Abstract
Objectives
To update the findings of a systematic review from the year 2016 on the evidence for the accuracy and potential benefits of cone beam computed tomography (CBCT) in periodontal diagnostics.
Material and methods
A systematic literature search was performed and the criteria for PICO, PRISMA and risk of bias assessment were applied. Only clinical trials (> 10 patients) conducted in humans on periodontal bone loss, i.e. vertical and/or horizontal or furcation involvement, in CBCT compared with clinical and/or conventional radiographic measures were included.
Results
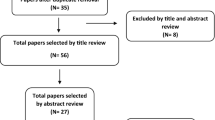
From 1152 articles identified, 11 case series on furcations and eight on vertical and/or horizontal bone loss were included. The studies showed moderate risk of bias and heterogeneous study designs. The agreement between non-surgical clinical or two-dimensional radiographic assessments of horizontal, vertical or interfurcal bone loss and CBCT measurements was analysed in 11 studies and was low in six studies with comparable study designs. A high accuracy (80–84%) of CBCT measurements compared with intra-surgical findings of furcation involvement was observed in four studies. Comparing CBCT with intra-surgical measurements of vertical or horizontal bone loss, an accuracy between 58 and 93% was found in four out of six studies. Three studies were analysed and indicated benefits of CBCT in decision making and/or a reduction of treatment costs and time in teeth of interest.
Conclusions
The findings provide additional evidence for the accuracy of CBCT in assessing periodontal bone loss.
Clinical relevance
CBCT is an accurate diagnostic tool in periodontology, which needs to be carefully considered in certain situations.

Similar content being viewed by others
References
Walter C, Schmidt JC, Dula K, Sculean A (2016) Cone beam computed tomography (CBCT) for diagnosis and treatment planning in periodontology: a systematic review. Quintessence Int 47:25–37. https://doi.org/10.3290/j.qi.a34724
Walter C, Kaner D, Berndt DC, Weiger R, Zitzmann NU (2009) Three-dimensional imaging as a pre-operative tool in decision making for furcation surgery. J Clin Periodontol 36:250–257. https://doi.org/10.1111/j.1600-051X.2008.01367.x
Walter C, Weiger R, Dietrich T, Lang NP, Zitzmann NU (2012) Does three-dimensional imaging offer a financial benefit for treating maxillary molars with furcation involvement? A pilot clinical case series. Clin Oral Implants Res 23:351–358. https://doi.org/10.1111/j.1600-0501.2011.02330.x
https://www.ncbi.nlm.nih.gov/pubmed/ Accessed 24 January 2020
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, Shekelle P, Stewart LA, Group P-P (2015) Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev 4:1. https://doi.org/10.1186/2046-4053-4-1
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6:e1000097. https://doi.org/10.1371/journal.pmed.1000097
Cumpston M, Chandler J (2019) Chapter IV: updating a review. In: Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ, Welch VA (editors). Cochrane handbook for systematic reviews of interventions version 6.0 (updated August 2019). Cochrane
Garner P, Hopewell S, Chandler J, MacLehose H, Akl EA, Beyene J, Chang S, Churchill R, Dearness K, Guyatt G, Lefebvre C, Liles B, Marshall R, Martínez García L, Mavergames C, Nasser M, Qaseem A, Sampson M, Soares-Weiser K, Takwoingi Y, Thabane L, Trivella M, Tugwell P, Welsh E, Wilson EC, Schünemann HJ (2016) When and how to update systematic review: consensus and checklist. BMJ 35:i3507
Miller SA, Forrest JL (2001) Enhancing your practice through evidence-based decision making: PICO, learning how to ask good questions. J Evid Based Dent Pract 1:136–141
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33:159–174
Moga C, Guo B, Schopflocher D, Harstall C (2012) Development of a quality appraisal tool for case series studies using a modified Delphi technique. http://www.ihe.ca/documents/Case%20series%20studies%20using%20a%20modified%20Delphi%20technique.pdf (accessed in august, 2019)
Walter C, Weiger R, Zitzmann NU (2010) Accuracy of three-dimensional imaging in assessing maxillary molar furcation involvement. J Clin Periodontol 37:436–441. https://doi.org/10.1111/j.1600-051X.2010.01556.x
