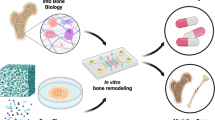
Abstract
Diabetes mellitus (DM) is related to impaired bone healing and an increased risk of bone fractures. While it is recognized that osteogenic differentiation and the function of osteoblasts are suppressed in DM, the influence of DM on osteoclasts is still unclear. Hyperglycemia and inflammatory environment are the hallmark of DM that causes dysregulation of various pro-inflammatory cytokines and alternated gene expression in periodontal ligament cells, osteoblasts, osteocytes, osteoclasts, and osteoclast precursors. A methodological review on conceptual and practical implications of in vitro study models is used for DM simulation on bone cells. Several major databases were screened to find literature related to the study objective. Published literature within last 20 years that used in vitro DM-simulated models to study how DM affects the cellular behavior of bone cells were selected for this review. Studies utilizing high glucose and serum acquired from diabetic animals are the mainly used methods to simulate the diabetic condition. The combination with various simulating factors such as lipopolysaccharide (LPS), hydrogen peroxide (H2O2), and advanced glycation end products (AGEs) have been reported in diabetic situations in vitro, as well. Through screening procedure, it was evident DM-simulated conditions exerted negative impact on bone-related cells. However, inconsistent results were found among different reported studies, which could be due to variation in culture conditions, concentrations of the stimulating factors and cell lineage, etc. This manuscript has concisely reviewed currently existing DM-simulated in vitro models and provides valuable insights of detailed components in simulating DM conditions in vitro. Studies using DM-simulated microenvironment revealed that in vitro simulation negatively impacted periodontal ligament cells, osteoblasts, osteocytes, osteoclasts, and osteoclast precursors. Contrarily, studies also indicated beneficial influence on bone-related cells when such conditions are reversed.

Similar content being viewed by others
References
Lontchi-Yimagou E, Sobngwi E, Matsha TE, Kengne AP (2013) Diabetes mellitus and inflammation. Curr Diab Rep 13:435–444
Jiao H, Xiao E, Graves DT (2015) Diabetes and its effect on bone and fracture healing. Curr Osteoporos Rep 13:327–335
Wild S, Roglic G, Green A, Sicree R, King H (2004) Global prevalence of diabetes: estimates for the year 2000 and projections for 2030. Diabetes Care 27:1047–1053
Kim JY, Lee SK, Jo KJ, Song DY, Lim DM, Park KY, Bonewald LF, Kim BJ (2013) Exendin-4 increases bone mineral density in type 2 diabetic OLETF rats potentially through the down-regulation of SOST/sclerostin in osteocytes. Life Sci 92:533–540
Hu Z, Ma C, Liang Y, Zou S, Liu X (2019) Osteoclasts in bone regeneration under type 2 diabetes mellitus. Acta Biomater 84:402–413
Loder RT (1988) The influence of diabetes mellitus on the healing of closed fractures. Clin Orthop Relat Res 210–216
Hu Z, Ma C, Rong X, Zou S, Liu X (2018) Immunomodulatory ECM-like microspheres for accelerated bone regeneration in diabetes mellitus. ACS Appl Mater Interfaces 10:2377–2390
Wu YY, Xiao E, Graves DT (2015) Diabetes mellitus related bone metabolism and periodontal disease. Int J Oral Sci 7:63–72
Chapple IL, Genco R, Working group 2 of joint EFPAAPw (2013) Diabetes and periodontal diseases: consensus report of the Joint EFP/AAP Workshop on Periodontitis and systemic diseases. J Clin Periodontol 40(Suppl 14):106–112
Lalla E, Papapanou PN (2011) Diabetes mellitus and periodontitis: a tale of two common interrelated diseases. Nat Rev Endocrinol 7:738–748
Furman BL (2015) Streptozotocin-induced diabetic models in mice and rats. Curr Protoc Pharmacol 70:1–20
