Abstract
Breast reconstruction (BR) aims to improve the satisfaction and quality of life (QOL) of breast cancer survivors. Clinical studies using patient-reported outcomes (PROs) can therefore provide relevant information to the patients and support decision-making. This scoping review was conducted to analyze recent trends in world regions, methods used, and factors investigated. The literature search was conducted in August 2022. Databases of PubMed, MEDLINE, and CINAHL were searched for relevant English-language studies published from 2017 to 2022. Studies involving women with breast cancer who underwent BR after mastectomy and investigated PROs after BR using BR-specific scales were included. Data on the country, publication year, study design, PRO measures (PROMs) used, time points of surveys, and research themes were collected. In total, 147 articles met the inclusion criteria. BREAST-Q was the most widely used, contributing to the increase in the number and diversification of studies in this area. Such research has been conducted mainly in North America and Europe and is still developing in Asia and other regions. The research themes involved a wide range of clinical and patient factors in addition to surgery, which could be influenced by research methods, time since surgery, and even cultural differences. Recent BR-specific PROMs have led to a worldwide development of research on factors that affect satisfaction and QOL after BR. PRO after BR may be influenced by local cultural and social features, and it would be necessary to accumulate data in each region to draw clinically useful conclusion.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Currently, surgical strategies for breast cancer are becoming increasingly diverse, including the development of breast reconstruction (BR) techniques and the widespread of prophylactic mastectomy. BR aims to improve the body image and quality of life (QOL) of breast cancer survivors; however, patients must choose the best treatment for themselves, considering implant-specific issues, donor-site sacrifice, psychological burden, costs, and physical and social rehabilitation. Thus, to help patients make a choice suitable for their situation and preferences, information on the advantages and disadvantages of each option in terms of QOL, complications, and aesthetic outcomes is necessary.
Outcome evaluation using patient-reported outcomes (PROs) is helpful for these areas. It enables scientifically quantify multidimensional outcomes that are only known to the patient, contributes to the consideration of patient-centered treatment strategies, supports decision making, and improves the quality of healthcare [1]. Only objective esthetic and symmetry evaluation has been used to assess BR outcomes in the past; however, with the advent of well-validated BR-specific PRO measures (PROMs) [2, 3], deep understanding of various aspects of patient’s life, such as body image, pain, ease of bra wear, and psychological aspects, has become possible.
Although these BR-specific measures have been incorporated into clinical studies and have deepened research on QOL after BR, the influencing factors are diverse and complex, and the evidence remains insufficient [4,5,6]. A scoping review of articles published in the last 5 years on this area was conducted to map and organize which world regions, which methods, and which factors were investigated. This review aimed to analyze the trend of studies, rather than study outcomes, to guide future research planning.
Methods
This scoping review was conducted according to the principles of the Preferred Reporting Items for Systematic Reviews and Meta-Analyses statement [7]. The following question guided the mapping of this scoping review: What world regions, what research methods are being used, and what research questions are being investigated in recent clinical studies on satisfaction and QOL after mastectomy and BR?
Literature search
The literature search was conducted in August 2022. PubMed, MEDLINE, and CINAHL databases were searched for relevant English-language studies published from 2017 to 2022. The combination of search terms “breast reconstruction” and “breast cancer” with “patient-reported outcomes” or “satisfaction” or “quality of life” was used.
Selection of eligible studies
The inclusion and exclusion criteria were predetermined to select the relevant studies. The studies were included if it fulfilled all of following criteria: (1) studies involving women with breast cancer or with hereditary breast and ovarian cancer syndrome (HBOC) and underwent therapeutic or prophylactic mastectomy (PM), (2) studies involving women who underwent immediate BR (IBR) or delayed BR (DBR), (3) studies that assessed postoperative satisfaction and QOL using the BR-specific PROMs (namely, BREAST-Q [8, 9], Breast Reconstruction Satisfaction Questionnaire (BRECON-31) [10,11,12], and the European Organization for Research and Treatment of Cancer Quality of life Questionnaire BRR26 (EORTC QLQ-BRR26) [13, 14], which were assessed as well-developed in a previous study), and examined factors that affect them [2], and (4) any type of BR including autologous and implant-based BR, and secondary procedures such as fat grafting, nipple reconstruction, contralateral symmetrization.
The exclusion criteria were as follows: (1) studies about BR following breast conserving surgery (BCS), (2) studies that compared BR with MT and BCS, and (3) opinion, review, letter, meta-analysis, case report, case series, pre-post study, qualitative study.
Two reviewers (MS and RN) independently screened the title and abstracts to determine whether the studies met the criteria. Disagreements were resolved by further discussion between the two reviewers.
Data collection, analysis, and reporting of results
After determining studies eligible for inclusion in the final review, data were extracted by a reviewer (MS) to identify the following aspects: (a) region and country of the first author, (b) publication year, (c) study design, (d) PROM used, (e) time point of the PRO survey, and (f) research theme. Endnote and Excel were used for the management and analysis of studies.
The number of publications was described by country, year, and methodology of PRO investigation. The main themes of the study were divided into the following four categories: (i) factors related to reconstructive surgery, (ii) clinical factors related to indication and treatment, (iii) patient factors, and (iv) factors affecting QOL and satisfaction. After the categorization was reconfirmed by another reviewer (RN), the distribution of study themes by region was analyzed.
Results
In total, 1177 studies were retrieved from the literature search, 294 full texts were reviewed, and 147 articles were included in the final analysis (Fig. 1).
Region and publication year
Table 1 shows the countries of affiliation of the first author. Of the 147 studies, 69 (46.9%) were from North America, followed by 57 (38.8%) from Europe. Moreover, 17 (11.6%) papers were from Asia, of which more than half were from China. Very few papers were published from the rest of the world.
As shown in the number of publications each year by region, the number consistently exceeds 10 in North America and is increasing in Europe and other regions (Fig. 2).
Method to investigate PROs
Table 2 shows the characteristic regarding the methodology of the studies included, which were as follows: 76 (51.7%) cross-sectional studies, 23 (15.6%) retrospective cohort, 42 (28.6%) prospective studies, and 6 (4.1%) randomized controlled trials (RCT). Propensity-score matching analysis was used in three cross-sectional and two retrospective cohort studies.
The BREAST-Q was utilized in most of the studies. Preoperative baseline surveys were conducted in 51 (34.7%) studies. The timing of the postoperative survey was defined in 65 (44.2%) of the studies, whereas others were not clearly defined (36.7%), had only a lower limit such as “six months or more” (16.3%), or were broad to include years (2.7%).