Darby I, Sanelli M, Shan S, Silver J, Singh A, Soedjono M, Ngo L (2014) Comparison of clinical and cone beam computed tomography measurements to diagnose furcation involvement. Int J Dent Hyg 13:241–245. https://doi.org/10.1111/idh.12116
Marinescu AG, Boariu M, Rusu D, Stratul SI, Ogodescu A (2014) Reliability of CBCT as an assessment tool for mandibular molars furcation defects. Proc SPIE 8925, Fifth International Conference on Lasers in Medicine: Biotechnologies Integrated in Daily Medicine, 89250J (14 January 2014); https://doi.org/10.1117/122045782
Qiao J, Wang S, Duan J, Zhang Y, Qiu Y, Sun C, Liu D (2014) The accuracy of cone-beam computed tomography in assessing maxillary molar furcation involvement. J Clin Periodontol 41:269–274. https://doi.org/10.1111/jcpe.12150
Cimbaljevic MM, Spin-Neto RR, Miletic VJ, Jankovic SM, Aleksic Z, Nikolic-Jakoba NS (2015) Clinical and CBCT-based diagnosis of furcation involvement in patients with severe periodontitis. Quintessence Int 46:863–870. https://doi.org/10.3290/j.qi.a34702
Pajnigara N, Kolte A, Kolte R, Pajnigara N, Lathiya V (2016) Diagnostic accuracy of cone beam computed tomography in identification and postoperative evaluation of furcation defects. J Indian Soc Periodontol 20:386–390. https://doi.org/10.4103/0972-124X.192307
Zhu J, Ouyang XY (2016) Assessing maxillary molar furcation involvement by cone beam computed tomography. Chin J Dent Res 19:145–151. https://doi.org/10.3290/j.cjdr.a36679
Padmanabhan S, Dommy A, Guru SR, Joseph A (2017) Comparative evaluation of cone-beam computed tomography versus direct surgical measurements in the diagnosis of mandibular molar furcation involvement. Contemp Clin Dent 8:439–445. https://doi.org/10.4103/ccd.ccd_515_17
Zhang W, Foss K, Wang BY (2018) A retrospective study on molar furcation assessment via clinical detection, intraoral radiography and cone beam computed tomography. BMC Oral Health 18:75. https://doi.org/10.1186/s12903-018-0544-0
Grimard BA, Hoidal MJ, Mills MP, Mellonig JT, Nummikoski PV, Mealey BL (2009) Comparison of clinical, periapical radiograph, and cone-beam volume tomography measurement techniques for assessing bone level changes following regenerative periodontal therapy. J Periodontol 80:48–55. https://doi.org/10.1902/jop.2009.080289
de Faria Vasconcelos K, Evangelista KM, Rodrigues CD, Estrela C, de Sousa TO, Silva MA (2012) Detection of periodontal bone loss using cone beam CT and intraoral radiography. Dentomaxillofac Radiol 41:64–69. https://doi.org/10.1259/dmfr/13676777
Haghgoo JM, Shokri A, Khodadoustan A, Khoshhal M, Rabienejad N, Farhadian M (2014) Comparison the accuracy of the cone-beam computed tomography with digital direct intraoral radiography, in assessment of periodontal osseous lesions. Avicenna J Dent Res 6:e21952
Banodkar AB, Gaikwad RP, Gunjikar TU, Lobo TA (2015) Evaluation of accuracy of cone beam computed tomography for measurement of periodontal defects: a clinical study. J Indian Soc Periodontol 19:285–289. https://doi.org/10.4103/0972-124X.154176
Goodarzi Pour D, Romoozi E, Soleimani Shayesteh Y (2015) Accuracy of cone beam computed tomography for detection of bone loss. J Dent (Tehran) 12:513–523
Suphanantachat S, Tantikul K, Tamsailom S, Kosalagood P, Nisapakultorn K, Tavedhikul K (2017) Comparison of clinical values between cone beam computed tomography and conventional intraoral radiography in periodontal and infrabony defect assessment. Dentomaxillofac Radiol 46:20160461. https://doi.org/10.1259/dmfr.20160461
Yang J, Li X, Duan D, Bai L, Zhao L, Xu Y (2019) Cone-beam computed tomography performance in measuring periodontal bone loss. J Oral Sci 61:61–66. https://doi.org/10.2334/josnusd.17-0332
Li F, Jia PY, Ouyang XY (2015) Comparison of measurements on cone beam computed tomography for periodontal intrabony defect with intra-surgical measurements. Chin J Dent Res 18:171–176
Dula K, Benic G, Bornstein M, Walter C, Dagassan-Berndt D, Filippi A, Hicklin S, Jeger F, Luebbers H-T, Sculean A, Sequeira-Byron P, Zehnder M (2015) SADMFR guidelines for the use of cone-beam computed tomography / digital volume tomography. A consensus workshop organized by the Swiss Association of Dentomaxillofacial Radiology. Part II: Endodontics, Periodontology, Reconstructive Dentistry, pediatric dentistry. Swiss Dent J 125:945–953