Al-Awar A, Kupai K, Veszelka M, Szucs G, Attieh Z, Murlasits Z, Torok S, Posa A, Varga C (2016) Experimental diabetes mellitus in different animal models. J Diabetes Res 2016:9051426
Chatzigeorgiou A, Halapas A (2009) The use of animal models in the study of diabetes mellitus. In vivo (Athens, Greece) 23:245–258
Jin Z, Wei W, Yang M, Du Y, Wan Y (2014) Mitochondrial complex I activity suppresses inflammation and enhances bone resorption by shifting macrophage-osteoclast polarization. Cell Metab 20:483–498
Kalaitzoglou E, Popescu I, Bunn RC, Fowlkes JL, Thrailkill KM (2016) Effects of type 1 diabetes on osteoblasts, osteocytes, and osteoclasts. Curr Osteoporos Rep 14:310–319
Rathinavelu S, Guidry-Elizondo C, Banu J (2018) Molecular modulation of osteoblasts and osteoclasts in type 2 diabetes. J Diabetes Res 2018:6354787
Garcia-Hernandez A, Arzate H, Gil-Chavarria I, Rojo R, Moreno-Fierros L (2012) High glucose concentrations alter the biomineralization process in human osteoblastic cells. Bone 50:276–288
Dong K, Hao P, Xu S, Liu S, Zhou W, Yue X, Rausch-Fan X, Liu Z (2017) Alpha-lipoic acid alleviates high-glucose suppressed osteogenic differentiation of MC3T3-E1 cells via antioxidant effect and PI3K/Akt signaling pathway. Cell Physiol Biochem 42:1897–1906
Wu M, Ai W, Chen L, Zhao S, Liu E (2016) Bradykinin receptors and EphB2/EphrinB2 pathway in response to high glucose-induced osteoblast dysfunction and hyperglycemia-induced bone deterioration in mice. Int J Mol Med 37:565–574
Kalyanaraman H, Schwaerzer G, Ramdani G, Castillo F, Scott BT, Dillmann W, Sah RL, Casteel DE, Pilz RB (2018) Protein kinase G activation reverses oxidative stress and restores osteoblast function and bone formation in male mice with type 1 diabetes. Diabetes 67:607–623
Xiong Y, Zhang Y, Guo Y, Yuan Y, Guo Q, Gong P, Wu Y (2017) 1alpha,25-dihydroxyvitamin D3 increases implant osseointegration in diabetic mice partly through FoxO1 inactivation in osteoblasts. Biochem Biophys Res Commun 494:626–633
Bartell SM, Kim HN, Ambrogini E, Han L, Iyer S, Serra Ucer S, Rabinovitch P, Jilka RL, Weinstein RS, Zhao H, O'Brien CA, Manolagas SC, Almeida M (2014) FoxO proteins restrain osteoclastogenesis and bone resorption by attenuating H2O2 accumulation. Nat Commun 5:3773
Liu C, Jiang D (2017) High glucose-induced LIF suppresses osteoblast differentiation via regulating STAT3/SOCS3 signaling. Cytokine 91:132–139
Pramojanee SN, Phimphilai M, Chattipakorn N, Chattipakorn SC (2014) Possible roles of insulin signaling in osteoblasts. Endocr Res 39:144–151
Akune T, Ogata N, Hoshi K, Kubota N, Terauchi Y, Tobe K, Takagi H, Azuma Y, Kadowaki T, Nakamura K, Kawaguchi H (2002) Insulin receptor substrate-2 maintains predominance of anabolic function over catabolic function of osteoblasts. J Cell Biol 159:147–156
Yang J, Zhang X, Wang W, Liu J (2010) Insulin stimulates osteoblast proliferation and differentiation through ERK and PI3K in MG-63 cells. Cell Biochem Funct 28:334–341
Ogata N, Chikazu D, Kubota N, Terauchi Y, Tobe K, Azuma Y, Ohta T, Kadowki T, Nakamura K, Kawaguchi H (2000) Insulin receptor substrate-1 in osteoblast is indispensable for maintaining bone turnover. J Clin Investig 105:935–943
Fulzele K, Riddle RC, DiGirolamo DJ, Cao X, Wan C, Chen D, Faugere MC, Aja S, Hussain MA, Bruning JC, Clemens TL (2010) Insulin receptor signaling in osteoblasts regulates postnatal bone acquisition and body composition. Cell 142:309–319
Pacicca DM, Brown T, Watkins D, Kover K, Yan Y, Prideaux M, Bonewald L (2019) Elevated glucose acts directly on osteocytes to increase sclerostin expression in diabetes. Sci Rep 9:17353
