Abstract
Background
In addition to the genetic complexity of hypertrophic cardiomyopathy (HCM), there must be other disease-modifying factors that contribute to its highly variable clinical and phenotypic expression. The authors aimed to investigate serum thiol/disulphide homeostasis as a proxy for oxidative stress using a novel automated assay in patients with HCM.
Methods
This cross-sectional study was conducted on 119 patients with HCM and 52 without HCM. The methods used to measure dynamic thiol/disulphide homeostasis as calorimetric and duplex quantities were developed in 2014.
Results
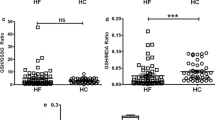
Median serum native thiol levels were significantly lower in patients with HCM than in those without (312.5 μmol/L [285–370 μmol/L] vs 421 μmol/L [349–469.5 μmol/L]; p < 0.001). Serum total thiol levels and disulphide levels were considerably lower than those in the control group ([844.68 ± 195.99 μmol/L vs 1158.92 ± 243.97 μmol/L; p < 0.001], [259.13 ± 65.66 μmol/L vs 375.02 ± 79.99 μmol/L; p < 0.001], respectively). Serum disulphide/native thiol ratios and disulphide/total thiol ratios were significantly lower in HCM patients than in controls (0.80 ± 0.09 vs 0.92 ± 0.05; p < 0.001 and 0.31 [0.30–0.32] vs 0.32 [0.32–0.33]; p < 0.001). Finally, reduced thiol ratios were higher and oxidized thiol ratios were significantly lower in patients with HCM than in controls.
Conclusions
Despite the fact that antioxidant capacity was impaired, the extracellular environment remained in a reducing state by keeping serum disulphide/native thiol ratios low. Therefore, the authors speculate that HCM may behave similarly to tumours with respect to serum thiol-disulphide levels.
Zusammenfassung
Hintergrund
Neben der genetischen Komplexität der hypertrophen Kardiomyopathie (HCM) muss es weitere krankheitsmodifizierende Faktoren geben, die zur hoch variablen klinischen und phänotypischen Ausprägung der Erkrankung beitragen. Ziel der vorliegenden Arbeit war es, die Thiol/Disulfid-Homöostase im Serum als einen Surrogatparameter für oxidativen Stress bei Patienten mit HCM zu untersuchen; dabei kam ein neuartiger automatisierter Assay zum Einsatz.
Methoden
In diese Querschnittstudie wurden 119 Patienten mit und 52 Patienten ohne HCM eingeschlossen. Die Verfahren zur Messung der dynamischen Thiol/Disulfid-Homöostase als kalorimetrische und Duplex-Mengen wurden 2014 entwickelt.
Ergebnisse
Die medianen Serumkonzentrationen von nativem Thiol waren bei Patienten mit HCM signifikant niedriger als bei Patienten ohne die Erkrankung: 312,5 μmol/l (285–370 μmol/l) vs. 421 μmol/l (349–469,5 μmol/l); p < 0,001. Die Gesamtthiol- und Disulfidkonzentrationen im Serum waren erheblich niedriger als in der Kontrollgruppe: 844,68 ± 195,99 μmol/l vs. 1158,92 ± 243,97 μmol/l; p < 0,001; 259,13 ± 65,66 μmol/l vs. 375,02 ± 79,99 μmol/l; p < 0,001. Das Verhältnis von Disulfiden zu nativem Thiol und von Disulfiden zu Gesamtthiol war bei Patienten mit HCM signifikant niedriger als in der Kontrollgruppe: 0,80 ± 0,09 vs. 0,92 ± 0,05; p < 0,001; 0,31 (0,30–0,32) vs. 0,32 (0,32–0,33); p < 0,001. Zudem war das Verhältnis reduzierter Thiole bei Patienten mit HCM höher als in der Kontrollgruppe, das Verhältnis oxidierter Thiole dagegen niedriger.
Schlussfolgerungen
Obwohl die antioxidative Kapazität beeinträchtigt war, blieb das extrazelluläre Milieu in einem reduzierten Zustand, indem die Verhältnisse von Disulfiden zu nativem Thiol im Serum niedrig gehalten wurden. Daher vermuten wir, dass sich die HCM in Bezug auf Thiol‑/Disulfidspiegel im Serum ähnlich verhält wie Tumoren.


