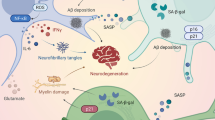
Abstract
Alzheimer's disease (AD) is a neurodegenerative disease closely related to the accumulation of beta-amyloid (Aβ) plaques. Growth differentiation factor 11 (GDF11) is one of the proteins that play a role in the aggravation of AD. Decreased concentration of GDF11 disrupts regenerative nervous system, blood vessels, and various vital systems. Low levels of GDF11 with age can be overcome with recombinant GDF11 (rGDF11) to rejuvenate the regenerative effect. Based on research results, rGDF11 enhance the proliferation rate of neuronal precursor cells as well as angiogenesis. rGDF11 can replace lost levels of GDF11, overcome astrogliosis and activation of nerve cell microglia. Therapeutic effect of rGDF11 leads to an improved prognosis in AD patients by neurogenesis and angiogenesis. The prospects of rGDF11 in the treatment of AD have great potential for further research in the future.
Similar content being viewed by others
Background
Alzheimer’s disease is a prominent neurodegenerative disease characterized by the progressive loss of cognitive abilities and disorganization of basic functions, such as walking, talking, attention as well as memory [1]. The term describes a combination of clinical syndrome that is associated with a distinct neuropathological process bound by two hallmark features: cumulation of extracellular neurotic plaques composed of 42-amino acid amyloid-beta (Aβ1-42), a cleavage product of amyloid precursor protein (APP), and intracellular neurofibrillary tangles collections composed of hyper-phosphorylated species of the microtubule-associated protein tau (MAPT) [2]. Currently, AD is the 5th leading cause of mortality and affects around 44 million people worldwide [3]. Around two-thirds of those diagnosed with AD are women [4]. Cases of AD show a growing trend as the world population progresses [1,2,3]. Prevalence of AD increases with age by a percentage of 10–30% in those over 65 years old and the frequency doubles every 10 years after the age of 60 [5].
The conventional Food and Drug Administration (FDA) also approved treatments for AD rejuvenate cholinergic and glutamatergic neuronal function to reestablish cognitive regulation, but do not alter the underlying course of neurodegeneration itself [6]. AD is one of the least well-served drug treatments despite the high prevalence, only five therapeutic drugs are availably approved namely memantine, donepezil, galantamine, rivastigmine, and N-methyl-D-aspartate receptor antagonist [7]. Cholinesterase inhibitors (ChEIs) such as donepezil, galantamine and rivastigmine increase acetylcholine at brain synapses and have been proven clinically useful in the treatment [6]. Unfortunately, as AD is a progressive illness, patients treated with symptomatic drugs, such as ChEIs, will continue to decline [8]. A cohort study by Hong Xu found that long-term use of ChEIs is associated with progressive cognitive decline (0.18 MMSE points/year, CI 0.07, 0.28) [9].
Growth differentiation factor 11, a protein in transforming growth factor-β (TGF-β) superfamily of growth and differentiation factors, came to prominence in recent age-related researches [10]. It is found to decrease with age and progressive illness [11]. Research by Jacob et al., on individuals aged 60 and 75 years and over showed a significant difference in the concentration of GDF11 with age [12]. Interestingly, new findings have proven the regenerative factors of GDF11 in the brain [13], heart [14], skeletal muscle [15], kidney [16], bone [17], and skin [18]. More extensive studies found that the pro-proliferation and differentiation effects of systemically administrated GDF11 elevate the number of neural stem cells, improve vasculature in the subventricular zone and increase neuronal activity markers as well as plasticity in the hippocampus and cortex [19].
This review aims to highlight the therapeutic prospects of GDF11 in the management of Alzheimer’s disease.
Material and methods
The review method used is literature review. The literature references are of relevant journals from entrusted search engines PubMed and ScienceDirect with keywords such as “Alzheimer’s disease”, “angiogenesis”, “GDF11” and “neurogenesis”. The criteria of inclusion are that of all studies related to GDF11 therapeutics. Studies should be at least 10 years old. From 82 journals that are reviewed, 62 are found to be appropriate as reference for this paper. The evaluated information, analyzed for credibility and reliability, is assembled into one scientific literature review.
