Abstract
The majority of calcium filtered by the glomerulus is reabsorbed along the nephron. Most is reabsorbed from the proximal tubule (> 60%) via a paracellular pathway composed of the tight junction proteins claudins-2 and -12, a process driven by sodium and consequently water reabsorption. The thick ascending limb reabsorbs the next greatest amount of calcium (20–25%), also by a paracellular pathway composed of claudins-16 and -19. This pathway is regulated by the CaSR, whose activity increases the expression of claudin-14, a protein that blocks paracellular calcium reabsorption. The fine tuning of urinary calcium excretion occurs in the distal convoluted and connecting tubule by a transcellular pathway composed of the apical calcium channel TRPV5, the calcium shuttling protein calbindin-D28K and the basolateral proteins PMCA1b and the sodium calcium exchanger, NCX. Not surprisingly, mutations in a subset of these genes cause monogenic disorders with hypercalciuria as a part of the phenotype. More commonly, “idiopathic” hypercalciuria is encountered clinically with genetic variations in CLDN14, the CASR and TRPV5 associating with kidney stones and increased urinary calcium excretion. An understanding of the molecular pathways conferring kidney tubular calcium reabsorption is employed in this review to help explain how dietary and medical interventions for this disorder lower urinary calcium excretion.

Similar content being viewed by others
References
Beggs MR, Alexander RT (2017) Intestinal absorption and renal reabsorption of calcium throughout postnatal development. Exp Biol Med (Maywood) 242:840–849. https://doi.org/10.1177/1535370217699536
Peacock M (2010) Calcium metabolism in health and disease. Clin J Am Soc Nephrol 5:S23–S30. https://doi.org/10.2215/CJN.05910809
Ross AC, Taylor CL, Yaktine AL, Del Valle HB (2011) Dietary reference intakes for calcium and vitamin D. The National Academies Press, Washington, DC
Alexander RT, Dimke H, Cordat E (2013) Proximal tubular NHEs: sodium, protons and calcium? Am J Physiol Renal Physiol 305:F229–F236. https://doi.org/10.1152/ajprenal.00065.2013
Alexander RT, Cordat E, Chambrey R, Dimke H, Eladari D (2016) Acidosis and urinary calcium excretion: insights from genetic disorders. J Am Soc Nephrol 27:3511–3520. https://doi.org/10.1681/ASN.2016030305
Wright FS, Bomsztyk K (1986) Calcium transport by the proximal tubule. Adv Exp Med Biol 208:165–170. https://doi.org/10.1007/978-1-4684-5206-8_18
Wiebe SA, Plain A, Pan W, O’Neill D, Braam B, Alexander RT (2019) NHE8 attenuates Ca2+ influx into NRK cells and the proximal tubule epithelium. Am J Physiol Renal Physiol 317:F240–F253. https://doi.org/10.1152/ajprenal.00329.2018
Plain A, Pan W, O’Neill D, Ure M, Beggs MR, Farhan M, Dimke H, Cordat E, Alexander RT (2020) Claudin-12 knockout mice demonstrate reduced proximal tubule calcium permeability. Int J Mol Sci 21:2074. https://doi.org/10.3390/ijms21062074
Curry JN, Saurette M, Askari M, Pei L, Filla MB, Beggs MR, Rowe PS, Fields T, Sommer AJ, Tanikawa C, Kamatani Y, Evan AP, Totonchi M, Alexander RT, Matsuda K, Yu AS (2020) Claudin-2 deficiency associates with hypercalciuria in mice and human kidney stone disease. J Clin Invest 130:1948–1960. https://doi.org/10.1172/JCI127750