Similar content being viewed by others
References
Elliott PM, Anastasakis A, Borger MA, Borggrefe M, Cecchi F et al (2014) ESC guidelines on diagnosis and management of hypertrophic cardiomyopathy: the Task Force for the Diagnosis and Management of Hypertrophic Cardiomyopathy of the European Society of Cardiology (ESC). Eur Heart J 35(39):2733–2779. https://doi.org/10.1093/eurheartj/ehu284
Ho CY, Day SM, Ashley EA, Michels M, Pereira AC, Jacoby D, Cirino AL, Fox JC, Lakdawala NK, Ware JS, Caleshu CA, Helms AS, Colan SD, Girolami F, Cecchi F, Seidman CE, Sajeev G, Signorovitch J, Green EM, Olivotto I (2018) Genotype and lifetime burden of disease in hypertrophic cardiomyopathy: insights from the sarcomeric human cardiomyopathy registry (SHaRe). Circulation 138(14):1387–1398. https://doi.org/10.1161/CIRCULATIONAHA.117.033200
Frey N, Luedde M, Katus HA (2011) Mechanisms of disease: hypertrophic cardiomyopathy. Nat Rev Cardiol 9(2):91–100. https://doi.org/10.1038/nrcardio.2011.159
Erel O, Neselioglu S (2014) A novel and automated assay for thiol/disulphide homeostasis. Clin Biochem 47(18):326–332. https://doi.org/10.1016/j.clinbiochem.2014.09.026
Altiparmak IH, Erkus ME, Sezen H, Demirbag R, Kaya Z, Sezen Y, Gunebakmaz O, Asoglu R, Besli F, Neselioglu S, Erel O (2016) Evaluation of thiol levels, thiol/disulfide homeostasis and their relation with inflammation in cardiac syndrome X. Coron Artery Dis 27(4):295–301. https://doi.org/10.1097/MCA.0000000000000362
Altıparmak IH, Erkuş ME, Sezen H, Demirbag R, Gunebakmaz O, Kaya Z, Sezen Y, Asoglu R, Dedeoglu IH, Neselioglu S, Erel O (2016) The relation of serum thiol levels and thiol/disulphide homeostasis with the severity of coronary artery disease. Kardiol Pol 74(11):1346–1353. https://doi.org/10.5603/KP.a2016.0085
Kızıltunç E, Gök M, Kundi H, Çetin M, Topçuoğlu C, Gülkan B, Çiçekçioğlu H, Örnek E (2016) Plasma thiols and thiol-disulfide homeostasis in patients with isolated coronary artery ectasia. Atherosclerosis 253:209–213. https://doi.org/10.1016/j.atherosclerosis.2016.07.904
Kundi H, Ates I, Kiziltunc E, Cetin M, Cicekcioglu H, Neselioglu S, Erel O, Ornek E (2015) A novel oxidative stress marker in acute myocardial infarction; thiol/disulphide homeostasis. Am J Emerg Med 33(11):1567–1571. https://doi.org/10.1016/j.ajem.2015.06.016
Ergin M, Caliskanturk M, Senat A, Akturk O, Erel O (2016) Disulfide stress in carbon monoxide poisoning. Clin Biochem 49(16/17):1243–1247. https://doi.org/10.1016/j.clinbiochem.2016.07.019
Topuz M, Kaplan M, Akkus O, Sen O, Yunsel HD, Allahverdiyev S, Erel O, Koc M, Gur M (2016) The prognostic importance of thiol/disulfide homeostasis in patients with acute pulmonary thromboembolism. Am J Emerg Med 34(12):2315–2319. https://doi.org/10.1016/j.ajem.2016.08.039
Dinc ME, Ozdemir C, Ayan NN, Bozan N, Ulusoy S, Koca C, Erel O (2017) Thiol/disulfide homeostasis as a novel indicator of oxidative stress in obstructive sleep apnea patients. Laryngoscope 127(7):244–250. https://doi.org/10.1002/lary.26444
Ates I, Ozkayar N, Inan B, Yilmaz FM, Topcuoglu C, Neselioglu S, Erel O, Dede F, Yilmaz N (2016) Dynamic thiol/disulphide homeostasis in patients with newly diagnosed primary hypertension. J Am Soc Hypertens 10(2):159–166. https://doi.org/10.1016/j.jash.2015.12.008
