Abstract
Purpose
To identify the symptom cluster among cancer survivors and examine their subgroup differences via network analysis based on nationally representative data.
Methods
This cross-sectional study included 2966 survivors participating in the 2020 National Health Interview Survey (NHIS). Participants self-reported the presence of 14 symptoms capturing four clusters (physical, somatic, sleep, and psychologic problems). Network analysis models were used to reveal the relationships between symptoms and those interactions. Network comparison tests were applied to compare subgroups.
Results
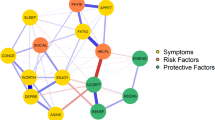
The core symptoms of the symptom cluster were fatigue (Bet = 33, Clo = 0.0067, Str = 0.9397), pain (Bet = 11, Clo = 0.0060, Str = 0.9226), wake up well rested (Bet = 25, Clo = 0.0057, Str = 0.8491), and anxiety (Bet = 5, Clo = 0.0043, Str = 0.9697) among cancer survivors. The core symptoms, network structure, and global strength were invariant between time since diagnoses (< 2 years vs. ≥ 2 years) or between numbers of cancers (1 vs. ≥ 2), yet varied between the comorbidity group and non-comorbidity group (≥ 1 vs. 0).
Conclusions
Fatigue would be a potential target for alleviating other symptoms through a negative feedback loop of other related symptoms of cancer survivors. In particular, cancer survivors with other chronic diseases should be the focus of attention and strengthen targeted intervention.



Similar content being viewed by others
Data availability
No datasets were generated or analysed during the current study.
References
Siegel RL, Miller KD, Fuchs HE, Jemal A (2022) Cancer statistics, 2022. CA Cancer J Clin 72(1):7–33. https://doi.org/10.3322/caac.21708
Cleeland CS (2007) Symptom burden: multiple symptoms and their impact as patient-reported outcomes. J Natl Cancer Inst Monogr 37:16–21. https://doi.org/10.1093/jncimonographs/lgm005
Wu HS, Harden JK (2015) Symptom burden and quality of life in survivorship: a review of the literature. Cancer Nurs 38(1):E29-54. https://doi.org/10.1097/NCC.0000000000000135
Miaskowski C, Aouizerat BE, Dodd M, Cooper B (2007) Conceptual issues in symptom clusters research and their implications for quality-of-life assessment in patients with cancer. JNCI Monographs 2007(37):39–46. https://doi.org/10.1093/jncimonographs/lgm003
Miaskowski C, Barsevick A, Berger A et al (2017) Advancing symptom science through symptom cluster research: expert panel proceedings and recommendations. JNCI J Natl Cancer Inst 109(4):djw253. https://doi.org/10.1093/jnci/djw253
Harrington CB, Hansen JA, Moskowitz M, Todd BL, Feuerstein M (2010) It’s not over when it’s over: long-term symptoms in cancer survivors—a systematic review. Int J Psychiatry Med 40(2):163–181. https://doi.org/10.2190/PM.40.2.c
Sanford SD, Beaumont JL, Butt Z, Sweet JJ, Cella D, Wagner LI (2014) Prospective longitudinal evaluation of a symptom cluster in breast cancer. J Pain Symptom Manage 47(4):721–730. https://doi.org/10.1016/j.jpainsymman.2013.05.010
Nho JH, Reul Kim S, Nam JH (2017) Symptom clustering and quality of life in patients with ovarian cancer undergoing chemotherapy. Eur J Oncol Nurs 30:8–14. https://doi.org/10.1016/j.ejon.2017.07.007
Harris CS, Kober KM, Cooper B et al (2022) Symptom clusters in outpatients with cancer using different dimensions of the symptom experience. Support Care Cancer 30(8):6889–6899. https://doi.org/10.1007/s00520-022-07125-z
Choi S, Ryu E (2018) Effects of symptom clusters and depression on the quality of life in patients with advanced lung cancer. Eur J Cancer Care 27(1):e12508. https://doi.org/10.1111/ecc.12508
Dong ST, Butow PN, Costa DSJ, Lovell MR, Agar M (2014) Symptom clusters in patients with advanced cancer: a systematic review of observational studies. J Pain Symptom Manage 48(3):411–450. https://doi.org/10.1016/j.jpainsymman.2013.10.027