Study themes
The classification of the main themes of the studies is presented in Table 3. Eighty-one (55.1%) studies were classified into BR surgery-related themes. Of which these studies, 20 (13.6%) compared autologous-tissue BR (ATBR) and implant-based BR (IBBR) [15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34]. Eight (5.4%) studies focused on ATBR-specific themes, which included three studies that compared ATBR types [35,36,37] and five studies that focused on abdominal-based flap techniques and various topics: laterality of pedicle [38], utilization of indocyanine green angiography [39], studies on the recipient vessels [40], nerve coaptation to the sensory nerve [41], and vascularized lymph node transfer performed simultaneously [42]. IBBR-specific themes were the most common topic of 34 (23.1%) studies, which included 10 studies that compared the direct-to-implant (DTI) procedure with staged procedure [43,44,45,46,47,48,49,50,51,52], 9 that compared subpectoral DTI with and without mesh support [53,54,55,56,57,58,59,60,61], 7 that compared subpectoral and pre-pectoral implant insertion [62,63,64,65,66,67,68], 4 that compared mesh types [69,70,71,72], 2 that compared implant types [73, 74], and 2 that were related to animation deformity [75, 76]. This reflects the transition in technique from conventional sub-pectoral, two-staged procedure to pre-pectoral, direct-to-implant procedure because of the widespread use of biological matrix and synthetic mesh. Moreover, 10 studies (6.8%) focused on mastectomy, of which six compared nipple-sparing mastectomy (NSM) with non-NSM [77,78,79,80,81,82], two analyzed NSM incision [83, 84], and two evaluated two new techniques: robotic mastectomy and IBBR [85] and endoscopic-assisted NSM and latissimus dorsi flap (LD) reconstruction [86]. In addition, 3 (2.0%) studies analyzed postoperative factors, of which 2 were about complications after BR, and one was about time since surgery. Furthermore, 6 (4.1%) studies examined surgical procedures other than primary breast reconstructive surgery, of which 3 analyzed re-reconstruction after failed IBBR [87,88,89], 2 evaluated fat grafting [90, 91], and 1 focused on contralateral symmetry procedure [92].
Thirty-nine (26.5%) studies were classified into the clinical theme. Of these studies, 20 (13.6%) assessed the effect of radiotherapy (RT) on ATBR [93,94,95,96,97,98,99], IBBR [100,101,102,103,104,105,106,107,108,109], or both [110,111,112]. Seven of these studies discussed the timing of BR and RT [95,96,97,98,99, 104, 108]. Moreover, 1 (0.7%) study examined the influence of chemotherapy [113], 3 (2.0%) compared immediate and delayed reconstruction [114,115,116], and 5 (3.4%) compared unilateral and bilateral reconstructions [117,118,119,120,121]. Eight studies with clinical themes (5.4%) focused on HBOC and PM, in which the issues to consider were complex, namely whether to perform contralateral PM in women with unilateral breast cancer [122,123,124] and compare them with women with bilateral breast cancer [125], comparison between BPM cases with and without previous cancer [126,127,128], and comparison between IBBR and ATBR for women with BRCA mutation [129]. Furthermore, 2 (1.4%) studies examined healthcare services such as the treating hospital [130] and the sex of the plastic surgeon [131].
Moreover, 21 (14.3%) studies had patient-related themes, of which 17 (11.6%) were on baseline characteristics. Obesity was the most frequently studied factor [132,133,134,135,136,137], followed by age [138,139,140] and pre-existing psychiatric problems [141,142,143]. Other baseline characteristics included race [144, 145], overall health status [146], socioeconomic status [147], and history of previous augmentation surgery [148]. Four studies (2.7%) examined the effect of postoperative patient factors such as postoperative opioid consumption [149], financial burden of BR [150], disparity between patient and observer perceptions of outcomes [151], and psychosocial well-being [152].
Six studies (4.1%) explored predictors of satisfaction and QOL after BR [153,154,155,156,157,158]. The factors extracted from these studies were nicotine dependence [155], antibody treatment [155], lymphedema [155], breast sensitivity [154], pain [154], scar thickness [154], time since surgery [153, 154], preoperative and postoperative psychosocial well-being [154, 156], preoperative sexual wellbeing [156], preoperative physical well-being of abdomen [157], reconstructive procedure [153], and race [157].
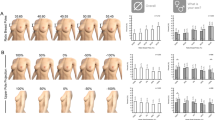
Figure 3 shows the distribution of the study themes by world regions. Studies on reconstructive techniques and treatment strategies have been conducted in all regions; however, studies on patient factors such as obesity, race, and age have been conducted mainly in North America.
Distribution of study themes by region. ATBR autologous-tissue breast reconstruction, BR breast reconstruction, DBR delayed breast reconstruction, HBOC hereditary breast and ovarian cancer syndrome, IBBR implant-based breast reconstruction, IBR immediate breast reconstruction, PM prophylactic mastectomy, RT radiation therapy
Discussion
BR-specific PROMs developed in North America and Europe have been translated and disseminated in many countries, and the BREAST-Q is now the most used worldwide, contributing to the increase in the number and diversification of studies in satisfaction and QOL after BR.
As regards recent trends in research themes, in addition to the basic theme of autologous tissues in comparison with implants, optimization of the outcomes of each surgery by stratifying treatment factors and patient factors has been investigated. Studies have also discussed ATBR techniques based on abdominal flap BR to further improve the QOL of patients; however, the introduction of new surgical materials such as acellular dermal matrices (ADM) has led to changes in surgical techniques in IBBR, and many studies have evaluated new techniques from the perspective of patient satisfaction and QOL.
Another major focus of the world is radiation therapy. Since BR is a part of breast cancer treatment, the timing of treatment and reconstruction is a major clinical issue. As patient factors, in addition to demographic factors such as race and age, obesity, preoperative psychiatric disorders, and postoperative psychological aspects are being considered, and these studies have been conducted mainly in North America. These patient factors should be considered potential confounders in future clinical studies. In clinical practice, patient education on these factors and patient support from the preoperative to the postoperative period were suggested to improve postoperative satisfaction and QOL.
Studies using BR-specific measures were expected to accumulate and be integrated into future meta-analyses with a higher level of evidence. However, potential barriers are the quality of each study [4, 5, 159] and the heterogeneity of cultural regions [5].
Regarding the methodology of the PRO surveys analyzed in this review, only six RCTs have been conducted in five years [28, 44, 57, 58, 71, 85]. In BR, where the patient makes the decision, RCTs are difficult to conduct ethically, especially in determining surgical techniques. A strategy to compensate for the limitations of observational studies in these areas is to employ propensity-matched analysis to adjust for confounding [5], which was performed in three cross-sectional studies [24, 26, 123] and two retrospective cohort studies [30, 68]. There were 42 prospective cohort studies, of which 22 were reported in the Mastectomy Reconstruction Outcomes Consortium (MROC) study [15, 19]. MROC was conducted in 11 institutions in the United States and Canada, and PRO was evaluated longitudinally from before surgery to 2 years after surgery, and data were accumulated for various analyses including the effect of RT [93, 96, 104, 105, 111], age [138], race [144], and other factors. Such multicenter studies are a valuable reference for future clinical research. Gallo et al. stated that appropriate BREAST-Q administration, reporting of appropriate time horizon, and sample size calculations were important to ensure sufficient data quality [159]. In the present study, the time points of PRO surveys were clearly prespecified in 44.1% of the studies analyzed. Despite conflicting reports that satisfaction improves with time since surgery [115, 160] and conversely declines [23, 31, 153], the short-term and long-term results likely vary because women’s breast shape changes considerably with age, and implant-reconstructed breasts are deformed by capsular contracture. Therefore, the appropriate timing of evaluation should be determined in advance according to the purpose of the study.
