Abstract
Background
The safety and efficacy of tirofiban for patients with acute ischemic stroke (AIS) remains controversial. We therefore conducted a systematic review and meta-analysis.
Methods
We searched PubMed, EMBASE, Cochrane Library, Web of Science, and related international clinical trials registries through March 31, 2019, using the terms “tirofiban” and “stroke”. All apparently unconfounded randomized controlled trials (RCTs) and cohort studies with two arms comparing treatment with and without tirofiban for AIS were included in this review. Primary outcomes included symptomatic intracranial hemorrhage (sICH), fatal ICH, mortality, and modified Rankin Scale (mRS 0–2) at 3 months.
Results
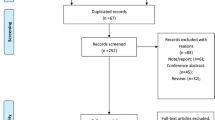
Seventeen studies including 2914 AIS patients were identified. Pooled results showed that tirofiban treatment in AIS did not increase the risk of sICH (OR, 0.95; 95% CI, 0.71–1.28; p = 0.75) or mortality (OR, 0.80; 95% CI; 0.64–1.02; p = 0.07). However, fatal ICH increased significantly in the tirofiban treatment group (OR, 2.84; 95% CI, 1.38–5.85; p = 0.005), and subgroup analysis showed that tirofiban via intra-arterial (IA) administration was associated with increased risk of fatal ICH (OR, 2.90; 95% CI, 1.12–7.55; p = 0.03), while intravenous (IV) administration was not (OR, 2.75; 95% CI, 0.92–8.20; p = 0.07). In addition, tirofiban showed no obvious improvement in functional outcome (mRS 0–2) (OR, 1.29; 95% CI, 0.97–1.71; p = 0.08).
Conclusion
Tirofiban seems to be safe in systemic treatment and may represent a potential choice for management of AIS. However, intra-arterial administration requires further adequately controlled studies in order to develop an appropriate protocol, similar to that in cardiology.



Similar content being viewed by others
References
Baxter Healthcare Corporation. AGGRASTAT® (tirofiban hydrochloride) injection, for intravenous use. Available at: https://www.accessdatafdagov/drugsatfda_docs/label/2019/020912s027,020913s026lblpdf. Accessed 28 May 2019
Siebler M, Hennerici MG, Schneider D, von Reutern GM, Seitz RJ, Rother J, Witte OW, Hamann G, Junghans U, Villringer A, Fiebach JB (2011) Safety of tirofiban in acute ischemic stroke: the SaTIS trial. Stroke 42(9):2388–2392. https://doi.org/10.1161/strokeaha.110.599662
Torgano G, Zecca B, Monzani V, Maestroni A, Rossi P, Cazzaniga M, Manganaro D, Boiti C, Zilioli E, Borutti G, Falaschi F, Mandelli C (2010) Effect of intravenous tirofiban and aspirin in reducing short-term and long-term neurologic deficit in patients with ischemic stroke: a double-blind randomized trial. Cerebrovasc Dis 29(3):275–281. https://doi.org/10.1159/000275503
Seitz RJ, Hamzavi M, Junghans U, Ringleb PA, Schranz C, Siebler M (2003) Thrombolysis with recombinant tissue plasminogen activator and tirofiban in stroke: preliminary observations. Stroke 34(8):1932–1935. https://doi.org/10.1161/01.Str.0000080535.61188.A6
Junghans U, Seitz RJ, Aulich A, Freund HJ, Siebler M (2001) Bleeding risk of tirofiban, a nonpeptide GPIIb/IIIa platelet receptor antagonist in progressive stroke: an open pilot study. Cerebrovasc Dis 12(4):308–312. https://doi.org/10.1159/000047726
Palumbo V, Saia V, Nappini S, Romani I, Nencini P, Inzitari D, Mangiafico S (2010) Preliminary evaluation of hemorrhagic risk of systemic tirofiban in acute stroke patients treated with endovascular approach. Cerebrovasc Dis 29(suppl 2):206. https://doi.org/10.1159/000321266
Zhao W, Che R, Shang S, Wu C, Li C, Wu L, Chen J, Duan J, Song H, Zhang H, Ling F, Wang Y, Liebeskind D, Feng W, Ji X (2017) Low-dose tirofiban improves functional outcome in acute ischemic stroke patients treated with endovascular thrombectomy. Stroke 48(12):3289–3294. https://doi.org/10.1161/strokeaha.117.019193
