Abstract
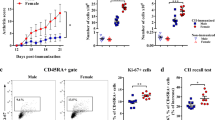
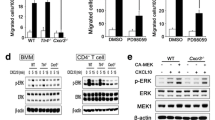
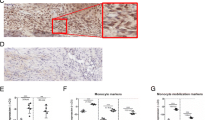
Monocytes’ plasticity has an important role in the development of rheumatoid arthritis (RA), an autoimmune disease exhibiting greater prevalence in women. Contribution of this phenomenon to sex bias in RA severity was investigated in rat collagen-induced arthritis (CIA) model of RA. The greater severity of CIA in females (exhibiting signs of bone resorption) was accompanied by the higher blood level of advanced oxidation protein products and a more pro-oxidant profile. Consistently, in females, the greater density of giant multinuclear cells (monocytes/macrophages and osteoclasts) in inflamed joint tissue was found. This correlated with the higher frequencies of CCR2- and CX3CR1- expressing cells (precursors of inflammatory monocytes/macrophages and osteoclasts) among CD11b+ splenocytes. This in conjunction with the enhanced migratory capacity of CD11b+ monocytic cells in females compared with males could be linked with the higher frequencies of CCR2+CX3CR1-CD43lowCD11b+ and CCR2-CX3CR1+CD43hiCD11b+ cells (corresponding to “classical” and “non-classical” monocytes, respectively) and the greater density of CD68+ cells (monocytes/macrophages and osteoclast precursors/osteoclasts) in blood and inflamed paws from female rats, respectively. Consistently, the higher levels of GM-CSF, TNF-α and IL-6, IL-1β (driving Th17 cell differentiation), and IL-17 followed by the lower level of IL-10 were measured in inflamed paw cultures from female compared with male rats. To the greater IL-17 production (associated with enhanced monocyte immigration and differentiation into osteoclasts) most likely contributed augmented Th17 cell generation in the lymph nodes draining arthritic joints from female compared with male rats. Overall, the study suggests the sex-specific contribution of monocytic lineage cells to CIA, and possibly RA development.






Similar content being viewed by others
References
Whitacre, C.C. 2001. Sex differences in autoimmune disease. Nature Immunology 2 (9): 777–780. https://doi.org/10.1038/ni0901-777.
Guo, Q., Y. Wang, D. Xu, J. Nossent, N.J. Pavlos, and J. Xu. 2018. Rheumatoid arthritis: Pathological mechanisms and modern pharmacologic therapies. Bone Res 6: 15. https://doi.org/10.1038/s41413-018-0016-9.
Lundstrom, E., H. Kallberg, L. Alfredsson, L. Klareskog, and L. Padyukov. 2009. Gene-environment interaction between the DRB1 shared epitope and smoking in the risk of anti-citrullinated protein antibody-positive rheumatoid arthritis: All alleles are important. Arthritis and Rheumatism 60 (6): 1597–1603. https://doi.org/10.1002/art.24572.
Sokka, T., S. Toloza, M. Cutolo, H. Kautiainen, H. Makinen, F. Gogus, V. Skakic, H. Badsha, T. Peets, A. Baranauskaite, P. Géher, I. Ujfalussy, F.N. Skopouli, M. Mavrommati, R. Alten, C. Pohl, J. Sibilia, A. Stancati, F. Salaffi, W. Romanowski, D. Zarowny-Wierzbinska, D. Henrohn, B. Bresnihan, P. Minnock, L.S. Knudsen, J.W. Jacobs, J. Calvo-Alen, J. Lazovskis, R. Pinheiro Gda, D. Karateev, D. Andersone, S. Rexhepi, Y. Yazici, T. Pincus, and QUEST-RA Group. 2009. Women, men, and rheumatoid arthritis: Analyses of disease activity, disease characteristics, and treatments in the QUEST-RA study. Arthritis Research & Therapy 11 (1): R7. https://doi.org/10.1186/ar2591.
Cutolo, M., S. Capellino, and R.H. Straub. 2008. Oestrogens in rheumatic diseases: Friend or foe? Rheumatology (Oxford) 47 (Suppl 3): iii2–iii5. https://doi.org/10.1093/rheumatology/ken150.
Chabchoub, G., E. Uz, A. Maalej, C.A. Mustafa, A. Rebai, M. Mnif, Z. Bahloul, N.R. Farid, T. Ozcelik, and H. Ayadi. 2009. Analysis of skewed X-chromosome inactivation in females with rheumatoid arthritis and autoimmune thyroid diseases. Arthritis Research & Therapy 11 (4): R106. https://doi.org/10.1186/ar2759.
Krasselt, M., and C. Baerwald. 2019. Sex, symptom severity, and quality of life in rheumatology. Clinical Reviews in Allergy and Immunology 56 (3): 346–361. https://doi.org/10.1007/s12016-017-8631-6.
Lambert, N.C. 2012. Microchimerism and rheumatic diseases. Joint, Bone, Spine 79 (6): 563–564. https://doi.org/10.1016/j.jbspin.2012.09.015.
Quintero, O.L., M.J. Amador-Patarroyo, G. Montoya-Ortiz, A. Rojas-Villarraga, and J.M. Anaya. 2012. Autoimmune disease and gender: Plausible mechanisms for the female predominance of autoimmunity. Journal of Autoimmunity 38 (2–3): J109–J119. https://doi.org/10.1016/j.jaut.2011.10.003.
