Abstract
Purpose
The treatment of low back pain associated to Disc Degenerative Disease (DDD) is still controversial. Segmental Fusion is the gold standard, but many studies have reported that motion-preserving devices bring substantial clinical benefits to patients. Concerns on the associated complications and on the long-term clinical effectiveness of such instrumentations are still present and have led recently to a decrease of the number of Lumbar Total Disk Replacements (TDR). The objective of this prospective study is to present the clinical and radiographic outcomes of the Maverick Lumbar disk prostheses (Medtronic, TE, Memphis, USA) at long-term follow-up.
Methods
Prospective, single center study of clinical outcome of the treatment with Maverick lumbar Prosthesis of patients with low back pain from DDD resistant to conservative treatment. Patients were examined preoperatively and at 3 months, 2 and 10 years post-operatively. Patients were examined preoperatively and at 3 months, 2 and 10 years post-operatively. Visual analog scale (VAS), Oswestry disability index (ODI) and 36-Item Short Form Health Survey questionnaire were assessed to study clinical outcomes. Radiographic studies allowed measurements of range of motion, adjacent segment disease and pelvic and lumbar parameters.
Results
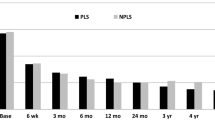
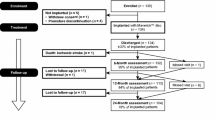
From an initial cohort of 87 patients who underwent TDR between 2003 and 2007 with the Maverick prosthesis, 61 were available at Final follow-up (70%). The clinical outcomes measured by VAS and ODI showed a significant improvement in all the postoperative stages of the follow-up (FU). At 10 years-FU, ODI experienced a mean decrease of 21.1 points, VAS for back pain decreased up to 3.85 and substantial clinical benefit was reached for 55.6% of the patients. Although Mobility of the prosthesis was preserved in 76.8% of the cases, TDR was not clearly protective against ALD.
Conclusions
A significant, clinically relevant, and lasting reduction of back pain has been achieved in patients who underwent a total disk arthroplasty or a Hybrid construct with Maverik prosthesis. TDR is a safe and effective technique to decrease pain in patients with one or two levels of DDD.


Similar content being viewed by others
References
Hoy D, Brooks P, Blyth F, Buchbinder R (2010) The Epidemiology of low back pain. Best Pract Res Clin Rheumatol 24:769–781. doi:10.1016/j.berh.2010.10.002
Siepe CJ, Heider F, Wiechert K et al (2014) Mid- to long-term results of total lumbar disc replacement: a prospective analysis with 5- to 10-year follow-up. Spine J 14:1417–1431. doi:10.1016/j.spinee.2013.08.028
Sköld C, Tropp H, Berg S (2013) Five-year follow-up of total disc replacement compared to fusion: a randomized controlled trial. Eur Spine J 22:2288–2295. doi:10.1007/s00586-013-2926-y
Aghayev E, Etter C, Bärlocher C et al (2014) Five-year results of lumbar disc prostheses in the SWISSspine registry. Eur Spine J 23:2114–2126. doi:10.1007/s00586-014-3418-4
Lu S, Hai Y, Kong C et al (2015) An 11-year minimum follow-up of the Charite III lumbar disc replacement for the treatment of symptomatic degenerative disc disease. Eur Spine J 24:2056–2064. doi:10.1007/s00586-015-3939-5
Park SJ, Lee CS, Chung SS et al (2016) Surgical results of metastatic spinal cord compression (MSCC) from non-small cell lung cancer (NSCLC): analysis of functional outcome, survival time, and complication. Spine J 16(3):322–328
Le Huec JC, Mathews H, Basso Y et al (2005) Clinical results of Maverick lumbar total disc replacement: 2-year prospective follow-up. Orthop Clin N Am 36:315–322. doi:10.1016/j.ocl.2005.02.001
Aunoble S, Meyrat R, Al Sawad Y et al (2010) Hybrid construct for two levels disc disease in lumbar spine. Eur Spine J 19:290–296. doi:10.1007/s00586-009-1182-7