Cultural backgrounds, women’s body shapes, and values differ among countries, and the response patterns and average values differ even with the same scale. Thus, the extent to which the findings of other county’s studies are applicable to Japanese populations is uncertain. They are more likely to be skinny than their Western counterparts, less likely to have large ptotic breasts, and have limited donor-site volume in the abdomen and thighs. Based on body shape, Asian studies may be more helpful for Japanese than for Westerners. For example, Cheng et al. analyzed 415 patients who underwent BR with abdominal free-flap BR in Taiwan, 76.8% were of normal weight (body mass index [BMI]; 18.5 < BMI < 24.9 kg/m2) and 23.2% were overweight (25 < BMI < 29.9 kg/m2) [137], whereas Srinivasa et al. reported that 24.3% of the 634 patients who underwent ATBR and enrolled in the MROC study were classified as normal weight, 34.5% as overweight, and 41.2% as class I or higher (29.9 kg/m2 < BMI) obese [136]. Differences between countries can also be seen in healthcare resources. Specifically, biomaterials such as ADMs cannot be used under Japanese health insurance; however, many of the IBBR-related studies included in this study involved cases in which ADM was used. This suggests that while the results of studies conducted in other countries are very informative, country-specific surveys and data accumulation are needed. Studies have also reported low response rates and low average values for the sexual well-being of Japanese women based on BREAST-Q [158, 161], and Japanese may have even lower scores than other Asian women [161]. A trend was found toward generating normative data for the interpretation of BREAST-Q [162,163,164]. Crittenden et al. reported that the Australian normative values were significantly lower than the US normative values on four of the five subscales [162], suggesting cultural and racial differences. Future work will require the creation of normative data in Japan to better understand the effect of BR.
This scoping review was conducted to map what studies on satisfaction and QOL after mastectomy and BR have been conducted, which demonstrated the increasing contribution of BR-specific PROMs worldwide and implied the need for further research in their respective culture using in appropriate methodology.
This study has several limitations. It dealt only with studies that measured postoperative satisfaction or QOL after mastectomy and BR. Therefore, important topics that may have influenced QOL after reconstructive surgery such as oncoplastic surgery [165], decision aids [166], and expectation management [167, 168] were not included in the analysis. Similarly, studies that utilized other valuable PROMs to investigate perioperative pain management, decision regrets, overall health status, etc., were excluded. The authors also recognize the need to consider sample size calculations [159] and minimally important difference [169] estimation in planning future studies using PROs.
In conclusion, recent BR-specific PROMs have led to a worldwide development of research on factors that affect satisfaction and QOL after BR, including a wide range of surgical, clinical, and patient factors. PROs after BR may be influenced by local cultural and social features; thus, accumulating data in each region is necessary.
References
Winters ZE, Benson JR, Pusic AL (2010) A systematic review of the clinical evidence to guide treatment recommendations in breast reconstruction based on patient- reported outcome measures and health-related quality of life. Ann Surg 252(6):929–942
Davies CF, Macefield R, Avery K et al (2021) Patient-reported outcome measures for post-mastectomy breast reconstruction: a systematic review of development and measurement properties. Ann Surg Oncol 28(1):386–404
Platt J, Zhong T (2018) Patient-centered breast reconstruction based on health-related quality-of-life evidence. Clin Plast Surg 45(1):137–143
Zehra S, Doyle F, Barry M et al (2020) Health-related quality of life following breast reconstruction compared to total mastectomy and breast-conserving surgery among breast cancer survivors: a systematic review and meta-analysis. Breast Cancer 27(4):534–566
Saldanha IJ, Cao W, Broyles JM et al (2021) Breast reconstruction after mastectomy: a systematic review and meta-analysis, Comparative Effectiveness Review No. 245. (Prepared by the Brown Evidence-based Practice Center under Contract No. 75Q80120D00001.) AHRQ Publication No. 21-EHC027. Rockville, MD: Agency for Healthcare Research and Quality; July 2021. https://doi.org/10.23970/AHRQEPCCER245
Khajuria A, Charles WN, Prokopenko M et al (2020) Immediate and delayed autologous abdominal microvascular flap breast reconstruction in patients receiving adjuvant, neoadjuvant or no radiotherapy: a meta-analysis of clinical and quality-of-life outcomes. BJS Open 4(2):182–196
Tricco AC, Lillie E, Zarin W et al (2018) PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med 169(7):467–473
Cano SJ, Klassen AF, Scott AM et al (2012) The BREAST-Q: further validation in independent clinical samples. Plast Reconstr Surg 129(2):293–302
Pusic AL, Klassen AF, Scott AM et al (2009) Development of a new patient-reported outcome measure for breast surgery: the BREAST-Q. Plast Reconstr Surg 124(2):345–353
Temple CL, Cook EF, Ross DC et al (2010) Development of a breast reconstruction satisfaction questionnaire (BRECON): dimensionality and clinical importance of breast symptoms, donor site issues, patient expectations, and relationships. J Surg Oncol 101(3):209–216
Temple-Oberle CF, Cook EF, Bettger-Hahn M et al (2012) Development of a breast reconstruction satisfaction questionnaire (BRECON-31): principal components analysis and clinimetric properties. J Surg Oncol 106(7):799–806
Temple-Oberle CF, Ayeni O, Cook EF et al (2013) The breast reconstruction satisfaction questionnaire (BRECON-31): an affirmative analysis. J Surg Oncol 107(5):451–455
Thomson HJ, Winters ZE, Brandberg Y et al (2013) The early development phases of a European Organisation for Research and Treatment of Cancer (EORTC) module to assess patient reported outcomes (PROs) in women undergoing breast reconstruction. Eur J Cancer 49(5):1018–1026
Winters ZE. Balta V, Thomson HJ et al (2014) Phase III development of the European organization for research and treatment of cancer quality of life questionnaire module for women undergoing breast reconstruction. Br J Surg 101(4):371–382
Pusic AL, Matros E, Fine N et al (2017) Patient-reported outcomes 1 year after immediate breast reconstruction: results of the mastectomy reconstruction outcomes consortium study. J Clin Oncol 35(22):2499–2506
Jeevan R, Browne JP, Gulliver-Clarke C et al (2017) Surgical determinants of patient-reported outcomes following postmastectomy reconstruction in women with breast cancer. Plast Reconstr Surg 139(5):1036e–1045e