Pathophysiology of Alzheimer’s disease
The loss of synapses, dendrites and neurons found in AD is of consequence of abnormal amyloid-β in plaques and hyper-phosphorylated-tau in neurofibrillary tangles deposition [20]. These pathological hallmarks have a complex complementary association with the cholinergic lesion as the loss of cortical cholinergic innervation is found to be caused by the neurofibrillary tangles in the nucleus basalis of Meynert (NBM) [21, 22]. There is a long-established relationship between cholinergic abnormalities and amyloid-β pathology [23]. Research in post mortem AD patients has shown “diminishing responsiveness of the acetylcholine-synthesizing enzyme choline acetyltransferase with increasing neurotic plaques” [23]. The cholinergic depletion promotes amyloid-β deposition and tau pathology in paths that correlate to cognitive impairment [24].
Amyloid precursor protein is a single-pass transmembrane protein composed of a large ectodomain consisting of an intramembranous portion with a short intracellular tail and is expressed at high levels in the brain [25, 26]. In the non-amyloidogenic pathway, APP is cleaved by α- and γ-secretases producing neuro-protective solute peptide APPα [27]. However, cleavage via the β- and γ-secretases in the amyloidogenic pathway produces extraneural amyloid-β fragments leading to deposition (Fig. 1) [27, 28]. Furthermore, this notion is also congruent with finding from Dominici et al. which found increased levels of β2 microglobulin in AD patients compared to non-AD MCI and healthy controls (2063 ng/mL ± 852 versus 1613 ± 503 and 1832 ± 382 ng/mL, p < 0.001 and < 0.033, respectively) [29].
Deposition of extracellular amyloid-β into insoluble plaques in the brain is associated with the aggregation of protein tau into intracellular neurofibrillary tangles [30]. The decline of neuronal function and subsequent persistent progressive neurodegeneration are caused by the irreversible nature of pathological tau hyperphosphorylation in AD [31]. Increase of tau phosphorylation diminished microtubules affinity resulting in unusual levels of the unbound tau molecules increment [31]. Build-up of pre-tangles is followed by structural rearrangement involving the formation of the characteristic pleated β-sheet structures, subsequently forming neurofibrillary tangles by self-assemble [30,31,32]. Cytoskeletal microtubules disruption act as the imminent cause of progressive synaptic loss by interfering with axoplasmic as well as dendritic transport [33]. Therefore, starvation of the trophic support cells subsequently manifests as neural death and clinically as cognitive impairment [34].
Signaling cascade of GDF11
The signaling cascade (Fig. 2) is divided into canonical pathway and non-canonical pathway. The difference between these two pathways is the intracellular accumulation of β-catenin and the resulting translocation in the nucleus that regulates the expression of target genes in the canonical pathway. Meanwhile, in the non-canonical pathway, β-catenin-independent fully controls the expression of genes that are not affected by the nucleus [35]. In the canonical pathway, GDF11 signaling utilizes the canonical receptors and the small mothers against decapentaplegic (SMAD) proteins of TGF-β [36, 37]. The GDF11 dimer binds to the Activin Receptors type IIA or IIB (ActRIIA/B), serine/thionine kinase activity protein, and leads to the recruitment and transphosphorylation of Activin-Like Kinase receptors (ALK) 4, 5, or 7 [36, 38]. The transphosphorylated ALK activates the Receptor-regulated SMAD (R-SMAD) 2 and 3 [36, 39, 40]. The co-SMAD, SMAD4, is recruited by the R-SMAD dimer to form a trimeric complex that ultimately translocate to the nucleus to regulate gene expression [41]. In the non-canonical pathway, mitogen-activated protein kinases (MAPKs) are the main non-SMAD pathways activating protein kinase B (AKT) and c-Jun N-terminal kinase (JNK) routes [42]. Transforming growth factor-β-activated kinase 1 (TAK1), also known as MAPKKK7, has been shown to transduce the family via MEK6, a member of the p38 kinase cascade. [43]. The tumor necrosis factor receptor-associated factor (TRAF) 2 or 6 are involved in the activation of the TAK1 complex [43]. Finally, autophosphorylation of TAK1 activates the downstream targets, which include members of the MAPK and nuclear factor kappa B (NF-kB) signaling pathways [44]. Moreover, a study found that microRNA-125b-5p (miR-125b-5p) may play a role in neuroprotection in patient with ischemic stroke mediated by upregulated circularRNA-UCK2 (circUCK2) that was discovered to function as a sponge for miR-125b-5p, boosting the production of GDF11, which decreases neuronal damage and therefore contributes to neuroprotection. The role of miRNA is not directly in signaling the production of GDF11, but circUCK2 is able to inhibit the activity of miR-125b-5p, which increases GDF11 expression. [45]. This is supported by bioinformatics analysis which revealed that GDF11 is the target gene for miR-129-5p [46].