Ergin M, Aydin C, Yurt EF, Cakir B, Erel O (2018) The variation of disulfides in the progression of type 2 diabetes mellitus. Exp Clin Endocrinol Diabetes. https://doi.org/10.1055/s-0044-100376
Bektas H, Vural G, Gumusyayla S, Deniz O, Alisik M, Erel O (2016) Dynamic thiol–disulfide homeostasis in acute ischemic stroke patients. Acta Neurol Belg 116(4):489–494. https://doi.org/10.1007/s13760-016-0598-1
Eroglu S, Haskul I, Aziz V, Yurtcu E, Karatas F, Neselioglu S, Erel O (2017) Dynamic thiol/disulphide homeostasis in patients with uterine myoma. Eur J Obstet Gynecol Reprod Biol 216:24–26. https://doi.org/10.1016/j.ejogrb.2017.06.045
Guney T, Kanat IF, Alkan A, Alisik M, Akinci S, Silay K, Neselioglu S, Dilek I, Erel O (2017) Assessment of serum thiol/disulfide homeostasis in multiple myeloma patients by a new method. Redox Rep 22(6):246–251. https://doi.org/10.1080/13510002.2016.1180100
Hanikoglu F, Hanikoglu A, Kucuksayan E, Alisik M, Gocener AA, Erel O, Baykara M, Cuoghi A, Tomasi A, Ozben T (2016) Dynamic thiol/disulphide homeostasis before and after radical prostatectomy in patients with prostate cancer. Free Radic Res 50(1):79–84. https://doi.org/10.1080/10715762.2016.1235787
Dirican N, Dirican A, Sen O, Aynali A, Atalay S, Bircan HA, Oztürk O, Erdogan S, Cakir M, Akkaya A (2016) Thiol/disulfide homeostasis: a prognostic biomarker for patients with advanced non-small cell lung cancer? Redox Rep 21(5):197–203. https://doi.org/10.1179/1351000215Y.0000000027
Lin CS, Liu CY, Sun YL, Chang LC, Chiu YT, Huang SY, Lin JH, Yang PC, Chu R, Huang MC, Mao SJ (1997) Alteration of endogenous antioxidant enzymes in naturally occurring hypertrophic cardiomyopathy. Biochem Mol Biol Int 43(6):1253–1263
Christiansen LB, Dela F, Koch J, Hansen CN, Leifsson PS, Yokota T (2015) Impaired cardiac mitochondrial oxidative phosphorylation and enhanced mitochondrial oxidative stress in feline hypertrophic cardiomyopathy. Am J Physiol Heart Circ Physiol 308(10):1237–1247. https://doi.org/10.1152/ajpheart.00727.2014
Dimitrow PP, Undas A, Wolkow P, Tracz W, Dubiel JS (2009) Enhanced oxidative stress in hypertrophic cardiomyopathy. Pharmacol Rep 61(3):491–495
Nakamura K, Kusano KF, Matsubara H, Nakamura Y, Miura A, Nishii N, Banba K, Nagase S, Miyaji K, Morita H, Saito H, Emori T, Ohe T (2005) Relationship between oxidative stress and systolic dysfunction in patients with hypertrophic cardiomyopathy. J Card Fail 11(2):117–123
Lombardi R, Rodriguez G, Chen SN, Ripplinger CM, Li W, Chen J, Willerson JT, Betocchi S, Wickline SA, Efimov IR, Marian AJ (2009) Resolution of established cardiac hypertrophy and fibrosis and prevention of systolic dysfunction in a transgenic rabbit model of human cardiomyopathy through thiol-sensitive mechanisms. Circulation 119(10):1398–1407. https://doi.org/10.1161/CIRCULATIONAHA.108.790501
Marian AJ, Senthil V, Chen SN, Lombardi R (2006) Antifibrotic effects of antioxidant N‑acetylcysteine in a mouse model of human hypertrophic cardiomyopathy mutation. J Am Coll Cardiol 47(4):827–834. https://doi.org/10.1016/j.jacc.2005.10.041
Wilder T, Ryba DM, Wieczorek DF, Wolska BM, Solaro RJ (2015) N‑acetylcysteine reverses diastolic dysfunction and hypertrophy in familial hypertrophic cardiomyopathy. Am J Physiol Heart Circ Physiol 309(10):1720–1730. https://doi.org/10.1152/ajpheart.00339.2015
