Abstract
Objectives
To correlate contrast-enhanced ultrasound (CEUS) kinetic parameters with traditional and molecular prognostic factors in invasive breast cancer.
Methods
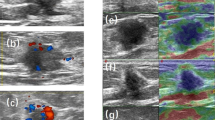
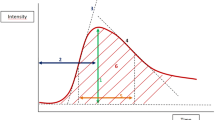
Seventy-five invasive breast cancers were evaluated with contrast harmonic imaging after the injection of a bolus dose of 2.4 ml sulphur hexafluoride microbubble contrast agent. The lognormal function was used for quantitative analysis of kinetic data. These parameters correlated with traditional prognostic factors (tumour size, histological type, tumour grade, axillary lymph node status) and immunohistochemical biomarkers (ER, PR and HER2 status).
Results
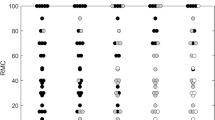
Statistically significant correlation was found between time-to-peak and tumour grade (P value = 0.023), PR status (P value = 0.042) and axillary node status (P value = 0.025). Wash-out ratio, measured at 21 s was significantly associated with ER status (P value = 0.042) and PR status (P value = 0.026).
Conclusions
Invasive breast carcinomas exhibiting earlier peak enhancement and faster elimination of microbubble contrast agent at CEUS are found to be associated with established predictors of poor prognosis.
Key Points
• Contrast-enhanced ultrasound (CEUS) can potentially determine the aggressiveness of invasive breast cancers.
• Early peak enhancement and accelerated wash-out at CEUS suggest poor prognosis.
• CEUS kinetics are similar to that of DCE-MRI in assessing tumour aggressiveness.




Similar content being viewed by others
References
Skaane P, Sager EM, Olsen JB et al (1999) Diagnostic value of ultrasonography in patients with palpable mammographically noncalcified breast tumors. Acta Radiol 40:163–168
Kedar RP, Cosgrove D, McCready VR, Bamber JC, Carter ER (1996) Microbubble contrast agent for color Doppler US: effect on breast masses. Work in progress. Radiology 198:679–686
Delorme S, Krix M (2006) Contrast-enhanced ultrasound for examining tumor biology. Cancer Imaging 6:148–152
Cuenod CA, Fournier L, Balvay D, Guinebretière J (2006) Tumor angiogenesis: pathophysiology and implications for contrast-enhanced MRI and CT assessment. Abdom Imaging 31:188–193
Lee T, Purdie TG, Stewart E (2003) CT imaging of angiogenesis. Q J Nucl Med 47:171–187
Griebel J, Mayr NA, de Vries A et al (1997) Assessment of tumor microcirculation: a new role of dynamic contrast MR imaging. J Magn Reson Imaging 7:111–119
Anderson H, Price P, Blomley M, Leach MO, Workman P, Cancer Research Campaign PK/PD Technologies Advisory Committee (2001) Measuring changes in human tumour vasculature in response to therapy using functional imaging techniques. Br J Cancer 85:1085–1093
Balleyguier C, Opolon P, Mathieu MC et al (2009) New potential and applications of contrast-enhanced ultrasound of the breast: own investigations and review of the literature. Eur J Radiol 69:14–23
Hwang M, Niermann KJ, Lyshchik A, Fleischer AC (2009) Sonographic assessment of tumor response: from in vivo models to clinical applications. Ultrasound Q 25:175–183
Szabó BK, Aspelin P, Kristoffersen Wiberg M, Tot T, Boné B (2003) Invasive breast cancer: correlation of dynamic MR features with prognostic factors. Eur Radiol 13:2425–2435
Chang Y, Kwon KH, Choi DL et al (2009) Magnetic resonance imaging of breast cancer and correlation with prognostic factors. Acta Radiol 50:990–998
D’Onofrio M, Zamboni GA, Malagò R et al (2009) Resectable pancreatic adenocarcinoma: is the enhancement pattern at contrast-enhanced ultrasonography a pre-operative prognostic factor? Ultrasound Med Biol 35:1929–1937
Massironi S, Conte D, Sciola V et al (2010) Contrast-enhanced ultrasonography in evaluating hepatic metastases from neuroendocrine tumours. Dig Liver Dis 42:635–641
Ouyang Q, Chen L, Zhao H, Xu R, Lin Q (2010) Detecting metastasis of lymph nodes and predicting aggressiveness in patients with breast carcinomas. J Ultrasound Med 29:343–352
Strouthos C, Lampaskis M, Sboros V, McNeilly A, Averkiou M (2010) Indicator dilution models for the quantification of microvascular blood flow with bolus administration of ultrasound contrast agents. IEEE Trans Ultrason Ferroelectr Freq Control 57:1296–1310