Nipp RD, El-Jawahri A, Moran SM et al (2017) The relationship between physical and psychological symptoms and health care utilization in hospitalized patients with advanced cancer: Symptoms and Health Care Utilization. Cancer 123(23):4720–4727. https://doi.org/10.1002/cncr.30912
Kirkova J, Aktas A, Walsh D, Davis MP (2011) Cancer symptom clusters: clinical and research methodology. J Palliat Med 14(10):1149–1166. https://doi.org/10.1089/jpm.2010.0507
Shim E, Ha H, Suh Y et al (2021) Network analyses of associations between cancer-related physical and psychological symptoms and quality of life in gastric cancer patients. Psychooncology 30(6):946–953. https://doi.org/10.1002/pon.5681
Mkhitaryan S, Crutzen R, Steenaart E, De Vries NK (2019) Network approach in health behavior research: how can we explore new questions? Health Psychol Behav Med 7(1):362–384. https://doi.org/10.1080/21642850.2019.1682587
Papachristou N, Barnaghi P, Cooper B et al (2019) Network analysis of the multidimensional symptom experience of oncology. Sci Rep 9(1):2258. https://doi.org/10.1038/s41598-018-36973-1
Beard C, Millner AJ, Forgeard MJC et al (2016) Network analysis of depression and anxiety symptom relationships in a psychiatric sample. Psychol Med 46(16):3359–3369. https://doi.org/10.1017/S0033291716002300
Borsboom D, Cramer AOJ (2013) Network analysis: an integrative approach to the structure of psychopathology. Annu Rev Clin Psychol 9(1):91–121. https://doi.org/10.1146/annurev-clinpsy-050212-185608
De Rooij BH, Oerlemans S, Van Deun K et al (2021) Symptom clusters in 1330 survivors of 7 cancer types from the PROFILES registry: a network analysis. Cancer 127(24):4665–4674. https://doi.org/10.1002/cncr.33852
Huang IC, Brinkman TM, Kenzik K et al (2013) Association between the prevalence of symptoms and health-related quality of life in adult survivors of childhood cancer: a report from the St Jude Lifetime Cohort Study. JCO 31(33):4242–4251. https://doi.org/10.1200/JCO.2012.47.8867
Shin H, Dudley WN, Bhakta N et al (2023) Associations of symptom clusters and health outcomes in adult survivors of childhood cancer: a report from the St Jude Lifetime Cohort Study. JCO 41(3):497–507. https://doi.org/10.1200/JCO.22.00361
Epskamp S, Cramer AO, Waldorp LJ, Schmittmann VD, Borsboom D (2012) qgraph: network visualizations of relationships in psychometric data. J Stat Softw 48(4):1–18. https://doi.org/10.18637/jss.v048.i04
Epskamp S, Fried EI (2018) A tutorial on regularized partial correlation networks. Psychol Methods 23(4):617–634. https://doi.org/10.1037/met0000167
Fang J, Wong CL, Liu CQ et al (2023) Identifying central symptom clusters and correlates in children with acute leukemia undergoing chemotherapy: a network analysis. Front Oncol 13:1236129. https://doi.org/10.3389/fonc.2023.1236129
Fernández-de-las-Peñas C, Palacios-Ceña M, Valera-Calero JA et al (2022) Understanding the interaction between clinical, emotional and psychophysical outcomes underlying tension-type headache: a network analysis approach. J Neurol 269(8):4525–4534. https://doi.org/10.1007/s00415-022-11039-5
Schlegl S, Smith KE, Vierl L et al (2021) Using network analysis to compare diagnosis-specific and age-specific symptom networks in eating disorders. Intl J Eating Disorders 54(8):1463–1476. https://doi.org/10.1002/eat.23523
Bloch F, Jackson MO, Tebaldi P (2019) Centrality measures in networks. Available at SSRN: https://doi.org/10.2139/ssrn.2749124
Opsahl T, Agneessens F, Skvoretz J (2010) Node centrality in weighted networks: generalizing degree and shortest paths. Soc Networks 32(3):245–251. https://doi.org/10.1016/j.socnet.2010.03.006