Pan W, Borovac J, Spicer Z, Hoenderop JG, Bindels RJ, Shull GE, Doschak MR, Cordat E, Alexander RT (2012) The epithelial sodium/proton exchanger, NHE3, is necessary for renal and intestinal calcium (re)absorption. Am J Physiol Renal Physiol 302:F943–F956. https://doi.org/10.1152/ajprenal.00504.2010
Sutton RA, Walker VR (1980) Responses to hydrochlorothiazide and acetazolamide in patients with calcium stones. Evidence suggesting a defect in renal tubular function. N Engl J Med 302:709–713. https://doi.org/10.1056/NEJM198003273021302
Worcester EM, Coe FL, Evan AP, Bergsland KJ, Parks JH, Willis LR, Clark DL, Gillen DL (2008) Evidence for increased postprandial distal nephron calcium delivery in hypercalciuric stone-forming patients. Am J Physiol Renal Physiol 295:F1286–F1294. https://doi.org/10.1152/ajprenal.90404.2008
Plain A, Alexander RT (2018) Claudins and nephrolithiasis. Curr Opin Nephrol Hypertens 27:268–276. https://doi.org/10.1097/MNH.0000000000000426
Edwards A, Bonny O (2018) A model of calcium transport and regulation in the proximal tubule. Am J Physiol Renal Physiol 315:F942–F953. https://doi.org/10.1152/ajprenal.00129.2018
Wang T, Yang CL, Abbiati T, Schultheis PJ, Shull GE, Giebisch G, Aronson PS (1999) Mechanism of proximal tubule bicarbonate absorption in NHE3 null mice. Am J Phys 277:F298–F302. https://doi.org/10.1152/ajprenal.1999.277.2.F298
Janecke AR, Heinz-Erian P, Yin J, Petersen B-S, Franke A, Lechner S, Fuchs I, Melancon S, Uhlig HH, Travis S, Marinier E, Perisic V, Ristic N, Gerner P, Booth IW, Wedenoja S, Baumgartner N, Vodopiutz J, Frechette-Duval M-C, De Lafollie J, Persad R, Warner N, Tse CM, Sud K, Zachos NC, Sarker R, Zhu X, Muise AM, Zimmer K-P, Witt H, Zoller H, Donowitz M, Müller T (2015) Reduced sodium/proton exchanger NHE3 activity causes congenital sodium diarrhea. Hum Mol Genet 24:6614–6623. https://doi.org/10.1093/hmg/ddv367
Rector FC (1983) Sodium, bicarbonate, and chloride absorption by the proximal tubule. Am J Phys 244:F461–F471. https://doi.org/10.1152/ajprenal.1983.244.5.F461
Kokko JP (1973) Proximal tubule potential difference. Dependence on glucose on glucose, HCO 3, and amino acids. J Clin Invest 52:1362–1367. https://doi.org/10.1172/JCI107308
Kiuchi-Saishin Y, Gotoh S, Furuse M, Takasuga A, Tano Y, Tsukita S (2002) Differential expression patterns of claudins, tight junction membrane proteins, in mouse nephron segments. J Am Soc Nephrol 13:875–886
Krug SM, Günzel D, Conrad MP, Rosenthal R, Fromm A, Amasheh S, Schulzke JD, Fromm M (2012) Claudin-17 forms tight junction channels with distinct anion selectivity. Cell Mol Life Sci 69:2765–2778. https://doi.org/10.1007/s00018-012-0949-x
Muto S, Hata M, Taniguchi J, Tsuruoka S, Moriwaki K, Saitou M, Furuse K, Sasaki H, Fujimura A, Imai M, Kusano E, Tsukita S, Furuse M (2010) Claudin-2-deficient mice are defective in the leaky and cation-selective paracellular permeability properties of renal proximal tubules. Proc Natl Acad Sci U S A 107:8011–8016. https://doi.org/10.1073/pnas.0912901107
Brown AJ, Dusso A, Slatopolsky E (1999) Vitamin D. Am J Physiol Ren Physiol 277:F157–F175. https://doi.org/10.1152/ajprenal.1999.277.2.F157