Recombinant GDF11 neurogenic properties
GDF11, a circulating protein present in the blood of young mammals has been shown to promote vascular remodeling and regeneration, as well as improving cognitive performance and synaptic plasticity in the elder mice [47]. The expression of GDF11 appears to be inversely linked to neurogenesis deterioration with age [48]. GDF11 was shown to be expressed in almost all neurons, astrocytes and ependymal cells in the brain and spinal cord, indicating that it may play a vital role [49].
Only recently that it has been found that GDF11 aids the temporal development of neurogenesis in the developing spinal cord [50]. In the hippocampus and cortex of old mice, GDF11 increased hippocampal neurogenesis and plasticity by increasing the number of neural stem cells and positively affects vasculature in the subventricular zone by exerting rejuvenating effects on brain endothelial cells [19, 49]. Changes in synaptic plasticity and neuron damage, present in AD, have been confirmed in a significant number of trials [51]. Neurons rely heavily on mitochondrial oxidative phosphorylation for energy production [52]. Apoptosis and inflammation are decreased after exogenous injection of rGDF11 as it protects mitochondria from oxidative stress [52, 53]. Production of the proinflammatory cytokine interleukin-18 by microglia was also slowly decreased upon rGDF11 administration, as was interleukin-15. It is found that GDF11 also reduces injuries of white matter and promotes presynaptic plasticity, which directly supports improvement in AD symptoms [12]. A study has found that GDF11 acts by activating central nervous system (CNS) active factors in vitro that induce endothelial cells and neurogenesis. It should be noted that GDF11 cannot penetrate the blood–brain barrier [19].
rGDF11 role in Alzheimer’s disease
Zhang et al. found that twice daily treatment with rGDF11 (0.1 mg/kg) improved cognition, had little effect on amyloid, increased vascular endothelial growth factor (VEGF) expression across brain blood vessels, increased blood vessel density and cerebral blood flow, reduced expression of inflammatory proteins (glial fibrillary acidic protein [GFAP] and ionized calcium-binding adaptor protein [Iba-1]) in the brain, and increased expression of vascular-related proteins in Alzheimer's mice [13]. This hypothesis is also supported by a study conducted by Lu et al., who observed an increase in peri-infarct cortex brain-derived neurotrophic factor (BDNF) in rGDF11 treatment. Significant increases were also observed in the proangiogenic factors Angiotensin-2 and VEGF receptor-2 phosphorylation in stroke-induced mice [57]. With its ability to increase angiogenesis, GDF11 plays a role in increasing cerebral vasculature which plays an important role in neurogenesis. This is evidenced by a study by Ceren, et.al., using mice in the hippocampus area that GDF11 increased blood vessel-occupied area, number of blood vessels, blood vessel branching. This finding was found in middle age-mice aged 22–23 months. In contrast to the 2- to 3-month-old test group that did not show any changes, which indicates that GDF11 exerts a broader influence on CNS function through changes in cerebral vasculature [19]. A similar study was conducted on 8- to 10-month-old rats induced by stroke. Investigation of angiogenesis was carried out 14 days after stroke and found an increase in BrdU+/CD31+ endothelial cells length and area, as well as significantly increased vascular branches. Tomato-lectin staining showed a similar effect, that the treatment with GDF11 significantly increased lectin-perfused vessel length and area around the peri-infarct cortical area of the test samples [57]. Another similar study also found a significant decrease in GFAP+ cells that decreased astrogliosis and decreased Iba-1+ cells that inhibit microglia activation. Another marker, CD31+ endothelial cells, has also been detected to have increased levels that support rapid angiogenesis [12]. Other than that, GDF11 therapy can decreased cerebral vascular Aβ in AD model mice. ELISAs for soluble and insoluble levels of Aβ40 and Aβ42 in the brain tissue and plasma show a lower Aβ40/Aβ42 ratio in GDF11-treated mice's brain tissue and plasma. In the same study also explained that gross insoluble Aβ42 was unaffected by western blot of prefrontal cortex tissue. There was also an increase in VEGF expression in the blood vessel walls which decreased plaque and density of Iba+ microglia cells [13]. Other than that, GDF11 as a molecule that can target vascular degradation, restore age-related loss in neurogenesis, and potentially alleviate cognitive dysfunction can be of great therapeutic value [58].
