Abstract
Purpose
To retrospectively analyse complications in endovascular aortic repair (EVAR) interventions and evaluate if the CIRSE (Cardiovascular and Interventional Radiological Society of Europe) complication classification system is appropriate as a standardized classification tool for EVAR patients.
Materials and Methods
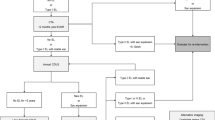
Demographic, procedural and complication data in 719 consecutive patients undergoing EVAR at one institution from January 2014 to October 2019 were retrospectively reviewed. Data (imaging reports, procedural reports, nurse notes, discharge summary reports) were collected consulting the electronic patient record system (EPR) of the hospital and cleaned and stored in a Microsoft Excel database. All the procedures were analysed in consensus by two interventional radiology consultants and a resident radiologist and if an intra- , peri- or post-procedural complication occurred, a grade (1–6) was assigned using the CIRSE grading complication classification system.
Results
Twenty-five patients were excluded from the analysis because of invalid or incomplete data. The final population was made up of 694 patients (mean age 75,4 y.o., 616 male/78 female, min age 23 y.o., max age 97 y.o.). Complications emerged in 211 patients (30,4% of cases, 22 female/189 male). The number of patients with CIRSE grade I, II, III, IV, V and VI complications was 36 (17%), 17 (8%), 121 (57,3%), 15 (7,1%), 3 (1,4%), 19 (9%). Nineteen (2,6%) patients succumbed after EVAR. Thirty-four complications (16,1%) were related to vascular access.
Conclusion
The CIRSE complication classification system represents a broadly applicable and feasible approach to evaluate the severity of complications in patients following EVAR. However, some deficit may be considered relevant and as starting standing-point for future improvements.







Similar content being viewed by others
References
Clavien PA, Barkun J, de Oliveira ML, et al. The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg. 2009;250(2):187–96. https://doi.org/10.1097/SLA.0b013e3181b13ca2 (PMID: 19638912).
Gradinscak DJ, Young N, Jones Y, et al. Risks of outpatient angiography and interventional procedures: a prospective study. AJR Am J Roentgenol. 2004;183(2):377–81. https://doi.org/10.2214/ajr.183.2.1830377 (PMID: 15269028).
Noori VJ, Healey CT, Eldrup-Jorgensen J, et al. Comparison of major adverse event rates after elective endovascular aneurysm repair in New England using a novel measure of complication severity. J Vasc Surg. 2019;70(1):74–9. https://doi.org/10.1016/j.jvs.2018.10.055 (Epub 2018 Dec 28 PMID: 30598356).
Martin II RC, Brennan MF, Jaques DP. Quality of complication reporting in the surgical literature. Ann Surg. 2002;235(6):803–13. https://doi.org/10.1097/00000658-200206000-00007 (PMID: 12035036; PMCID: PMC1422509).
Strasberg SM, Linehan DC, Hawkins WG. The accordion severity grading system of surgical complications. Ann Surg. 2009;250(2):177–86. https://doi.org/10.1097/SLA.0b013e3181afde41 (PMID: 19638919).
Hay JL, Atkinson TM, Reeve BB, et al. NCI PRO-CTCAE Study group. Cognitive interviewing of the US national cancer institute’s patient-reported outcomes version of the common terminology criteria for adverse events (PRO-CTCAE). Qual Life Res. 2014;23(1):257–69. https://doi.org/10.1007/s11136-013-0470-1 (Epub 2013 Jul 20. PMID: 23868457; PMCID: PMC3896507).
Khuri SF, Daley J, Henderson W, et al. The department of veterans affairs’ NSQIP: the first national, validated, outcome-based, risk-adjusted, and peer-controlled program for the measurement and enhancement of the quality of surgical care. National VA surgical quality improvement program. Ann Surg. 1998;228(4):491–507. https://doi.org/10.1097/00000658-199810000-00006 (PMID: 9790339; PMCID: PMC1191523).
Khalilzadeh O, Baerlocher MO, Shyn PB, et al. Proposal of a new adverse event classification by the society of interventional radiology standards of practice committeel. J Vasc Interv Radiol. 2017;28(10):1432-7.e3. https://doi.org/10.1016/j.jvir.2017.06.019 (Epub 2017 Jul 27. Erratum in: J Vasc Interv Radiol. 2018 Jan;29(1):146. PMID: 28757285).
Filippiadis DK, Binkert C, Pellerin O, et al. Cirse quality assurance document and standards for classification of complications: the cirse classification system. Cardiovasc Intervent Radiol. 2017;40(8):1141–6. https://doi.org/10.1007/s00270-017-1703-4 (Epub 2017 Jun 5 PMID: 28584945).
