Abstract
Background
Mechanical Thrombectomy (MT) has improved outcomes in acute ischemic stroke (AIS) due to Large Vessel Obstruction (LVO). However, there is limited data on the safety and outcomes of MT in AIS patients with thrombocytopenia. This study aims to assess the efficacy and safety of MT in this population.
Methods
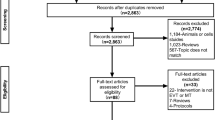
Following the PRISMA guidelines, a comprehensive systematic review was conducted using PubMed, Embase, Web of Science, and Scopus. Studies meeting inclusion criteria underwent rigorous risk of bias assessment using the ROBINS-I tool. We compared outcomes between patients with and without thrombocytopenia undergoing MT. Using the R software version 4.3.1, meta-analyses were conducted employing random-effect models.
Results
This meta-analysis encompassed data from 5 studies. Thrombocytopenic AIS patients who underwent MT (n = 974) exhibited lower rates of functional independence (OR 0.83, 95% CI 0.71–0.98; p = 0.030) compared to patients with normal platelet counts (n = 2036). In addition, the thrombocytopenic group experienced higher mortality as compared to the group with normal platelet counts (OR 1.76, 95% CI 1.26–2.45; p < 0.001). Rates of sICH were found to be similar between groups (OR 1.20, 95% CI 0.74–1.93; p = 0.456), as were rates of successful recanalization (OR 0.94, 95% CI 0.47–1.87; p = 0.863). Lastly, no significant differences were observed in procedure times between thrombocytopenic and non-thrombocytopenic groups.
Conclusion
As compared to patients without thrombocytopenia, thrombocytopenic AIS patients undergoing MT displayed lower functional independence and higher mortality rates, with no significant differences in sICH or successful recanalization.






Similar content being viewed by others
References
Al-Mufti F et al (2022) Thrombectomy in special populations: report of the society of neurointerventional surgery standards and guidelines committee. J NeuroInterv Surg 14(10):1033–1041
Mönch S et al (2019) Thrombocytopenia and declines in platelet counts: predictors of mortality and outcome after mechanical thrombectomy. J Neurol 266:1588–1595
Wang TY et al (2009) Incidence and prognostic significance of thrombocytopenia developed during acute coronary syndrome in contemporary clinical practice. Circulation 119(18):2454–2462
Desai SM et al (2019) Endovascular thrombectomy, platelet count, and intracranial hemorrhage. World Neurosurg 127:e1039–e1043
Higgins J et al (2020) Cochrane handbook for systematic reviews of interventions version 60, 2019. The cochrane collaboration: cochrane. Wiley, pp 261–262
Cappellari M et al (2020) Direct thrombectomy for stroke in the presence of absolute exclusion criteria for thrombolysis. J Neurol 267:3731–3740
Ždraljević M et al (2022) Influence of thrombocytopenia on the outcome of mechanical thrombectomy in patients with acute ischemic stroke. J Stroke Cerebrovasc Dis 31(2):106240
Fujiwara S et al (2023) Impact of thrombocytopenia on hemorrhagic complications after endovascular therapy for acute large vessel occlusion: sub-analysis of RESCUE-Japan registry 2. J Neurol Sci 449:120659
Nogueira RG, Smith WS (2009) Safety and efficacy of endovascular thrombectomy in patients with abnormal hemostasis: pooled analysis of the MERCI and multi MERCI trials. Stroke 40(2):516–522
Lin C et al (2021) Fibrinogen level combined with platelet count for predicting hemorrhagic transformation in acute ischemic stroke patients treated with mechanical thrombectomy. Front Neurol 12:716020
Tohgi H et al (1991) Platelet volume, aggregation, and adenosine triphosphate release in cerebral thrombosis. Stroke 22(1):17–21
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
R.K. has the following conflicts: Research support from: Cerenovus Inc, Medtronic, Endovascular Engineering, Frontior Bio, Sensome Inc, Endomimetics, Ancure LLC, Neurogami Medical, MIVI Biosciences, Monarch Biosciences, Stryker Inc, Conway Medical, Pireus Medical, and Bionau Labs outside the submitted work. He holds the following research grants Research Grants: NIH (R01NS076491, R44NS107111, R43NS110114 and R21NS128199) and NSF (081215707) outside the submitted work. AAR serving on advisory boards for AstraZeneca, Novo Nordisk, and Boston Scientific outside the submitted work. D.F.K. holds equity in Nested Knowledge, Superior Medical Editors, and Conway Medical, Marblehead Medical and Piraeus Medical. He receives grant support from MicroVention, Medtronic, Balt, and Insera Therapeutics; has served on the Data Safety Monitoring Board for Vesalio; and received royalties from Medtronicoutside the submitted work.
Ethics approval
Ethics approval was not required for this study.
Informed consent
Informed consent was not required for this study.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Toruno, M.A., Al-Janabi, O.M., Ghozy, S. et al. Outcomes of mechanical thrombectomy in patients with acute ischemic stroke and thrombocytopenia: systematic review and meta-analysis. J Neurol (2024). https://doi.org/10.1007/s00415-024-12363-8
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00415-024-12363-8