Experiments on rats by Ma et al., tested neurobehavioral levels through two tests using the modified neurological severity score (mNSS) test and the adhesive removal somatosensory test. Administration of rGDF11 injected on day 7 (first step) and day 14 (second step) showed good manifestations after mice were induced with right middle cerebral artery occlusion/reperfusion (MCAO/R) models. In the same study, phosphor-Smad2/3 and CD31 + levels were also tested and it was concluded that angiogenesis affects neuro behavioral prognostic improvement [59]. An experiment by Zhang et al., using mice, found that there was an increase in phosphorylated-Smad2/3 (phosphor-Smad2/3) in both the young age (1.5 months of age) and middle age (9 months of age). Immunofluorescence was performed on all three brain sections; cortex, dentate gyrus, and thalamus. There was a significant increase in the concentration of phospho-Smad2/3 in young age mice compared to the middle age group in rGDF11 treatment, which makes the therapeutic effect of rGDF11 promising as a preventive modality of AD [55, 60]. A study also found that GDF11 regulation could improve cognitive function and cerebrovascular function as a treatment in cerebral amyloid angiopathy (CAA) which is present in more than 90% of patients with AD. Intravenous administration of rGDF11 also enhances angiogenesis (marked by a significant increase in expression of the endothelial cell marker CD31+) in mice with AD complicated by CAA as seen by increased expression of VGEF/VGEFR, CD31, Collagen IV, and laminin [13]. Moreover, similar study reported that mice subject also showed decreased glial activation accompanied by a decrease in the ratio of A40/42 in brain parenchyma and lower expression of inflammation markers in the vasculature [61]. Another study using the same population setting was also found that GDF11 regulation associated with a lower damaged in intima and organelles in endothelial cells, such as mitochondria via VEGF pathway that serve a role in mediating specific cell death pathways [62].
Several studies targeting a variety of enzymes for the development of novel medicines to treat Alzheimer's disease have recently begun. In recent decades, there has been a growing emphasis on discovering new putative and unique protein or enzymatic targets for Alzheimer's disease with promising result. Some in vivo studies found that protein-based targeting such as GDF11 has shown a large benefit on Alzheimer’s including effect on neurogenesis, angiogenesis, brain perfusion, and cognitive function (Table 1). These results are achieved through the injection of GDF11 protein or receptor; or even by regulating protein transcription and translation using miRNA than mRNA. Based on previous evidence, GDF11 could be a novel therapeutic target protein for humans that focused as curative than preventive intervention. However, this approach is generally not to be administered as a monotherapy because of the complex and multi-faceted pathophysiology of Alzheimer's. Moreover, this kind of approach could be permanent and lifelong because it involves continuous drug administration to get optimal results and prevent disease recurrence. Studies and research are still needed to develop this method, including drug dosage, duration of therapy, presence or absence of mutation effects, and possible polypharmacy effects, as well as the costs required.
Conclusion
In our study, based on the reviews of several journals, recombinant GDF11 can be utilized to rejuvenate normal cognitive function of Alzheimer's patients' brains through its pro-neurogenesis and pro-angiogenesis properties. Moreover, its potential in maintaining the stability of neural progenitors makes rGDF11 act as a curative as well as a secondary preventive for neuronal damage in the brain. These results provide promising results for rGDF11 as AD therapy.