Marian AJ, Tan Y, Li L, Chang J, Syrris P, Hessabi M, Rahbar MH, Willerson JT, Cheong BY, Liu CY, Kleiman NS, Bluemke DA, Nagueh SF (2018) Hypertrophy regression with N‑acetylcysteine in hypertrophic cardiomyopathy (HALT-HCM): a randomized, placebo-controlled, double-blind pilot study. Circ Res 122(8):1109–1118. https://doi.org/10.1161/CIRCRESAHA.117.312647
Senthil V, Chen SN, Tsybouleva N, Halder T, Nagueh SF, Willerson JT, Roberts R, Marian AJ (2005) Prevention of cardiac hypertrophy by atorvastatin in a transgenic rabbit model of human hypertrophic cardiomyopathy. Circ Res 97(3):285–292. https://doi.org/10.1161/01.RES.0000177090.07296.ac
Patel R, Nagueh SF, Tsybouleva N, Abdellatif M, Lutucuta S, Kopelen HA, Quinones MA, Zoghbi WA, Entman ML, Roberts R, Marian AJ (2001) Simvastatin induces regression of cardiac hypertrophy and fibrosis and improves cardiac function in a transgenic rabbit model of human hypertrophic cardiomyopathy. Circulation 104(3):317–324
Marian AJ, Braunwald E (2017) Hypertrophic cardiomyopathy: genetics, pathogenesis, clinical manifestations, diagnosis, and therapy. Circ Res 121(7):749–770. https://doi.org/10.1161/CIRCRESAHA.117.311059
Sugden PH, Clerk A (2006) Oxidative stress and growth-regulating intracellular signaling pathways in cardiac myocytes. Antioxid Redox Signal 8(11/12):2111–2124. https://doi.org/10.1089/ars.2006.8.2111
Kirlin WG, Cai J, Thompson SA, Diaz D, Kavanagh TJ, Jones DP (1999) Glutathione redox potential in response to differentiation and enzyme inducers. Free Radic Biol Med 27(11/12):1208–1218. https://doi.org/10.1016/S0891-5849(99)00145-8
Jonas CR, Ziegler TR, Gu LH, Jones DP (2002) Extracellular thiol/disulfide redox state affects proliferation rate in a human colon carcinoma (Caco2) cell line. Free Radic Biol Med 33(11):1499–1506
Kwon SH, Pimentel DR, Remondino A, Sawyer DB, Colucci WS (2003) H2O2 regulates cardiac myocyte phenotype via concentration-dependent activation of distinct kinase pathways. J Mol Cell Cardiol 35(6):615–621
Lang CA, Mills BJ, Mastropaolo W, Liu MC (2000) Blood glutathione decreases in chronic diseases. J Lab Clin Med 135(5):402–405. https://doi.org/10.1067/mlc.2000.105977
Liu RM, Liu Y, Forman HJ, Olman M, Tarpey MM (2004) Glutathione regulates transforming growth factor-β-stimulated collagen production in fibroblasts. Am J Physiol Lung Cell Mol Physiol 286:L121. https://doi.org/10.1152/ajplung.00231.2003
Acknowledgements
The authors would like to thank Professor Dr. Ramazan Akdemir, the dean of the Medicine Faculty of Sakarya University, for all his contributions to this research.
Funding
This research was supported by a Sakarya University Project Support Fund.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
M. Sari, U. Erkorkmaz, H. Yazar, I. Kocayigit, B. Omar, E. Alizade, M.N.M. Aksoy, A. Uslu, G.C. Cakar and S. Pala declare that they have no competing interests.
For this article no studies with human participants or animals were performed by any of the authors. All studies performed were in accordance with the ethical standards indicated in each case.
Rights and permissions
About this article
Cite this article
Sari, M., Erkorkmaz, U., Yazar, H. et al. Dynamic thiol/disulphide homeostasis in patients with hypertrophic cardiomyopathy. Herz 46, 164–171 (2021). https://doi.org/10.1007/s00059-019-04853-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00059-019-04853-7