Summary
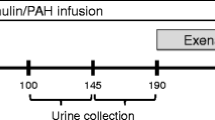
Renal functional reserve capacity was evaluated in 19 normotensive type I diabetics without microalbuminuria. All patients had normal basal renal function as assessed by 24-hour creatinine clearances higher than 120 ml/min. PAH, inulin, and creatinine clearances were carried out every hour before, during, and after infusion of an amino acid (AA) solution. The same experiment was repeated after ACE inhibition with captopril (25 mg). Two groups of patients were found: Group A (responders) showed a significant rise in GFR after AA infusion (inulin clearances from 117±8 to 138±10 ml/min) (p<0.05), whereas in Group B (non-responders) no significant change in GFR was observed. Groups were comparable in age, duration of diabetes, metabolic control, and mean arterial blood pressure.
Group B, however, had a significantly higher basal inulin clearance (167±17 ml/min) than Group A (117±8 ml/min).
In Group A ACE inhibition completely blocked the AA-induced rise in GFR, while basal GFR in Group B was significantly reduced (167±17 to 148±8 ml/min) after captopril administration. In both groups renal plasma flow was enhanced by ACE inhibition.
A rise in glucagon was observed in all patients during AA infusion.
It is concluded that type I diabetics with normal basal renal function already have reduced (Group A) renal functional reserve capacity, which is completely abolished (Group B) when concomitant hyperfiltration occurs. ACE inhibition reduces hyperfiltration and is capable of blocking the AA-induced rise in GFR in these patients.
Similar content being viewed by others
Abbreviations
- ACE:
-
Angiotensin converting enzyme
- ANP:
-
Atriales natriuretisches Peptid
- AS:
-
Aminosäuren
- BE:
-
Broteinheit
- GFR:
-
Glomeruläre Filtrationsrate
- PAH:
-
Paraaminohippursäure
Literatur
Anderson AR, Sandahl Christiansen J, Andersen JK, Kreiner S, Deckert T (1983) Diabetic nephropathy in type I (insulin dependent) diabetes: an epidemiological study. Diabetologia 25:496–501
Anderson S, Meyer TW, De Graphenreid RL, Rennke HG, Brenner BM (1984) Control of glomerular hypertension preserves glomerular structure and function in rats with renal ablation. Clin Res 32:564A
Anderson S, Rennke HG, Brenner BM (1986) Therapeutic adventage of converting enzyme inhibitors in arresting progressive renal disease associated with systemic hypertension in the rat. J Clin Invest 77:1993–2000
Borch-Johnsen K, Kragh Andersen P, Deckert T (1985) The effect of proteinuria on relative mortality in type I (insulin-dependent) diabetes mellitus. Diabetologia 28:590–596
Bosch JP, Saccaggi A, Lauer A, Ronco C, Belledonne M, Glabman S (1983) Renal functional reserve in humans. Effect of protein intake on glomerular filtration rate. Am J Med 75:943–950
Brenner BM (1983) Hemodynamically mediated glomerular injury and the progressive nature of kidney disease. Kidney Int 23:647–655
Brenner BM, Meyer TW, Hostetter TH (1982) Dietary protein intake and the progressive nature of kidney disease: The role of hemodynamically mediated glomerular injury in the pathogenesis of progressive glomerular sclerosis in aging, renal ablation, and intrinsic renal disease. N Engl J Med 307:652–659
Brenner BM, Troy JL, Daugharty TM (1971) The dynamics of glomerular ultrafiltration in the rat. J Clin Invest 50:1776–1792
Butturini U, Bonomini V (1958) Über die Wirkung von Glukagon und Insulin auf Nierenfunktion, Harnausscheidung der Phosphat-, Bicarbonat- und Ammoniakionen und titrierbare Acidität beim Menschen. Helvet Med Acta 5:617–624
del Castillo E, Fuenzalida R, Uranga L (1977) Increased glomerular filtration rate and glomerulopressin activity in diabetic dogs. Horm Metab Res 9:46–53
Davison JM, Dunlop W (1980) Renal hemodynamics and tubular function in normal human pregnancy. Kidney Int 18:152–161
Dworkin LD, Hostetter TH, Rennke HG, Brenner BM (1984) Hemodynamic bases for glomerular injury in rats with desoxycorticosterone-salt hypertension. J Clin Invest 73:1448–1461
Eisenhauer T, Scholz K, Scheler F (1985) Increase of glomerular filtration rate following aminoacid infusion is suppressed by indomethacin in normal subjects. Proc Eur Dial Transplant Assoc Eur Ren Assoc 22:1049–1053
