Abstract
Purpose
To provide the first meta-analysis of the impact of magnetic resonance imaging (MRI) on thoracolumbar fractures (TLFs) classification and decision-making.
Methods
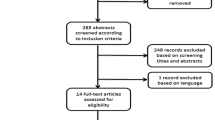
A systematic review was conducted following PRISMA guidelines. We searched PubMed, Scopus, Cochrane, and Web of Science from inception to June 30, 2023 for studies evaluating the change in TLFs classification and treatment decisions after MRI. The studies extracted key findings, objectives, and patient population. A meta-analysis was performed for the pooled frequency of change in AO fracture classification or treatment decisions from surgical to conservative or vice versa after MRI.
Results
This meta-analysis included four studies comprising 554 patients. The pooled frequency of change in TLFs classification was 17% (95% CI 9–31%), and treatment decision was 22% (95% CI 11–40%). An upgrade from type A to type B was reported in 15.7% (95% CI 7.2–30.6%), and downgrading type B to type A in 1.2% (95% CI 0.17–8.3%). A change from conservative to surgery recommendation of 17% (95% CI 5.0–43%) was higher than a change from surgery to conservative 2% (95% CI 1–34%).
Conclusions
MRI can significantly change the thoracolumbar classification and decision-making, primarily due to upgrading type A to type B fractures and changing from conservative to surgery, respectively. These findings suggest that MRI could change decision-making sufficiently to justify its use for TLFs. Type A subtypes, indeterminate PLC status, and spine regions might help to predict a change in TLFs’ classification. However, more studies are needed to confirm the association of these variables with changes in treatment decisions to set the indications of MRI in neurologically intact patients with TLFs. An interactive version of our analysis can be accessed from here: https://databoard.shinyapps.io/mri_spine/.






Similar content being viewed by others
Availability of data and material
Not applicable.
Code availability
Software application or custom code: Not applicable.
References
Schroeder GD, Harrop JS, Vaccaro AR (2017) Thoracolumbar trauma classification. Neurosurg Clin N Am 28:23–29. https://doi.org/10.1016/j.nec.2016.07.007
Denis F (1983) The three column spine and its significance in the classification of acute thoracolumbar spinal injuries. Spine (Phila Pa 1976) 8:817–831. https://doi.org/10.1097/00007632-198311000-00003
Magerl F, Aebi M, Gertzbein SD et al (1994) A comprehensive classification of thoracic and lumbar injuries. Eur Spine J 3:184–201. https://doi.org/10.1007/BF02221591
Vaccaro AR, Lehman RA, Hurlbert RJ et al (2005) A new classification of thoracolumbar injuries: the importance of injury morphology, the integrity of the posterior ligamentous complex, and neurologic status. Spine (Phila Pa 1976) 30:2325–2333. https://doi.org/10.1097/01.brs.0000182986.43345.cb
Vaccaro AR, Oner C, Kepler CK et al (2013) AOSpine thoracolumbar spine injury classification system: fracture description, neurological status, and key modifiers. Spine 38:2028–2037. https://doi.org/10.1097/BRS.0b013e3182a8a381
Rajasekaran S, Vaccaro AR, Kanna RM et al (2017) The value of CT and MRI in the classification and surgical decision-making among spine surgeons in thoracolumbar spinal injuries. Eur Spine J 26:1463–1469. https://doi.org/10.1007/s00586-016-4623-0
Aly MM, Al-Shoaibi AM, Zahrani A, Al Fattani A (2021) Analysis of the combined computed tomography findings improves the accuracy of computed tomography for detecting posterior ligamentous complex injury of the thoracolumbar spine as defined by magnetic resonance imaging. World Neurosurg. https://doi.org/10.1016/j.wneu.2021.04.106
Leferink V, Veldhuis E, Zimmerman K et al (2002) Classificational problems in ligamentary distraction type vertebral fractures: 30% of all B-type fractures are initially unrecognised. Eur Spine J 11:246–250. https://doi.org/10.1007/s00586-001-0366-6
Petersilge CA, Pathria MN, Emery SE, Masaryk TJ (1995) Thora columbar burst fractures: evaluation with MR imaging. Radiology 194:49–54
