Abstract
Background
Laparoscopic total extraperitoneal repair (TEP) of inguinal hernia has been associated with higher rates of recurrence compared to open methods. The aim of the present study was to determine independent risk factors for recurrence within 2 years after TEP.
Methods
This was a single-centre prospective cohort study with consecutive inclusion of patients undergoing inguinal hernia repair from 2010 to 2014. Systematic follow-up was conducted 6 months and 2 years postoperatively. Risk factors for recurrence after 2 years were analysed in univariate and multivariate analyses.
Results
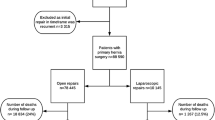
A total of 1194 patients underwent TEP for inguinal or femoral hernia in the study period, of which 1047 were eligible for analyses. After 2 years, 56 (5.3%) patients had presented with recurrence. The following factors were associated with recurrence in univariate analyses: body mass index (BMI) >30 (HR 3.64; p = 0.011), medial vs. lateral hernia (HR 2.37; p = 0.004), repair of recurrent hernia vs. primary repair (HR 2.12; p = 0.049), and length of stay >1 day (HR 1.77; p = 0.043). In multivariate analyses, factors independently associated with recurrence after 2 years were BMI >30 (HR 3.74; p = 0.026) and medial vs. lateral hernia (HR 2.39; p = 0.004).
Conclusion
The recurrence rate after TEP is higher than reported after open hernia repair. Attempts to decrease the rate should be persuaded. Good surgical technique with precise dissection and correct placement of the mesh, especially in medial hernias and obese patients, may be key points to improve outcomes after TEP.

Similar content being viewed by others
References
Scott NW, McCormack K, Graham P, Go PM, Ross SJ, Grant AM (2002) Open mesh versus non-mesh for repair of femoral and inguinal hernia. Cochrane Database Syst Rev (4): Cd002197. doi:10.1002/14651858.cd002197
Liem MS, van Duyn EB, van der Graaf Y, van Vroonhoven TJ (2003) Recurrences after conventional anterior and laparoscopic inguinal hernia repair: a randomized comparison. Ann Surg 237(1):136–141. doi:10.1097/01.sla.0000041049.69383.0e
van der Pool AE, Harlaar JJ, den Hoed PT, Weidema WF, van Veen RN (2010) Long-term follow-up evaluation of chronic pain after endoscopic total extraperitoneal repair of primary and recurrent inguinal hernia. Surg Endosc 24(7):1707–1711. doi:10.1007/s00464-009-0833-4
Bisgaard T, Bay-Nielsen M, Christensen IJ, Kehlet H (2007) Risk of recurrence 5 years or more after primary Lichtenstein mesh and sutured inguinal hernia repair. Br J Surg 94(8):1038–1040. doi:10.1002/bjs.5756
Bittner R, Montgomery MA, Arregui E, Bansal V, Bingener J, Bisgaard T, Buhck H, Dudai M, Ferzli GS, Fitzgibbons RJ, Fortelny RH, Grimes KL, Klinge U, Kockerling F, Kumar S, Kukleta J, Lomanto D, Misra MC, Morales-Conde S, Reinpold W, Rosenberg J, Singh K, Timoney M, Weyhe D, Chowbey P (2015) Update of guidelines on laparoscopic (TAPP) and endoscopic (TEP) treatment of inguinal hernia (International Endohernia Society). Surg Endosc 29(2):289–321. doi:10.1007/s00464-014-3917-8
McCormack K, Scott NW, Go PM, Ross S, Grant AM (2003) Laparoscopic techniques versus open techniques for inguinal hernia repair. Cochrane Database Syst Rev (1): Cd001785. doi:10.1002/14651858.cd001785
Eklund AS, Montgomery AK, Rasmussen IC, Sandbue RP, Bergkvist LA, Rudberg CR (2009) Low recurrence rate after laparoscopic (TEP) and open (Lichtenstein) inguinal hernia repair: a randomized, multicenter trial with 5-year follow-up. Ann Surg 249(1):33–38. doi:10.1097/SLA.0b013e31819255d0
Schmedt CG, Sauerland S, Bittner R (2005) Comparison of endoscopic procedures vs Lichtenstein and other open mesh techniques for inguinal hernia repair: a meta-analysis of randomized controlled trials. Surg Endosc 19(2):188–199. doi:10.1007/s00464-004-9126-0
Lamb AD, Robson AJ, Nixon SJ (2006) Recurrence after totally extraperitoneal laparoscopic repair: implications for operative technique and surgical training. Surg J R Coll Surg Edinb Irel 4(5):299–307
von Elm E, Altman DG, Egger M, Pocock SJ, Gotzsche PC, Vandenbroucke JP (2008) The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol 61(4):344–349. doi:10.1016/j.jclinepi.2007.11.008
Bhangu A, Singh P, Pinkney T, Blazeby JM (2015) A detailed analysis of outcome reporting from randomised controlled trials and meta-analyses of inguinal hernia repair. Hernia J Hernias Abdom Wall Surg 19(1):65–75. doi:10.1007/s10029-014-1299-4
Bobo Z, Nan W, Qin Q, Tao W, Jianguo L, Xianli H (2014) Meta-analysis of randomized controlled trials comparing Lichtenstein and totally extraperitoneal laparoscopic hernioplasty in treatment of inguinal hernias. J Surg Res 192(2):409–420. doi:10.1016/j.jss.2014.05.082