Eisenhauer T, Talartschik J, Scheler F (1986a) Angiotensin converting enzyme inhibition by captopril reduces amino acid-mediated increase in glomerular filtration rate. J Hypertension 4:Suppl 5, S258-S260
Eisenhauer T, Talartschik J, Scheler F (1986b) Detection of fluid overload by plasma concentration of human atrial natriuretic peptide (h-ANP) in patients wih renal failure. Klin Wochenschr 64:Suppl VI, 68–72
El Nahas AM, Coles GA (1986) Dietary treatment of chronic renal failure: ten unanswered questions. Lancet I:597–600
Elrick H, Huffman ER, Hlad CJ, Whipple N, Staub A (1958) Effects of glucagon on renal function in man. J Clin Endocrinol Metab 18:813–824
Graf H, Stummvoll HK, Luger A, Prager R (1983) Effect of amino acid infusion on glomerular filtration rate. N Engl J Med 308:159–160
Hostetter TH (1986) Diabetic nephropathy. In: The Kidney II hrsg. v.: BM Brenner, FC Rector. Saunders, Philadelphia London, 1377–1402
Hostetter TH, Troy IL, Brenner BM (1981) Glomerular haemodynamics in experimental diabetes. Kidney Int 19:410–415
Knowles HC (1974) Magnitude of the renal failure problem in diabetes. Kidney Int 6:2–7
Kramer P, Köthe E, Girndt J (1974) Konventionelle Clearance-Verfahren, Stand und Bedeutung. Mitteilungen der Arbeitsgemeinschaft für Klinische Nephrologie e.V., Bundesrepublik Deutschland und West Berlin 3:25–56
Mogensen CE (1976) Renal function changes in diabetes. Diabetes 25:872–879
Mogensen CE (1984) Microalbuminuria predicts clinical proteinuria and early mortality in maturity-onset diabetes. N Engl J Med 310:356–360
Parving HH, Anderson AR, Smidt UM, Homme E, Mathiesen ER, Svendsen PA (1987) Effect of antihypertensive treatment on kidney function in diabetic nephropathy. Br Med J 294:1443–1447
Parving HH, Noer J, Kehlet H, Mogensen CE, Svendsen PA, Heding L (1977) The effect of short-term glucagon infusion on kidney function in normal man. Diabetologia 13:323–325
Parving HH, Sandahl Christiansen JS, Noer J, Tronier B, Mogensen CE (1980) The effect of glucagon infusion on kidney function in short-term insulin dependent juvenile diabetics. Diabetologia 19:340–344
Popper H, Brod J (1938) Die physiologischen Schwankungen der Nierenarbeit. Z Klin Med 134:196–223
Premen AJ (1985) Importance of the liver during glucagon-mediated increases in canine renal hemodynamics. Am J Physiol 249:F319-F322
Ter Wee PM, Geerlings W, Rosman JB, Sluiter WJ, Van der Geest S, Donker AJM (1985) Testing renal reserve filtration capacity with an amino acid solution. Nephron 41:193–199
Ter Wee PM, Rosman JB, Van der Geest S, Sluiter WG, Donker AJM (1986a) Renal haemodynamics during separate and combined infusion of amino acids and dopamine. Kidney Int 29:870–874
Ter Wee PM, Smit AJ, Rosman JB, Sluiter WJ, Donker AJM (1986b) Effect of intravenous infusion of low-dose dopamine on renal function in normal individuals and in patients with renal disease. Am J Nephrol 6:42–46
Uranga J, Fuenzalida R, Rapoport AL, del Castillo E (1979) Effect of glucagon and glomerulopressin on the renal function of the dog. Horm Metab Res 11:275–279
Viberti GC, Jarrett RJ, Mahmud M, Hill MD, Argyropoulos A, Keen H (1982) Microalbuminuria as a predictor of clinical nephropathy in insulin-dependent diabetes mellitus. Lancet I:1430–1432
Wisemann MJ, Redmond S, House F, Keen H, Viberti GC (1985) The glomerular hyperfiltration of diabetes is not associated with elevated plasma levels of glucagon and growth hormone. Diabetologia 28:718–721
Zatz R, Rentz-Dunn B, Meyer TW, Anderson S, Rennke HG, Brenner BM (1986) Prevention of diabetic glomerulopathy by pharmacological amelioration of glomerular capillary hypertension. J Clin Invest 77:1925–1930
Author information
Authors and Affiliations
Additional information
Herrn Prof. Dr. med. F. Scheler zum 65. Geburtstag gewidmet.
Rights and permissions
About this article
Cite this article
Eisenhauer, T., Jungmann, E., Warneboldt, D. et al. Verhalten der renalen Funktionsreserve von Typ I Diabetikern: Einfluß der Konversionshemmung. Klin Wochenschr 68, 750–757 (1990). https://doi.org/10.1007/BF01647243
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF01647243