Farman AG (2005) ALARA still applies. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 100:395–397. https://doi.org/10.1016/j.tripleo.2005.05.055
Sowby FD (1978) International Commission on Radiological Protection: 1978 Stockholm meeting. Radiology 129:533–535. https://doi.org/10.1148/129.2.533
Yusof NA, Noor E, Yusof MY (2020) The accuracy of linear measurements in cone beam computed tomography for assessing intrabony and furcation defects: a systematic review and meta-analysis. J Oral Res 8:527–539. https://doi.org/10.17126/joralres.2019.077
Herrera D, Matesanz P, Martin C, Oud V, Feres M, Teughels W (2020) Adjunctive effect of locally delivered antimicrobials in periodontitis therapy. A systematic review and meta-analysis. J Clin Periodontol. https://doi.org/10.1111/JCPE.13230
Schmidt JC, Sahrmann P, Weiger R, Schmidlin PR, Walter C (2013) Biologic width dimensions – a systematic review. J Clin Periodontol 40:493–504. https://doi.org/10.1111/jcpe.12078
Schmidt JC, Walter C, Amato M, Weiger R (2014) Treatment of periodontal-endodontic lesions – a systematic review. J Clin Periodontol 41:779–790. https://doi.org/10.1111/jcpe.12265
Salvi GE, Stähli A, Schmidt JC, Ramseier CA, Sculean A, Walter C (2020) Adjunctive laser or antimicrobial photodynamic therapy to non-surgical mechanical instrumentation in patients with untreated periodontitis. A systematic review and meta-analysis. J Clin Periodontol. https://doi.org/10.1111/jcpe.13236
Eggmann F, Connert T, Bühler J, Dagassan-Berndt D, Weiger R, Walter C (2017) Do periapical and periodontal pathologies affect Schneiderian membrane appearance? Systematic review of studies using cone-beam computed tomography. Clin Oral Investig 21:1611–1630. https://doi.org/10.1007/s00784-016-1944-7
Buset SL, Zitzmann NU, Weiger R, Walter C (2015) Non-surgical periodontal therapy supplemented with systemically administered azithromycin: a systematic review of RCTs. Clin Oral Investig 19:1763–1775. https://doi.org/10.1007/s00784-015-1499-z
Buset SL, Walter C, Friedmann A, Weiger R, Borgnakke WS, Zitzmann NU (2016) Are periodontal diseases really silent? A systematic review of their effect on quality of life. J Clin Periodontol 43:333–344. https://doi.org/10.1111/jcpe.12517
Schulze R, Heil U, Gross D, Bruellmann DD, Dranischnikow E, Schwanecke U, Schoemer E (2011) Artefacts in CBCT: a review. Dentomaxillofac Radiol 40:265–273. https://doi.org/10.1259/dmfr/30642039
Pauwels R, Faruangsaeng T, Charoenkarn T, Ngonphloy N, Panmekiate S (2015) Effect of exposure parameters and voxel size on bone structure analysis in CBCT. Dentomaxillofac Radiol 44:20150078. https://doi.org/10.1259/dmfr.20150078
Stovold E, Beecher D, Foxlee R, Noel-Storr A (2014) Study flow diagrams in Cochrane systematic review updates: an adapted PRISMA flow diagram. Syst Rev 3:54. https://doi.org/10.1186/2046-4053-3-54
Hamp SE, Nyman S, Lindhe J (1975) Periodontal treatment of multirooted teeth. Results after 5 years. J Clin Periodontol 2:126–135. https://doi.org/10.1111/j.1600-051x1975.tb01734.x
Funding
The study was self-funded by the authors and their institutions.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Online Resource 1
PRISMA checklist. (DOC 65 kb)
Online Resource 2
Electronic search strategy for the databases PubMed, Scopus and The Cochrane Library. (DOCX 15 kb)
Online Resource 3
Studies excluded based on full-text analysis, and reasons for exclusion. (DOCX 16 kb)
Online Resource 4
Criteria for assessing the methodological and reporting quality of case series studies according to Moga et al. [11]. (DOCX 16 kb)
Online Resource 5
Quality assessment of included studies on accuracy of CBCT in FI (a) and in detecting vertical and horizontal bone loss (b) according to Moga et al. [11]. (DOCX 31 kb)
Rights and permissions
About this article
Cite this article
Walter, C., Schmidt, J.C., Rinne, C.A. et al. Cone beam computed tomography (CBCT) for diagnosis and treatment planning in periodontology: systematic review update. Clin Oral Invest 24, 2943–2958 (2020). https://doi.org/10.1007/s00784-020-03326-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-020-03326-0