Pirro O, Mestak O, Vindigni V et al (2017) Comparison of patient-reported outcomes after implant versus autologous tissue breast reconstruction using the BREAST-Q. Plast Reconstr Surg Glob Open 5(1):e1217
Thorarinsson A, Frojd V, Kolby L et al (2017) Long-term health-related quality of life after breast reconstruction: comparing 4 different methods of reconstruction. Plast Reconstr Surg Glob Open 5(6):e1316
Santosa KB, Qi J, Kim HM et al (2018) Long-term patient-reported outcomes in postmastectomy breast reconstruction. JAMA Surg 153(10):891–899
Fracon S, Renzi N, Manara M et al (2018) Patient satisfaction after breast reconstruction: implants vs. autologous tissues. Acta Chir Plast 59(3–4):120–128
Alshammari SM, Aldossary MY, Almutairi K et al (2019) Patient-reported outcomes after breast reconstructive surgery: a prospective cross-sectional study. Ann Med Surg (Lond) 39:22–25
Nelson JA, Allen RJ Jr, Polanco T et al (2019) Long-term patient-reported outcomes following postmastectomy breast reconstruction: an 8-year examination of 3268 patients. Ann Surg 270(3):473–483
Duraes EFR, Schwarz GS, de Sousa JB et al (2020) Factors influencing the aesthetic outcome and quality of life after breast reconstruction: a cross-sectional study. Ann Plast Surg 84(5):494–506
Kouwenberg CAE, de Ligt KM, Kranenburg LW et al (2020) Long-term health-related quality of life after four common surgical treatment options for breast cancer and the effect of complications: a retrospective patient-reported survey among 1871 patients. Plast Reconstr Surg 146(1):1–13
Ticha P, Mestak O, Wu M et al (2020) Patient-reported outcomes of three different types of breast reconstruction with correlation to the clinical data 5 years postoperatively. Aesthetic Plast Surg 44(6):2021–2029
He S, Ding B, Li G et al (2021) Comparison of outcomes between immediate implantbased and autologous reconstruction: 15-year, single-center experience in a propensity score-matched Chinese cohort. Cancer Biol Med 19(9):1410–1421
Misere RM, van Kuijk SM, Claassens EL et al (2021) Breast-related and body-related quality of life following autologous breast reconstruction is superior to implant-based breast reconstruction - a long-term follow-up study. Breast 59:176–182
Tallroth L, Velander P, Klasson S (2021) A short-term comparison of expander prosthesis and DIEP flap in breast reconstructions: a prospective randomized study. J Plast Reconstr Aesthet Surg 74(6):1193–1202
Cai L, Momeni A (2022) The impact of reconstructive modality and postoperative complications on decision regret and patient-reported outcomes following breast reconstruction. Aesthetic Plast Surg 46(2):655–660
Nelson JA, Shamsunder MG, Myers PL et al (2022) Matched preliminary analysis of patient-reported outcomes following autologous and implant-based breast reconstruction. Ann Surg Oncol 29(8):5266–5275
Shiraishi M, Sowa Y, Tsuge I et al (2022) Long-term patient satisfaction and quality of life following breast reconstruction using the BREAST-Q: a prospective cohort study. Front Oncol 12:815498
Persichetti P, Barone M, Salzillo R et al (2022) Impact on patient’s appearance perception of autologous and implant based breast reconstruction following mastectomy using BREAST-Q. Aesthetic Plast Surg 46(3):1153–1163
Wolska J, Ammari T, Turnbull A et al (2022) Comparison of long-term outcomes of breast conservation and reconstruction after mastectomy using BREAST-Q. J Plast Reconstr Aesthet Surg 75(9):2930–2940
Gao P, Bai P, Kong X et al (2022) Patient-reported outcomes and complications following breast reconstruction: a comparison between biological matrix-assisted direct-to-implant and Latissimus Dorsi Flap. Front Oncol 12:766076
Erdmann-Sager J, Wilkins EG, Pusic AL et al (2018) Complications and patient-reported outcomes after abdominally based breast reconstruction: results of the mastectomy reconstruction outcomes consortium study. Plast Reconstr Surg 141(2):271–281
Atisha DM, Tessiatore KM, Rushing CN et al (2019) A national snapshot of patient-reported outcomes comparing types of abdominal flaps for breast reconstruction. Plast Reconstr Surg 143(3):667–677
Opsomer D, Vyncke T, Ryx M et al (2020) Comparing the lumbar and SGAP flaps to the DIEP flap using the BREAST-Q. Plast Reconstr Surg 146(3):276e–282e
Sergesketter AR, Shammas RL, Taskindoust M et al (2021) A Comparison of patient-reported outcomes in bipedicled total abdominal versus unipedicled hemiabdominal free flaps for unilateral breast reconstruction. J Reconstr Microsurg 37(9):753–763
Malagon-Lopez P, Vila J, Carrasco-Lopez C et al (2019) Intraoperative indocyanine green angiography for fat necrosis reduction in the deep inferior epigastric perforator (DIEP) flap. Aesthet Surg J 39(4):NP45–NP54
Ho OA, Lin YL, Pappalardo M et al (2018) Nipple-sparing mastectomy and breast reconstruction with a deep inferior epigastric perforator flap using thoracodorsal recipient vessels and a low lateral incision. J Surg Oncol 118(4):621–629
Cornelissen AJM, Beugels J, van Kuijk SMJ et al (2018) Sensation of the autologous reconstructed breast improves quality of life: a pilot study. Breast Cancer Res Treat 167(3):687–695
Di Taranto G, Coleman GJ, Hardwicke J et al (2022) A comparative study between deep inferior epigastric artery perforator flap breast reconstruction and DIEP flap breast reconstruction coupled with vascularized lymph node transfer: improving the quality of life of patients with breast cancer related lymphedema without affecting donor site outcomes. Microsurgery 43:213–221
Srinivasa DR, Garvey PB, Qi J et al (2017) Direct-to-implant versus two-stage tissue expander/implant reconstruction: 2-year risks and patient-reported outcomes from a prospective multicenter study. Plast Reconstr Surg 140(5):869–877
Negenborn VL, Young-Afat DA, Dikmans REG et al (2018) Quality of life and patient satisfaction after one-stage implant-based breast reconstruction with an acellular dermal matrix versus two-stage breast reconstruction (BRIOS): primary outcome of a randomised, controlled trial. Lancet Oncol 19(9):1205–1214
Cattelani L, Polotto S, Arcuri MF et al (2018) One-step prepectoral breast reconstruction with dermal matrix-covered implant compared to submuscular implantation: functional and cost evaluation. Clin Breast Cancer 18(4):e703–e711
Ghilli M, Mariniello MD, Camilleri V et al (2020) PROMs in post-mastectomy care: patient self-reports (BREAST-Q) as a powerful instrument to personalize medical services. Eur J Surg Oncol 46(6):1034–1040
Caputo GG, Vigato E, Rampino Cordaro E et al (2021) Comparative study of patient outcomes between direct to implant and two-stage implant-based breast reconstruction after mastectomy. J Plast Reconstr Aesthet Surg 74(10):2573–2579
