Abstract
Purpose
Previous studies have indicated disrupted functional connectivity in multiple brain regions and resting-state networks in episodic migraine, but it is unclear how brain network property is disrupted in chronic migraine.
Methods
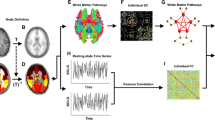
Using resting-state functional magnetic resonance imaging and voxel-wise functional connectivity density analysis, we examined the large-scale functional connectivity pattern over the whole brain in 17 patients with chronic migraine without medication overuse compared to 35 healthy controls. The associations between functional connectivity density and clinical variables were also explored.
Results
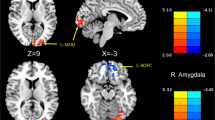
Compared with controls, chronic migraine patients showed decreased local and distant functional connectivity density in the dorsolateral and medial prefrontal cortexes and precuneus and increased local and distant functional connectivity density in the hippocampal complex. The patients also presented increased local functional connectivity density in the orbital frontal gyrus and cerebellum and increased distant functional connectivity density in the temporal pole. Moreover, local functional connectivity density in several brain regions, such as the left superior temporal gyrus and dorsal anterior cingulate cortex, was found to be correlated with headache frequency or pain intensity.
Conclusion
Chronic migraine is associated with functional connectivity alterations in regions involved in multisensory integration, affective and cognitive processing, and pain modulation. Both local and distant functional connectivity density are complementary biomarkers for investigating the neural mechanism of this disorder. Some local functional connectivity density alterations may be useful for assessing the disease burden of chronic migraine.




Similar content being viewed by others
References
Headache Classification Committee of International Headache Society (2013) The international classification of headache disorders, 3rd edition (beta version). Cephalalgia 33:629–808
Buse DC, Manack A, Serrano D, Turkel C, Lipton RB (2010) Sociodemographic and comorbidity profiles of chronic migraine and episodic migraine sufferers. J Neurol Neurosurg Psychiatry 81:428–432
Schulte LH, Allers A, May A (2017) Hypothalamus as a mediator of chronic migraine: evidence from high-resolution fMRI. Neurology 88:2011–2016
Schulte LH, Allers A, May A (2018) Visual stimulation leads to activation of the nociceptive trigeminal nucleus in chronic migraine. Neurology 90:e1973–e1978
Androulakis XM, Krebs K, Peterlin BL, Zhang T, Maleki N, Sen S, Rorden C, Herath P (2017) Modulation of intrinsic resting-state fMRI networks in women with chronic migraine. Neurology 89:163–169
Coppola G, Di Renzo A, Petolicchio B, Tinelli E, Di Lorenzo C, Parisi V, Serrao M, Calistri V, Tardioli S, Cartocci G, Schoenen J, Caramia F, Di Piero V, Pierelli F (2019) Aberrant interactions of cortical networks in chronic migraine: a resting-state fMRI study. Neurology 92:e2550–e2558
Filippi M, Messina R (2019) The chronic migraine brain: what have we learned from neuroimaging? Front Neurol 10:1356
Schwedt TJ, Schlaggar BL, Mar S, Nolan T, Coalson RS, Nardos B, Benzinger T, Larson-Prior LJ (2013) Atypical resting-state functional connectivity of affective pain regions in chronic migraine. Headache 53:737–751
Chen Z, Chen X, Liu M, Dong Z, Ma L, Yu S (2017) Altered functional connectivity of amygdala underlying the neuromechanism of migraine pathogenesis. J Headache Pain 18:7
Chen Z, Chen X, Liu M, Ma L, Yu S (2019) Volume of hypothalamus as a diagnostic biomarker of chronic migraine. Front Neurol 10:606
Coppola G, Di Renzo A, Petolicchio B, Tinelli E, Di Lorenzo C, Serrao M, Calistri V, Tardioli S, Cartocci G, Parisi V, Caramia F, Di Piero V, Pierelli F (2020) Increased neural connectivity between the hypothalamus and cortical resting-state functional networks in chronic migraine. J Neurol 267:185–191
Chen Z, Chen X, Liu M, Liu S, Shu S, Ma L, Yu S (2016) Altered functional connectivity of the marginal division in migraine: a resting-state fMRI study. J Headache Pain 17:89
Lee MJ, Park BY, Cho S, Kim ST, Park H, Chung CS (2019) Increased connectivity of pain matrix in chronic migraine: a resting-state functional MRI study. J Headache Pain 20:29
