Abstract
Background
The study aimed to establish a link between blood ethylene oxide (EO) levels and periodontitis, given the growing concern about EO’s detrimental health effects.
Materials and methods
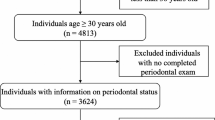
The study included 1006 adults from the 2013–2014 National Health and Nutrition Examination Survey (NHANES) dataset. We assessed periodontitis prevalence across groups, used weighted binary logistic regression and restricted cubic spline fitting for HbEO-periodontitis association, and employed Receiver Operating Characteristic (ROC) curves for prediction.
Results
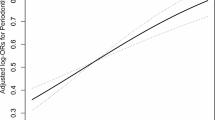
In the periodontitis group, HbEO levels were significantly higher (40.57 vs. 28.87 pmol/g Hb, P < 0.001). The highest HbEO quartile showed increased periodontitis risk (OR = 2.88, 95% CI: 1.31, 6.31, P = 0.01). A “J”-shaped nonlinear HbEO-periodontitis relationship existed (NL-P value = 0.0116), with an inflection point at ln-HbEO = 2.96 (EO = 19.30 pmol/g Hb). Beyond this, ln-HbEO correlated with higher periodontitis risk. A predictive model incorporating sex, age, education, poverty income ratio, alcohol consumption, and HbEO had 69.9% sensitivity and 69.2% specificity. The model achieved an area under the ROC curve of 0.761.
Conclusions
These findings suggest a correlation between HbEO levels and an increased susceptibility to periodontitis.




Similar content being viewed by others
Data availability
The NHANES dataset is publicly available online, accessible at cdc.gov/nchs/nhanes/index.htm.
References
Gimeno P et al (2018) Identification and quantification of ethylene oxide in sterilized medical devices using multiple headspace GC/MS measurement. J Pharm Biomed Anal 158:119–127
Agency for Toxic Substances and Disease Registry (ATSDR). Toxicological profile for ethylene oxide (draft for public comment). Atlanta, GA: U.S. Department of Health and Human Services, Public Health Service.]. https://wwwn.cdc.gov/TSP/ToxProfiles/ToxProfiles.aspx?id=734&tid=133
Kowalska A, Manning L (2022) Food Safety Governance and Guardianship: the role of the private Sector in addressing the EU Ethylene Oxide Incident. Foods 11(2)
Zekri N et al (2023) Physicochemical characterization and antioxidant properties of essential oils of M. pulegium (L.), M. suaveolens (Ehrh.) And M. Spicata (L.) from Moroccan Middle-Atlas. Foods 12(4)
Dias FN et al (2009) Sterilization of medical devices by ethylene oxide, determination of the dissipation of residues, and use of Green Fluorescent Protein as an indicator of process control. J Biomed Mater Res B Appl Biomater 91(2):626–630
Jones RR et al (2023) Ethylene oxide emissions and incident breast cancer and non-hodgkin lymphoma in a US cohort. J Natl Cancer Inst 115(4):405–412
Yu XY, Song P, Zou MH (2018) Obesity Paradox and Smoking Gun: a mystery of statistical Confounding? Circ Res 122(12):1642–1644
Rubinstein ML et al (2018) Adolescent exposure to toxic volatile Organic Chemicals from E-Cigarettes. Pediatrics 141(4)
Jain RB (2020) Associations between observed concentrations of ethylene oxide in whole blood and smoking, exposure to environmental tobacco smoke, and cancers including breast cancer: data for US children, adolescents, and adults. Environ Sci Pollut Res Int 27(17):20912–20919
Bono R et al (1999) Formation of N-(2-hydroxyethyl)valine due to exposure to ethylene oxide via tobacco smoke: a risk factor for onset of cancer. Environ Res 81(1):62–71
Kirman CR et al (2021) Ethylene oxide review: characterization of total exposure via endogenous and exogenous pathways and their implications to risk assessment and risk management. J Toxicol Environ Health B Crit Rev 24(1):1–29
Törnqvist M et al (1989) Unsaturated lipids and intestinal bacteria as sources of endogenous production of ethene and ethylene oxide. Carcinogenesis 10(1):39–41
Sheehan PJ et al (2021) Ethylene Oxide exposure in U.S. populations residing Near sterilization and other Industrial facilities: Context based on endogenous and total Equivalent Concentration exposures. Int J Environ Res Public Health 18(2)
Thier R, Bolt HM (2000) Carcinogenicity and genotoxicity of ethylene oxide: new aspects and recent advances. Crit Rev Toxicol 30(5):595–608
Jinot J et al (2018) Carcinogenicity of ethylene oxide: key findings and scientific issues. Toxicol Mech Methods 28(5):386–396
Ghosh M, Godderis L (2016) Genotoxicity of ethylene oxide: A review of micronucleus assay results in human population. Mutat Res Rev Mutat Res 770(Pt A):84–91
Ogawa M et al (2006) Hemoglobin adducts as a marker of exposure to chemical substances, especially PRTR class I designated chemical substances. J Occup Health 48(5):314–328