Gao P, Bai P, Ren Y et al (2021) Biological matrix-assisted one-stage implant-based breast reconstruction versus two-stage implant-based breast reconstruction: patient-reported outcomes and complications. Aesthetic Plast Surg 45(6):2581–2590
Innocenti A, Melita D, Affortunati M et al (2021) Immediate-implant-based-breast-reconstruction with two-stage expander-implant reconstruction versus one-stage-reconstruction with acellular dermal matrix: analysis of patients’ satisfaction. Acta Biomed 92(3):e2021228
Sgarzani R, Pasquali S, Buggi F et al (2021) Sub-muscular reconstruction after NAC sparing mastectomy: direct to implant breast reconstruction with human ADM versus tissue expander. Aesthetic Plast Surg 45(2):413–420
Dimovska EOF, Chen C, Chou HH et al (2021) Outcomes and quality of life in immediate one-stage versus two-stage breast reconstructions without an acellular dermal matrix: 17-years of experience. J Surg Oncol 124(4):510–520
Riggio E, Alfieri S, Toffoli E et al (2022) A descriptive comparison of satisfaction and well-being between expander-based and direct-to-implant breast reconstruction after Nipple-sparing Mastectomy. Aesthetic Plast Surg 47(1):30–39
Sorkin M, Qi J, Kim HM et al (2017) Acellular dermal matrix in immediate expander/implant breast reconstruction: a multicenter assessment of risks and benefits. Plast Reconstr Surg 140(6):1091–1100
Ganesh Kumar, Berlin NL, Kim HM N et al (2021) Development of an evidence-based approach to the use of acellular dermal matrix in immediate expander-implant-based breast reconstruction. J Plast Reconstr Aesthet Surg 74(1):30–40
Chen G, Zhang Y, Xue J et al (2019) Surgical outcomes of implant-based breast reconstruction using TiLoop Bra mesh combined with pectoralis major disconnection. Ann Plast Surg 83(4):396–400
Gao P, Wang Z, Kong X et al (2020) Comparisons of therapeutic and aesthetic effects of one-stage implant-based breast reconstruction with and without biological matrix. Cancer Manag Res 12:13381–13392
Lohmander F, Lagergren J, Johansson H et al (2020) Quality of life and patient satisfaction after implant-based breast reconstruction with or without acellular dermal matrix: randomized clinical trial. BJS Open 4(5):811–820
Lohmander F, Lagergren J, Johansson H et al (2021) Effect of immediate implant-based breast reconstruction after mastectomy with and without acellular dermal matrix among women with breast cancer: a randomized clinical trial. JAMA Netw Open 4(10):e2127806
Sewart E, Turner NL, Conroy EJ et al (2021) Patient-reported outcomes of immediate implant-based breast reconstruction with and without biological or synthetic mesh. BJS Open 5(1):zraa063
Wang S, He S, Zhang X et al (2021) Acellular bovine pericardium matrix in immediate breast reconstruction compared with conventional implant-based breast reconstruction. JPRAS Open 29:1–9
Wilson RL, Kirwan CC, O’Donoghue JM et al (2022) BROWSE: A multicentre comparison of nine year outcomes in acellular dermal matrix based and complete submuscular implant-based immediate breast reconstruction-aesthetics, capsular contracture and patient reported outcomes. Eur J Surg Oncol 48(1):73–81
Baker BG, Irri R, MacCallum V et al (2018) A prospective comparison of short-term outcomes of subpectoral and prepectoral strattice-based immediate breast reconstruction. Plast Reconstr Surg 141(5):1077–1084
Thangarajah F, Treeter T, Krug B et al (2019) Comparison of subpectoral versus prepectoral immediate implant reconstruction after skin- and nipple-sparing mastectomy in breast cancer patients: a retrospective hospital-based cohort study. Breast Care (Basel) 14(6):382–387
Manrique OJ, Kapoor T, Banuelos J et al (2020) Single-stage direct-to-implant breast reconstruction: a comparison between subpectoral versus prepectoral implant placement. Ann Plast Surg 84(4):361–365
Caputo GG, Zingaretti N, Kiprianidis I et al (2021) Quality of life and early functional evaluation in direct-to-implant breast reconstruction after mastectomy: a comparative study between prepectoral versus dual-plane reconstruction. Clin Breast Cancer 21(4):344–351
Le NK, Persing S, Dinis J et al (2021) A comparison of BREAST-Q scores between prepectoral and subpectoral direct-to-implant breast reconstruction. Plast Reconstr Surg 148(5):708e–714e
Ng EI, Quah GS, Graham S et al (2021) Immediate prepectoral implant reconstruction using TiLOOP Bra Pocket results in improved patient satisfaction over dual plane reconstruction. ANZ J Surg 91(4):701–707
Nelson JA, Shamsunder MG, Vorstenbosch J et al (2022) Prepectoral and subpectoral tissue expander-based breast reconstruction: a propensity-matched analysis of 90-day clinical and health-related quality-of-life outcomes. Plast Reconstr Surg 149(4):607e–616e
Hallberg H, Elander A, Kolby L et al (2019) A biological or a synthetic mesh in immediate breast reconstruction? A cohort-study of long-term health related quality of life (HrQoL). Eur J Surg Oncol 45(10):1812–1816
Ohlinger R, Alwafai Z, Paepke S et al (2021) Patient quality of life after subpectoral implant-based breast reconstruction with synthetic or biological materials. Anticancer Res 41(6):3075–3082
Stein MJ, Arnaout A, Lichtenstein JB et al (2021) A comparison of patient-reported outcomes between Alloderm and Dermacell in immediate alloplastic breast reconstruction: a randomized control trial. J Plast Reconstr Aesthet Surg 74(1):41–47
Gao P, Wang X, Bai P et al (2022) Clinical outcomes and patient satisfaction with the use of biological and synthetic meshes in one-stage implant-based breast reconstruction. Breast Cancer 29(3):450–457
Khavanin N, Clemens MW, Pusic AL et al (2017) Shaped versus round implants in breast reconstruction: a multi-institutional comparison of surgical and patient-reported outcomes. Plast Reconstr Surg 139(5):1063–1070
Vorstenbosch J, McCarthy CM, Shamsunder MG et al (2021) Smooth versus textured implant breast reconstruction: patient-reported outcomes and complications. Plast Reconstr Surg 148(5):959–967
Bernini M, Sordi S, Bembi N et al (2022) Selective denervation of pectoralis major muscle improves cosmetic outcome and quality of life in retro-pectoral implant based breast reconstruction. Clin Breast Cancer 22(1):60–66
Fracol M, Qiu CS, Chiu MW et al (2020) The relationship between animation deformity and patient-reported outcomes: application of the BREAST-Q to a quantitative stratification of animation severity. Plast Reconstr Surg 145(1):11–17
Bailey CR, Ogbuagu O, Baltodano PA et al (2017) Quality-of-life outcomes improve with nipple-sparing mastectomy and breast reconstruction. Plast Reconstr Surg 140(2):219–226
Romanoff A, Zabor EC, Stempel M et al (2018) A comparison of patient-reported outcomes after nipple-sparing mastectomy and conventional mastectomy with reconstruction. Ann Surg Oncol 25(10):2909–2916
