Abstract
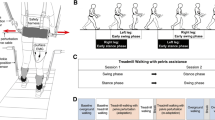
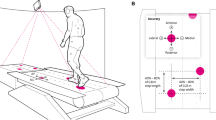
The purpose of this study was to determine whether the application of a varied pelvis perturbation force would improve dynamic balance control and gait stability of people with incomplete spinal cord injury (iSCI). Fourteen participants with iSCI completed the test in two conditions, i.e., walking paired with pelvis perturbation force and treadmill walking only, with 1-week interval in between. The order of the testing condition was randomized across participants. For the pelvis pertubation condition, subjects walked on a treadmill with no force for 1 min, with a varied pelvis perturbation force that was bilaterally applied in the medial–lateral direction for 10 min, without force for 1 min, and then with the perturbation for another 10 min after a sitting break. For the treadmill only condition, a protocol that was similar to the perturbation condition was used but no force was applied. Margin of stability (MoS), weight shifting, and other spatiotemporal gait parameters were calculated. Compared to treadmill training only, participants showed significant smaller MoS and double-leg support time after treadmill walking with pelvis perturbation. In addition, participants showed significantly greater improvements in overground walking speed after treadmill walking with pelvis perturbation than treadmill only (p = 0.021). Results from this study suggest that applying a varied pelvis perturbation force during treadmill walking could improve dynamic balance control in people with iSCI, which could be transferred to overground walking. These findings may be used to develop a new intervention to improve balance and walking function in people with iSCI.






Similar content being viewed by others
References
Bauby CE, Kuo AD (2000) Active control of lateral balance in human walking. J Biomech 33:1433–1440
Berg KO, Maki BE, Williams JI, Holliday PJ, Wood-Dauphinee SL (1992) Clinical and laboratory measures of postural balance in an elderly population. Arch Phys Med Rehabil 73:1073–1080
Brach JS, Berlin JE, VanSwearingen JM, Newman AB, Studenski SA (2005) Too much or too little step width variability is associated with a fall history in older persons who walk at or near normal gait speed. J Neuroeng Rehabil 2:21
Churchland MM, Yu BM, Ryu SI, Santhanam G, Shenoy KV (2006) Neural variability in premotor cortex provides a signature of motor preparation. J Neurosci 26:3697–3712
Classen J, Liepert J, Wise SP, Hallett M, Cohen LG (1998) Rapid plasticity of human cortical movement representation induced by practice. J Neurophysiol 79:1117–1123
Day KV, Kautz SA, Wu SS, Suter SP, Behrman AL (2012) Foot placement variability as a walking balance mechanism post-spinal cord injury. Clin Biomech (Bristol, Avon) 27:145–150
de Jong LAF, van Dijsseldonk RB, Keijsers NLW, Groen BE (2019) Test-retest reliability of stability outcome measures during treadmill walking in patients with balance problems and healthy controls. Gait Posture 76:92–97
Diedrichsen J, White O, Newman D, Lally N (2010) Use-dependent and error-based learning of motor behaviors. J Neurosci 30:5159–5166
Dingwell JB, John J, Cusumano JP (2010) Do humans optimally exploit redundancy to control step variability in walking? Plos Comput Biol 6(7):e1000856
Donelan JM, Shipman DW, Kram R, Kuo AD (2004) Mechanical and metabolic requirements for active lateral stabilization in human walking. J Biomech 37:827–835
Edgerton VR, Roy RR (2009) Activity-dependent plasticity of spinal locomotion: implications for sensory processing. Exerc Sport Sci Rev 37:171–178
Field-Fote EC, Roach KE (2011) Influence of a locomotor training approach on walking speed and distance in people with chronic spinal cord injury: a randomized clinical trial. Phys Ther 91:48–60
Finley JM, Dhaher YY, Perreault EJ (2012) Contributions of feed-forward and feedback strategies at the human ankle during control of unstable loads. Exp Brain Res 217:53–66