Schlingmann KP, Kaufmann M, Weber S, Irwin A, Goos C, John U, Misselwitz J, Klaus G, Kuwertz-Bröking E, Fehrenbach H, Wingen AM, Güran T, Hoenderop JG, Bindels RJ, Prosser DE, Jones G, Konrad M (2011) Mutations in CYP24A1 and idiopathic infantile hypercalcemia. N Engl J Med 365:410–421. https://doi.org/10.1056/NEJMoa1103864
Blanchard A, Curis E, Guyon-Roger T, Kahila D, Treard C, Baudouin V, Bérard E, Champion G, Cochat P, Dubourg J, de la Faille R, Devuyst O, Deschenes G, Fischbach M, Harambat J, Houillier P, Karras A, Knebelmann B, Lavocat M-P, Loirat C, Merieau E, Niaudet P, Nobili F, Novo R, Salomon R, Ulinski T, Jeunemaître X, Vargas-Poussou R (2016) Observations of a large Dent disease cohort. Kidney Int 90:430–439. https://doi.org/10.1016/j.kint.2016.04.022
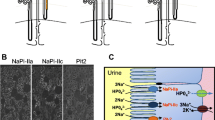
Bergwitz C, Roslin NM, Tieder M, Loredo-Osti JC, Bastepe M, Abu-Zahra H, Frappier D, Burkett K, Carpenter TO, Anderson D, Garabedian M, Sermet I, Fujiwara TM, Morgan K, Tenenhouse HS, Juppner H (2006) SLC34A3 mutations in patients with hereditary hypophosphatemic rickets with hypercalciuria predict a key role for the sodium-phosphate cotransporter NaPi-IIc in maintaining phosphate homeostasis. Am J Hum Genet 78:179–192. https://doi.org/10.1086/499409
Downie ML, Garcia SCL, Kleta R, Bockenhauer D (2020) Inherited tubulopathies of the kidney: insights from genetics. Clin J Am Soc Nephrol. https://doi.org/10.2215/CJN.14481119
Simon DB, Karet FE, Hamdan JM, DiPietro A, Sanjad SA, Lifton RP (1996) Bartter’s syndrome, hypokalaemic alkalosis with hypercalciuria, is caused by mutations in the Na-K-2Cl cotransporter NKCC2. Nat Genet 13:183–188. https://doi.org/10.1038/ng0696-183
Simon DB, Karet FE, Rodriguez-Soriano J, Hamdan JH, DiPietro A, Trachtman H, Sanjad SA, Lifton RP (1996) Genetic heterogeneity of Bartter’s syndrome revealed by mutations in the K+ channel, ROMK. Nat Genet 14:152–156. https://doi.org/10.1038/ng1096-152
Simon DB, Bindra RS, Mansfield TA, Nelson-Williams C, Mendonca E, Stone R, Schurman S, Nayir A, Alpay H, Bakkaloglu A, Rodriguez-Soriano J, Morales JM, Sanjad SA, Taylor CM, Pilz D, Brem A, Trachtman H, Griswold W, Richard GA, John E, Lifton RP (1997) Mutations in the chloride channel gene, CLCNKB, cause Bartter’s syndrome type III. Nat Genet 17:171–178. https://doi.org/10.1038/ng1097-171
Birkenhäger R, Otto E, Schürmann MJ, Vollmer M, Ruf EM, Maier-Lutz I, Beekmann F, Fekete A, Omran H, Feldmann D, Milford DV, Jeck N, Konrad M, Landau D, Knoers NV, Antignac C, Sudbrak R, Kispert A, Hildebrandt F (2001) Mutation of BSND causes Bartter syndrome with sensorineural deafness and kidney failure. Nat Genet 29:310–314. https://doi.org/10.1038/ng752
Carmosino M, Gerbino A, Hendy GN, Torretta S, Rizzo F, Debellis L, Procino G, Svelto M (2015) NKCC2 activity is inhibited by the Bartter’s syndrome type 5 gain-of-function CaR-A843E mutant in renal cells. Biol Cell 107:98–110. https://doi.org/10.1111/boc.201400069
Toka HR, Al-Romaih K, Koshy JM, DiBartolo S, Kos CH, Quinn SJ, Curhan GC, Mount DB, Brown EM, Pollak MR (2012) Deficiency of the calcium-sensing receptor in the kidney causes parathyroid hormone-independent hypocalciuria. J Am Soc Nephrol 23:1879–1890. https://doi.org/10.1681/ASN.2012030323