Yoon-Flannery K, DeStefano LM, De La Cruz LM et al (2018) Quality of life and sexual well-being after nipple sparing mastectomy: a matched comparison of patients using the breast Q. J Surg Oncol 118(1):238–242
Opsomer D, Vyncke T, Depypere B et al (2021) Nipple reconstruction in autologous breast reconstruction after areola-sparing mastectomy. J Plast Reconstr Aesthet Surg 74(6):1223–1228
Santosa KB, Qi J, Kim HM et al (2021) Comparing Nipple-sparing mastectomy to secondary nipple reconstruction: a multi-institutional study. Ann Surg 274(2):390–395
Racz JM, Harless CA, Hoskin TL et al (2022) Sexual well-being after nipple-sparing mastectomy: does preservation of the nipple matter? Ann Surg Oncol 29:4167–4179
Corso G, De Lorenzi F, Vicini E et al (2018) Nipple-sparing mastectomy with different approaches: surgical incisions, complications, and cosmetic results preliminary results of 100 consecutive patients at a single center. J Plast Reconstr Aesthet Surg 71(12):1751–1760
Odom EB, Parikh RP, Um G et al (2018) Nipple-sparing mastectomy incisions for cancer extirpation prospective cohort trial: perfusion, complications, and patient outcomes. Plast Reconstr Surg 142(1):13–26
Toesca A, Sangalli C, Maisonneuve P et al (2022) A randomized trial of robotic mastectomy versus open surgery in women with breast cancer or BrCA mutation. Ann Surg 276(1):11–19
Qiu J, Wen N, Xie Y et al (2022) Novel technique for endoscopic-assisted nipple-sparing mastectomy and immediate breast reconstruction with endoscopic-assisted latissimus dorsi muscle flap harvest through a single axillary incision: a retrospective cohort study of comparing endoscopic and open surgery. Gland Surg 11(8):1383–1394
Haque S, Kanapathy M, Bollen E et al (2021) Patient-reported outcome and cost implication of acute salvage of infected implant-based breast reconstruction with negative pressure wound therapy with Instillation (NPWTi) compared to standard care. J Plast Reconstr Aesthet Surg 74(12):3300–3306
Asaad M, Slovacek C, Mitchell D et al (2022) Surgical and patient-reported outcomes of autologous versus implant-based reconstruction following infected breast device explantation. Plast Reconstr Surg 149(6):1080e–1089e
Shammas RL, Sergesketter AR, Taskindoust M et al (2022) Assessing the influence of failed implant reconstruction on patient satisfaction and decision regret after salvage free-flap breast reconstruction. J Reconstr Microsurg 38(6):441–450
Bennett KG, Qi J, Kim HM et al (2017) Association of fat grafting with patient-reported outcomes in postmastectomy breast reconstruction. JAMA Surg 152(10):944–950
Qureshi AA, Odom EB, Parikh RP et al (2017) Patient-reported outcomes of aesthetics and satisfaction in immediate breast reconstruction after nipple-sparing mastectomy with implants and fat grafting. Aesthet Surg J 37(9):999–1008
Razdan SN, Panchal H, Albornoz CR et al (2019) Impact of contralateral symmetry procedures on long-term patient-reported outcomes following unilateral prosthetic breast reconstruction. J Reconstr Microsurg 35(2):124–128
Cooke AL, Diaz-Abele J, Hayakawa T et al (2017) Radiation therapy versus no radiation therapy to the neo-breast following skin-sparing mastectomy and immediate autologous free flap reconstruction for breast cancer: patient-reported and surgical outcomes at 1 year-a mastectomy reconstruction outcomes consortium (MROC) substudy. Int J Radiat Oncol Biol Phys 99(1):165–172
Pont LP, Marcelli S, Robustillo M et al (2017) Immediate breast reconstruction with abdominal free flap and adjuvant radiotherapy: evaluation of quality of life and outcomes. Plast Reconstr Surg 140(4):681–690
He S, Yin J, Robb GL et al (2017) Considering the optimal timing of breast reconstruction with abdominal flaps with adjuvant irradiation in 370 consecutive pedicled transverse rectus abdominis myocutaneous flap and free deep inferior epigastric perforator flap performed in a chinese oncology center: is there a significant difference between immediate and delayed? Ann Plast Surg 78(6):633–640
Billig J, Jagsi R, Qi J et al (2017) Should Immediate autologous breast reconstruction be considered in women who require postmastectomy radiation therapy? A prospective analysis of outcomes. Plast Reconstr Surg 139(6):1279–1288
Steele KH, Macmillan RD, Ball GR et al (2018) Multicentre study of patient-reported and clinical outcomes following immediate and delayed autologous breast reconstruction and radiotherapy (ABRAR study). J Plast Reconstr Aesthet Surg 71(2):185–193
O’Connell RL, Di Micco R, Khabra K et al (2018) Comparison of immediate versus delayed diep flap reconstruction in women who require postmastectomy radiotherapy. Plast Reconstr Surg 142(3):594–605
Kamel GN, Nash D, Jacobson J et al (2019) Patient-reported satisfaction and quality of life in postmastectomy radiated patients: a comparison between delayed and delayed immediate autologous breast reconstruction in a predominantly minority patient population. J Reconstr Microsurg 35(6):445–451
Hamann M, Brunnbauer M, Scheithauer H et al (2019) Quality of life in breast cancer patients and surgical results of immediate tissue expander/implant-based breast reconstruction after mastectomy. Arch Gynecol Obstet 300(2):409–420
Tejera Hernandez AA, Vega Benitez VM, Rocca Cardenas JC et al (2019) Inverse radiotherapy planning in reconstructive surgery for breast cancer. Int J Surg 63:77–82
Thiboutot E, Craighead P, Webb C et al (2019) Patient-reported satisfaction following radiation of implant-based breast reconstruction. Plast Surg (Oakv) 27(2):147–155
Koppiker CB, Ul Noor A, Dixit S et al (2019) Implant-based breast reconstruction with autologous lower dermal sling and radiation therapy outcomes. Indian J Surg 81(6):543–551
Yoon AP, Qi J, Kim HM et al (2020) Patient-reported outcomes after irradiation of tissue expander versus permanent implant in breast reconstruction: a multicenter prospective study. Plast Reconstr Surg 145(5):917e–926e
Olinger TA, Berlin NL, Qi J et al (2020) Outcomes of immediate implant-based mastectomy reconstruction in women with previous breast radiotherapy. Plast Reconstr Surg 145(6):1029e–1036e
Seth AK, Cordeiro PG (2020) Stability of long-term outcomes in implant-based breast reconstruction: an evaluation of 12-year surgeon- and patient-reported outcomes in 3489 nonirradiated and irradiated implants. Plast Reconstr Surg 146(3):474–484
Coude Adam H, Frisell A, Liu Y et al (2021) Effect of radiotherapy on expanders and permanent implants in immediate breast reconstruction: long-term surgical and patient-reported outcomes in a large multicentre cohort. Br J Surg 108(12):1474–1482
Nelson JA, Cordeiro PG, Polanco T et al (2022) Association of radiation timing with long-term satisfaction and health-related quality of life in prosthetic breast reconstruction. Plast Reconstr Surg 150(1):32e–41e