Availability of data and materials
Not applicable.
Abbreviations
- AD:
-
Alzheimer's disease
- Aβ:
-
Beta-amyloid
- GDF11:
-
Growth differentiation factor 11
- rGDF11:
-
Recombinant GDF11
- Aβ1-42:
-
42-Amino-acid amyloid-beta
- APP:
-
Amyloid precursor protein
- MAPT:
-
Microtubule-Associated Protein Tau
- FDA:
-
Food and Drug Administration
- ChEIs:
-
Cholinesterase inhibitors
- TGF-β:
-
Transforming growth factor-β
- NBM:
-
Nucleus basalis of Meynert
- SMAD:
-
Small mothers against decapentaplegic
- ActRIIA/B:
-
Activin Receptors type IIA or IIB
- ALK:
-
Activin-like kinase receptors
- MAPKs:
-
Mitogen-activated protein kinases
- AKT:
-
Protein kinase B
- JNK:
-
C-Jun N-terminal kinase
- TAK1:
-
Transforming growth factor-β-activated kinase 1
- TRAF:
-
Tumor necrosis factor receptor-associated factor
- NF-kB:
-
Nuclear factor kappa B
- miR-125b-5p:
-
MicroRNA-125b-5p
- circUCK2:
-
CircularRNA-UCK2
- CNS:
-
Central nervous system
- VEGF:
-
Vascular endothelial growth factor
- GFAP:
-
Glial fibrillary acidic protein
- Iba-1:
-
Ionized calcium-binding adaptor protein
- BDNF:
-
Brain-derived neurotrophic factor
- mNSS:
-
Modified neurological severity score
- MCAO/R:
-
Middle cerebral artery occlusion/reperfusion
- phosphor-Smad2/3:
-
Phosphorylated-Smad2/3
- CAA:
-
Cerebral amyloid angiopathy
References
Penney J, Ralvenius WT, Tsai L-H. Modeling Alzheimer’s disease with iPSC-derived brain cells. Mol Psychiatry. 2020;25:148–67.
Erkkinen MG, Kim M-O, Geschwind MD. Clinical neurology and epidemiology of the major neurodegenerative diseases. Cold Spring Harb Perspect Biol. 2018;10: a033118.
Dumurgier J, Sabia S. Epidemiology of Alzheimer’s disease: latest trends. Rev Prat. 2020;70:149–51.
Mielke MM. Sex and gender differences in Alzheimer’s disease dementia. Psychiatr Times. 2018;35:14–7.
Eratne D, Loi SM, Farrand S, Kelso W, Velakoulis D, Looi JC. Alzheimer’s disease: clinical update on epidemiology, pathophysiology and diagnosis. Aust Psychiatry Bull R Aust N Zeal Coll Psychiatr. 2018;26:347–57.
Hampel H, Mesulam M-M, Cuello AC, Farlow MR, Giacobini E, Grossberg GT, et al. The cholinergic system in the pathophysiology and treatment of Alzheimer’s disease. Brain. 2018;141:1917–33.
Cummings JL, Tong G, Ballard C. Treatment combinations for Alzheimer’s disease: current and future pharmacotherapy options. J Alzheimers Dis. 2019;67:779–94.
Hogan DB. Long-term efficacy and toxicity of cholinesterase inhibitors in the treatment of Alzheimer disease. Can J Psychiatry. 2014;59:618–23.
Xu H, Garcia-Ptacek S, Jönsson L, Anders W, Nordström P, Eriksdotter M. Long term effects of cholinesterase inhibitors on cognitive decline and mortality. Neurology. 2021. https://doi.org/10.1212/WNL.0000000000011832.
Idkowiak-Baldys J, Santhanam U, Buchanan SM, Pfaff KL, Rubin LL, Lyga J. Growth differentiation factor 11 (GDF11) has pronounced effects on skin biology. PLoS ONE. 2019;14:e0218035–e0218035.
Poggioli T, Vujic A, Yang P, Macias-Trevino C, Uygur A, Loffredo FS, et al. Circulating growth differentiation factor 11/8 levels decline with age. Circ Res. 2016;118:29–37.