Floor-Westerdijk MJ, Schepers HM, Veltink PH, van Asseldonk EHF, Buurke JH (2012) Use of inertial sensors for ambulatory assessment of center-of-mass displacements during walking. IEEE T Bio-Med Eng 59:2080–2084
Forrest GF, Lorenz DJ, Hutchinson K, Vanhiel LR, Basso DM, Datta S, Sisto SA, Harkema SJ (2012) Ambulation and balance outcomes measure different aspects of recovery in individuals with chronic, incomplete spinal cord injury. Arch Phys Med Rehabil 93:1553–1564
Gardner MB, Holden MK, Leikauskas JM, Richard RL (1998) Partial body weight support with treadmill locomotion to improve gait after incomplete spinal cord injury: a single-subject experimental design. Phys Ther 78:361–374
Hausdorff JM (2005) Gait variability: methods, modeling and meaning. J Neuroeng Rehabil 2:19
Hebb D (1949) The organization of behavior: a neuropsychological theory. Wiley, New York
Herzfeld DJ, Shadmehr R (2014) Motor variability is not noise, but grist for the learning mill. Nat Neurosci 17:149–150
Hof AL, Gazendam MG, Sinke WE (2005) The condition for dynamic stability. J Biomech 38:1–8
Hof AL, van Bockel RM, Schoppen T, Postema K (2007) Control of lateral balance in walking. Experimental findings in normal subjects and above-knee amputees. Gait Posture 25:250–258
Houldin A, Chua R, Carpenter MG, Lam T (2012) Limited interlimb transfer of locomotor adaptations to a velocity-dependent force field during unipedal walking. J Neurophysiol 108:943–952
Kerr R, Booth B (1978) Specific and varied practice of motor skill. Percept Mot Skills 46:395–401
Kim CM, Eng JJ, Whittaker MW (2004) Level walking and ambulatory capacity in persons with incomplete spinal cord injury: relationship with muscle strength. Spinal Cord 42:156–162
Lemay JF, Duclos C, Nadeau S, Gagnon D, Desrosiers E (2014) Postural and dynamic balance while walking in adults with incomplete spinal cord injury. J Electromyogr Kinesiol 24:739–746
Lin JT, Hsu CJ, Dee W, Chen D, Rymer WZ, Wu M (2019a) Error variability affects the after effects following motor learning of lateral balance control during walking in people with spinal cord injury. Eur J Neurosci 50:3221–3234
Lin JT, Hsu CJ, Dee W, Chen D, Rymer WZ, Wu M (2019b) Motor adaptation to weight shifting assistance transfers to overground walking in people with spinal cord injury. PM&R 11(11):1200–1209
MacKinnon CD, Winter DA (1993) Control of whole body balance in the frontal plane during human walking. J Biomech 26:633–644
Marchal-Crespo L, Tsangaridis P, Obwegeser D, Maggioni S, Riener R (2019) Haptic error modulation outperforms visual error amplification when learning a modified gait pattern. Front Neurosci-Switz 13:61
McAndrew Young PM, Wilken JM, Dingwell JB (2012) Dynamic margins of stability during human walking in destabilizing environments. J Biomech 45:1053–1059
Nam KY, Kim HJ, Kwon BS, Park JW, Lee HJ, Yoo A (2017) Robot-assisted gait training (Lokomat) improves walking function and activity in people with spinal cord injury: a systematic review. J Neuroeng Rehabil 14:24
Osborne LC, Lisberger SG, Bialek W (2005) A sensory source for motor variation. Nature 437:412–416
Pai YC (2003) Movement termination and stability in standing. Exerc Sport Sci Rev 31:19–25
Patton JL, Stoykov ME, Kovic M, Mussa-Ivaldi FA (2006) Evaluation of robotic training forces that either enhance or reduce error in chronic hemiparetic stroke survivors. Exp Brain Res 168:368–383
Peebles AT, Reinholdt A, Bruetsch AP, Lynch SG, Huisinga JM (2016) Dynamic margin of stability during gait is altered in persons with multiple sclerosis. J Biomech 49:3949–3955
Pepin A, Ladouceur M, Barbeau H (2003) Treadmill walking in incomplete spinal-cord-injured subjects: 2. Factors limiting the maximal speed. Spinal Cord 41:271–279
Ryu E (2011) Effects of skewness and kurtosis on normal-theory based maximum likelihood test statistic in multilevel structural equation modeling. Behav Res Methods 43:1066–1074