van Abel M, Hoenderop JGJ, van der Kemp AWCM, Friedlaender MM, van Leeuwen JPTM, Bindels RJM (2005) Coordinated control of renal Ca2+ transport proteins by parathyroid hormone. Kidney Int 68:1708–1721. https://doi.org/10.1111/j.1523-1755.2005.00587.x
Sato T, Courbebaisse M, Ide N, Fan Y, Hanai J, Kaludjerovic J, Densmore MJ, Yuan Q, Toka HR, Pollak MR, Hou J, Lanske B (2017) Parathyroid hormone controls paracellular Ca2+ transport in the thick ascending limb by regulating the tight-junction protein Claudin14. Proc Natl Acad Sci U S A 114:E3344–E3353. https://doi.org/10.1073/pnas.1616733114
Watanabe S, Fukumoto S, Chang H, Takeuchi Y, Hasegawa Y, Okazaki R, Chikatsu N, Fujita T (2002) Association between activating mutations of calcium-sensing receptor and Bartter’s syndrome. Lancet 360:692–694. https://doi.org/10.1016/S0140-6736(02)09842-2
Pearce SHS, Williamson C, Kifor O, Bai M, Coulthard MG, Davies M, Lewis-Barned N, McCredie D, Powell H, Kendall-Taylor P, Brown EM, Thakker RV (1996) A familial syndrome of hypocalcemia with hypercalciuria due to mutations in the calcium-sensing receptor. N Engl J Med 335:1115–1122. https://doi.org/10.1056/NEJM199610103351505
Pollak MR, Brown EM, Chou YH, Hebert SC, Marx SJ, Steinmann B, Levi T, Seidman CE, Seidman JG (1993) Mutations in the human Ca(2+)-sensing receptor gene cause familial hypocalciuric hypercalcemia and neonatal severe hyperparathyroidism. Cell 75:1297–1303. https://doi.org/10.1016/0092-8674(93)90617-y
Diaz-Thomas A, Cannon J, Iyer P, Al-Maawali A, Fazalullah M, Diamond F, Mueller OT, Root AW, Alyaarubi S (2014) A novel CASR mutation associated with neonatal severe hyperparathyroidism transmitted as an autosomal recessive disorder. J Pediatr Endocrinol Metab 27:851–856. https://doi.org/10.1515/jpem-2013-0343
Nesbit MA, Hannan FM, Howles SA, Babinsky VN, Head RA, Cranston T, Rust N, Hobbs MR, Heath H, Thakker RV (2013) Mutations affecting G-protein subunit α11 in hypercalcemia and hypocalcemia. N Engl J Med 368:2476–2486. https://doi.org/10.1056/NEJMoa1300253
Isojima T, Doi K, Mitsui J, Oda Y, Tokuhiro E, Yasoda A, Yorifuji T, Horikawa R, Yoshimura J, Ishiura H, Morishita S, Tsuji S, Kitanaka S (2014) A recurrent de novo FAM111A mutation causes Kenny-Caffey syndrome type 2. J Bone Miner Res 29:992–998. https://doi.org/10.1002/jbmr.2091
Fine DA, Rozenblatt-Rosen O, Padi M, Korkhin A, James RL, Adelmant G, Yoon R, Guo L, Berrios C, Zhang Y, Calderwood MA, Velmurgan S, Cheng J, Marto JA, Hill DE, Cusick ME, Vidal M, Florens L, Washburn MP, Litovchick L, DeCaprio JA (2012) Identification of FAM111A as an SV40 host range restriction and adenovirus helper factor. PLoS Pathog 8:e1002949. https://doi.org/10.1371/journal.ppat.1002949
Konrad M, Schaller A, Seelow D, Pandey AV, Waldegger S, Lesslauer A, Vitzthum H, Suzuki Y, Luk JM, Becker C, Schlingmann KP, Schmid M, Rodriguez-Soriano J, Ariceta G, Cano F, Enriquez R, Jüppner H, Bakkaloglu SA, Hediger MA, Gallati S, Neuhauss SCF, Nürnberg P, Weber S (2006) Mutations in the tight-junction gene claudin 19 (CLDN19) are associated with renal magnesium wasting, renal failure, and severe ocular involvement. Am J Hum Genet 79:949–957