Sun T, Yan Z, Cai J, Shao X, Wang D, Ding Y, Feng Y, Yang J, Luo E, Feng X, Jing D (2019) Effects of mechanical vibration on cell morphology, proliferation, apoptosis, and cytokine expression/secretion in osteocyte-like MLO-Y4 cells exposed to high glucose. Cell Biol Int
Wittrant Y, Gorin Y, Woodruff K, Horn D, Abboud HE, Mohan S, Abboud-Werner SL (2008) High d(+)glucose concentration inhibits RANKL-induced osteoclastogenesis. Bone 42:1122–1130
Cai ZY, Yang B, Shi YX, Zhang WL, Liu F, Zhao W, Yang MW (2018) High glucose downregulates the effects of autophagy on osteoclastogenesis via the AMPK/mTOR/ULK1 pathway. Biochem Biophys Res Commun 503:428–435
Shen Y, Guo S, Chen G, Ding Y, Wu Y, Tian W (2018) Hyperglycemia Induces osteoclastogenesis and bone destruction through the activation of Ca(2+)/calmodulin-dependent protein kinase II. Calcif Tissue Int
Tanaka T, Takei Y, Yamanouchi D (2016) Hyperglycemia suppresses calcium phosphate–induced aneurysm formation through inhibition of macrophage activation. J Am Heart Assoc 5
Kurihara C, Tanaka T, Yamanouchi D (2017) Hyperglycemia attenuates receptor activator of NF-κB ligand-induced macrophage activation by suppressing insulin signaling. J Surg Res 214:168–175
Xiao E, Mattos M, Vieira GHA, Chen S, Correa JD, Wu Y, Albiero ML, Bittinger K, Graves DT (2017) Diabetes enhances IL-17 expression and alters the oral microbiome to increase its pathogenicity. Cell Host Microbe 22:e4
Kim HS, Park JW, Yeo SI, Choi BJ, Suh JY (2006) Effects of high glucose on cellular activity of periodontal ligament cells in vitro. Diabetes Res Clin Pract 74:41–47
Kato H, Taguchi Y, Tominaga K, Kimura D, Yamawaki I, Noguchi M, Yamauchi N, Tamura I, Tanaka A, Umeda M (2016) High glucose concentrations suppress the proliferation of human periodontal ligament stem cells and their differentiation into osteoblasts. J Periodontol 87:e44–51
Li M, Li CZ (2016) High glucose improves healing of periodontal wound by inhibiting proliferation and osteogenetic differentiation of human PDL cells. Int Wound J 13:39–43
Nishimura F, Naruishi K, Yamada H, Kono T, Takashiba S, Murayama Y (2000) High glucose suppresses cathepsin activity in periodontal-ligament-derived fibroblastic cells. J Dental Res 79:1614–1617
Lew JH, Naruishi K, Kajiura Y, Nishikawa Y, Ikuta T, Kido JI, Nagata T (2018) High glucose-mediated cytokine regulation in gingival fibroblasts and THP-1 macrophage: a possible mechanism of severe periodontitis with diabetes. Cell Physiol Biochem 50:973–986
Li X, Ma XY, Feng YF, Ma ZS, Wang J, Ma TC, Qi W, Lei W, Wang L (2015) Osseointegration of chitosan coated porous titanium alloy implant by reactive oxygen species-mediated activation of the PI3K/AKT pathway under diabetic conditions. Biomaterials 36:44–54
Jiang H, Ma X, Zhou W, Dong K, Rausch-Fan X, Liu S, Li S (2017) The effects of hierarchical micro/nano-structured titanium surface on osteoblast proliferation and differentiation under diabetic conditions. Implant Dent 26:263–269
Kwon H, Lim W, Kim J, Jeon S, Kim S, Karna S, Cha H, Kim O, Choi H (2013) Effect of 635 nm irradiation on high glucose-boosted inflammatory responses in LPS-induced MC3T3-E1 cells. Lasers Med Sci 28:717–724
Sun M, Yang J, Wang J, Hao T, Jiang D, Bao G, Liu G (2016) TNF-alpha is upregulated in T2DM patients with fracture and promotes the apoptosis of osteoblast cells in vitro in the presence of high glucose. Cytokine 80:35–42
Feng YF, Wang L, Zhang Y, Li X, Ma ZS, Zou JW, Lei W, Zhang ZY (2013) Effect of reactive oxygen species overproduction on osteogenesis of porous titanium implant in the present of diabetes mellitus. Biomaterials 34:2234–2243
Takagi M, Kasayama S, Yamamoto T, Motomura T, Hashimoto K, Yamamoto H, Sato B, Okada S, Kishimoto T (1997) Advanced glycation endproducts stimulate interleukin-6 production by human bone-derived cells. J Bone Miner Res 12:439–446