Rak, J.M., L. Maestroni, N. Balandraud, S. Guis, H. Boudinet, M.C. Guzian, Z. Yan, D. Azzouz, I. Auger, C. Roudier, M. Martin, R. Didelot, J. Roudier, and N.C. Lambert. 2009. Transfer of the shared epitope through microchimerism in women with rheumatoid arthritis. Arthritis and Rheumatism 60 (1): 73–80. https://doi.org/10.1002/art.24224.
Andersson, A., A. Stubelius, M.N. Karlsson, C. Engdahl, M. Erlandsson, L. Grahnemo, M.K. Lagerquist, and U. Islander. 2015. Estrogen regulates T helper 17 phenotype and localization in experimental autoimmune arthritis. Arthritis Research & Therapy 17: 32. https://doi.org/10.1186/s13075-015-0548-y.
Ganesan, K., C. Balachandran, B.M. Manohar, and R. Puvanakrishnan. 2008. Comparative studies on the interplay of testosterone, estrogen and progesterone in collagen induced arthritis in rats. Bone 43 (4): 758–765. https://doi.org/10.1016/j.bone.2008.05.025.
Krause, M.L., and A. Makol. 2016. Management of rheumatoid arthritis during pregnancy: Challenges and solutions. Open access Rheumatology : Research and Reviews 8: 23–36. https://doi.org/10.2147/OARRR.S85340.
Islander, U., C. Jochems, M.K. Lagerquist, H. Forsblad-d’Elia, and H. Carlsten. 2011. Estrogens in rheumatoid arthritis; the immune system and bone. Molecular and Cellular Endocrinology 335 (1): 14–29. https://doi.org/10.1016/j.mce.2010.05.018.
Kovacs, W.J., and N.J. Olsen. 2011. Sexual dimorphism of RA manifestations: Genes, hormones and behavior. Nature Reviews Rheumatology 7 (5): 307–310. https://doi.org/10.1038/nrrheum.2010.231.
Firestein, G.S. 2003. Evolving concepts of rheumatoid arthritis. Nature 423 (6937): 356–361. https://doi.org/10.1038/nature01661.
Gordon, S., and P.R. Taylor. 2005. Monocyte and macrophage heterogeneity. Nature Reviews. Immunology 5 (12): 953–964. https://doi.org/10.1038/nri1733.
Madel, M.B., L. Ibanez, A. Wakkach, T.J. de Vries, A. Teti, F. Apparailly, and C. Blin-Wakkach. 2019. Immune function and diversity of osteoclasts in normal and pathological conditions. Frontiers in Immunology 10: 1408. https://doi.org/10.3389/fimmu.2019.01408.
Tak, P.P., and B. Bresnihan. 2000. The pathogenesis and prevention of joint damage in rheumatoid arthritis: Advances from synovial biopsy and tissue analysis. Arthritis and Rheumatism 43 (12): 2619–2633. https://doi.org/10.1002/1529-0131(200012)43:12<2619::AID-ANR1>3.0.CO;2-V.
Hirose, S., Q. Lin, M. Ohtsuji, H. Nishimura, and J.S. Verbeek. 2019. Monocyte subsets involved in the development of systemic lupus erythematosus and rheumatoid arthritis. International Immunology 31 (11): 687–696. https://doi.org/10.1093/intimm/dxz036.
Puchner, A., V. Saferding, M. Bonelli, Y. Mikami, M. Hofmann, J.S. Brunner, M. Caldera, E. Goncalves-Alves, N.B. Binder, A. Fischer, E. Simader, C.W. Steiner, H. Leiss, S. Hayer, B. Niederreiter, T. Karonitsch, M.I. Koenders, B.K. Podesser, J.J. O’Shea, J. Menche, J.S. Smolen, K. Redlich, and S. Blüml. 2018. Non-classical monocytes as mediators of tissue destruction in arthritis. Annals of the Rheumatic Diseases 77 (10): 1490–1497. https://doi.org/10.1136/annrheumdis-2018-213250.
Kinne, R.W., B. Stuhlmuller, and G.R. Burmester. 2007. Cells of the synovium in rheumatoid arthritis. Macrophages. Arthritis Research & Therapy 9 (6): 224. https://doi.org/10.1186/ar2333.
Matthys, P., K. Vermeire, T. Mitera, H. Heremans, S. Huang, D. Schols, C. De Wolf-Peeters, and A. Billiau. 1999. Enhanced autoimmune arthritis in IFN-gamma receptor-deficient mice is conditioned by mycobacteria in Freund’s adjuvant and by increased expansion of Mac-1+ myeloid cells. Journal of Immunology 163 (6): 3503–3510.
Herenius, M.M., R.M. Thurlings, C.A. Wijbrandts, R.J. Bennink, S.E. Dohmen, C. Voermans, D. Wouters, et al. 2011. Monocyte migration to the synovium in rheumatoid arthritis patients treated with adalimumab. Annals of the Rheumatic Diseases 70 (6): 1160–1162. https://doi.org/10.1136/ard.2010.141549.