Gruber P, Hlavica M, Berberat J, Victor Ineichen B, Diepers M, Nedeltchev K, Kahles T, Remonda L (2018) Acute administration of tirofiban versus aspirin in emergent carotid artery stenting. Interv Neuroradiol. https://doi.org/10.1177/1591019918808777
Kellert L, Hametner C, Rohde S, Bendszus M, Hacke W, Ringleb P, Stampfl S (2013) Endovascular stroke therapy: tirofiban is associated with risk of fatal intracerebral hemorrhage and poor outcome. Stroke 44(5):1453–1455. https://doi.org/10.1161/strokeaha.111.000502
Wu Y, Yin C, Yang J, Jiang L, Parsons MW, Lin L (2018) Endovascular thrombectomy: tirofiban increases bleeding risk in acute stroke patients. Stroke 49(11):2783–2785. https://doi.org/10.1161/strokeaha.118.022919
Powers WJ, Rabinstein AA, Ackerson T, Adeoye OM, Bambakidis NC, Becker K, Biller J, Brown M, Demaerschalk BM, Hoh B, Jauch EC, Kidwell CS, Leslie-Mazwi TM, Ovbiagele B, Scott PA, Sheth KN, Southerland AM, Summers DV, Tirschwell DL (2018) 2018 guidelines for the early management of patients with acute ischemic stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 49(3):e46–e110. https://doi.org/10.1161/str.0000000000000158
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, Shekelle P, Stewart LA (2015) Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev 4:1. https://doi.org/10.1186/2046-4053-4-1
Higgins JP, Altman DG, Gotzsche PC, Juni P, Moher D, Oxman AD, Savovic J, Schulz KF, Weeks L, Sterne JA (2011) The Cochrane Collaboration's tool for assessing risk of bias in randomised trials. BMJ (Clinical Research Ed) 343:d5928. https://doi.org/10.1136/bmj.d5928
Stang A (2010) Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25(9):603–605. https://doi.org/10.1007/s10654-010-9491-z
Wahlgren N, Ahmed N, Davalos A, Ford GA, Grond M, Hacke W, Hennerici MG, Kaste M, Kuelkens S, Larrue V, Lees KR, Roine RO, Soinne L, Toni D, Vanhooren G (2007) Thrombolysis with alteplase for acute ischaemic stroke in the safe implementation of thrombolysis in stroke-monitoring study (SITS-MOST): an observational study. Lancet 369(9558):275–282. https://doi.org/10.1016/s0140-6736(07)60149-4
Hacke W, Kaste M, Bluhmki E, Brozman M, Davalos A, Guidetti D, Larrue V, Lees KR, Medeghri Z, Machnig T, Schneider D, von Kummer R, Wahlgren N, Toni D (2008) Thrombolysis with alteplase 3 to 4.5 hours after acute ischemic stroke. N Engl J Med 359(13):1317–1329. https://doi.org/10.1056/NEJMoa0804656
Higashida RT, Furlan AJ, Roberts H, Tomsick T, Connors B, Barr J, Dillon W, Warach S, Broderick J, Tilley B, Sacks D (2003) Trial design and reporting standards for intra-arterial cerebral thrombolysis for acute ischemic stroke. Stroke 34(8):e109–e137. https://doi.org/10.1161/01.Str.0000082721.62796.09
Renieri L, Consoli A, Rosi A, Chiarotti I, Vignoli C, Lanzetta C, Limbucci N, Nappini S, Nencini P, Inzitari D, Mangiafico S (2014) Safety and clinical outcome in patients treated with GP IIbIIIa inhibitors (Tirofiban) in endovascular treatment of acute ischemic stroke: a single centre experience. Cerebrovasc Dis 37(Suppl 1):652
Li W, Lin L, Zhang M, Wu Y, Liu C, Li X, Huang S, Liang C, Wang Y, Chen J, Feng W (2016) Safety and preliminary efficacy of early tirofiban treatment after alteplase in acute ischemic stroke patients. Stroke 47(10):2649–2651. https://doi.org/10.1161/strokeaha.116.014413
Lin L, Li W, Liu CC, Wu Y, Huang SH, Li XS, Liang CR, Wang H, Zhang LL, Xu ZQ, Wang YJ, Feng W, Zhang M (2017) Safety and preliminary efficacy of intravenous tirofiban in acute ischemic stroke patient without arterial occlusion on neurovascular imaging studies. J Neurol Sci 383:175–179. https://doi.org/10.1016/j.jns.2017.10.041
Kang DH, Yoon W, Kim SK, Baek BH, Lee YY, Kim YW, Kim YS, Hwang YH, Kim JT, Park MS (2018) Endovascular treatment for emergent large vessel occlusion due to severe intracranial atherosclerotic stenosis. J Neurosurg 1–8. https://doi.org/10.3171/2018.1.Jns172350
