling, suggesting that this level is sufficient to provide clinically relevant benefit.
In conclusion, the data shown here strongly supports the development of gene-correction approaches to treat patients with XIAP deficiency and overcome complications associated with HSCT.
Data Availability
Not applicable.
Code Availability
Not applicable.
References
Rigaud S, Fondanèche M-C, Lambert N, Pasquier B, Mateo V, Soulas P, et al. XIAP deficiency in humans causes an X-linked lymphoproliferative syndrome. Nature. 2006;444(7115):110–4.
Latour S, Aguilar C. XIAP deficiency syndrome in humans. Semin Cell Dev Biol. 2015;39:115–23.
Aguilar C, Lenoir C, Lambert N, Bègue B, Brousse N, Canioni D, et al. Characterization of Crohn disease in X-linked inhibitor of apoptosis–deficient male patients and female symptomatic carriers. J Allergy Clin Immunol. 2014;134(5):1131-1141.e9.
Schwerd T, Pandey S, Yang H-T, Bagola K, Jameson E, Jung J, et al. Impaired antibacterial autophagy links granulomatous intestinal inflammation in Niemann-Pick disease type C1 and XIAP deficiency with NOD2 variants in Crohn’s disease. Gut. 2017;66(6):1060–73.
Marsh RA, Madden L, Kitchen BJ, Mody R, McClimon B, Jordan MB, et al. XIAP deficiency: a unique primary immunodeficiency best classified as X-linked familial hemophagocytic lymphohistiocytosis and not as X-linked lymphoproliferative disease. Blood. 2010;116(7):1079–82.
Speckmann C, Lehmberg K, Albert MH, Damgaard RB, Fritsch M, Gyrd-Hansen M, et al. X-linked inhibitor of apoptosis (XIAP) deficiency: the spectrum of presenting manifestations beyond hemophagocytic lymphohistiocytosis. Clin Immunol. 2013;149(1):133–41.
Mudde ACA, Booth C, Marsh RA. Evolution of Our Understanding of XIAP Deficiency. Front Pediatr. 2021;9:660520.
Marsh RA, Rao K, Satwani P, Lehmberg K, Müller I, Li D, et al. Allogeneic hematopoietic cell transplantation for XIAP deficiency: an international survey reveals poor outcomes. Blood. 2013;121(6):877–83.
Arnold DE, Nofal R, Wakefield C, Lehmberg K, Wustrau K, Albert MH, et al. Reduced-intensity/reduced-toxicity conditioning approaches are tolerated in XIAP Deficiency but patients fare poorly with acute GVHD. J Clin Immunol. 2022;42(1):36–45.
Ono S, Okano T, Hoshino A, Yanagimachi M, Hamamoto K, Nakazawa Y, et al. Hematopoietic stem cell transplantation for XIAP deficiency in Japan. J Clin Immunol. 2017;37(1):85–91.
Aiuti A, Cattaneo F, Galimberti S, Benninghoff U, Cassani B, Callegaro L, et al. Gene Therapy for immunodeficiency due to adenosine deaminase deficiency. N Engl J Med. 2009;360(5):447–58.
Kohn DB, Booth C, Shaw KL, Xu-Bayford J, Garabedian E, Trevisan V, et al. Autologous Ex vivo lentiviral gene therapy for adenosine deaminase deficiency. N Engl J Med. 2021;384(21):2002–13.
Mamcarz E, Zhou S, Lockey T, Abdelsamed H, Cross SJ, Kang G, et al. Lentiviral gene therapy combined with low-dose busulfan in infants with SCID-X1. N Engl J Med. 2019;380(16):1525–34.
Morris EC, Fox T, Chakraverty R, Tendeiro R, Snell K, Rivat C, et al. Gene therapy for Wiskott-Aldrich syndrome in a severely affected adult. Blood. 2017;130(11):1327–35.
Magnani A, Semeraro M, Adam F, Booth C, Dupré L, Morris EC, et al. Long-term safety and efficacy of lentiviral hematopoietic stem/progenitor cell gene therapy for Wiskott-Aldrich syndrome. Nat Med. 2022;28(1):71–80.
Kohn DB, Booth C, Kang EM, Pai SY, Shaw KL, Santilli G, et al. Lentiviral gene therapy for X-linked chronic granulomatous disease. Nat Med. 2020;26(2):200–6.