Simon DB, Lu Y, Choate KA, Velazquez H, Al-Sabban E, Praga M, Casari G, Bettinelli A, Colussi G, Rodriguez-Soriano J, McCredie D, Milford D, Sanjad S, Lifton RP (1999) Paracellin-1, a renal tight junction protein required for paracellular Mg2+ resorption. Science 285:103–106. https://doi.org/10.1126/science.285.5424.103
Konrad M, Hou J, Weber S, Dötsch J, Kari JA, Seeman T, Kuwertz-Bröking E, Peco-Antic A, Tasic V, Dittrich K, Alshaya HO, von Vigier RO, Gallati S, Goodenough DA, Schaller A (2008) CLDN16 genotype predicts renal decline in familial hypomagnesemia with hypercalciuria and nephrocalcinosis. J Am Soc Nephrol 19:171–181. https://doi.org/10.1681/ASN.2007060709
Müller D, Kausalya PJ, Claverie-Martin F, Meij IC, Eggert P, Garcia-Nieto V, Hunziker W (2003) A novel claudin 16 mutation associated with childhood hypercalciuria abolishes binding to ZO-1 and results in lysosomal mistargeting. Am J Hum Genet 73:1293–1301. https://doi.org/10.1086/380418
Hadj-Rabia S, Brideau G, Al-Sarraj Y, Maroun RC, Figueres M-L, Leclerc-Mercier S, Olinger E, Baron S, Chaussain C, Nochy D, Taha RZ, Knebelmann B, Joshi V, Curmi PA, Kambouris M, Vargas-Poussou R, Bodemer C, Devuyst O, Houillier P, El-Shanti H (2018) Multiplex epithelium dysfunction due to CLDN10 mutation: the HELIX syndrome. Genet Med 20:190–201. https://doi.org/10.1038/gim.2017.71
Bongers EMHF, Shelton LM, Milatz S, Verkaart S, Bech AP, Schoots J, Cornelissen EAM, Bleich M, Hoenderop JGJ, Wetzels JFM, Lugtenberg D, Nijenhuis T (2017) A novel hypokalemic-alkalotic salt-losing tubulopathy in patients with CLDN10 mutations. J Am Soc Nephrol 28:3118–3128. https://doi.org/10.1681/ASN.2016080881
Breiderhoff T, Himmerkus N, Drewell H, Plain A, Günzel D, Mutig K, Willnow TE, Müller D, Bleich M (2018) Deletion of claudin-10 rescues claudin-16–deficient mice from hypomagnesemia and hypercalciuria. Kidney Int 93:580–588. https://doi.org/10.1016/j.kint.2017.08.029
Gong Y, Renigunta V, Himmerkus N, Zhang J, Renigunta A, Bleich M, Hou J (2012) Claudin-14 regulates renal Ca++ transport in response to CaSR signalling via a novel microRNA pathway. EMBO J 31:1999–2012. https://doi.org/10.1038/emboj.2012.49
Gong Y, Hou J (2014) Claudin-14 underlies Ca++-sensing receptor–mediated Ca++ metabolism via NFAT-microRNA–based mechanisms. J Am Soc Nephrol 25:745–760. https://doi.org/10.1681/ASN.2013050553
Thorleifsson G, Holm H, Edvardsson V, Walters GB, Styrkarsdottir U, Gudbjartsson DF, Sulem P, Halldorsson BV, de Vegt F, d’Ancona FCH, den Heijer M, Franzson L, Christiansen C, Alexandersen P, Rafnar T, Kristjansson K, Sigurdsson G, Kiemeney LA, Bodvarsson M, Indridason OS, Palsson R, Kong A, Thorsteinsdottir U, Stefansson K (2009) Sequence variants in the CLDN14 gene associate with kidney stones and bone mineral density. Nat Genet 41:926–930. https://doi.org/10.1038/ng.404
Arcidiacono T, Simonini M, Lanzani C, Citterio L, Salvi E, Barlassina C, Spotti D, Cusi D, Manunta P, Vezzoli G (2018) Claudin-14 gene polymorphisms and urine calcium excretion. Clin J Am Soc Nephrol 13:1542–1549. https://doi.org/10.2215/CJN.01770218
Ure ME, Heydari E, Pan W, Ramesh A, Rehman S, Morgan C, Pinsk M, Erickson R, Herrmann JM, Dimke H, Cordat E, Lemaire M, Walter M, Alexander RT (2017) A variant in a cis-regulatory element enhances claudin-14 expression and is associated with pediatric-onset hypercalciuria and kidney stones. Hum Mutat 38:649–657. https://doi.org/10.1002/humu.23202