Pekkanen L, Neva MH, Kautiainen H et al (2013) Disability and health-related quality of life in patients undergoing spinal fusion: a comparison with a general population sample. BMC Musculoskelet Disord 14:211. doi:10.1186/1471-2474-14-211
Chiou WK, Lee YH, Chen WJ et al (1996) A non-invasive protocol for the determination of lumbar spine mobility. Clin Biomech 11:474–480. doi:10.1016/S0268-0033(96)00035-6
Mimura M, Panjabi MM, Oxland TR et al (1994) Disc degeneration affects the multidirectional flexibility of the lumbar spine. Spine (Phila Pa 1976) 19:1371–1380
Schwab FJ, Blondel B, Bess S et al (2013) Radiographical spinopelvic parameters and disability in the setting of adult spinal deformity: a prospective multicenter analysis. Spine (Phila Pa 1976) 38:E803–E812. doi:10.1097/BRS.0b013e318292b7b9
Aoki Y, Nakajima A, Takahashi H et al (2015) Influence of pelvic incidence-lumbar lordosis mismatch on surgical outcomes of short-segment transforaminal lumbar interbody fusion. BMC Musculoskelet Disord 16:213. doi:10.1186/s12891-015-0676-1
Le Huec JC, Hasegawa K (2016) Normative values for the spine shape parameters using 3D standing analysis from a database of 268 asymptomatic Caucasian and Japanese subjects. Eur Spine J. doi:10.1007/s00586-016-4485-5
Copay AG, Glassman SD, Subach BR et al (2008) Minimum clinically important difference in lumbar spine surgery patients: a choice of methods using the Oswestry Disability Index, Medical Outcomes Study questionnaire Short Form 36, and Pain Scales. Spine J 8:968–974. doi:10.1016/j.spinee.2007.11.006
Glassman SD, Copay AG, Berven SH et al (2008) Defining substantial clinical benefit following lumbar spine arthrodesis. J Bone Jt Surg Am 90:1839–1847. doi:10.2106/JBJS.G.01095
David T (2007) Long-term results of one-level lumbar arthroplasty: minimum 10-year follow-up of the CHARITE artificial disc in 106 patients. Spine (Phila Pa 1976) 32:661–666. doi:10.1097/01.brs.0000257554.67505.45
Park C-K, Ryu K-S, Lee K-Y, Lee H-J (2012) Clinical outcome of lumbar total disc replacement using ProDisc-L in degenerative disc disease: minimum 5-year follow-up results at a single institute. Spine (Phila Pa 1976) 37:672–677. doi:10.1097/BRS.0b013e31822ecd85
Tropiano P, Huang RC, Girardi FP et al (2005) Lumbar total disc replacement. Seven to eleven-year follow-up. J Bone Jt Surg Am 87:490–496. doi:10.2106/JBJS.C.01345
Geisler FH, McAfee PC, Banco RJ et al (2009) Prospective, randomized, multicenter FDA IDE study of CHARITÉ artificial disc versus lumbar fusion: effect at 5-year follow-up of prior surgery and prior discectomy on clinical outcomes following lumbar arthroplasty. SAS J 3(1):17–25. doi:10.1016/SASJ-2008-0019-RR
Saavedra-Pozo FM, Deusdara RAM, Benzel EC (2014) Adjacent segment disease perspective and review of the literature. Ochsner J 14:78–83
Van Den Eerenbeemt KD, Ostelo RW, Van Royen BJ et al (2010) Total disc replacement surgery for symptomatic degenerative lumbar disc disease: a systematic review of the literature. Eur Spine J 19:1262–1280. doi:10.1007/s00586-010-1445-3
Alahmadi H, Deutsch H (2014) Outcome of salvage lumbar fusion after lumbar arthroplasty. Asian Spine J 8:13–18. doi:10.4184/asj.2014.8.1.13
Roussouly P, Berthonnaud E, Dimnet J (2003) Geometrical and mechanical analysis of lumbar lordosis in an asymptomatic population: proposed classification. Rev Chir orthopédique réparatrice l’appareil Mot 89:632–639
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author(s) declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Plais, N., Thevenot, X., Cogniet, A. et al. Maverick total disc arthroplasty performs well at 10 years follow-up: a prospective study with HRQL and balance analysis. Eur Spine J 27, 720–727 (2018). https://doi.org/10.1007/s00586-017-5065-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-017-5065-z