Booth C, Carmo M, Gaspar H. Gene therapy for haemophagocytic lymphohistiocytosis. Curr Gene Ther. 2014;14(6):437–46.
Soheili T, Durand A, Sepulveda FE, Riviere J, Lagresle-Peyrou C, Sadek H, et al. Gene transfer into hematopoietic stem cells reduces HLH manifestations in a murine model of Munc13-4 deficiency. Blood Adv. 2017;1(27):2781–9.
Ghosh S, Carmo M, Calero-Garcia M, Ricciardelli I, Bustamante Ogando JC, Blundell MP, et al. T-cell gene therapy for perforin deficiency corrects cytotoxicity defects and prevents hemophagocytic lymphohistiocytosis manifestations. J Allergy Clin Immunol. 2018;142(3):904-913.e3.
Takushi SE, Paik NY, Fedanov A, Prince C, Doering CB, Spencer HT, et al. Lentiviral gene therapy for familial hemophagocytic lymphohistiocytosis Type 3, caused by UNC13D genetic defects. Hum Gene Ther. 2020;31(11–12):626–38.
Eckelman BP, Salvesen GS, Scott FL. Human inhibitor of apoptosis proteins: why XIAP is the black sheep of the family. EMBO Rep. 2006;7(10):988–94.
Deveraux QL, Leo E, Stennicke HR, Welsh K, Salvesen GS, Reed JC. Cleavage of human inhibitor of apoptosis protein XIAP results in fragments with distinct specificities for caspases. EMBO J. 1999;18(19):5242–51.
Scott FL, Denault J-B, Riedl SJ, Shin H, Renatus M, Salvesen GS. XIAP inhibits caspase-3 and -7 using two binding sites: evolutionarily conserved mechanism of IAPs. EMBO J. 2005;24(3):645–55.
Shiozaki EN, Chai J, Rigotti DJ, Riedl SJ, Li P, Srinivasula SM, et al. Mechanism of XIAP-mediated inhibition of caspase-9. Mol Cell. 2003;11(2):519–27.
Knop J, Spilgies LM, Rufli S, Reinhart R, Vasilikos L, Yabal M, et al. TNFR2 induced priming of the inflammasome leads to a RIPK1-dependent cell death in the absence of XIAP. Cell Death Dis. 2019;10(10):1–14.
Damgaard RB, Nachbur U, Yabal M, Wong WW-LL, Fiil BK, Kastirr M, et al. The ubiquitin ligase XIAP recruits LUBAC for NOD2 signaling in inflammation and innate immunity. Mol Cell. 2012;46(6):746–58.
Damgaard RB, Fiil BK, Speckmann C, Yabal M, zur Stadt U, Bekker-Jensen S, et al. Disease-causing mutations in the XIAP BIR2 domain impair NOD2-dependent immune signalling. EMBO Mol Med. 2013;5(8):1278–95.
Worthey EA, Mayer AN, Syverson GD, Helbling D, Bonacci BB, Decker B, et al. Making a definitive diagnosis: successful clinical application of whole exome sequencing in a child with intractable inflammatory bowel disease. Genet Med. 2011;13(3):255–62.
Zeissig Y, Petersen B-S, Milutinovic S, Bosse E, Mayr G, Peuker K, et al. XIAP variants in male Crohn’s disease. Gut. 2015;64(1):66–76.
Wada T, Kanegane H, Ohta K, Katoh F, Imamura T, Nakazawa Y, et al. Sustained elevation of serum interleukin-18 and its association with hemophagocytic lymphohistiocytosis in XIAP deficiency. Cytokine. 2014;65(1):74–8.
Geerlinks AV, Dvorak AM, Jordan MB, Schiffrin EJ, Behrens EM, Marsh R. A Case of XIAP Deficiency successfully managed with Tadekinig Alfa (rhIL-18BP). J Clin Immunol. 2022;2022(1):1–3.
Hsieh W-C, Chuang Y-T, Chiang I-H, Hsu S-C, Miaw S-C, Lai M-Z. Inability to resolve specific infection generates innate immunodeficiency syndrome in Xiap-/- mice. Blood. 2014;124(18):2847–57.