Miranda C, Giner M, Montoya MJ, Vazquez MA, Miranda MJ, Perez-Cano R (2016) Influence of high glucose and advanced glycation end-products (ages) levels in human osteoblast-like cells gene expression. BMC Musculoskelet Disord 17:377
Hu XF, Wang L, Lu YZ, Xiang G, Wu ZX, Yan YB, Zhang Y, Zhao X, Zang Y, Shi L, Lei W, Feng YF (2017) Adiponectin improves the osteointegration of titanium implant under diabetic conditions by reversing mitochondrial dysfunction via the AMPK pathway in vivo and in vitro. Acta Biomater 61:233–248
Tanaka K, Yamaguchi T, Kanazawa I, Sugimoto T (2015) Effects of high glucose and advanced glycation end products on the expressions of sclerostin and RANKL as well as apoptosis in osteocyte-like MLO-Y4-A2 cells. Biochem Biophys Res Commun 461:193–199
Tessaro FHG, Ayala TS, Nolasco EL, Bella LM, Martins JO (2017) Insulin influences LPS-induced TNF-alpha and IL-6 release through distinct pathways in mouse macrophages from different compartments. Cell Physiol Biochem 42:2093–2104
Zheng J, Chen S, Albiero ML, Vieira GHA, Wang J, Feng JQ, Graves DT (2018) Diabetes activates periodontal ligament fibroblasts via NF-κB in vivo. J Dental Res 97:580–588
Li DX, Deng TZ, Lv J, Ke J (2014) Advanced glycation end products (AGEs) and their receptor (RAGE) induce apoptosis of periodontal ligament fibroblasts. Braz J Med Biol Res 47:1036–1043
Li Z, Li C, Zhou Y, Chen W, Luo G, Zhang Z, Wang H, Zhang Y, Xu D, Sheng P (2016) Advanced glycation end products biphasically modulate bone resorption in osteoclast-like cells. Am J Physiol Endocrinol Metab 310:E355–E366
Wang L, Hu X, Ma X, Ma Z, Zhang Y, Lu Y, Li X, Lei W, Feng Y (2016) Promotion of osteointegration under diabetic conditions by tantalum coating-based surface modification on 3-dimensional printed porous titanium implants. Colloids Surf B Biointerfaces 148:440–452
Ma XY, Feng YF, Wang TS, Lei W, Li X, Zhou DP, Wen XX, Yu HL, Xiang LB, Wang L (2017) Involvement of FAK-mediated BMP-2/Smad pathway in mediating osteoblast adhesion and differentiation on nano-HA/chitosan composite coated titanium implant under diabetic conditions. Biomater Sci 6:225–238
Ehnert S, Freude T, Ihle C, Mayer L, Braun B, Graeser J, Flesch I, Stockle U, Nussler AK, Pscherer S (2015) Factors circulating in the blood of type 2 diabetes mellitus patients affect osteoblast maturation—description of a novel in vitro model. Exp Cell Res 332:247–258
Zhang Y, Yang JH (2013) Activation of the PI3K/Akt pathway by oxidative stress mediates high glucose-induced increase of adipogenic differentiation in primary rat osteoblasts. J Cell Biochem 114:2595–2602
Funding
This work was supported by the National Nature Science Foundation of China [Grant numbers: 81701031, 31100690], Postdoctoral Science Foundation of China [Grant number: 2017M622981], Project funded by Chongqing Special Postdoctoral Science Foundation [Grant number: XmT2018009], and Chongqing Research Program of Basic Research and Frontier Technology [Grant number: cstc2017jcyjAX0376].
Author information
Authors and Affiliations
Contributions
YL and AS contributed equally to this work on writing the manuscript. HZ and LL searched literatures; DL and TF analyzed and selected literature; JS and PJ gave the idea of this manuscript; YH and TC made correction of this manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
All authors have no conflicts of interest.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
No informed consent was necessary for this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Li, Y., Shrestha, A., Zhang, H. et al. Impact of diabetes mellitus simulations on bone cell behavior through in vitro models. J Bone Miner Metab 38, 607–619 (2020). https://doi.org/10.1007/s00774-020-01101-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00774-020-01101-5