Saracco A, Szabo B, Aspelin P et al (2012) Differentiation between benign and malignant breast tumors using kinetic features of real-time harmonic contrast-enhanced ultrasound. Acta Radiol 53:382–388
Shah SS, Ketterling RP, Goetz MP et al (2010) Impact of American Society of Clinical Oncology/College of American Pathologists guideline recommendations on HER2 interpretation in breast cancer. Hum Pathol 41:103–106
Carmeliet P (2005) Angiogenesis in life, disease and medicine. Nature 438:932–936
Folkman J (1971) Tumor angiogenesis: therapeutic implications. N Engl J Med 285:1182–1186
Mann RM, Kuhl CK, Kinkel K, Boetes C (2008) Breast MRI: guidelines from the European Society of Breast Imaging. Eur Radiol 18:1307–1318
Kuhl CK (2000) MRI of breast tumors. Eur Radiol 10:46–58
Kuhl CK, Mielcareck P, Klaschik S et al (1999) Dynamic breast MR imaging: are signal intensity time course data useful for differential diagnosis of enhancing lesions? Radiology 211:101–110
Caproni N, Marchisio F, Pecchi A et al (2010) Contrast-enhanced ultrasound in the characterisation of breast masses: utility of quantitative analysis in comparison with MRI. Eur Radiol 20:1384–1395
Zhao H, Xu R, Ouyang Q, Chen L, Dong B, Huihua Y (2010) Contrast-enhanced ultrasound is helpful in the differentiation of malignant and benign breast lesions. Eur J Radiol 73:288–293
Uzzan B, Nicolas P, Cucherat M, Perret G (2004) Microvessel density as a prognostic factor in women with breast cancer: a systematic review of the literature and meta-analysis. Cancer Res 64:2941–2955
Delli Carpini J, Carpini JD, Karam AK, Montgomery L (2010) Vascular endothelial growth factor and its relationship to the prognosis and treatment of breast, ovarian, and cervical cancer. Angiogenesis 13:43–58
Knopp MV, Weiss E, Sinn HP et al (1999) Pathophysiologic basis of contrast enhancement in breast tumors. J Magn Reson Imaging 10:260–266
Frouge C, Guinebretière JM, Contesso G, Di Paola R, Bléry M (1994) Correlation between contrast enhancement in dynamic magnetic resonance imaging of the breast and tumor angiogenesis. Invest Radiol 29:1043–1049
Buadu LD, Murakami J, Murayama S et al (1996) Breast lesions: correlation of contrast medium enhancement patterns on MR images with histopathologic findings and tumor angiogenesis. Radiology 200:639–649
Boné B, Szabó BK, Perbeck LG, Veress B, Aspelin P (2003) Can contrast-enhanced MR imaging predict survival in breast cancer? Acta Radiol 44:373–378
Pickles MD, Manton DJ, Lowry M, Turnbull LW (2009) Prognostic value of pre-treatment DCE-MRI parameters in predicting disease free and overall survival for breast cancer patients undergoing neoadjuvant chemotherapy. Eur J Radiol 71:498–505
Du J, Li F, Fang H, Xia J, Zhu C (2008) Correlation of real-time gray scale contrast-enhanced ultrasonography with microvessel density and vascular endothelial growth factor expression for assessment of angiogenesis in breast lesions. J Ultrasound Med 27:821–831
Acknowledgements
Dr. Saracco has received honoraria from Philips for lectures on contrast-enhanced ultrasound.
There is an overlap in patient cohort with an already published paper: Saracco A, Szabó BK, Aspelin P, Leifland K, Wilczek B, Celebioglu F, Axelsson R (2012) Differentiation between benign and malignant breast tumors using kinetic features of real-time harmonic contrast-enhanced ultrasound. Acta Radiol 53:382-388.
The aims and methods of the two papers are different, and there is an overlap in 75 malignant tumours. The CEUS kinetics were analysed with a more advanced mathematical modelling, and we correlated CEUS enhancement kinetics with prognostic factors in the recent study, whereas the purpose of the already published paper was to find out whether CEUS kinetics are able to differentiate between benign and malignant tumours.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Szabó, B.K., Saracco, A., Tánczos, E. et al. Correlation of contrast-enhanced ultrasound kinetics with prognostic factors in invasive breast cancer. Eur Radiol 23, 3228–3236 (2013). https://doi.org/10.1007/s00330-013-2960-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-013-2960-5