Hardison SE, Brown GD. C-type lectin receptors orchestrate antifungal immunity. Nat Immunol. 2012;13(9):817–22.
Yabal M, Müller N, Adler H, Knies N, Groß CJ, Damgaard RB, et al. XIAP restricts TNF- and RIP3-dependent cell death and inflammasome activation. Cell Rep. 2014;7(6):1796–808.
Lawlor KE, Khan N, Mildenhall A, Gerlic M, Croker BA, D’Cruz AA, et al. RIPK3 promotes cell death and NLRP3 inflammasome activation in the absence of MLKL. Nat Commun. 2015;6:6282.
Wong WW-L, Vince JE, Lalaoui N, Lawlor KE, Chau D, Bankovacki A, et al. cIAPs and XIAP regulate myelopoiesis through cytokine production in an RIPK1- and RIPK3-dependent manner. Blood. 2014;123(16):2562–72.
Tu H, Costa M. XIAP’s Profile in Human Cancer. Biomolecules. 2020;10(11):1–15.
Srivastava AK, Singh PK, Singh D, Dalela D, Rath SK, Goel MM, et al. Evaluation of urinary XIAP as a diagnostic biomarker of carcinoma of urinary bladder. Tumor Biol. 2014;35(8):8243–8.
Xu J, Hua X, Yang R, Jin H, Li J, Zhu J, et al. XIAP Interaction with E2F1 and Sp1 via its BIR2 and BIR3 domains specific activated MMP2 to promote bladder cancer invasion. Oncog. 2019;8(12):1–9.
Jiang G, Huang C, Liao X, Li J, Wu XR, Zeng F, et al. The RING domain in the anti-apoptotic protein XIAP stabilizes c-Myc protein and preserves anchorage-independent growth of bladder cancer cells. J Biol Chem. 2019;294(15):5935–44.
Wang J, Liu Y, Ji R, Gu Q, Zhao X, Liu Y, et al. Prognostic value of the X-linked inhibitor of apoptosis protein for invasive ductal breast cancer with triple-negative phenotype. Hum Pathol. 2010;41(8):1186–95.
Huang X, Wang X nan, Yuan X dong, Wu W yong, Lobie PE, Wu Z. XIAP facilitates breast and colon carcinoma growth via promotion of p62 depletion through ubiquitination-dependent proteasomal degradation. Oncogene. 2018;38(9):1448–60.
Hussain AR, Siraj AK, Ahmed M, Bu R, Pratheeshkumar P, Alrashed AM, et al. XIAP over-expression is an independent poor prognostic marker in Middle Eastern breast cancer and can be targeted to induce efficient apoptosis. BMC Cancer. 2017;17(1):640.
Miyamoto M, Takano M, Iwaya K, Shinomiya N, Kato M, Aoyama T, et al. X-chromosome-linked inhibitor of apoptosis as a key factor for chemoresistance in clear cell carcinoma of the ovary. Br J Cancer. 2014;110(12):2881–6.
Zhang Y, Huang F, Luo Q, Wu X, Liu Z, Chen H, et al. Inhibition of XIAP increases carboplatin sensitivity in ovarian cancer. Onco Targets Ther. 2018;11:8751–9.
Shaw TJ, Lacasse EC, Durkin JP, Vanderhyden BC. Downregulation of XIAP expression in ovarian cancer cells induces cell death in vitro and in vivo. Int J cancer. 2008;122(6):1430–4.
Cheng Y-J, Jiang H-S, Hsu S-L, Lin L-C, Wu C-L, Ghanta VK, et al. XIAP-mediated protection of H460 lung cancer cells against cisplatin. Eur J Pharmacol. 2010;627(1–3):75–84.
Wu XB, Li QH, Zhang N, Li M, Li K. MiR-142 inhibits lung cancer cell proliferation and promotes apoptosis by targeting XIAP. Eur Rev Med Pharmacol Sci. 2019;23(17):7430–7.
Krepela E, Dankova P, Moravcikova E, Krepelova A, Prochazka J, Cermak J, et al. Increased expression of inhibitor of apoptosis proteins, survivin and XIAP, in non-small cell lung carcinoma. Int J Oncol. 2009;35(6):1449–62.