Qureshi S, Dhall SS, Anderson PA et al (2019) Congress of neurological surgeons systematic review and evidence-based guidelines on the evaluation and treatment of patients with thoracolumbar spine trauma: radiological evaluation. Clin Neurosurg 84:E28–E31. https://doi.org/10.1093/neuros/nyy373
Pizones J, Izquierdo E, Álvarez P et al (2011) Impact of magnetic resonance imaging on decision making for thoracolumbar traumatic fracture diagnosis and treatment. Eur Spine J 20(Suppl 3):390–396. https://doi.org/10.1007/s00586-011-1913-4
Winklhofer S, Thekkumthala-Sommer M, Schmidt D et al (2013) Magnetic resonance imaging frequently changes classification of acute traumatic thoracolumbar spine injuries. Skeletal Radiol 42:779–786. https://doi.org/10.1007/s00256-012-1551-x
Aly MM, Al-Shoaibi AM, Abduraba Ali S et al (2022) How often would MRI change the thoracolumbar fracture classification or decision-making compared to ct alone? Orig Res Glob Spine J. https://doi.org/10.1177/21925682221089579
Durmaz A, İlter MH, Tuzlali H (2021) Is magnetic resonance imaging needed for decision making diagnosis and treatment of thoracic and lumbar vertebral fractures? Eur J Orthop Surg Traumatol. https://doi.org/10.1007/S00590-021-03165-Z
Whiting PF, Rutjes AWSS, Westwood ME et al (2011) QUADAS-2: arevised tool for quality assessment of diagnostic accuracy studies. Ann Intern Med 155:529–536
Aly MM, Al-Shoaibi AM, Aljuzair AH et al (2022) GSJ-systematic review a proposal for a standardized imaging algorithm to improve the accuracy and reliability for the diagnosis of thoracolumbar posterior ligamentous complex injury in computed tomography and magnetic resonance imaging. Glob Spine J. https://doi.org/10.1177/21925682221129220
Bossuyt PM, Reitsma JB, Bruns DE et al (2015) STARD 2015: An updated list of essential items for reporting diagnostic accuracy studies. BMJ 351:1–9. https://doi.org/10.1136/bmj.h5527
Javier P, Sánchez-Mariscal F, Zúñiga L, Patricia Álvarez EI (2013) Prospective analysis of magnetic resonance imaging accuracy in diagnosing traumatic injuries of the posterior ligamentous complex of the thoracolumbar spine. Spine (Phila Pa 1976) 38:745–751
Aly MM, Elemam R, El-Sharkawi M, Hurlbert JR (2022) Injury of the thoracolumbar posterior ligamentous complex: a bibliometric literature review. World Neurosurg. https://doi.org/10.1016/J.WNEU.2022.01.041
Van Middendorp JJ, Patel AA, Schuetz M, Joaquim AF (2013) The precision, accuracy and validity of detecting posterior ligamentous complex injuries of the thoracic and lumbar spine: a critical appraisal of the literature. Eur Spine J 22:461–474. https://doi.org/10.1007/s00586-012-2602-7
Wu CC, Jin HM, Yan YZ et al (2018) Biomechanical role of the thoracolumbar ligaments of the posterior ligamentous complex: a finite element study. World Neurosurg 112:e125–e133. https://doi.org/10.1016/j.wneu.2017.12.171
Rosenthal BD, Boody BS, Jenkins TJ et al (2018) Thoracolumbar burst fractures. Clin Spine Surg 31:143–151. https://doi.org/10.1097/BSD.0000000000000634
Aly MM, Al-Shoaibi AM, Al-Aithan A et al (2021) Can vertical laminar fracture further discriminate fracture severity between thoracolumbar AO type A3 and A4 fractures? World Neurosurg. https://doi.org/10.1016/J.WNEU.2021.08.035
Benedetti PF, Fahr LM, Kuhns LR, Hayman LA (2000) MR imaging findings in spinal ligamentous injury. Am J Roentgenol 175:661–665. https://doi.org/10.2214/ajr.175.3.1750661
Acknowledgements
Not applicable.
Funding
No specific funding was received for this work.
Author information
Authors and Affiliations
Contributions
Contribution: All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by MA, YS, RE, JP, AZ, and SW. The first draft of the manuscript was written by the first author; all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no commercial associations that might pose a conflict of interest in relation to the manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Aly, M.M., Soliman, Y., Elemam, R.A. et al. How frequently MRI modifies thoracolumbar fractures’ classification or decision-making? A systematic review and meta-analysis. Eur Spine J 33, 1540–1549 (2024). https://doi.org/10.1007/s00586-023-08087-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-08087-4