Egan, P.J., A. van Nieuwenhuijze, I.K. Campbell, and I.P. Wicks. 2008. Promotion of the local differentiation of murine Th17 cells by synovial macrophages during acute inflammatory arthritis. Arthritis and Rheumatism 58 (12): 3720–3729. https://doi.org/10.1002/art.24075.
Schett, G. 2007. Cells of the synovium in rheumatoid arthritis. Osteoclasts. Arthritis Research & Therapy 9 (1): 203. https://doi.org/10.1186/ar2110.
An, G., C. Acharya, X. Feng, K. Wen, M. Zhong, L. Zhang, N.C. Munshi, L. Qiu, Y.T. Tai, and K.C. Anderson. 2016. Osteoclasts promote immune suppressive microenvironment in multiple myeloma: Therapeutic implication. Blood 128 (12): 1590–1603. https://doi.org/10.1182/blood-2016-03-707547.
Grassi, F., C. Manferdini, L. Cattini, A. Piacentini, E. Gabusi, A. Facchini, and G. Lisignoli. 2011. T cell suppression by osteoclasts in vitro. Journal of Cellular Physiology 226 (4): 982–990. https://doi.org/10.1002/jcp.22411.
Ibanez, L., G. Abou-Ezzi, T. Ciucci, V. Amiot, N. Belaid, D. Obino, A. Mansour, M. Rouleau, A. Wakkach, and C. Blin-Wakkach. 2016. Inflammatory osteoclasts prime TNFalpha-producing CD4(+) T cells and express CX3 CR1. Journal of Bone and Mineral Research 31 (10): 1899–1908. https://doi.org/10.1002/jbmr.2868.
Kiesel, J.R., Z.S. Buchwald, and R. Aurora. 2009. Cross-presentation by osteoclasts induces FoxP3 in CD8+ T cells. Journal of Immunology 182 (9): 5477–5487. https://doi.org/10.4049/jimmunol.0803897.
Roberts, C.A., A.K. Dickinson, and L.S. Taams. 2015. The interplay between monocytes/macrophages and CD4(+) T cell subsets in rheumatoid arthritis. Frontiers in Immunology 6: 571. https://doi.org/10.3389/fimmu.2015.00571.
Li, H., S. Hong, J. Qian, Y. Zheng, J. Yang, and Q. Yi. 2010. Cross talk between the bone and immune systems: Osteoclasts function as antigen-presenting cells and activate CD4+ and CD8+ T cells. Blood 116 (2): 210–217. https://doi.org/10.1182/blood-2009-11-255026.
Shahrara, S., S.R. Pickens, A.M. Mandelin 2nd, W.J. Karpus, Q. Huang, J.K. Kolls, and R.M. Pope. 2010. IL-17-mediated monocyte migration occurs partially through CC chemokine ligand 2/monocyte chemoattractant protein-1 induction. Journal of Immunology 184 (8): 4479–4487. https://doi.org/10.4049/jimmunol.0901942.
Adamopoulos, I.E., C.C. Chao, R. Geissler, D. Laface, W. Blumenschein, Y. Iwakura, T. McClanahan, and E.P. Bowman. 2010. Interleukin-17A upregulates receptor activator of NF-kappaB on osteoclast precursors. Arthritis Research & Therapy 12 (1): R29. https://doi.org/10.1186/ar2936.
D'Amelio, P., M.A. Cristofaro, C. Tamone, E. Morra, S. Di Bella, G. Isaia, A. Grimaldi, et al. 2008. Role of iron metabolism and oxidative damage in postmenopausal bone loss. Bone 43 (6): 1010–1015. https://doi.org/10.1016/j.bone.2008.08.107.
Jung, S.M., K.W. Kim, C.W. Yang, S.H. Park, and J.H. Ju. 2014. Cytokine-mediated bone destruction in rheumatoid arthritis. Journal of Immunology Research 2014: 263625–263615. https://doi.org/10.1155/2014/263625.
Kotake, S., N. Udagawa, N. Takahashi, K. Matsuzaki, K. Itoh, S. Ishiyama, S. Saito, K. Inoue, N. Kamatani, M.T. Gillespie, T.J. Martin, and T. Suda. 1999. IL-17 in synovial fluids from patients with rheumatoid arthritis is a potent stimulator of osteoclastogenesis. The Journal of Clinical Investigation 103 (9): 1345–1352. https://doi.org/10.1172/JCI5703.
Lubberts, E., L. van den Bersselaar, B. Oppers-Walgreen, P. Schwarzenberger, C.J. Coenen-de Roo, J.K. Kolls, L.A. Joosten, and W.B. van den Berg. 2003. IL-17 promotes bone erosion in murine collagen-induced arthritis through loss of the receptor activator of NF-kappa B ligand/osteoprotegerin balance. Journal of Immunology 170 (5): 2655–2662. https://doi.org/10.4049/jimmunol.170.5.2655.
Acosta-Rodriguez, E.V., G. Napolitani, A. Lanzavecchia, and F. Sallusto. 2007. Interleukins 1beta and 6 but not transforming growth factor-beta are essential for the differentiation of interleukin 17-producing human T helper cells. Nature Immunology 8 (9): 942–949. https://doi.org/10.1038/ni1496.