Wilcox ER, Burton QL, Naz S, Riazuddin S, Smith TN, Ploplis B, Belyantseva I, Ben-Yosef T, Liburd NA, Morell RJ, Kachar B, Wu DK, Griffith AJ, Riazuddin S, Friedman TB (2001) Mutations in the gene encoding tight junction claudin-14 cause autosomal recessive deafness DFNB29. Cell 104:165–172. https://doi.org/10.1016/S0092-8674(01)00200-8
Hoenderop JG, Müller D, Van Der Kemp AW, Hartog A, Suzuki M, Ishibashi K, Imai M, Sweep F, Willems PH, Van Os CH, Bindels RJ (2001) Calcitriol controls the epithelial calcium channel in kidney. J Am Soc Nephrol 12:1342–1349
de Groot T, Lee K, Langeslag M, Xi Q, Jalink K, Bindels RJM, Hoenderop JGJ (2009) Parathyroid hormone activates TRPV5 via PKA-dependent phosphorylation. J Am Soc Nephrol 20:1693–1704. https://doi.org/10.1681/ASN.2008080873
Hsu Y-J, Dimke H, Hoenderop JGJ, Bindels RJM (2010) Calcitonin-stimulated renal Ca2+ reabsorption occurs independently of TRPV5. Nephrol Dial Transplant 25:1428–1435. https://doi.org/10.1093/ndt/gfp645
Hoenderop JGJ, van Leeuwen JPTM, van der Eerden BCJ, Kersten FFJ, van derKemp AWCM, Mérillat A-M, Waarsing JH, Rossier BC, Vallon V, Hummler E, Bindels RJM (2003) Renal Ca2+ wasting, hyperabsorption, and reduced bone thickness in mice lacking TRPV5. J Clin Invest 112:1906–1914. https://doi.org/10.1172/JCI200319826
Renkema KY, Lee K, Topala CN, Goossens M, Houillier P, Bindels RJ, Hoenderop JG (2009) TRPV5 gene polymorphisms in renal hypercalciuria. Nephrol Dial Transplant 24:1919–1924. https://doi.org/10.1093/ndt/gfn735
Oddsson A, Sulem P, Helgason H, Edvardsson VO, Thorleifsson G, Sveinbjörnsson G, Haraldsdottir E, Eyjolfsson GI, Sigurdardottir O, Olafsson I, Masson G, Holm H, Gudbjartsson DF, Thorsteinsdottir U, Indridason OS, Palsson R, Stefansson K (2015) Common and rare variants associated with kidney stones and biochemical traits. Nat Commun 6:7975. https://doi.org/10.1038/ncomms8975
Khaleel A, Wu M-S, Wong HS-C, Hsu Y-W, Chou Y-H, Chen H-Y (2015) A single nucleotide polymorphism (rs4236480) in TRPV5 calcium channel gene is associated with stone multiplicity in calcium nephrolithiasis patients. Mediat Inflamm 2015:375427. https://doi.org/10.1155/2015/375427
Nie M, Bal MS, Yang Z, Liu J, Rivera C, Wenzel A, Beck BB, Sakhaee K, Marciano DK, Wolf MTF (2016) Mucin-1 increases renal TRPV5 activity in vitro, and urinary level associates with calcium nephrolithiasis in patients. J Am Soc Nephrol 27:3447–3458. https://doi.org/10.1681/ASN.2015101100
Wolf MTF, Wu X-R, Huang C-L (2013) Uromodulin upregulates TRPV5 by impairing caveolin-mediated endocytosis. Kidney Int 84:130–137. https://doi.org/10.1038/ki.2013.63
Nijenhuis T, Vallon V, van der Kemp AWCM, Loffing J, Hoenderop JGJ, Bindels RJM (2005) Enhanced passive Ca2+ reabsorption and reduced Mg2+ channel abundance explains thiazide-induced hypocalciuria and hypomagnesemia. J Clin Invest 115:1651–1658. https://doi.org/10.1172/JCI24134
Habbig S, Beck BB, Hoppe B (2011) Nephrocalcinosis and urolithiasis in children. Kidney Int 80:1278–1291. https://doi.org/10.1038/ki.2011.336
Butani L, Kalia A (2004) Idiopathic hypercalciuria in children--how valid are the existing diagnostic criteria? Pediatr Nephrol 19:577–582. https://doi.org/10.1007/s00467-004-1470-8