Burcharth J, Andresen K, Pommergaard HC, Bisgaard T, Rosenberg J (2014) Recurrence patterns of direct and indirect inguinal hernias in a nationwide population in Denmark. Surgery 155(1):173–177. doi:10.1016/j.surg.2013.06.006
Sajid, Ladwa N, Kalra L, Hutson K, Sains P, Baig MK (2012) A meta-analysis examining the use of tacker fixation versus no-fixation of mesh in laparoscopic inguinal hernia repair. Int J Surg (Lond Engl) 10(5):224–231. doi:10.1016/j.ijsu.2012.03.001
Garg P, Nair S, Shereef M, Thakur JD, Nain N, Menon GR, Ismail M (2011) Mesh fixation compared to nonfixation in total extraperitoneal inguinal hernia repair: a randomized controlled trial in a rural center in India. Surg Endosc 25(10):3300–3306. doi:10.1007/s00464-011-1708-z
Eker HH, Langeveld HR, Klitsie PJ, van’t Riet M, Stassen LP, Weidema WF, Steyerberg EW, Lange JF, Bonjer HJ, Jeekel J (2012) Randomized clinical trial of total extraperitoneal inguinal hernioplasty vs Lichtenstein repair: a long-term follow-up study. Arch Surg (Chicago, Ill: 1960) 147(3):256–260. doi:10.1001/archsurg.2011.2023
Miserez M, Peeters E, Aufenacker T, Bouillot JL, Campanelli G, Conze J, Fortelny R, Heikkinen T, Jorgensen LN, Kukleta J, Morales-Conde S, Nordin P, Schumpelick V, Smedberg S, Smietanski M, Weber G, Simons MP (2014) Update with level 1 studies of the European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia J Hernias Abdom Wall Surg 18(2):151–163. doi:10.1007/s10029-014-1236-6
Dulucq JL, Wintringer P, Mahajna A (2009) Laparoscopic totally extraperitoneal inguinal hernia repair: lessons learned from 3100 hernia repairs over 15 years. Surg Endosc 23(3):482–486. doi:10.1007/s00464-008-0118-3
Feliu-Pala X, Martin-Gomez M, Morales-Conde S, Fernandez-Sallent E (2001) The impact of the surgeon’s experience on the results of laparoscopic hernia repair. Surg Endosc 15(12):1467–1470. doi:10.1007/s00464-001-9017-6
Neumayer LA, Gawande AA, Wang J, Giobbie-Hurder A, Itani KM, Fitzgibbons RJ Jr, Reda D, Jonasson O (2005) Proficiency of surgeons in inguinal hernia repair: effect of experience and age. Ann Surg 242(3):344–348 (discussion 348–352)
Lau H, Patil NG, Yuen WK (2006) Day-case endoscopic totally extraperitoneal inguinal hernioplasty versus open Lichtenstein hernioplasty for unilateral primary inguinal hernia in males: a randomized trial. Surg Endosc 20(1):76–81. doi:10.1007/s00464-005-0203-9
Kingsnorth A, LeBlanc K (2003) Hernias: inguinal and incisional. Lancet 362(9395):1561–1571. doi:10.1016/s0140-6736(03)14746-0
Felix E, Scott S, Crafton B, Geis P, Duncan T, Sewell R, McKernan B (1998) Causes of recurrence after laparoscopic hernioplasty. A multicenter study. Surg Endosc 12(3):226–231
Wilkiemeyer M, Pappas TN, Giobbie-Hurder A, Itani KM, Jonasson O, Neumayer LA (2005) Does resident post graduate year influence the outcomes of inguinal hernia repair? Ann Surg 241(6):879–882 (discussion 882–874)
Vos PM, Simons MP, Luitse JS, van Geldere D, Koelemaij MJ, Obertop H (1998) Follow-up after inguinal hernia repair. Questionnaire compared with physical examination: a prospective study in 299 patients. Eur J Surg Acta Chirurgica 164(7):533–536. doi:10.1080/110241598750005903
Kald A, Nilsson E (1991) Quality assessment in hernia surgery. Quality Assur Health Care Off J Int Soc Qual Assur Health Care/ISQA 3(3):205–210
Haapaniemi S, Nilsson E (2002) Recurrence and pain 3 years after groin hernia repair. Validation of postal questionnaire and selective physical examination as a method of follow-up. Eur J Surg Acta Chirurgica 168(1):22–28. doi:10.1080/110241502317307535
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
LSI declares no conflict of interest. AR declares no conflict of interest. KWB declares no conflict of interest.
Ethical approval
The study was approved by the local research ethics committee (REC).
Human and animal rights
Compliance with ethical standards was adhered to through Institutional Review Board approval and the study including human participants have been performed in accordance with the ethical standards of the Declaration of Helsinki and its later amendments.
Informed consent
All patients were included after written informed consent.
Rights and permissions
About this article
Cite this article
Schjøth-Iversen, L., Refsum, A. & Brudvik, K.W. Factors associated with hernia recurrence after laparoscopic total extraperitoneal repair for inguinal hernia: a 2-year prospective cohort study. Hernia 21, 729–735 (2017). https://doi.org/10.1007/s10029-017-1634-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-017-1634-7