Hudobenko J, Ganesh BP, Jiang J, Mohan EC, Lee S, Sheth S, et al. Growth differentiation factor-11 supplementation improves survival and promotes recovery after ischemic stroke in aged mice. Aging (Albany NY). 2020;12:8049–66.
Zhang W, Guo Y, Li B, Zhang Q, Liu JH, Gu GJ, et al. GDF11 Rejuvenates cerebrovascular structure and function in an animal model of Alzheimer’s disease. J Alzheimer’s Dis. 2018;62:807–19.
Loffredo FS, Steinhauser ML, Jay SM, Gannon J, Pancoast JR, Yalamanchi P, et al. Growth differentiation factor 11 is a circulating factor that reverses age-related cardiac hypertrophy. Cell. 2013;153:828–39.
Sinha M, Jang YC, Oh J, Khong D, Wu EY, Manohar R, et al. Restoring systemic GDF11 levels reverses age-related dysfunction in mouse skeletal muscle. Science. 2014;344:649–52.
Zhang Y, Li Q, Liu D, Huang Q, Cai G, Cui S, et al. GDF11 improves tubular regeneration after acute kidney injury in elderly mice. Sci Rep. 2016;6:34624.
Zhang Y, Shao J, Wang Z, Yang T, Liu S, Liu Y, et al. Growth differentiation factor 11 is a protective factor for osteoblastogenesis by targeting PPARgamma. Gene. 2015;557:209–14.
Rochette L, Mazini L, Meloux A, Zeller M, Cottin Y, Vergely C, et al. Anti-aging effects of GDF11 on skin. Int J Mol Sci. 2020;21:2598.
Ozek C, Krolewski RC, Buchanan SM, Rubin LL. Growth differentiation factor 11 treatment leads to neuronal and vascular improvements in the hippocampus of aged mice. Sci Rep. 2018;8:17293.
DeTure MA, Dickson DW. The neuropathological diagnosis of Alzheimer’s disease. Mol Neurodegener. 2019;14:32.
Ferreira-Vieira TH, Guimaraes IM, Silva FR, Ribeiro FM. Alzheimer’s disease: targeting the cholinergic system. Curr Neuropharmacol. 2016;14:101–15.
Mesulam M-M. Cholinergic circuitry of the human nucleus basalis and its fate in Alzheimer’s disease. J Comp Neurol. 2013. https://doi.org/10.1002/cne.23415.
Majdi A, Sadigh-Eteghad S, Rahigh Aghsan S, Farajdokht F, Vatandoust SM, Namvaran A, et al. Amyloid-β, tau, and the cholinergic system in Alzheimer’s disease: seeking direction in a tangle of clues. Rev Neurosci. 2020;31:391–413.
Ramos-Rodriguez JJ, Pacheco-Herrero M, Thyssen D, Murillo-Carretero MI, Berrocoso E, Spires-Jones TL, et al. Rapid β-amyloid deposition and cognitive impairment after cholinergic denervation in APP/PS1 mice. J Neuropathol Exp Neurol. 2013;72:272–85.
Galvão F, Grokoski KC, da Silva BB, Lamers ML, Siqueira IR. The amyloid precursor protein (APP) processing as a biological link between Alzheimer’s disease and cancer. Ageing Res Rev. 2019;49:83–91.
Coronel R, Bernabeu-Zornoza A, Palmer C, Muñiz-Moreno M, Zambrano A, Cano E, et al. Role of amyloid precursor protein (APP) and its derivatives in the biology and cell fate specification of neural stem cells. Mol Neurobiol. 2018;55:7107–17.
Menon P. The amyloid-β precursor protein (APP) and its adaptor protein Fe65: two key players in Alzheimer’s disease. Department of Biochemistry and Biophysics: Stockholm University; 2020.
Sun X, Chen W-D, Wang Y-D. β-Amyloid: the key peptide in the pathogenesis of Alzheimer’s disease. Front Pharmacol. 2015;6:221.