Segura, E., M. Touzot, A. Bohineust, A. Cappuccio, G. Chiocchia, A. Hosmalin, M. Dalod, V. Soumelis, and S. Amigorena. 2013. Human inflammatory dendritic cells induce Th17 cell differentiation. Immunity 38 (2): 336–348. https://doi.org/10.1016/j.immuni.2012.10.018.
McInnes, I.B., and G. Schett. 2007. Cytokines in the pathogenesis of rheumatoid arthritis. Nature Reviews. Immunology 7 (6): 429–442. https://doi.org/10.1038/nri2094.
Vierboom, M.P., M. Jonker, P.P. Tak, and B.A.T. Hart. 2007. Preclinical models of arthritic disease in non-human primates. Drug Discovery Today 12 (7–8): 327–335. https://doi.org/10.1016/j.drudis.2007.02.012.
Umar, S., J. Zargan, K. Umar, S. Ahmad, C.K. Katiyar, and H.A. Khan. 2012. Modulation of the oxidative stress and inflammatory cytokine response by thymoquinone in the collagen induced arthritis in Wistar rats. Chemico-Biological Interactions 197 (1): 40–46. https://doi.org/10.1016/j.cbi.2012.03.003.
Brand, D.D., A.H. Kang, and E.F. Rosloniec. 2004. The mouse model of collagen-induced arthritis. Methods in Molecular Medicine 102: 295–312. https://doi.org/10.1385/1-59259-805-6:295.
Griffiths, M.M., G.W. Cannon, T. Corsi, V. Reese, and K. Kunzler. 2007. Collagen-induced arthritis in rats. Methods in Molecular Medicine 136: 201–214. https://doi.org/10.1007/978-1-59745-402-5_15.
Dimitrijevic, M., N. Arsenovic-Ranin, B. Bufan, M. Nacka-Aleksic, M.L. Macanovic, P. Milovanovic, M. Duric, J. Sopta, and G. Leposavic. 2018. Collagen-induced arthritis in dark Agouti rats as a model for study of immunological sexual dimorphisms in the human disease. Experimental and Molecular Pathology 105 (1): 10–22. https://doi.org/10.1016/j.yexmp.2018.05.007.
Dimitrijevic, M., N. Arsenovic-Ranin, D. Kosec, B. Bufan, M. Nacka-Aleksic, I. Pilipovic, and G. Leposavic. 2019. Sexual dimorphism in Th17/Treg axis in lymph nodes draining inflamed joints in rats with collagen-induced arthritis. Brain, Behavior, and Immunity 76: 198–214. https://doi.org/10.1016/j.bbi.2018.11.311.
Patel, A.A., and S. Yona. 2019. Inherited and environmental factors influence human monocyte heterogeneity. Frontiers in Immunology 10: 2581. https://doi.org/10.3389/fimmu.2019.02581.
De Klerck, B., I. Carpentier, R.J. Lories, Y. Habraken, J. Piette, G. Carmeliet, R. Beyaert, A. Billiau, and P. Matthys. 2004. Enhanced osteoclast development in collagen-induced arthritis in interferon-gamma receptor knock-out mice as related to increased splenic CD11b+ myelopoiesis. Arthritis Research & Therapy 6 (3): R220–R231. https://doi.org/10.1186/ar1167.
Chistiakov, D.A., M.C. Killingsworth, V.A. Myasoedova, A.N. Orekhov, and Y.V. Bobryshev. 2017. CD68/macrosialin: Not just a histochemical marker. Laboratory Investigation 97 (1): 4–13. https://doi.org/10.1038/labinvest.2016.116.
Benaglio, F., B. Vitolo, M. Scarabelli, E. Binda, S. Bugatti, R. Caporali, C. Montecucco, and A. Manzo. 2015. The draining lymph node in rheumatoid arthritis: Current concepts and research perspectives. BioMed Research International 2015: 420251–420210. https://doi.org/10.1155/2015/420251.
Leonavičienė, L., R. Bradūnaitė, D. Vaitkienė, A. Vasiliauskas, and A. Keturkienė. 2008. Collagen-induced arthritis and pro−/antioxidant status in Wistar and Lewis rats. Biologija 54 (4): 290–300. https://doi.org/10.2478/v10054-008-0059-8.
Hawkins, P., R. Armstrong, T. Boden, P. Garside, K. Knight, E. Lilley, M. Seed, M. Wilkinson, and R.O. Williams. 2015. Applying refinement to the use of mice and rats in rheumatoid arthritis research. Inflammopharmacology 23 (4): 131–150. https://doi.org/10.1007/s10787-015-0241-4.
Hou, W., L. Meng, L. Tian, W. Zhu, C. Jiang, and S. Lu. 2010. A systematic comparison between collagen-induced arthritis and pristane-induced arthritis in dark Agouti rats. Clinical and Experimental Rheumatology 28 (4): 532–538.
Djikic, J., M. Nacka-Aleksic, I. Pilipovic, Z. Stojic-Vukanic, B. Bufan, D. Kosec, M. Dimitrijevic, and G. Leposavic. 2014. Age-associated changes in rat immune system: Lessons learned from experimental autoimmune encephalomyelitis. Experimental Gerontology 58: 179–197. https://doi.org/10.1016/j.exger.2014.08.005.