Tomasi D, Volkow ND (2010) Functional connectivity density mapping. Proc Natl Acad Sci U S A 107:9885–9890
Huskisson EC (1974) Measurement of pain. Lancet 2:1127–1131
Jensen MP, Turner JA, Romano JM, Fisher LD (1999) Comparative reliability and validity of chronic pain intensity measures. Pain 83:157–162
Beucke JC, Sepulcre J, Talukdar T, Linnman C, Zschenderlein K, Endrass T, Kaufmann C, Kathmann N (2013) Abnormally high degree connectivity of the orbitofrontal cortex in obsessive-compulsive disorder. JAMA psychiatry 70:619–629
Chen Z, Chen X, Liu M, Dong Z, Ma L, Yu S (2017) Altered functional connectivity architecture of the brain in medication overuse headache using resting state fMRI. J Headache Pain 18:25
Tomasi D, Volkow ND (2012) Aging and functional brain networks. Mol Psychiatry 17(471):549–458
Tomasi D, Wang GJ, Volkow ND (2013) Energetic cost of brain functional connectivity. Proc Natl Acad Sci U S A 110:13642–13647
Sepulcre J, Liu H, Talukdar T, Martincorena I, Yeo BT, Buckner RL (2010) The organization of local and distant functional connectivity in the human brain. PLoS Comput Biol 6:e1000808
Petrovic P, Kalso E, Petersson KM, Ingvar M (2002) Placebo and opioid analgesia-- imaging a shared neuronal network. Science 295:1737–1740
Wiech K, Ploner M, Tracey I (2008) Neurocognitive aspects of pain perception. Trends Cogn Sci 12:306–313
Buckner RL, Andrews-Hanna JR, Schacter DL (2008) The brain’s default network: anatomy, function, and relevance to disease. Ann N Y Acad Sci 1124:1–38
Alshelh Z, Marciszewski KK, Akhter R, Di Pietro F, Mills EP, Vickers ER, Peck CC, Murray GM, Henderson LA (2018) Disruption of default mode network dynamics in acute and chronic pain states. Neuroimage Clin 17:222–231
Dai Z, Zhong J, Xiao P, Zhu Y, Chen F, Pan P, Shi H (2015) Gray matter correlates of migraine and gender effect: a meta-analysis of voxel-based morphometry studies. Neuroscience 299:88–96
Zou Y, Tang W, Li X, Xu M, Li J (2019) Acupuncture reversible effects on altered default mode network of chronic migraine accompanied with clinical symptom relief. Neural Plast 2019:5047463
Chen Z, Chen X, Liu M, Liu S, Ma L, Yu S (2017) Disrupted functional connectivity of periaqueductal gray subregions in episodic migraine. J Headache Pain 18:36
Huang X, Zhang D, Chen Y, Wang P, Mao C, Miao Z, Liu C, Xu C, Wu X, Yin X (2019) Altered functional connectivity of the red nucleus and substantia nigra in migraine without aura. J Headache Pain 20:104
Moulton EA, Elman I, Pendse G, Schmahmann J, Becerra L, Borsook D (2011) Aversion-related circuitry in the cerebellum: responses to noxious heat and unpleasant images. J Neurosci 31:3795–3804
Ruscheweyh R, Kühnel M, Filippopulos F, Blum B, Eggert T, Straube A (2014) Altered experimental pain perception after cerebellar infarction. Pain 155:1303–1312
Mehnert J, May A (2019) Functional and structural alterations in the migraine cerebellum. J Cereb Blood Flow Metab 39:730–739
Koppen H, Boele HJ, Palm-Meinders IH, Koutstaal BJ, Horlings CG, Koekkoek BK, van der Geest J, Smit AE, van Buchem MA, Launer LJ, Terwindt GM, Bloem BR, Kruit MC, Ferrari MD, De Zeeuw CI (2017) Cerebellar function and ischemic brain lesions in migraine patients from the general population. Cephalalgia 37:177–190
Kringelbach ML (2005) The human orbitofrontal cortex: linking reward to hedonic experience. Nat Rev Neurosci 6:691–702
Elliott R, Dolan RJ, Frith CD (2000) Dissociable functions in the medial and lateral orbitofrontal cortex: evidence from human neuroimaging studies. Cereb Cortex 10:308–317
Leknes S, Tracey I (2008) A common neurobiology for pain and pleasure. Nat Rev Neurosci 9:314–320
Li Z, Zeng F, Yin T, Lan L, Makris N, Jorgenson K, Guo T, Wu F, Gao Y, Dong M, Liu M, Yang J, Li Y, Gong Q, Liang F, Kong J (2017) Acupuncture modulates the abnormal brainstem activity in migraine without aura patients. Neuroimage Clin 15:367–375
Fumal A, Laureys S, Di Clemente L, Boly M, Bohotin V, Vandenheede M, Coppola G, Salmon E, Kupers R, Schoenen J (2006) Orbitofrontal cortex involvement in chronic analgesic-overuse headache evolving from episodic migraine. Brain 129:543–550