Dominici R, Finazzi D, Polito L, Oldoni E, Bugari G, Montanelli A, et al. Comparison of β2-microglobulin serum level between Alzheimer’s patients, cognitive healthy and mild cognitive impaired individuals. Biomarkers. 2018;23:603–8.
Lucey BP, Hicks TJ, McLeland JS, Toedebusch CD, Boyd J, Elbert DL, et al. Effect of sleep on overnight cerebrospinal fluid amyloid β kinetics. Ann Neurol. 2018;83:197–204.
Alonso AD, Beharry C, Corbo CP, Cohen LS. Molecular mechanism of prion-like tau-induced neurodegeneration. Alzheimer’s Dement. 2016;12:1090–7.
Wu X-L, Piña-Crespo J, Zhang Y-W, Chen X-C, Xu H-X. Tau-mediated neurodegeneration and potential implications in diagnosis and treatment of Alzheimer’s disease. Chin Med J (Engl). 2017;130:2978–90.
Fernandez-Valenzuela JJ, Sanchez-Varo R, Muñoz-Castro C, De Castro V, Sanchez-Mejias E, Navarro V, et al. Enhancing microtubule stabilization rescues cognitive deficits and ameliorates pathological phenotype in an amyloidogenic Alzheimer’s disease model. Sci Rep. 2020;10:14776.
Alonso AD, Cohen LS, Corbo C, Morozova V, ElIdrissi A, Phillips G, et al. Hyperphosphorylation of tau associates with changes in its function beyond microtubule stability. Front Cell Neurosci. 2018;12:338.
Ackers I, Malgor R. Interrelationship of canonical and non-canonical Wnt signalling pathways in chronic metabolic diseases. Diabetes Vasc Dis Res. 2018;15:3–13.
Jamaiyar A, Wan W, Janota DM, Enrick MK, Chilian WM, Yin L. The versatility and paradox of GDF 11. Pharmacol Ther. 2017;175:28–34.
Rahman MS, Akhtar N, Jamil HM, Banik RS, Asaduzzaman SM. TGF-β/BMP signaling and other molecular events: regulation of osteoblastogenesis and bone formation. Bone Res. 2015;3:15005.
Walker RG, Czepnik M, Goebel EJ, McCoy JC, Vujic A, Cho M, et al. Structural basis for potency differences between GDF8 and GDF11. BMC Biol. 2017;15:19.
Hata A, Chen Y-G. TGF-β signaling from receptors to smads. Cold Spring Harb Perspect Biol. 2016;8: a022061.
Gerardo-Ramírez M, Lazzarini-Lechuga R, Hernández-Rizo S, Jiménez-Salazar JE, Simoni-Nieves A, García-Ruiz C, et al. GDF11 exhibits tumor suppressive properties in hepatocellular carcinoma cells by restricting clonal expansion and invasion. Biochim Biophys Acta Mol Basis Dis. 2019;1865:1540–54.
Bajikar SS, Wang C-C, Borten MA, Pereira EJ, Atkins KA, Janes KA. Tumor-suppressor inactivation of GDF11 occurs by precursor sequestration in triple-negative breast cancer. Dev Cell. 2017;43:418-435.e13.
Wang Z, Dou M, Liu F, Jiang P, Ye S, Ma L, et al. GDF11 induces differentiation and apoptosis and inhibits migration of C172 neural stem cells via modulating MAPK signaling pathway. PeerJ. 2018;6: e5524.
Hindi SM, Sato S, Xiong G, Bohnert KR, Gibb AA, Gallot YS, et al. TAK1 regulates skeletal muscle mass and mitochondrial function. JCI Insight. 2018. https://doi.org/10.1172/jci.insight.98441.
Wang C, Deng L, Hong M, Akkaraju GR, Inoue J, Chen ZJ. TAK1 is a ubiquitin-dependent kinase of MKK and IKK. Nature. 2001;412:346–51.
Chen W, Wang H, Feng J, Chen L. Overexpression of circRNA circUCK2 attenuates cell apoptosis in cerebral ischemia-reperfusion injury via miR-125b-5p/GDF11 signaling. Mol Therapy Nucleic Acids. 2020;22:673–83.
