Abstract
Background
Postoperative delirium is a common disorder in older adults that is associated with higher morbidity and mortality, prolonged cognitive impairment, development of dementia, higher institutionalization rates, and rising healthcare costs. The probability of delirium after surgery increases with patients’ age, with pre-existing cognitive impairment, and with comorbidities, and its diagnosis and treatment is dependent on the knowledge of diagnostic criteria, risk factors, and treatment options of the medical staff. In this study, we will investigate whether a cross-sectoral and multimodal intervention for preventing delirium can reduce the prevalence of delirium and postoperative cognitive decline (POCD) in patients older than 70 years undergoing elective surgery. Additionally, we will analyze whether the intervention is cost-effective.
Methods
The study will be conducted at five medical centers (with two or three surgical departments each) in the southwest of Germany. The study employs a stepped-wedge design with cluster randomization of the medical centers. Measurements are performed at six consecutive points: preadmission, preoperative, and postoperative with daily delirium screening up to day 7 and POCD evaluations at 2, 6, and 12 months after surgery. Recruitment goals are to enroll 1500 patients older than 70 years undergoing elective operative procedures (cardiac, thoracic, vascular, proximal big joints and spine, genitourinary, gastrointestinal, and general elective surgery procedures).
Discussion
Results of the trial should form the basis of future standards for preventing delirium and POCD in surgical wards. Key aims are the improvement of patient safety and quality of life, as well as the reduction of the long-term risk of conversion to dementia. Furthermore, from an economic perspective, we expect benefits and decreased costs for hospitals, patients, and healthcare insurances.
Trial registration
German Clinical Trials Register, DRKS00013311. Registered on 10 November 2017.
Similar content being viewed by others
Background
Delirium is associated with increased morbidity and mortality, cognitive impairment, dementia, and higher institutionalization rates [1]. The incidence of postoperative delirium (POD) depends on factors predisposing to delirium such as age, the presence of brain damage, dementia, deficits in cognitive, sensory, or mobility functions, multiple comorbidities, polypharmacy, and frailty [2]. Early indicators of cognitive deficits, including hyposmia [3], sleep disorders [4, 5], and subjective memory impairment [6, 7], are also relevant risk factors for delirium. The perioperative phase is a major trigger of postoperative delirium because of the administration of anesthesia, the surgical procedures, and other factors related to the operation itself, such as pain and immunological activation [2]. Postoperative cognitive dysfunction (POCD) often appears after POD [8, 9] and has been studied in relation to the preoperative status in order to measure the delirium’s impact, particularly on the risk of developing dementia [10], and in order to estimate the related health costs. POD and POCD are associated with higher mortality and postoperative complications (such as infections, falls, decubitus ulcers, incontinence) [9], with prolonged hospital stays [11], with the need for longer/extended intensive care and therapy and higher nursing workload burden [12], and with increased costs for both hospitals and healthcare insurance providers [2, 13].
Delirium is a healthcare quality indicator in older adults, and therefore delirium prevention is an essential parameter for patients’ safety [14, 15]. The incidence of delirium and its severity and duration can be significantly decreased and may be stratified by taking delirium risk factors into account [16]. Current guidelines for POD management [17] emphasize the importance of delirium prevention. A multimodal nonpharmacological approach [14, 18] is considered the best pathway [16, 19]. In a meta-analysis [20], this approach reduced the delirium risk by 53% (95% CI, 0.38 to 0.58) when comparing intervention and control groups.
For elective surgery, it is possible to implement a preadmission delirium prevention plan [21], adapting care to the patient’s age and delirium risk. However, surgical centers typically do not implement preadmission procedures for delirium risk assessment, and recommended interventions for the management of delirium are not standardized.
In this study, we will develop a cross-sectoral and “best practice” multimodal delirium prevention approach in five medical centers. The proposed multisectoral model for delirium prevention integrates and builds upon several multimodal admission models [16] with preadmission risk reduction counseling (“prehabilitation”), perioperative monitoring [22], and training based on international guides [17, 23] of multidisciplinary patient care providers, including operation room personnel, service staff, and families. The study will optimize delirium assessment, establish a cross-sectoral intervention bundle for preventing delirium, and evaluate the effectiveness and cost-efficiency of this all-encompassing approach. To this end, evidence-based delirium diagnoses, neuropsychological tests, and multimodal multiprofessional interventions will be implemented. Follow-up POCD evaluations will be performed 2, 6, and 12 months after surgery. Furthermore, relatives will be asked about their care burden, and a cross-sectoral analysis of the perioperative patient pathway will be performed.
The project, recruiting a total of 1500 patients, has the following objectives:
-
a)
The evaluation of the perioperative delirium prevalence with the I-Confusion Assessment Method-based scoring system for delirium diagnosis and delirium severity (I-CAM-S) [9], which is used for the first time in a large multicenter German sample.
-
b)
The implementation of a multisector, individualized, multiprofessional and multimodal delirium and POCD prevention program.
-
c)
The evaluation of the prevalence of POCD at 2 and 6 months after surgery, and the persistence of POCD after 12 months.
-
d)
The evaluation of changes in medication during the pre-admission and perioperative phases, especially with respect to avoidance of anticholinergic drugs and other pharmacologic agents associated with delirium.