Neijenhuijs KI, Peeters CFW, Van Weert H, Cuijpers P, de Leeuw IV (2021) Symptom clusters among cancer survivors: what can machine learning techniques tell us? BMC Med Res Methodol 21(1):166. https://doi.org/10.1186/s12874-021-01352-4
Ma Y, He B, Jiang M et al (2020) Prevalence and risk factors of cancer-related fatigue: a systematic review and meta-analysis. Int J Nurs Stud 111:103707. https://doi.org/10.1016/j.ijnurstu.2020.103707
Trudel-Fitzgerald C, Savard J, Ivers H (2013) Which symptoms come first? Exploration of temporal relationships between cancer-related symptoms over an 18-month period. Ann Behav Med 45(3):329–337. https://doi.org/10.1007/s12160-012-9459-1
Sotelo JL, Musselman D, Nemeroff C (2014) The biology of depression in cancer and the relationship between depression and cancer progression. Int Rev Psychiatry 26(1):16–30. https://doi.org/10.3109/09540261.2013.875891
Götze H, Friedrich M, Taubenheim S, Dietz A, Lordick F, Mehnert A (2020) Depression and anxiety in long-term survivors 5 and 10 years after cancer diagnosis. Support Care Cancer 28(1):211–220. https://doi.org/10.1007/s00520-019-04805-1
Bai W, Zhao YJ, Cai H et al (2022) Network analysis of depression, anxiety, insomnia and quality of life among Macau residents during the COVID-19 pandemic. J Affect Disord 311:181–188. https://doi.org/10.1016/j.jad.2022.05.061
Cox RC, Olatunji BO (2021) Sleep in a pandemic: implications of COVID-19 for sleep through the lens of the 3P model of insomnia. Am Psychol 76(7):1159–1171. https://doi.org/10.1037/amp0000850
Mullarkey MC, Marchetti I, Beevers CG (2019) Using network analysis to identify central symptoms of adolescent depression. J Clin Child Adolesc Psychol 48(4):656–668. https://doi.org/10.1080/15374416.2018.1437735
Rutten RJT, Broekman TG, Schippers GM, Schellekens AFA (2021) Symptom networks in patients with substance use disorders. Drug Alcohol Depend 229:109080. https://doi.org/10.1016/j.drugalcdep.2021.109080
Nguyen LT, Alexander K, Yates P (2018) Psychoeducational intervention for symptom management of fatigue, pain, and sleep disturbance cluster among cancer patients: a pilot quasi-experimental study. J Pain Symptom Manage 55(6):1459–1472. https://doi.org/10.1016/j.jpainsymman.2018.02.019
Cillessen L, Johannsen M, Speckens AEM, Zachariae R (2019) Mindfulness-based interventions for psychological and physical health outcomes in cancer patients and survivors: a systematic review and meta-analysis of randomized controlled trials. Psychooncology 28(12):2257–2269. https://doi.org/10.1002/pon.5214
Zhao C, Lai L, Zhang L et al (2021) The effects of acceptance and commitment therapy on the psychological and physical outcomes among cancer patients: a meta-analysis with trial sequential analysis. J Psychosom Res 140:110304. https://doi.org/10.1016/j.jpsychores.2020.110304
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection, and analysis were performed by Zhen Zhang and Jiahui Lao. The first draft of the manuscript was written by Zhen Zhang. Supervision and writing—review and editing were performed by Min Zhang, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
The National Health Interview Survey (NHIS) is publicly available. The data we used were collected by the National Center for Health Statistics (NCHS). The NHIS protocols were authorized by the NCHS ethics review board. So, the ethical approval was not required.
Consent to participate
All survey participants provided informed consent to participate in NHIS.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, Z., Lao, J., Liu, M. et al. Symptom cluster among cancer survivors from a nationally representative survey: a network analysis. Support Care Cancer 32, 333 (2024). https://doi.org/10.1007/s00520-024-08531-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00520-024-08531-1