Sewart E, Turner NL, Conroy EJ et al (2022) The impact of radiotherapy on patient-reported outcomes of immediate implant-based breast reconstruction with and without mesh. Ann Surg 275(5):992–1001
Devulapalli C, Bello RJ, Moin E et al (2018) The effect of radiation on quality of life throughout the breast reconstruction process: a prospective, longitudinal pilot study of 200 patients with long-term follow-up. Plast Reconstr Surg 141(3):579–589
Jagsi R, Momoh AO, Qi J et al (2018) Impact of radiotherapy on complications and patient-reported outcomes after breast reconstruction. J Natl Cancer Inst 110(2):157–165
Reinders FCJ, Young-Afat DA, Batenburg MCT et al (2020) Higher reconstruction failure and less patient-reported satisfaction after post mastectomy radiotherapy with immediate implant-based breast reconstruction compared to immediate autologous breast reconstruction. Breast Cancer 27(3):435–444
Hart SE, Brown DL, Kim HM et al (2021) Association of clinical complications of chemotherapy and patient-reported outcomes after immediate breast reconstruction. JAMA Surg 156(9):847–855
Yoon AP, Qi J, Brown DL et al (2018) Outcomes of immediate versus delayed breast reconstruction: results of a multicenter prospective study. Breast 37:72–79
Dempsey K, Mathieu E, Brennan M et al (2022) The role of breast reconstruction choice on body image patient-reported outcomes at four years post-mastectomy for breast cancer: a longitudinal prospective cohort study. Psychooncology 31(1):54–61
Ochoa O, Garza R, 3rd, Pisano S et al (2022) Prospective longitudinal patient-reported satisfaction and health-related quality of life following DIEP flap breast reconstruction: effects of reconstruction timing. Plast Reconstr Surg 149(5):848e–857e
Kuykendall LV, Tugertimur B, Agoris C et al (2017) Unilateral versus bilateral breast reconstruction: is less really more? Ann Plast Surg 78(6S Suppl 5):S275–S278
Taylor EM, Wilkins EG, Pusic AL et al (2019) Impact of unilateral versus bilateral breast reconstruction on procedure choices and outcomes. Plast Reconstr Surg 143(6):1159e–1168e
Allen RJ Jr, Sobti N, Patel AR et al (2020) Laterality and patient-reported outcomes following autologous breast reconstruction with free abdominal tissue: an 8-year examination of BREAST-Q data. Plast Reconstr Surg 146(5):964–975
McFadden EM, Lopez-Obregon B, Stone JP et al (2018) Direct-to-implant breast reconstruction with autoderm. Plast Reconstr Surg Glob Open 6(12):e2027
Cogliandro A, Salzillo R, Barone M et al (2022) Direct-to-implant breast reconstruction after unilateral and bilateral mastectomy: cross-sectional study of patient satisfaction and quality of life with BREAST-Q. Aesthetic Plast Surg 47:43–49
Momoh AO, Cohen WA, Kidwell KM et al (2017) Tradeoffs associated with contralateral prophylactic mastectomy in women choosing breast reconstruction: results of a prospective multicenter cohort. Ann Surg 266(1):158–164
Asaad M, Boukovalas S, Chu CK et al (2020) Financial toxicity and contralateral prophylactic mastectomy: an analysis using propensity score methods. Breast Cancer Res Treat 183(3):649–659
Kerrebijn I, Retrouvey H, Harma M et al (2021) Contralateral prophylactic mastectomy at the time of delayed microvascular breast reconstruction adversely affects patient-reported outcomes: a retrospective cohort study. J Plast Reconstr Aesthet Surg 74(4):785–791
Kazzazi F, Haggie R, Forouhi P et al (2018) A comparison of patient satisfaction (using the BREAST-Q questionnaire) with bilateral breast reconstruction following risk-reducing or therapeutic mastectomy. J Plast Reconstr Aesthet Surg 71(9):1324–1331
Bai L, Arver B, Johansson H et al (2019) Body image problems in women with and without breast cancer 6–20 years after bilateral risk-reducing surgery - a prospective follow-up study. Breast 44:120–127
Gandhi A, Duxbury P, Murphy J et al (2022) Patient reported outcome measures in a cohort of patients at high risk of breast cancer treated by bilateral risk reducing mastectomy and breast reconstruction. J Plast Reconstr Aesthet Surg 75(1):69–76
Herold N, Hellmich M, Lichtenheldt F et al (2022) Satisfaction and quality of life of healthy and unilateral diseased BRCA1/2 pathogenic variant carriers after risk-reducing mastectomy and reconstruction using the BREAST-Q questionnaire. Genes (Basel) 13(8):1357
Moberg IO, Schou Bredal I, Schneider MR et al (2018) Complications, risk factors, and patients-reported outcomes after skin-sparing mastectomy followed by breast reconstruction in women with BRCA mutations. J Plast Surg Hand Surg 52(4):234–239
Berlin NL, Tandon VJ, Qi J et al (2019) Hospital variations in clinical complications and patient-reported outcomes at 2 years after immediate breast reconstruction. Ann Surg 269(5):959–965
Hsu JJ, Kubiak CA, Billig JI et al (2021) Perceived versus patient-reported significance of surgeon gender in breast reconstruction. Plast Reconstr Surg 148(4):720–728
Kamel GN, Mehta K, Nash D et al (2019) Patient-reported satisfaction and quality of life in obese patients: a comparison between microsurgical and prosthetic implant recipients. Plast Reconstr Surg 144(6):960e–966e
Klement KA, Hijjawi JB, LoGiudice JA et al (2019) Microsurgical breast reconstruction in the obese: a better option than tissue expander/implant reconstruction? Plast Reconstr Surg 144(3):539–546
Ochoa O, Garza R, 3rd, Pisano S et al (2019) Prospective longitudinal patient-reported satisfaction and health-related quality of life following DIEP flap breast reconstruction: relationship with body mass index. Plast Reconstr Surg 143(6):1589–1600
Nelson JA, Sobti N, Patel A et al (2020) The impact of obesity on patient-reported outcomes following autologous breast reconstruction. Ann Surg Oncol 27(6):1877–1888
Srinivasa DR, Clemens MW, Qi J et al (2020) obesity and breast reconstruction: complications and patient-reported outcomes in a multicenter prospective study. Plast Reconstr Surg 145(3):481e–490e
Cheng MH, Koide S, Chen C et al (2021) Comparisons between normal body mass index and overweight patients who underwent unilateral microsurgical breast reconstructions. Ann Surg Oncol 28(1):353–362
Kuykendall LV, Zhang A, Tugertimur B et al (2018) Outcomes in deep inferior epigastric perforator flap and implant-based reconstruction: does age really matter? Cancer Control 25(1):1073274817744603
Oh DD, Flitcroft K, Brennan ME et al (2018) Patient-reported outcomes of breast reconstruction in older women: audit of a large metropolitan public/private practice in Sydney, Australia. Psychooncology 27(12):2815–2822
Dominici L, Hu J, Zheng Y et al (2021) Association of local therapy with quality-of-life outcomes in young women with breast cancer. JAMA Surg 156(10):e213758
Klifto KM, Bekheet FN, Manahan MA et al (2021) The effects of depression and anti-depressants on quality of life after breast reconstruction: a post-hoc analysis. Cureus 13(10):e18675