Cheang I et al (2022) Inverse association between blood ethylene oxide levels and obesity in the general population: NHANES 2013–2016. Front Endocrinol (Lausanne) 13:926971
Lynch DW et al (1984) Carcinogenic and toxicologic effects of inhaled ethylene oxide and propylene oxide in F344 rats. Toxicol Appl Pharmacol 76(1):69–84
Lundin A, Panas I, Ahlberg E (2007) A mechanistic investigation of ethylene oxide hydrolysis to ethanediol. J Phys Chem A 111(37):9087–9092
Steenland K et al (1991) Mortality among workers exposed to ethylene oxide. N Engl J Med 324(20):1402–1407
Han L, Wang Q (2023) Association between hemoglobin adducts of ethylene oxide levels and the risk of short sleep duration in the general population: an analysis based on the National Health and Nutrition Examination Survey. Environ Sci Pollut Res Int 30(31):76761–76768
Estrin WJ et al (1987) Evidence of neurologic dysfunction related to long-term ethylene oxide exposure. Arch Neurol 44(12):1283–1286
Csanády GA et al (2000) A physiological toxicokinetic model for exogenous and endogenous ethylene and ethylene oxide in rat, mouse, and human: formation of 2-hydroxyethyl adducts with hemoglobin and DNA. Toxicol Appl Pharmacol 165(1):1–26
Zhu X et al (2022) Blood ethylene oxide, systemic inflammation, and serum lipid profiles: results from NHANES 2013–2016. Chemosphere 299:134336
Wu N., et al (2022) Association between blood ethylene oxide levels and the prevalence of hypertension. Environ Sci Pollut Res Int 29(51):76937–76943.
Huang Q et al (2023) Association between ethylene oxide exposure and prevalence of COPD: evidence from NHANES 2013–2016. Sci Total Environ 885:163871
Kassebaum NJ et al (2017) Global, Regional, and National Prevalence, incidence, and disability-adjusted life years for oral conditions for 195 countries, 1990–2015: a systematic analysis for the Global Burden of Diseases, injuries, and risk factors. J Dent Res 96(4):380–387
Akinkugbe AA et al (2016) Systematic Review and Meta-analysis of the Association between Exposure to Environmental Tobacco Smoke and Periodontitis endpoints among nonsmokers. Nicotine Tob Res 18(11):2047–2056
(2018) Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet 392(10159):1789–1858
Ren ZH et al (2020) Global and regional burdens of oral cancer from 1990 to 2017: results from the global burden of disease study. Cancer Commun (Lond) 40(2–3):81–92
Beukers NG et al (2017) Periodontitis is an independent risk indicator for atherosclerotic cardiovascular diseases among 60 174 participants in a large dental school in the Netherlands. J Epidemiol Community Health 71(1):37–42
Huang K et al (2023) The modification of meteorological factors on the relationship between air pollution and periodontal diseases: an exploration based on different interaction strategies. Environ Geochem Health
Schaefer AS et al (2013) Validation of reported genetic risk factors for periodontitis in a large-scale replication study. J Clin Periodontol 40(6):563–572
Han DH et al Mercury exposure and Periodontitis among a Korean Population: the Shiw ha-Banwol Environmental Health Study. J Periodontol 80(12):1928–1936
Cátala-Valentín AR et al (2022) E-Cigarette aerosols promote oral S. Aureus colonization by delaying an Immune Response and Bacterial Clearing. Cells 11(5)
Yang M et al (2018) High-throughput, simultaneous quantitation of hemoglobin adducts of acrylamide, glycidamide, and ethylene oxide using UHPLC-MS/MS. J Chromatogr B Analyt Technol Biomed Life Sci 1086:197–205
Eke PI et al (2012) Update of the case definitions for population-based surveillance of periodontitis. J Periodontol 83(12):1449–1454
Curry SJ et al (2018) Behavioral weight loss interventions to prevent obesity-related morbidity and mortality in adults: US Preventive Services Task Force Recommendation Statement. JAMA 320(11):1163–1171
SSY AL et al (2019) Association between time since quitting smoking and periodontitis in former smokers in the National Health and Nutrition Examination Surveys (NHANES) 2009 to 2012. J Periodontol 90(1):16–25
Cepeda MS et al Association of flossing/inter-dental cleaning and periodontitis in adu lts. J Clin Periodontol 44(9):866–871
Chan MY et al (2014) Relationship between body mass index and fracture risk is mediated by bone mineral density. J Bone Min Res 29(11):2327–2335
Montero E et al (2019) Development and validation of a predictive model for periodontitis using NHANES 2011–2012 data. J Clin Periodontol 46(4):420–429
Zaorsky NG et al (2022) Pan-cancer analysis of prognostic metastatic phenotypes. Int J Cancer 150(1):132–141
Çetin MB et al (2022) The relationship between body mass index and stage/grade of periodontitis: a retrospective study. Clin Oral Investig 26(2):1937–1945