Gunn, M.D., S. Kyuwa, C. Tam, T. Kakiuchi, A. Matsuzawa, L.T. Williams, and H. Nakano. 1999. Mice lacking expression of secondary lymphoid organ chemokine have defects in lymphocyte homing and dendritic cell localization. The Journal of Experimental Medicine 189 (3): 451–460. https://doi.org/10.1084/jem.189.3.451.
Stirpe, F., M. Ravaioli, M.G. Battelli, S. Musiani, and G.L. Grazi. 2002. Xanthine oxidoreductase activity in human liver disease. The American Journal of Gastroenterology 97 (8): 2079–2085. https://doi.org/10.1111/j.1572-0241.2002.05925.x.
Erel, O. 2005. A new automated colorimetric method for measuring total oxidant status. Clinical Biochemistry 38 (12): 1103–1111. https://doi.org/10.1016/j.clinbiochem.2005.08.008.
Erel, O. 2004. A novel automated direct measurement method for total antioxidant capacity using a new generation, more stable ABTS radical cation. Clinical Biochemistry 37 (4): 277–285. https://doi.org/10.1016/j.clinbiochem.2003.11.015.
Alamdari, D.H., K. Paletas, T. Pegiou, M. Sarigianni, C. Befani, and G. Koliakos. 2007. A novel assay for the evaluation of the prooxidant-antioxidant balance, before and after antioxidant vitamin administration in type II diabetes patients. Clinical Biochemistry 40 (3–4): 248–254. https://doi.org/10.1016/j.clinbiochem.2006.10.017.
Kotur-Stevuljevic, J., N. Bogavac-Stanojevic, Z. Jelic-Ivanovic, A. Stefanovic, T. Gojkovic, J. Joksic, M. Sopic, B. Gulan, J. Janac, and S. Milosevic. 2015. Oxidative stress and paraoxonase 1 status in acute ischemic stroke patients. Atherosclerosis 241 (1): 192–198. https://doi.org/10.1016/j.atherosclerosis.2015.05.016.
Auclair, C. , and E. Voisin. 1985. Nitroblue tetrazolium reduction. In CRC handbook of methods for oxygen radical research, ed. R. A. Greenwald, 123–132. CRC Press.
Girotti, M.J., N. Khan, and B.A. McLellan. 1991. Early measurement of systemic lipid peroxidation products in the plasma of major blunt trauma patients. The Journal of Trauma 31 (1): 32–35.
Witko-Sarsat, V., M. Friedlander, C. Capeillere-Blandin, T. Nguyen-Khoa, A.T. Nguyen, J. Zingraff, P. Jungers, and B. Descamps-Latscha. 1996. Advanced oxidation protein products as a novel marker of oxidative stress in uremia. Kidney International 49 (5): 1304–1313.
Bradford, M.M. 1976. A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Analytical Biochemistry 72: 248–254.
Chabbi-Achengli, Y., T. Coman, C. Collet, J. Callebert, M. Corcelli, H. Lin, R. Rignault, M. Dy, M.C. de Vernejoul, and F. Cote. 2016. Serotonin is involved in autoimmune arthritis through Th17 immunity and bone resorption. The American Journal of Pathology 186 (4): 927–937. https://doi.org/10.1016/j.ajpath.2015.11.018.
Quinonez-Flores, C.M., S.A. Gonzalez-Chavez, D. Del Rio Najera, and C. Pacheco-Tena. 2016. Oxidative stress relevance in the pathogenesis of the rheumatoid arthritis: A systematic review. BioMed Research International 2016: 6097417–6097414. https://doi.org/10.1155/2016/6097417.
Cristani, M., A. Speciale, A. Saija, S. Gangemi, P.L. Minciullo, and F. Cimino. 2016. Circulating advanced oxidation protein products as oxidative stress biomarkers and progression mediators in pathological conditions related to inflammation and immune dysregulation. Current Medicinal Chemistry 23 (34): 3862–3882. https://doi.org/10.2174/0929867323666160902154748.
Nakamichi, Y., T. Mizoguchi, A. Arai, Y. Kobayashi, M. Sato, J.M. Penninger, H. Yasuda, S. Kato, H.F. DeLuca, T. Suda, N. Udagawa, and N. Takahashi. 2012. Spleen serves as a reservoir of osteoclast precursors through vitamin D-induced IL-34 expression in osteopetrotic op/op mice. Proceedings of the National Academy of Sciences of the United States of America 109 (25): 10006–10011. https://doi.org/10.1073/pnas.1207361109.
Swirski, F.K., M. Nahrendorf, M. Etzrodt, M. Wildgruber, V. Cortez-Retamozo, P. Panizzi, J.L. Figueiredo, R.H. Kohler, A. Chudnovskiy, P. Waterman, E. Aikawa, T.R. Mempel, P. Libby, R. Weissleder, and M.J. Pittet. 2009. Identification of splenic reservoir monocytes and their deployment to inflammatory sites. Science 325 (5940): 612–616. https://doi.org/10.1126/science.1175202.
Ancuta, P., K.Y. Liu, V. Misra, V.S. Wacleche, A. Gosselin, X. Zhou, and D. Gabuzda. 2009. Transcriptional profiling reveals developmental relationship and distinct biological functions of CD16+ and CD16- monocyte subsets. BMC Genomics 10: 403. https://doi.org/10.1186/1471-2164-10-403.