Mehta SK, Sheth AH, Olawoyin O et al (2020) Patients with psychiatric illness report worse patient-reported outcomes and receive lower rates of autologous breast reconstruction. Breast J 26(10):1931–1936
Shamsunder MG, Chu JJ, Polanco TO et al (2022) The impact of psychiatric diagnoses on patient-reported satisfaction and quality of life in post-mastectomy breast reconstruction. Ann Surg. https://doi.org/10.1097/SLA.0000000000005478
Berlin NL, Momoh AO, Qi J et al (2017) Racial and ethnic variations in one-year clinical and patient-reported outcomes following breast reconstruction. Am J Surg 214(2):312–317
Oskar S, Nelson JA, Hicks MEV et al (2022) The impact of race on perioperative and patient-reported outcomes following autologous breast reconstruction. Plast Reconstr Surg 149(1):15–27
Mehta SK, Olawoyin O, Chouairi F et al (2020) Worse overall health status negatively impacts satisfaction with breast reconstruction. J Plast Reconstr Aesthet Surg 73(11):2056–2062
Le NK, Gabrick KS, Chouairi F et al (2020) Impact of socioeconomic status on psychological functioning in survivorship following breast cancer and reconstruction. Breast J 26(9):1695–1701
Baker BG, Sewart E, Harvey J et al (2022) Implant-based reconstruction following mastectomy in patients who have had a previous breast augmentation: lessons from the national multicenter implant breast reconstruction evaluation study. Plast Reconstr Surg 149(2):324–337
Nelson JA, Polanco TO, Shamsunder MG et al (2021) Perioperative inpatient opioid consumption following autologous free-flap breast reconstruction patients: an examination of risk and patient-reported outcomes. Ann Surg Oncol 28(12):7823–7833
Coroneos CJ, Lin YL, Sidey-Gibbons C et al (2021) Correlation between financial toxicity, quality of life, and patient satisfaction in an insured population of breast cancer surgical patients: a single-institution retrospective study. J Am Coll Surg 232(3):253–263
Wu SS, Duraes EFR, Scomacao I et al (2022) Beauty is in the eye of the beholder: factors influencing disparity in perceptions of breast reconstruction aesthetic outcomes. Plast Reconstr Surg 150(1):42e–50e
Gil-Olarte P, Gil-Olarte MA, Gomez-Molinero R et al (2022) Psychosocial and sexual well-being in breast cancer survivors undergoing immediate breast reconstruction: The mediating role of breast satisfaction. Eur J Cancer Care (Engl) 31:e13686
Santanelli Di Pompeo F, Barone M, Salzillo R et al (2022) Predictive factors of satisfaction following breast reconstruction: do they influence patients? Aesthetic Plast Surg 46(2):610–618
Matthews H, Carroll N, Renshaw D et al (2017) Predictors of satisfaction and quality of life following post-mastectomy breast reconstruction. Psychooncology 26(11):1860–1865
Cereijo-Garea C, Pita-Fernandez S, Acea-Nebril B et al (2018) Predictive factors of satisfaction and quality of life after immediate breast reconstruction using the BREAST-Q((c)). J Clin Nurs 27(7–8):1464–1474
van de Grift TC, Mureau MAM, Negenborn VN et al (2020) Predictors of women’s sexual outcomes after implant-based breast reconstruction. Psychooncology 29(8):1272–1279
Stone JP, Bello RJ, Siotos C et al (2020) Patient-related risk factors for worsened abdominal well-being after autologous breast reconstruction. Plast Reconstr Surg 145(3):475e–480e
Shiraishi M, Sowa Y, Inafuku N (2022) Long-term survey of sexual well-being after breast reconstruction using the BREAST-Q in the Japanese population. Asian J Surg 46:150–155
Gallo L, Chu JJ, Shamsunder MG et al (2022) Best practices for BREAST-Q research: a systematic review of study methodology. Plast Reconstr Surg 150(3):526e–535e
Fontein DBY, Oros M, Held L et al (2022) Patient-reported outcomes in free-flap breast reconstructive surgery over time (PRO-BREST). Breast Care (Basel) 17(3):272–278
Saiga M, Taira N, Kimata Y et al (2017) Development of a Japanese version of the BREAST-Q and the traditional psychometric test of the mastectomy module for the assessment of HRQOL and patient satisfaction following breast surgery. Breast Cancer 24(2):288–298
Crittenden TA, Smallman A, Dean NR (2022) Normative data for the BREAST-Q Reconstruction module in an Australian population and comparison with US norms and breast reconstruction patient outcomes. J Plast Reconstr Aesthet Surg 75(7):2219–2228
Klifto KM, Aravind P, Major M et al (2020) Differences between breast cancer reconstruction and institutionally established normative data using the BREAST-Q reconstruction module: a comparative study. Plast Reconstr Surg 145(6):1371–1379
Mundy LR, Homa K, Klassen AF et al (2017) Breast cancer and reconstruction: normative data for interpreting the BREAST-Q. Plast Reconstr Surg 139(5):1046e–1055e
Li Y, Guo J, Sui Y et al (2022) Quality of life in patients with breast cancer following breast conservation surgery: a systematic review and meta-analysis. J Healthc Eng 2022:3877984
Berlin NL, Tandon VJ, Hawley ST et al (2019) Feasibility and efficacy of decision aids to improve decision making for postmastectomy breast reconstruction: a systematic review and meta-analysis. Med Decis Making 39(1):5–20
Pusic AL, Klassen AF, Snell L et al (2012) Measuring and managing patient expectations for breast reconstruction: impact on quality of life and patient satisfaction. Expert Rev Pharmacoecon Outcomes Res 12(2):149–158
Shamsunder MG, Polanco TO, McCarthy CM et al (2021) Understanding preoperative breast satisfaction among patients undergoing mastectomy and immediate reconstruction: BREAST-Q insights. Plast Reconstr Surg 148(6):891e–902e
Voineskos SH, Klassen AF, Cano SJ et al (2020) Giving meaning to differences in BREAST-Q scores: minimal important difference for breast reconstruction patients. Plast Reconstr Surg 145(1):11e–20e
Acknowledgements
This work was supported by JSPS KAKENHI Grant Number 22K16988 and the Okayama University Female Staff Support Grant. The authors would like to thank Enago (www.enago.jp) for the English language review.
Funding
Open access funding provided by Okayama University.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no potential conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
This article is published under an open access license. Please check the 'Copyright Information' section either on this page or in the PDF for details of this license and what re-use is permitted. If your intended use exceeds what is permitted by the license or if you are unable to locate the licence and re-use information, please contact the Rights and Permissions team.
About this article
Cite this article
Saiga, M., Nakagiri, R., Mukai, Y. et al. Trends and issues in clinical research on satisfaction and quality of life after mastectomy and breast reconstruction: a 5-year scoping review. Int J Clin Oncol 28, 847–859 (2023). https://doi.org/10.1007/s10147-023-02347-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-023-02347-5