Flanagan L, Kehoe J, Fay J, Bacon O, Lindner AUU, Kay EWW, et al. High levels of X-linked Inhibitor-of-Apoptosis Protein (XIAP) are indicative of radio chemotherapy resistance in rectal cancer. Radiat Oncol. 2015;10(1):131.
Moussata D, Amara S, Siddeek B, Decaussin M, Hehlgans S, Paul-Bellon R, et al. XIAP as a radioresistance factor and prognostic marker for radiotherapy in human rectal adenocarcinoma. Am J Pathol. 2012;181(4):1271–8.
Bao W, Zhu F, Duan Y, Yang Y, Cai H. HtrA1 resensitizes multidrug-resistant hepatocellular carcinoma cells by targeting XIAP. Biomed Pharmacother. 2015;70(C):97–102.
Devi GR. XIAP as target for therapeutic apoptosis in prostate cancer. Drug News Perspect. 2004;17(2):127–34.
Danquah M, Duke CB, Patil R, Miller DD, Mahato RI. Combination therapy of antiandrogen and XIAP inhibitor for treating advanced prostate cancer. Pharm Res. 2012;29(8):2079–91.
Berezovskaya O, Schimmer AD, Glinskii AB, Pinilla C, Hoffman RM, Reed JC, et al. Increased EXpression of apoptosis inhibitor protein XIAP contributes to anoikis resistance of circulating human prostate cancer metastasis precursor cells. Cancer Res. 2005;65(6):2378–86.
Nakano Y, Bilim V, Yuuki K, Muto A, Kato T, Nagaoka A, et al. Molecular targeting of Bcl-2 overcomes prostate cancer cell adaptation to XIAP gene downregulation. Prostate Cancer Prostatic Dis. 2008;12(1):34–40.
Hofer-Warbinek R, Schmid JA, Stehlik C, Binder BR, Lipp J, De Martin R. Activation of NF-κB by XIAP, the X chromosome-linked inhibitor of apoptosis, in endothelial cells involves TAK1 *. J Biol Chem. 2000;275(29):22064–8.
Harlin H, Reffey SB, Duckett CS, Lindsten T, Thompson CB. Characterization of XIAP-deficient mice. Mol Cell Biol. 2001;21(10):3604–8.
Montiel-Equihua CA, Zhang L, Knight S, Saadeh H, Scholz S, Carmo M, et al. The β-globin locus control region in combination with the EF1α short promoter allows enhanced lentiviral vector-mediated erythroid gene expression with conserved multilineage activity. Mol Ther. 2012;20(7):1400–9.
Lawlor KE, Feltham R, Yabal M, Conos SA, Chen KW, Ziehe S, et al. XIAP Loss triggers RIPK3- and caspase-8-driven IL-1β Activation and cell death as a consequence of TLR-MyD88-induced cIAP1-TRAF2 degradation. Cell Rep. 2017;20(3):668–82.
Ammann S, Elling R, Gyrd-Hansen M, Dückers G, Bredius R, Burns SO, et al. A new functional assay for the diagnosis of X-linked inhibitor of apoptosis (XIAP) deficiency. Clin Exp Immunol. 2014;176(3):394–400.
Morgan RA, Gray D, Lomova A, Kohn DB. Hematopoietic Stem cell gene therapy: progress and lessons learned. Cell Stem Cell. 2017;21(5):574–90.
Staal FJT, Aiuti A, Cavazzana M. Autologous stem-cell-based gene therapy for inherited disorders: state of the art and perspectives. Front Pediatr. 2019;7:443.
Ogura Y, Inohara N, Benito A, Chen FF, Yamaoka S, Nunez G. Nod2, a Nod1/Apaf-1 family member that is restricted to monocytes and activates NF-kappaB. J Biol Chem. 2001;276(7):4812–8.
Cartier N, Hacein-Bey-Abina S, Bartholomae CC, Veres G, Schmidt M, Kutschera I, et al. Hematopoietic stem cell gene therapy with a lentiviral vector in X-linked adrenoleukodystrophy. Science (80- ). 2009;326(5954):818–23.
Biffi A, Montini E, Lorioli L, Cesani M, Fumagalli F, Plati T, et al. Lentiviral hematopoietic stem cell gene therapy benefits metachromatic leukodystrophy. Science. 2013;341(6148):1233158.