Ziegler-Heitbrock, L., P. Ancuta, S. Crowe, M. Dalod, V. Grau, D.N. Hart, P.J. Leenen, et al. 2010. Nomenclature of monocytes and dendritic cells in blood. Blood 116 (16): e74–e80. https://doi.org/10.1182/blood-2010-02-258558.
Kinne, R.W., R. Brauer, B. Stuhlmuller, E. Palombo-Kinne, and G.R. Burmester. 2000. Macrophages in rheumatoid arthritis. Arthritis Research 2 (3): 189–202. https://doi.org/10.1186/ar86.
Wang, W., D.J. Ferguson, J.M. Quinn, A.H. Simpson, and N.A. Athanasou. 1997. Osteoclasts are capable of particle phagocytosis and bone resorption. The Journal of Pathology 182 (1): 92–98. https://doi.org/10.1002/(SICI)1096-9896(199705)182:1<92::AID-PATH813>3.0.CO;2-E.
Victor, V.M., M. Minano, N. Guayerbas, M. Del Rio, S. Medina, and M. De la Fuente. 1998. Effects of endotoxic shock in several functions of murine peritoneal macrophages. Molecular and Cellular Biochemistry 189 (1–2): 25–31. https://doi.org/10.1023/a:1006891926301.
Evans, H.G., N.J. Gullick, S. Kelly, C. Pitzalis, G.M. Lord, B.W. Kirkham, and L.S. Taams. 2009. In vivo activated monocytes from the site of inflammation in humans specifically promote Th17 responses. Proceedings of the National Academy of Sciences of the United States of America 106 (15): 6232–6237. https://doi.org/10.1073/pnas.0808144106.
Schett, G., and E. Gravallese. 2012. Bone erosion in rheumatoid arthritis: Mechanisms, diagnosis and treatment. Nature Reviews Rheumatology 8 (11): 656–664. https://doi.org/10.1038/nrrheum.2012.153.
Ahuja, V., S.E. Miller, and D.N. Howell. 1995. Identification of two subpopulations of rat monocytes expressing disparate molecular forms and quantities of CD43. Cellular Immunology 163 (1): 59–69. https://doi.org/10.1006/cimm.1995.1099.
Rana, A.K., Y. Li, Q. Dang, and F. Yang. 2018. Monocytes in rheumatoid arthritis: Circulating precursors of macrophages and osteoclasts and, their heterogeneity and plasticity role in RA pathogenesis. International Immunopharmacology 65: 348–359. https://doi.org/10.1016/j.intimp.2018.10.016.
Sayegh, S., O. El Atat, K. Diallo, B. Rauwel, Y. Degboe, E. Cavaignac, A. Constantin, et al. 2019. Rheumatoid synovial fluids regulate the immunomodulatory potential of adipose-derived mesenchymal stem cells through a TNF/NF-kappaB-dependent mechanism. Frontiers in Immunology 10: 1482. https://doi.org/10.3389/fimmu.2019.01482.
Palmblad, K., E. Sundberg, M. Diez, R. Soderling, A.C. Aveberger, U. Andersson, and H.E. Harris. 2007. Morphological characterization of intra-articular HMGB1 expression during the course of collagen-induced arthritis. Arthritis Research & Therapy 9 (2): R35. https://doi.org/10.1186/ar2155.
Thornton, S., L.E. Duwel, G.P. Boivin, Y. Ma, and R. Hirsch. 1999. Association of the course of collagen-induced arthritis with distinct patterns of cytokine and chemokine messenger RNA expression. Arthritis and Rheumatism 42 (6): 1109–1118. https://doi.org/10.1002/1529-0131(199906)42:6<1109::AID-ANR7>3.0.CO;2-7.
Robert, M., and P. Miossec. 2018. IL-17 in rheumatoid arthritis and precision medicine: From synovitis expression to circulating bioactive levels. Front Med (Lausanne) 5: 364. https://doi.org/10.3389/fmed.2018.00364.
Kawabe, T., M. Matsushima, N. Hashimoto, K. Imaizumi, and Y. Hasegawa. 2011. CD40/CD40 ligand interactions in immune responses and pulmonary immunity. Nagoya Journal of Medical Science 73 (3–4): 69–78.
Fujiwara, N., and K. Kobayashi. 2005. Macrophages in inflammation. Current Drug Targets. Inflammation and Allergy 4 (3): 281–286. https://doi.org/10.2174/1568010054022024.
Dimitrijevic, M., N. Arsenovic-Ranin, D. Kosec, B. Bufan, M. Nacka-Aleksic, I. Pilipovic, and G. Leposavic. 2020. Sex differences in Tfh cell help to B cells contribute to sexual dimorphism in severity of rat collagen-induced arthritis. Scientific Reports 10 (1): 1214. https://doi.org/10.1038/s41598-020-58127-y.
Shi, C., and E.G. Pamer. 2011. Monocyte recruitment during infection and inflammation. Nature Reviews. Immunology 11 (11): 762–774. https://doi.org/10.1038/nri3070.
Luo, Q., P. Xiao, X. Li, Z. Deng, C. Qing, R. Su, J. Xu, Y. Guo, Z. Huang, and J. Li. 2018. Overexpression of CD64 on CD14(++)CD16(−) and CD14(++)CD16(+) monocytes of rheumatoid arthritis patients correlates with disease activity. Experimental and Therapeutic Medicine 16 (3): 2703–2711. https://doi.org/10.3892/etm.2018.6452.