Scivoletto G, Romanelli A, Mariotti A, Marinucci D, Tamburella F, Mammone A, Cosentino E, Sterzi S, Molinari M (2008) Clinical factors that affect walking level and performance in chronic spinal cord lesion patients. Spine (Phila Pa 1976) 33:259–264
Shadmehr R, Huang HJ, Ahmed AA (2016) A representation of effort in decision-making and motor control. Curr Biol 26:1929–1934
Shea CH, Kohl RM (1990) Specificity and variability of practice. Res Q Exerc Sport 61:169–177
Shumway-Cook A, Gruber W, Baldwin M, Liao S (1997) The effect of multidimensional exercises on balance, mobility, and fall risk in community-dwelling older adults. Phys Ther 77:46–57
Sohn WJ, Tan AQ, Hayes HB, Pochiraju S, Deffeyes J, Trumbower RD (2018) Variability of leg kinematics during overground walking in persons with chronic incomplete spinal cord injury. J Neurotrauma 35:2519–2529
Stokes HE, Thompson JD, Franz JR (2017) The neuromuscular origins of kinematic variability during perturbed walking. Sci Rep 7:808
Tumer EC, Brainard MS (2007) Performance variability enables adaptive plasticity of 'crystallized' adult birdsong. Nature 450:1240–1244
van Beers RJ, Brenner E, Smeets JB (2013) Random walk of motor planning in task-irrelevant dimensions. J Neurophysiol 109:969–977
van Hedel HJ, Dietz V (2010) Rehabilitation of locomotion after spinal cord injury. Restor Neurol Neurosci 28:123–134
Vistamehr A, Kautz SA, Bowden MG, Neptune RR (2016) Correlations between measures of dynamic balance in individuals with post-stroke hemiparesis. J Biomech 49:396–400
Wannapakhe J, Arrayawichanon P, Saengsuwan J, Amatachaya S (2015) Medical complications and falls in patients with spinal cord injury during the immediate phase after completing a rehabilitation program. J Spinal Cord Med 38:84–90
Wirz M, Muller R, Bastiaenen C (2010) Falls in persons with spinal cord injury: validity and reliability of the Berg Balance Scale. Neurorehabil Neural Repair 24:70–77
Wu M, Hornby TG, Landry JM, Roth H, Schmit BD (2011) A cable-driven locomotor training system for restoration of gait in human SCI. Gait Posture 33:256–260
Wu HG, Miyamoto YR, Castro LNG, Olveczky BP, Smith MA (2014) Temporal structure of motor variability is dynamically regulated and predicts motor learning ability. Nat Neurosci 17:312–321
Wu M, Kim J, Arora P, Gaebler-Spira DJ, Zhang Y (2016a) Kinematic and EMG responses to pelvis and leg assistance force during treadmill walking in children with cerebral palsy. Neural Plast 2016:5020348
Wu M, Landry JM, Kim J, Schmit BD, Yen SC, McDonald J, Zhang Y (2016b) Repeat exposure to leg swing perturbations during treadmill training induces long-term retention of increased step length in human SCI: a pilot randomized controlled Study. Am J Phys Med Rehabil 95:911–920
Yang JF, Norton J, Nevett-Duchcherer J, Roy FD, Gross DP, Gorassini MA (2011) Volitional muscle strength in the legs predicts changes in walking speed following locomotor training in people with chronic spinal cord injury. Phys Ther 91:931–943
Yen SC, Schmit BD, Landry JM, Roth H, Wu M (2012) Locomotor adaptation to resistance during treadmill training transfers to overground walking in human SCI. Exp Brain Res 216:473–482
Zeni JA Jr, Richards JG, Higginson JS (2008) Two simple methods for determining gait events during treadmill and overground walking using kinematic data. Gait Posture 27:710–714
Acknowledgements
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article. This study is supported by National Institutes of Health (NIH) (Grant No. NIH/NICHD, R01HD083314). We thank Ms. Jill Landry for editing the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No potential conflict of interest was reported by the authors.
Additional information
Communicated by Francesco Lacquaniti.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lin, JT., Hsu, CJ., Dee, W. et al. Varied movement errors drive learning of dynamic balance control during walking in people with incomplete spinal cord injury: a pilot study. Exp Brain Res 238, 981–993 (2020). https://doi.org/10.1007/s00221-020-05776-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00221-020-05776-0