Fumagalli F, Calbi V, Natali Sora MG, Sessa M, Baldoli C, Rancoita PMV, et al. Lentiviral haematopoietic stem-cell gene therapy for early-onset metachromatic leukodystrophy: long-term results from a non-randomised, open-label, phase 1/2 trial and expanded access. Lancet. 2022;399(10322):372–83.
Varghese AS, Lee H, Bonney D, Hughes S, Wynn R. Complications of reduced intensity conditioning HSCT for XIAP deficiency (alloimmune cytopenias and HLH) successfully managed with donor lymphocyte infusion. J Pediatr Hematol Oncol. 2015;37(3):e198–9.
Bauler LD, Duckett CS, O’Riordan MXD. XIAP regulates cytosol-specific innate immunity to Listeria infection. PLoS Pathog. 2008;4(8): e1000142.
Pachlopnik Schmid J, Canioni D, Moshous D, Touzot F, Mahlaoui N, Hauck F, et al. Clinical similarities and differences of patients with X-linked lymphoproliferative syndrome type 1 (XLP-1/SAP deficiency) versus type 2 (XLP-2/XIAP deficiency). Blood. 2011;117(5):1522–9.
Yang X, Miyawaki T, Kanegane H. SAP and XIAP deficiency in hemophagocytic lymphohistiocytosis. Pediatr Int. 2012;54(4):447–54.
Chen RY, Li XZ, Lin Q, Zhu Y, Shen YY, Xu QY, et al. Epstein-Barr virus-related hemophagocytic lymphohistiocytosis complicated with coronary artery dilation and acute renal injury in a boy with a novel X-linked inhibitor of apoptosis protein (XIAP) variant: A case report. BMC Pediatr. 2020;20(1):1–7.
Stein S, Ott MG, Schultze-Strasser S, Jauch A, Burwinkel B, Kinner A, et al. Genomic instability and myelodysplasia with monosomy 7 consequent to EVI1 activation after gene therapy for chronic granulomatous disease. Nat Med. 2010;16(2):198–204.
Biasco L, Baricordi C, Aiuti A. Retroviral Integrations in Gene Therapy Trials. Mol Ther. 2012;20(4):709.
Scholz SJ, Fronza R, Bartholomä CC, Cesana D, Montini E, Von Kalle C, et al. Lentiviral vector promoter is decisive for aberrant transcript formation. Hum Gene Ther. 2017;28(10):875–85.
Schwarzer A, Talbot SR, Selich A, Morgan M, Schott JW, Dittrich-Breiholz O, et al. Predicting genotoxicity of viral vectors for stem cell gene therapy using gene expression-based machine learning. Mol Ther. 2021;29(12):3383–97.
Dziadzio M, Amman S, Canning C, Boyle F, Hassan A, Cale C, et al. Symptomatic males and female carriers in a large Caucasian kindred wth XIAP deficiency. J Clin Immunol. 2015;35(5):439–44.
Acknowledgements
We thank the patients and their families as well as the clinical teams.
Funding
JT is supported by the Medical Research Council (MRC) in conjunction with GOSH Children’s Charity. Funding was provided by Action Medical Research (GN2761). All research at GOSH is supported by the National Institute of Health Research (NIHR) GOSH Biomedical Research Centre (BRC).
Author information
Authors and Affiliations
Contributions
CB conceived the study. JT, NP, BH, and CB designed the study. JT performed the majority of experimental work. JT and NP collected the data. JT and CB wrote the manuscript. NP, AB, AR, and AM performed work on other promoter elements and murine studies. HBG and AT reviewed data. All authors critically reviewed and edited the manuscript.
Corresponding author
Ethics declarations
Ethics Approval
Ethical approval in place.
Consent to Participate/for Publication
Informed consent was obtained from the patient and/or parents of each patient for research samples, and patients were treated in accordance with the Declaration of Helsinki.
Conflict of Interest
HBG is an employee of Orchard Therapeutics and holds equity in the company.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Topal, J., Panchal, N., Barroeta, A. et al. Lentiviral Gene Transfer Corrects Immune Abnormalities in XIAP Deficiency. J Clin Immunol 43, 440–451 (2023). https://doi.org/10.1007/s10875-022-01389-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10875-022-01389-0