Abdel Meguid, M.H., Y.H. Hamad, R.S. Swilam, and M.S. Barakat. 2013. Relation of interleukin-6 in rheumatoid arthritis patients to systemic bone loss and structural bone damage. Rheumatology International 33 (3): 697–703. https://doi.org/10.1007/s00296-012-2375-7.
Dimitroulas, T., S.N. Nikas, P. Trontzas, and G.D. Kitas. 2013. Biologic therapies and systemic bone loss in rheumatoid arthritis. Autoimmunity Reviews 12 (10): 958–966. https://doi.org/10.1016/j.autrev.2013.03.015.
Gengenbacher, M., H.J. Sebald, P.M. Villiger, W. Hofstetter, and M. Seitz. 2008. Infliximab inhibits bone resorption by circulating osteoclast precursor cells in patients with rheumatoid arthritis and ankylosing spondylitis. Annals of the Rheumatic Diseases 67 (5): 620–624. https://doi.org/10.1136/ard.2007.076711.
Ritchlin, C.T., S.A. Haas-Smith, P. Li, D.G. Hicks, and E.M. Schwarz. 2003. Mechanisms of TNF-alpha- and RANKL-mediated osteoclastogenesis and bone resorption in psoriatic arthritis. The Journal of Clinical Investigation 111 (6): 821–831. https://doi.org/10.1172/JCI16069.
Kim, J.H., H.M. Jin, K. Kim, I. Song, B.U. Youn, K. Matsuo, and N. Kim. 2009. The mechanism of osteoclast differentiation induced by IL-1. Journal of Immunology 183 (3): 1862–1870. https://doi.org/10.4049/jimmunol.0803007.
Wicks, I.P., and A.W. Roberts. 2016. Targeting GM-CSF in inflammatory diseases. Nature Reviews Rheumatology 12 (1): 37–48. https://doi.org/10.1038/nrrheum.2015.161.
Chung, Y., S.H. Chang, G.J. Martinez, X.O. Yang, R. Nurieva, H.S. Kang, L. Ma, S.S. Watowich, A.M. Jetten, Q. Tian, and C. Dong. 2009. Critical regulation of early Th17 cell differentiation by interleukin-1 signaling. Immunity 30 (4): 576–587. https://doi.org/10.1016/j.immuni.2009.02.007.
Tarrant, T.K., P. Liu, R.R. Rampersad, D. Esserman, L.R. Rothlein, R.G. Timoshchenko, M.W. McGinnis, D.J. Fitzhugh, D.D. Patel, and A.M. Fong. 2012. Decreased Th17 and antigen-specific humoral responses in CX(3) CR1-deficient mice in the collagen-induced arthritis model. Arthritis and Rheumatism 64 (5): 1379–1387. https://doi.org/10.1002/art.34320.
Gal-Oz, S.T., B. Maier, H. Yoshida, K. Seddu, N. Elbaz, C. Czysz, O. Zuk, B.E. Stranger, H. Ner-Gaon, and T. Shay. 2019. ImmGen report: Sexual dimorphism in the immune system transcriptome. Nature Communications 10 (1): 4295. https://doi.org/10.1038/s41467-019-12348-6.
Fuseini, H., J.Y. Cephus, P. Wu, J.B. Davis, D.C. Contreras, V.D. Gandhi, J.C. Rathmell, and D.C. Newcomb. 2019. ERalpha signaling increased IL-17A production in Th17 cells by upregulating IL-23R expression, mitochondrial respiration, and proliferation. Frontiers in Immunology 10: 2740. https://doi.org/10.3389/fimmu.2019.02740.
Ruiz-Limon, P., R. Ortega-Castro, N. Barbarroja, C. Perez-Sanchez, C. Jamin, A.M. Patino-Trives, M. Luque-Tevar, et al. 2019. Molecular characterization of monocyte subsets reveals specific and distinctive molecular signatures associated with cardiovascular disease in rheumatoid arthritis. Frontiers in Immunology 10: 1111. https://doi.org/10.3389/fimmu.2019.01111.
Ha, H., H.B. Kwak, S.W. Lee, H.M. Jin, H.M. Kim, H.H. Kim, and Z.H. Lee. 2004. Reactive oxygen species mediate RANK signaling in osteoclasts. Experimental Cell Research 301 (2): 119–127. https://doi.org/10.1016/j.yexcr.2004.07.035.
Lo, Y.Y., and T.F. Cruz. 1995. Involvement of reactive oxygen species in cytokine and growth factor induction of c-fos expression in chondrocytes. The Journal of Biological Chemistry 270 (20): 11727–11730. https://doi.org/10.1074/jbc.270.20.11727.
Availability of Data and Material
Data available upon request.
Funding
The study was funded by the Ministry of Education, Science and Technological Development of the Republic of Serbia (grants no 451-03-68/2020-14/200161 and 451-03-68/2020-14/200007).
Author information
Authors and Affiliations
Contributions
Conception and design of the study: M.D. and G.L. Acquisition, analysis, and interpretation of data: N.A-R., D.K., B.B., I.P., M.N-A., J.K-S., L.S., J.S., and M.D. Drafting the manuscript: N.A-R. and M.D. Critical revision of the manuscript: G.L.