Alexander RT, Licht C, Smoyer W, Rosenblum NR (2019) Disease of the kidney and urinary tract in children. In: Yu A, Chertow G, Luyckx V, Marsden P, Skorecki K, Taal M (eds) Brenner and Rector’s the kidney, 11th edn. Elsevier Inc, Amsterdam
Issler N, Dufek S, Kleta R, Bockenhauer D, Smeulders N, Van’t Hoff W (2017) Epidemiology of paediatric renal stone disease: a 22-year single centre experience in the UK. BMC Nephrol 18:136. https://doi.org/10.1186/s12882-017-0505-x
Valavi E, Nickavar A, Aeene A (2019) Urinary metabolic abnormalities in children with idiopathic hematuria. J Pediatr Urol 15:165.e1–165.e4. https://doi.org/10.1016/j.jpurol.2018.11.003
Stojanović VD, Milosević BO, Djapić MB, Bubalo JD (2007) Idiopathic hypercalciuria associated with urinary tract infection in children. Pediatr Nephrol 22:1291–1295. https://doi.org/10.1007/s00467-007-0519-x
Vachvanichsanong P, Malagon M, Moore ES (2001) Urinary tract infection in children associated with idiopathic hypercalciuria. Scand J Urol Nephrol 35:112–116. https://doi.org/10.1080/003655901750170461
Scott P, Ouimet D, Valiquette L, Guay G, Proulx Y, Trouvé ML, Gagnon B, Bonnardeaux A (1999) Suggestive evidence for a susceptibility gene near the vitamin D receptor locus in idiopathic calcium stone formation. J Am Soc Nephrol 10:1007–1013
Vezzoli G, Tanini A, Ferrucci L, Soldati L, Bianchin C, Franceschelli F, Malentacchi C, Porfirio B, Adamo D, Terranegra A, Falchetti A, Cusi D, Bianchi G, Brandi ML (2002) Influence of calcium-sensing receptor gene on urinary calcium excretion in stone-forming patients. J Am Soc Nephrol 13:2517–2523. https://doi.org/10.1097/01.asn.0000030077.72157.d2
Vezzoli G, Terranegra A, Arcidiacono T, Biasion R, Coviello D, Syren ML, Paloschi V, Giannini S, Mignogna G, Rubinacci A, Ferraretto A, Cusi D, Bianchi G, Soldati L (2007) R990G polymorphism of calcium-sensing receptor does produce a gain-of-function and predispose to primary hypercalciuria. Kidney Int 71:1155–1162. https://doi.org/10.1038/sj.ki.5002156
Frick KK, Krieger NS, Bushinsky DA (2015) Modeling hypercalciuria in the genetic hypercalciuric stone-forming rat. Curr Opin Nephrol Hypertens 24:336–344. https://doi.org/10.1097/MNH.0000000000000130
Sforzini C, Milani D, Fossali E, Barbato A, Grumieri G, Bianchetti MG, Selicorni A (2002) Renal tract ultrasonography and calcium homeostasis in Williams-Beuren syndrome. Pediatr Nephrol 17:899–902. https://doi.org/10.1007/s00467-002-0889-z
Hawkes CP, Roy SM, Dekelbab B, Frazier B, Grover M, Haidet J, Listman J, Madsen S, Roan M, Rodd C, Sopher A, Tebben P, Levine MA (2020) Hypercalcemia in children using the ketogenic diet: a multicenter study. J Clin Endocrinol Metab. https://doi.org/10.1210/clinem/dgaa759
Han H, Segal AM, Seifter JL, Dwyer JT (2015) Nutritional management of kidney stones (nephrolithiasis). Clin Nutr Res 4:137–152. https://doi.org/10.7762/cnr.2015.4.3.137
Bao Y, Tu X, Wei Q (2020) Water for preventing urinary stones. Cochrane Database Syst Rev 2:CD004292. https://doi.org/10.1002/14651858.CD004292.pub4