Eke PI et al (2018) Periodontitis in US adults: National Health and Nutrition Examination Survey 2009–2014. J Am Dent Assoc 149(7):576–588e6
Saxlin T et al (2010) Overweight and obesity weakly predict the development of periodontal infection. J Clin Periodontol 37(12):1059–1067
Khan S et al (2020) Obesity and periodontitis in Australian adults: a population-based cross-sectional study. Int Dent J 70(1):53–61
Li XY et al (2022) The association of healthy eating index with periodontitis in NHANES 2013–2014. Front Nutr 9:968073
Gay IC, Tran DT, Paquette DW (2018) Alcohol intake and periodontitis in adults aged ≥ 30 years: NHANES 2009–2012. J Periodontol 89(6):625–634
Yan Y et al (2022) Periodontitis is Associated with Heart failure: a Population-based study (NHANES III). Front Physiol 13:854606
Törnqvist M et al (2002) Protein adducts: quantitative and qualitative aspects of their formation, analysis and applications. J Chromatogr B Analyt Technol Biomed Life Sci 778(1–2):279–308
Bitencourt FV et al (2023) The role of Dyslipidemia in Periodontitis. Nutrients 15(2)
Moayed M, Mahdavian L (2017) Recycling Monoethylene Glycol (MEG) from the recirculating Waste of an Ethylene Oxide Unit. Open Chem 15(1):167–174
Almerich-Silla JM et al (2015) Oxidative stress parameters in Saliva and its Association with Periodontal Disease and types of Bacteria. Dis Markers 2015:653537
Chang H et al (2023) In vivo toxicity evaluation of tumor targeted glycol chitosan nanoparticles in healthy mice: repeated high-dose of glycol chitosan nanoparticles potentially induce cardiotoxicity. J Nanobiotechnol 21(1):82
da Cunha Mendes GC, da Silva Brandão TR, Miranda Silva CL (2008) Ethylene oxide potential toxicity. Expert Rev Med Devices 5(3):323–328
Zeng G et al (2021) Association between blood ethylene oxide levels and the risk of cardiovascular diseases in the general population. Environ Sci Pollut Res Int 28(45):64921–64928
Li Z et al (2023) The association between ethylene oxide exposure and asthma risk: a population-based study. Environ Sci Pollut Res Int 30(9):24154–24167
Taboza ZA et al (2018) Periodontitis, edentulism and glycemic control in patients with type 2 diabetes: a cross-sectional study. BMJ Open Diabetes Res Care 6(1):e000453
Priyamvara A et al (2020) Periodontal inflammation and the risk of Cardiovascular Disease. Curr Atheroscler Rep 22(7):28
Lertpimonchai A et al (2019) Periodontitis as the risk factor of chronic kidney disease: mediation analysis. J Clin Periodontol 46(6):631–639
(2008) American Academy of Periodontology statement on risk assessment. J Periodontol 79(2):202
Acknowledgements
The authors extend their gratitude to Zhang Jing from Shanghai Tongren Hospital for his substantial contributions to the development of the nhanesR package and webpage. Additionally, the authors express their appreciation to the NHANES databases for granting access to the data.
Funding
This work was funded by the Science and Technology Planning Project of Sichuan Province (2021YJ0170), the Project of Chengdu Science and Technology Bureau (2019-YF05-00498-SN), National Natural Science Foundation of China (82370884), Sichuan Province science and technology plan project (2021YFS0101), National Natural Science Foundation of China (82104069), and Sichuan Science and Technology Program (2022089).
Author information
Authors and Affiliations
Contributions
XY drafted the manuscript and conducted statistical analysis. TYJ, RZY, and Li Linke conducted statistical analysis and contributed to the writing of the methods section. LYJ and XJ were responsible for guiding and reviewing this article. All authors have read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
All the data used in our study were obtained from the National Health and Nutrition Examination Survey (NHANES). NHANES is a nationally representative cross-sectional study conducted under the direction of the National Center for Health Statistics (NCHS) to assess the health and nutrition status of the non-institutionalized population of the United States using a complex, multistage, and probabilistic sampling design. All of the surveys were authorized by the NCHS Ethics Review Board before being conducted, and all participants signed informed consent forms. More information is available at http://www.cdc.gov/nchs/nhanes/.
Consent for publication
Not applicable.
Competing of interests
None of the authors have any potential conflicts of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Xue, Y., Tang, Y., Ren, Z. et al. Association between blood ethylene oxide levels and the prevalence of periodontitis: evidence from NHANES 2013–2014. Clin Oral Invest 28, 293 (2024). https://doi.org/10.1007/s00784-024-05690-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00784-024-05690-7