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
All experimental procedures and animal care were performed in keeping with the Directive 2010/63/EU of the European Parliament and of the Council on the protection of animals used for scientific purposes and the governmental regulations (The Law on Animal Welfare, “Official Gazette of Republic of Serbia”, no. 41/2009) and approved by The Ministry of Agriculture, Forestry and Water Economy of the Republic of Serbia (permit no. 323-07-01577/2016-05/14). The ARRIVE guidelines for reporting animal research were fully implemented in the study.
Statement of Informed Consent
Not applicable.
Consent for Publication
Not applicable
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Supplementary Fig. 1
Sex differences in the clinical and histological presentation of CIA. (a) A line graph indicates daily arthritic score (mean ± SEM) from the 12th to the 39th day post-immunization (d.p.i.) in male (n = 9) and female (n = 10) CIA rats. Mann–Whitney U test: * p ≤ 0.05, from the 17th to the 39th d.p.i. (b) Line graph indicates daily arthritic score (mean ± SEM) from the 13th to the 21st day post-immunization (d.p.i.) in male and female CIA rats. Mann–Whitney U test: n = 8 rats/sex. * p ≤ 0.05. Photographs show representative arthritic joints (arrows) of hind paws from male and female CIA rats. (c) Photomicrographs of HE-stained sections of paraffin-embedded joints from male and female CIA rats show replacement of the normal bone marrow cell populations by inflammatory cells. In females, numerous multinuclear giant cells (red arrows) are present as opposed to male CIA rats. Original magnification × 400. The bar indicates 100 μm (PNG 2723 kb)
Supplementary Fig. 2
Fluorescence minus one controls for flow cytometry analysis of CD11b/CCR2/CX3CR1 staining of splenocytes. For setting cutoff boundaries, gates were controlled using fluorescence minus one (FMO) controls obtained by omitting a single antibody from the labeling antibody cocktail. Flow cytometry dot plots represent FMO controls without anti-CX3CR1 or anti-CCR2 Abs within CD11b+ splenocytes (gated as shown in Fig. 3) isolated from CIA rats on the 21st day post-immunization (PNG 98 kb).
Supplementary Fig. 3
Fluorescence minus one controls for flow cytometry analysis of CD11b/CD43/CCR2/CX3CR1 staining of peripheral blood cells. For setting cutoff boundaries, gates were controlled using fluorescence minus one (FMO) controls obtained by omitting a single antibody from the labeling antibody cocktail. Flow cytometry dot plots represent FMO controls without (upper) CD43 mAb within CD11b+ peripheral blood cells (gated as shown in Fig. 4a) and (lower) anti-CX3CR1 or anti-CCR2 Abs within CD11b+CD43+ peripheral blood cells isolated from CIA rats on the 21st day post-immunization (PNG 157 kb).
Supplementary Fig. 4
Sex differences in the activation of Th cells, Th17 cell function, and frequency of CD40+CD11b+ antigen presenting cells in draining lymph nodes from CIA rats, popliteal draining lymph nodes (DLNs) were retrieved from male and female CIA rats on the 21st day post-immunization. (a) Scatter plots with bar indicate the frequencies of activated Th cells (CD25+Foxp3-CD4+) and Th17 cells (IL-17+CD4+TCRαβ+) in DLNs from CIA rats and the concentration of IL-17 in supernatants of collagen type II-stimulated and unstimulated (medium) DLN cell cultures from male and female rats (see MATERIAL AND METHODS). Linear graph shows the correlation between the frequency of activated Th cells (CD25+Foxp3-CD4+) and the frequency of Th17 cells (IL-17+CD4+TCRαβ+) in DLNs from CIA rats. Pearson’s r value is shown in the graph. (b) Representative flow cytometry dot plots show (upper) CD11b staining and (lower) CD40 vs CD11b staining of DLN cells from male and female rats. Number indicates percent in the region. Scatter plots with bar indicate the frequency and the number of (upper) CD11b+ cells and (lower) CD40+CD11b+ cells in DLNs of male and female rats. The Number indicates percent in the region. Results are expressed as mean ± SEM. (c) The linear graph shows the correlation between the frequency of activated Th cells (CD25+Foxp3-CD4+) and the frequency of CD40+CD11b+ cells in DLNs from CIA rats. Pearson’s r value is shown in the graph. n = 8 rats/sex. * p ≤ 0.05, ** p ≤ 0.01, and *** p ≤ 0.001 (PNG 590 kb).
Supplementary Fig. 5
Gating strategy for activated Th cells and Th17 cells, popliteal draining lymph nodes (DLNs) were retrieved from CIA rats on the 21st day post-immunization. Flow cytometry dot plots show gating strategy for (a) activated The cells (CD25+Foxp3-CD4+) and (b) Th17 cells (IL-17+CD4+TCRαβ+) (PNG 101 kb).
Rights and permissions
About this article
Cite this article
Dimitrijević, M., Arsenović-Ranin, N., Bufan, B. et al. Sex-Based Differences in Monocytic Lineage Cells Contribute to More Severe Collagen-Induced Arthritis in Female Rats Compared with Male Rats. Inflammation 43, 2312–2331 (2020). https://doi.org/10.1007/s10753-020-01302-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-020-01302-0