Abstract
Background
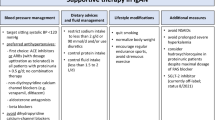
Chloroquine, an antimalarial agent, has been reported to prevent the risk of thrombosis and decrease renal damage in patients with systemic lupus erythematosus (SLE); however, its detailed mechanisms remain unclear. Plasminogen activator inhibitor-1 (PAI-1) is an inhibitor of fibrinolysis and is involved in fibrin deposition in glomeruli. Since upregulation of glomerular Toll-like receptor 3 (TLR3) signaling reportedly plays a pivotal role in the pathogenesis of lupus nephritis (LN), we examined whether chloroquine affects TLR3-mediated expression of PAI-1 in cultured human glomerular endothelial cells (GECs).
Methods
We examined the effect of polyinosinic-polycytidylic acid (poly IC), an authentic double-stranded RNA, on PAI-1 and tissue plasminogen activator (t-PA) expression in GECs. Then, we analyzed whether pretreatment of chloroquine or dexamethasone inhibits poly IC-induced expression of these proteins using reverse-transcriptase polymerase chain reaction and enzyme-linked immunosorbent assay.
Results
Poly IC increased PAI-1 expression in a time- and concentration-dependent manner, but did not affect t-PA expression in GECs. RNA interference against TLR3 inhibited poly IC-induced PAI-1 expression. Interestingly, pretreating cells with chloroquine, and also hydroxychloroquine, but not dexamethasone, attenuated poly IC-induced PAI-1 expression in GECs.
Conclusion
Considering that TLR3 signaling is implicated in LN pathogenesis, our results suggest that chloroquine exert postulated renoprotective effects by inhibiting PAI-1 expression.



Similar content being viewed by others
References
Wallace DJ, Gudsoorkar VS, Weisman MH, Venuturupalli SR. New insights into mechanisms of therapeutic effects of antimalarial agents in SLE. Nat Rev Rheumatol. 2012;8:522–33.
Tang C, Godfrey T, Stawell R, Nikpour M. Hydroxychloroquine in lupus: emerging evidence supporting multiple beneficial effects. Intern Med J. 2012;42:968–78.
Ruiz-Irastorza G, Egurbide MV, Pijoan JI, Garmendia M, Villar I, Martinez-Berriotxoa A, Erdozain JG, Aguirre C. Effect of antimalarials on thrombosis and survival in patient with systemic lupus erythematosus. Lupus. 2006;15:577–83.
Tektonidou MG, Laskari K, Panagiotakos DB, Moutsopoulos HM. Risk factors for thrombosis and primary thrombosis prevention in patient with systemic lupus erythematosus with or without antiphospholipid antibodies. Arthritis Rheum. 2009;61:29–36.
Bertsias G, Tektonidou M, Amoura Z, Aringer M, Bajema I, Berden JH, et al. Joint European League Against Rheumatism and European Renal Association-European Dialysis and Transplant Association (EULAR/ERA-EDTA) recommendations for the management of adults and paediatric lupus nephritis. Ann Rheum Dis. 2012;71:1771–82.
Hamano K, Iwano M, Akai Y, Sato H, Kubo A, Nishitani Y, Uyama H, Yoshida Y, Miyazaki M, Shiiki H, Kohno S, Dohi K. Expression of glomerular plasminogen activator inhibitor type 1 in glomerulonephritis. Am J Kidney Dis. 2002;39:695–705.
Hagberg N, Rönnblom L. Systemic lupus erythematosus—a disease with a dysregulated type I interferon system. Scand J Immunol. 2015;82:199–207.
Anders HJ. Pseudoviral immunity—a novel concept for lupus. Trends Mol Med. 2009;15:553–61.
Hägele H, Allam R, Pawar RD, Anders HJ. Double-stranded RNA activates type I interferon secretion in glomerular endothelial cells via retinoic acid-inducible gene (RIG)-I. Nephrol Dial Transplant. 2009; 24: 3312–8.
Wörnle M, Roeder M, Sauter M, Merkle M, Ribeiro A. Effect of dsRNA on mesangial cell synthesis of plasminogen activator inhibitor type 1 and tissue plasminogen activator. Nephron Exp Nephrol. 2009;113:e57–65.
Tanaka H, Imaizumi T. Inflammatory chemokine expression via toll-like receptor 3 signaling in normal human mesangial cells. Clin Dev Immunol. 2013;2013:984708. https://doi.org/10.1155/2013/984708.
Imaizumi T, Aizawa T, Hayakari R, Xing F, Meng P, Tsuruga K, Matsumiya T, Yoshida H, Wang L, Tatsuta T, Tanaka H. Tumor necrosis factor-α synergistically enhances polyinosinic–polycytidylic acid-induced Toll-like receptor 3 signaling in cultured normal human mesangial cells: possible involvement in the pathogenesis of lupus nephritis. Clin Exp Nephrol. 2015;19:75–81.
Imaizumi T, Hayakari R, Matsumiya T, Yoshida H, Tsuruga K, Watanabe S, Kawaguchi S, Tanaka H. Chloroquine attenuates TLR3/IFN-β signaling in cultured normal human mesangial cells: a possible protective effect against renal damage in lupus nephritis. Mod Rheumatol. 2017;27:1004–9.
Liu Q, Imaizumi T, Kawaguchi S, Aizawa T, Matsumiya T, Watanabe S, Tsugawa K, Yoshida H, Tsuruga K, Joh K, Kijima H, Tanaka H. Toll-like receptor 3 signaling contributes to regional neutrophil recruitment in cultured human glomerular endothelial cells. Nephron. 2018;139:349–58.
Bhargavan B, Kanmogne GD. Toll-like receptor-3 mediates HIV-1-induced interleukin-6 expression in the human brain endothelium via TAK1 and JNK pathways: implication for viral neuropathogenesis. Mol Neurobiol. 2018;55:5976–92.
Keeton M, Ahn C, Eguchi Y, Burlingame R, Loskutoff DJ. Expression of type 1 plasminogen activator inhibitor in renal tissue in murine lupus nephritis. Kidney Int. 1995;47:148–57.
Imaizumi T, Hayakari R, Watanabe S, Aizawa T, Matsumiya T, Yoshida H, Tsuruga K, Kawaguch S, Tanaka H. Cylindromatosis (CYLD), a deubiquitinase, attenuates inflammatory signaling pathways by activating Toll-like receptor 3 in human mesangial cells. Kidney Blood Press Res. 2017;42:942–50.
Acknowledgements
This study was supported by Grants-in-Aid of the Japan Society for Promotion of Science (JSPS KAKENHI Grant number: 16K10055 to H. T.).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Ethical approval
This study was not involved human subjects which required ethical approval.
About this article
Cite this article
Aizawa, T., Imaizumi, T., Hirono, K. et al. Chloroquine attenuates TLR3-mediated plasminogen activator inhibitor-1 expression in cultured human glomerular endothelial cells. Clin Exp Nephrol 23, 448–454 (2019). https://doi.org/10.1007/s10157-018-1659-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10157-018-1659-y