Yu T, Lin Y, Jin A, Zhang P, Zhou X, Fang M, Liu X (2018) Safety and efficiency of low dose intra-arterial tirofiban in mechanical thrombectomy during acute ischemic stroke. Curr Neurovasc Res 15(2):145–150. https://doi.org/10.2174/1567202615666180605104931
Liu J, Shi Q, Sun Y, He J, Yang B, Zhang C, Guo R (2019) Efficacy of tirofiban administered at different time points after intravenous thrombolytic therapy with alteplase in patients with acute ischemic stroke. J Stroke Cerebrovasc Dis. https://doi.org/10.1016/j.jstrokecerebrovasdis.2018.12.044
Pan X, Zheng D, Zheng Y, Chan PWL, Lin Y, Zou J, Zhou J, Yang J (2019) Safety and efficacy of tirofiban combined with endovascular treatment in acute ischemic stroke. Eur J Neurol. https://doi.org/10.1111/ene.13946
Zhang S, Hao Y, Tian X, Zi W, Wang H, Yang D, Zhang M, Zhang X, Bai Y, Li Z, Sun B, Li S, Fan X, Liu X, Xu G (2019) Safety of intra-arterial tirofiban administration in ischemic stroke patients after unsuccessful mechanical thrombectomy. J Vasc Interv Radiol 30(2):141–147.e141. https://doi.org/10.1016/j.jvir.2018.08.021
Yang M, Huo X, Miao Z, Wang Y (2019) Platelet glycoprotein IIb/IIIa receptor inhibitor tirofiban in acute ischemic stroke. Drugs. https://doi.org/10.1007/s40265-019-01078-0
Platelet Receptor Inhibition in Ischemic Syndrome Management in Patients Limited by Unstable Signs and Symptoms (PRISM-PLUS) Study Investigators (1998) Inhibition of the platelet glycoprotein IIb/IIIa receptor with tirofiban in unstable angina and non–Q-wave myocardial infarction. N Engl J Med 338(21):1488–1497. https://doi.org/10.1056/nejm199805213382102
National Institute of Neurological Disorders and Stroke rt-PA Stroke Study Group (1995) Tissue plasminogen activator for acute ischemic stroke. N Engl J Med 333(24):1581–1588. https://doi.org/10.1056/nejm199512143332401
Hacke W, Kaste M, Fieschi C, von Kummer R, Davalos A, Meier D, Larrue V, Bluhmki E, Davis S, Donnan G, Schneider D, Diez-Tejedor E, Trouillas P (1998) Randomised double-blind placebo-controlled trial of thrombolytic therapy with intravenous alteplase in acute ischaemic stroke (ECASS II). Second European-Australasian acute stroke study investigators. Lancet 352(9136):1245–1251. https://doi.org/10.1016/S0140-6736(98)08020-9
von Kummer R, Broderick JP, Campbell BC, Demchuk A, Goyal M, Hill MD, Treurniet KM, Majoie CB, Marquering HA, Mazya MV, San Roman L, Saver JL, Strbian D, Whiteley W, Hacke W (2015) The Heidelberg bleeding classification: classification of bleeding events after ischemic stroke and reperfusion therapy. Stroke 46(10):2981–2986. https://doi.org/10.1161/strokeaha.115.010049
Funding
This work was supported by Changzhou Science and Technology Program (Grant No.CE20195048; CJ20190034), the Science and Technology Development Foundation of Nanjing Medical University (Grant No. NMUB2018061) and Natural Science Foundation of Jiangsu Province (Grant No.BK20191157) .
Author information
Authors and Affiliations
Contributions
J.H.G., Q.Z.S., and G.J.L. conceptualized and designed the study, and J.H.G. and J.J.S. selected studies and planned the analysis. J.H.G., J.J.S., and H.Y. contributed to the development of the selection criteria, the assessment strategy for the risk of bias, and the data extraction criteria. Z.Q.S. and Q.W. provided statistical expertise. J.H.G. drafted the manuscript, and D.S., Z.Q.S., and G.J.L. participated in critical revision of the manuscript. All authors read, provided feedback, and approved the final manuscript as submitted.
Corresponding authors
Ethics declarations
Conflict of interest
All authors declare that they do not have a conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOC 239 kb)
Rights and permissions
About this article
Cite this article
Gong, J., Shang, J., Yu, H. et al. Tirofiban for acute ischemic stroke: systematic review and meta-analysis. Eur J Clin Pharmacol 76, 475–481 (2020). https://doi.org/10.1007/s00228-019-02817-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-019-02817-8