Liu X, Deng X, Ding R, Cheng X, Jia J. Chondrocyte suppression is mediated by miR-129-5p via GDF11/SMAD3 signaling in developmental dysplasia of the hip. J Orthop Res Off Publ Orthop Res Soc. 2020;38:2559–72.
Villeda SA, Plambeck KE, Middeldorp J, Castellano JM, Mosher KI, Luo J, et al. Young blood reverses age-related impairments in cognitive function and synaptic plasticity in mice. Nat Med. 2014;20:659–63.
Rochette L, Vergely C. ‘Pro-youthful’ factors in the ‘labyrinth’ of cardiac rejuvenation. Exp Gerontol. 2016;83:1–5.
Hayashi Y, Mikawa S, Masumoto K, Katou F, Sato K. GDF11 expression in the adult rat central nervous system. J Chem Neuroanat. 2018;89:21–36.
Shi Y, Liu J-P. Gdf11 facilitates temporal progression of neurogenesis in the developing spinal cord. J Neurosci. 2011;31:883–93.
Koppensteiner P, Trinchese F, Fà M, Puzzo D, Gulisano W, Yan S, et al. Time-dependent reversal of synaptic plasticity induced by physiological concentrations of oligomeric Aβ42: an early index of Alzheimer’s disease. Sci Rep. 2016;6:32553.
Cenini G, Lloret A, Cascella R. Oxidative stress in neurodegenerative diseases: from a mitochondrial point of view. Oxid Med Cell Longev. 2019;2019:2105607.
Rochette L, Malka G. Neuroprotective potential of GDF11: myth or reality? Int J Mol Sci. 2019;20:3563.
Katsimpardi L, Litterman NK, Schein PA, Miller CM, Loffredo FS, Wojtkiewicz GR, et al. Vascular and neurogenic rejuvenation of the aging mouse brain by young systemic factors. Science. 2014;344:630–4.
Zhang M, Jadavji NM, Yoo H-S, Smith PD. Recombinant growth differentiation factor 11 influences short-term memory and enhances Sox2 expression in middle-aged mice. Behav Brain Res. 2018;341:45–9.
Finkenzeller G, Stark GB, Strassburg S. Growth differentiation factor 11 supports migration and sprouting of endothelial progenitor cells. J Surg Res. 2015;198:50–6.
Lu L, Bai X, Cao Y, Luo H, Yang X, Kang L, et al. Growth differentiation factor 11 promotes neurovascular recovery after stroke in mice. Front Cell Neurosci. 2018;12:205.
Katsimpardi L, Rubin LL. Young systemic factors as a medicine for age-related neurodegenerative diseases. Neurogenes (Austin, Tex). 2015;2:e1004971–e1004971.
Ma J, Zhang L, Niu T, Ai C, Jia G, Jin X, et al. Growth differentiation factor 11 improves neurobehavioral recovery and stimulates angiogenesis in rats subjected to cerebral ischemia/reperfusion. Brain Res Bull. 2018;139:38–47.
Zhang S, Cui W. Sox2, a key factor in the regulation of pluripotency and neural differentiation. World J Stem Cells. 2014;6:305–11.
Giannoni P, Arango-Lievano M, Das NI, Rousset M-C, Baranger K, Rivera S, et al. Cerebrovascular pathology during the progression of experimental Alzheimer’s disease. Neurobiol Dis. 2016;88:107–17.
Morin-Brureau M, Lebrun A, Rousset M-C, Fagni L, Bockaert J, de Bock F, et al. Epileptiform activity induces vascular remodeling and zonula occludens 1 downregulation in organotypic hippocampal cultures: role of VEGF signaling pathways. J Neurosci. 2011;31:10677–88.
Acknowledgements
Not applicable.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
BGL and WH contributed to literature mining and manuscript writing. IPEW supervised the project and edited the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
All authors have given their consent for publication.
Competing interests
There is no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
de Liyis, B.G., Halim, W. & Widyadharma, I.P.E. Potential role of recombinant growth differentiation factor 11 in Alzheimer’s disease treatment. Egypt J Neurol Psychiatry Neurosurg 58, 49 (2022). https://doi.org/10.1186/s41983-022-00487-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s41983-022-00487-5