Riederer F, Gantenbein AR, Marti M, Luechinger R, Kollias S, Sándor PS (2013) Decrease of gray matter volume in the midbrain is associated with treatment response in medication-overuse headache: possible influence of orbitofrontal cortex. J Neurosci 33:15343–15349
Bilgiç B, Kocaman G, Arslan AB, Noyan H, Sherifov R, Alkan A, Asil T, Parman Y, Baykan B (2016) Volumetric differences suggest involvement of cerebellum and brainstem in chronic migraine. Cephalalgia 36:301–308
Coppola G, Petolicchio B, Di Renzo A, Tinelli E, Di Lorenzo C, Parisi V, Serrao M, Calistri V, Tardioli S, Cartocci G, Ambrosini A, Caramia F, Di Piero V, Pierelli F (2017) Cerebral gray matter volume in patients with chronic migraine: correlations with clinical features. J Headache Pain 18:115
DeSouza DD, Woldeamanuel YW, Sanjanwala BM, Bissell DA, Bishop JH, Peretz A, Cowan RP (2020) Altered structural brain network topology in chronic migraine. Brain Struct Funct 225:161–172
Liu MG, Chen J (2009) Roles of the hippocampal formation in pain information processing. Neurosci Bull 25:237–266
Vachon-Presseau E, Roy M, Martel MO, Caron E, Marin MF, Chen J, Albouy G, Plante I, Sullivan MJ, Lupien SJ, Rainville P (2013) The stress model of chronic pain: evidence from basal cortisol and hippocampal structure and function in humans. Brain 136:815–827
Liu HY, Chou KH, Lee PL, Fuh JL, Niddam DM, Lai KL, Hsiao FJ, Lin YY, Chen WT, Wang SJ, Lin CP (2017) Hippocampus and amygdala volume in relation to migraine frequency and prognosis. Cephalalgia 37:1329–1336
Liu J, Ma S, Mu J, Chen T, Xu Q, Dun W, Tian J, Zhang M (2017) Integration of white matter network is associated with interindividual differences in psychologically mediated placebo response in migraine patients. Hum Brain Mapp 38:5250–5259
Moulton EA, Becerra L, Maleki N, Pendse G, Tully S, Hargreaves R, Burstein R, Borsook D (2011) Painful heat reveals hyperexcitability of the temporal pole in interictal and ictal migraine states. Cereb Cortex 21:435–448
Neeb L, Bastian K, Villringer K, Israel H, Reuter U, Fiebach JB (2017) Structural gray matter alterations in chronic migraine: implications for a progressive disease? Headache 57:400–416
Hubbard CS, Khan SA, Keaser ML, Mathur VA, Goyal M, Seminowicz DA (2014) Altered brain structure and function correlate with disease severity and pain catastrophizing in migraine patients. eNeuro 1(e20):14
Seeley WW, Menon V, Schatzberg AF, Keller J, Glover GH, Kenna H, Reiss AL, Greicius MD (2007) Dissociable intrinsic connectivity networks for salience processing and executive control. J Neurosci 27:2349–2356
Funding
This study was supported by the National Nature Science Foundation of China (grant numbers 81701669, 81701667, and 81701679), the Nature Science Foundation of Jiangsu Province (grant numbers BK20170368 and BK20170367), the Natural Science Foundation of Tianjin (19JCQNJC09800), and the Scientific Research Program of Jiangsu Provincial Health and Family Planning Commission (H201621).
Author information
Authors and Affiliations
Contributions
Study design: Jun Ke. Literature research: Hui Dai and Chunhong Hu. Data acquisition: Ximing Wang, Su Hu, and Hongru Zhao. Data processing and statistical analysis: Xiaodong Zhang and Yunyan Su. Data interpretation: Lingling Dai, Yang Yu, and Hongru Zhao. Manuscript preparation: Lingling Dai and Yang Yu. Manuscript editing: Lingling Dai, Yang Yu, Hongru Zhao, Xiaodong Zhang, Yunyan Su, Ximing Wang, Su Hu, Hui Dai, Chunhong Hu, and Jun Ke. Funding acquisition: Jun Ke, Yunyan Su, Xiaodong Zhang, and Ximing Wang. Manuscript final version approval: Lingling Dai, Yang Yu, Hongru Zhao, Xiaodong Zhang, Yunyan Su, Ximing Wang, Su Hu, Hui Dai, Chunhong Hu, and Jun Ke.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study protocol was in accordance with the Declaration of Helsinki and was approved by the ethics committee of the First Affiliated Hospital of Soochow University.
Informed consent
All participants provided written informed consent.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dai, L., Yu, Y., Zhao, H. et al. Altered local and distant functional connectivity density in chronic migraine: a resting-state functional MRI study. Neuroradiology 63, 555–562 (2021). https://doi.org/10.1007/s00234-020-02582-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-020-02582-x