Johnson RJ, Perez-Pozo SE, Lillo JL, Grases F, Schold JD, Kuwabara M, Sato Y, Hernando AA, Garcia G, Jensen T, Rivard C, Sanchez-Lozada LG, Roncal C, Lanaspa MA (2018) Fructose increases risk for kidney stones: potential role in metabolic syndrome and heat stress. BMC Nephrol 19:315. https://doi.org/10.1186/s12882-018-1105-0
Borghi L, Schianchi T, Meschi T, Guerra A, Allegri F, Maggiore U, Novarini A (2002) Comparison of two diets for the prevention of recurrent stones in idiopathic hypercalciuria. N Engl J Med 346:77–84. https://doi.org/10.1056/NEJMoa010369
Lin B-B, Lin M-E, Huang R-H, Hong Y-K, Lin B-L, He X-J (2020) Dietary and lifestyle factors for primary prevention of nephrolithiasis: a systematic review and meta-analysis. BMC Nephrol 21:26. https://doi.org/10.1186/s12882-020-01925-3
Phillips R, Hanchanale VS, Myatt A, Somani B, Nabi G, Biyani CS (2015) Citrate salts for preventing and treating calcium containing kidney stones in adults. Cochrane Database Syst Rev:CD010057. https://doi.org/10.1002/14651858.CD010057.pub2
Vigen R, Weideman RA, Reilly RF (2011) Thiazides diuretics in the treatment of nephrolithiasis: are we using them in an evidence-based fashion? Int Urol Nephrol 43:813–819. https://doi.org/10.1007/s11255-010-9824-6
Mortensen JT, Schultz A, Ostergaard AH (1986) Thiazides in the prophylactic treatment of recurrent idiopathic kidney stones. Int Urol Nephrol 18:265–269. https://doi.org/10.1007/BF02082712
Laerum E, Larsen S (1984) Thiazide prophylaxis of urolithiasis. A double-blind study in general practice. Acta Med Scand 215:383–389
Bendinelli B, Masala G, Garamella G, Palli D, Caini S (2019) Do thiazide diuretics increase the risk of skin cancer? A critical review of the scientific evidence and updated meta-analysis. Curr Cardiol Rep 21:92. https://doi.org/10.1007/s11886-019-1183-z
Choi JN, Lee JS, Shin JI (2011) Low-dose thiazide diuretics in children with idiopathic renal hypercalciuria. Acta Paediatr 100:e71–e74. https://doi.org/10.1111/j.1651-2227.2011.02191.x
Alexander RT, McArthur E, Jandoc R, Welk B, Fuster DG, Garg AX, Quinn RR (2018) Thiazide diuretic dose and risk of kidney stones in older adults: a retrospective cohort study. Can J Kidney Health Dis 5:2054358118787480. https://doi.org/10.1177/2054358118787480
Funding
ML Downie is funded by the Canadian Kidney Research Scientist and Core Education Training Program (KRESCENT) as well as the St. Peter’s Trust for Kidney, Bladder & Prostate Research. Research in the Alexander laboratory is funded by grants from the Women and Children’s Health Research Institute, which is supported by the Stollery Children’s Hospital Foundation, the Canadian Institutes of Health Research, the Kidney Foundation of Canada and the National Sciences and Engineering Research Council of Canada. Dr. Alexander is a Stollery Science laboratory Distinguished Researcher and the Canada Research Chair in Renal Epithelial Transport Physiology.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Dr. Alexander has received consulting fees or honoraria from Ardylex, Ultragenyx and Advicenne. Dr. Downie has no conflicts to declare.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Downie, M.L., Alexander, R.T. Molecular mechanisms altering tubular calcium reabsorption. Pediatr Nephrol 37, 707–718 (2022). https://doi.org/10.1007/s00467-021-05049-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-021-05049-0