Lee WA, Brown MP, Nelson PR, Huber TS. Total percutaneous access for endovascular aortic aneurysm repair (“preclose” technique). J Vasc Surg. 2007;45(6):1095–101. https://doi.org/10.1016/j.jvs.2007.01.050 (Epub 2007 Mar 29 PMID: 17398056).
Moll F, Powell J, Fraedrich G, et al. Management of abdominal aortic aneurysms clinical practice guidelines of the European Society for Vascular Surgery. Eur J Vasc Endovasc Surg. 2011;41(Suppl 1):S1-58. https://doi.org/10.1016/j.ejvs.2010.09.011 (PMID: 21215940).
Seely AJ, Ivanovic J, Threader J, et al. Systematic classification of morbidity and mortality after thoracic surgery. Ann Thorac Surg. 2010;90(3):936–42. https://doi.org/10.1016/j.athoracsur.2010.05.014 (PMID: 20732521).
De Bruin JL, Baas AF, Buth J, et al. Long-term outcome of open or endovascular repair of abdominal aortic aneurysm. N Engl J Med. 2010;362(20):1881–9. https://doi.org/10.1056/NEJMoa0909499 (PMID: 20484396).
Nordon IM, Karthikesalingam A, Hinchliffe RJ, et al. Secondary interventions following endovascular aneurysm repair (EVAR) and the enduring value of graft surveillance. Eur J Vasc Endovasc Surg. 2010;39(5):547–54. https://doi.org/10.1016/j.ejvs.2009.11.002 (Epub 2009 Nov 25 PMID: 19939711).
Baderkhan H, et al. Detection of late complications after endovascular abdominal aortic aneurysm repair and implications for follow up based on retrospective assessment of a two centre cohort. Eur J Vasc Endovasc Surg. 2020;60(2):171–9. https://doi.org/10.1016/j.ejvs.2020.02.021 (Epub 2020 Mar 21 PMID: 32209282).
Chaikof EL, Dalman RL, Eskandari MK, et al. The society for vascular surgery practice guidelines on the care of patients with an abdominal aortic aneurysm. J Vasc Surg. 2018;67(1):2-77.e2. https://doi.org/10.1016/j.jvs.2017.10.044 (PMID: 29268916).
Stather PW, Sidloff D, Dattani N, et al. Systematic review and meta-analysis of the early and late outcomes of open and endovascular repair of abdominal aortic aneurysm. Br J Surg. 2013;100(7):863–72. https://doi.org/10.1002/bjs.9101 (Epub 2013 Mar 8 PMID: 23475697).
Fonseca R, Rockman C, Pitti A, et al. Intermediate-term EVAR outcomes in octogenarians. J Vasc Surg. 2010;52(3):556–60. https://doi.org/10.1016/j.jvs.2010.03.051.
Rueda-Ochoa OL, van Bakel P, Hoeks SE, et al. Survival After uncomplicated EVAR in octogenarians is similar to the general population of octogenarians without an abdominal aortic aneurysm. Eur J Vasc Endovasc Surg. 2020;59(5):740–7. https://doi.org/10.1016/j.ejvs.2020.01.026 (Epub 2020 Feb 27 PMID: 32115359).
Murray D, Ghosh J, Khwaja N, et al. Access for endovascular aneurysm repair. J Endovasc Ther. 2006;13(6):754–61. https://doi.org/10.1583/06-1835.1 (PMID: 17154706).
Vatakencherry G, Molloy C, Sheth N, Liao M, Lam CK. Percutaneous access planning, techniques and considerations for endovascular aortic repair (EVAR). Cardiovasc Diagn Ther. 2018;8(Suppl 1):S184-90. https://doi.org/10.21037/cdt.2018.03.06.PMID:29850430;PMCID:PMC5949597.
Dwivedi K, Regi JM, Cleveland TJ, et al. Long-term evaluation of percutaneous groin access for EVAR. Cardiovasc Intervent Radiol. 2019;1:28–33. https://doi.org/10.1007/s00270-018-2072-3 (Epub 2018 Oct 4. PMID: 30288590; PMCID: PMC6267668).
Acknowledgements
These data were submitted as a manuscript and accepted for CIRSE 2020 in September
Funding
This study was not supported by any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Consent for Publication
Consent for publication was obtained for every individual person’s data included in the study.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this type of study, formal consent is not required.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Castiglione, D., Easwaran, A., Prashar, A. et al. Assessment of EVAR Complications using CIRSE Complication Classification System in the UK Tertiary Referral Centre: A ∼6-Year Retrospective Analysis (2014–2019). Cardiovasc Intervent Radiol 44, 1174–1183 (2021). https://doi.org/10.1007/s00270-021-02847-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-021-02847-9