-
e)
The evaluation of the care burden of the patients’ relatives.
-
f)
The economic evaluation of the multimodal intervention, studying its cost-effectiveness. From the point of view of the hospital departments, initial hospital costs will be evaluated. From the point of view of the health and care insurance company Allgemeine Ortskrankenkasse (AOK) Baden-Württemberg (Germany), inpatient and outpatient costs during the 12 months before and after the surgery will be analyzed in relation to outcome differences.
Methods
Design
We have designed a cross-sectoral longitudinal study that aims to include 1500 patients undergoing elective surgery. The study employs a stepped-wedge design with cluster randomization of five medical centers. The study will have seven periods, each lasting 12 weeks (see Fig. 1). The study will evaluate an all-encompassing “best practice” multimodal intervention for preventing delirium and POCD that includes six consecutive measurement points: preadmission, preoperative, and postoperative including daily delirium screening for 7 days after surgery and 2, 6, and 12 months after surgery. We aim to show that: the cross-sectoral multimodal and multidisciplinary intervention reduces the delirium rate by at least 40% compared with treatment as usual; the cross-sectoral multimodal and multidisciplinary intervention reduces the rate of postoperative cognitive decline by at least 20% compared with treatment as usual; and the cross-sectoral intervention, including the team training and the modules for nonpharmacological prevention, is cost-effective and therefore the improvement in quality of life imposes no additional costs because the care needs of the patients and caregivers are lower than with the standard treatment.
The study strategy is registered, constructed, and presented according to the recommendations of the Standard Protocol Items: Recommendations for Interventional Trials (SPIRIT) [24, 25] (see Additional file 1: SPIRIT checklist). The items from the World Health Organization Trial Registration Data Set are presented in Table 1.
Trial overview
The consortium leader will manage the project, oversee the financial transfers, monitor the progress according to the planned schedule, and communicate with the study sponsor Innovationsfonds des Gemeinsamen Bundesausschusses. The consortium leader is also part of the steering committee, whose main tasks are dealing promptly with the everyday project issues, monitoring the recruitment progress and the implementation of the intervention modules, and managing the study documentation. The members of the steering committee are also part of the project committee, which includes two members from each study site. The project committee accompanies the study and coordinates the joint publications as well as the requests for data analysis. If necessary, the project committee, based on interim analyses performed every 3 months, can decide on early termination of the project. Moreover, in its meetings every 6 months, the committee may deal with any relevant project issues. An international scientific advisory board of well-established professionals, including a geriatrician, an anesthetist, a gerontologist, and a delirium expert, ensures the scientific quality of the trial. The advisory board is comprised of four delirium and POCD experts. An external Regional Ethics and Data Monitoring Board (REDMB) includes national experts on delirium and POCD who are independent of the sponsor and trial investigators, and have no competing interests. They may be called upon to deal with ethically difficult issues, and they will also act as a monitoring board for adverse events (AEs). Furthermore, if the trial was to terminate early, the REDMB would take part in that decision.
Participants
Inclusion criteria
Eligible patients are aged 70 years or older and scheduled for elective surgery (cardiac, thorax, vessels, proximal large joints or spine, genitourinary, abdominal, or general elective surgery procedures) with a planned duration of surgery of at least 60 min (cut-to-suture time) under general, spinal, or regional anesthesia. As delirium is a high risk in dementia and frailty, we include patients with dementia or frailty who can consent to the trial or whose substitute decision-makers provide consent.
Exclusion criteria
Patients undergoing emergency surgery procedures, patients unable to consent due to insufficient mastery of the German language or with newly discovered severe dementia (red flag: Mini Mental State Examination (MMSE) < 15, Montreal Cognitive Assessment (MoCA) < 8) without a substitute decision-maker, patients with a poor clinical prognosis (expected survival of less than 15 months), and patients who have a long driving distance to the study site (> 120 km) are to be excluded from the trial.
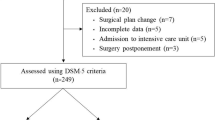
The recruitment procedure is described in Fig. 2. Patients who are not able to consent may also be recruited if the legal guardian consents to the patient’s study participation, given that such patients are especially at risk of developing delirium and POCD after surgery [10], and they could eminently benefit from the intervention.
Intervention
The intervention implements a cross-sectoral all-encompassing multimodal delirium prevention and management approach, and will be carried out in each study center after the center is randomized to take part in the intervention phase of the trial:
-
1.
All personnel training: within 4–6 weeks before the start of the intervention phase, nurses and therapeutic, medical, and support staff involved in the care of study patients will be trained with respect to dementia and delirium care, delirium diagnosis, and depression using a standardized training plan. Staff will be trained to three different levels of expertise: more than 70% of the staff are to receive basic training (90-min training time); more than 20% of nurses are to receive advanced training (“delirium scout” training—450-min training time); and more than 10% are to receive expert-level training (“delirium champion” training—900-min training time). Additionally, at least 70% of the physicians will receive 90 min extra of specific training about delirium risk, diagnosis, treatment, and prevention. The courses will be adjusted to the specific surgical and anesthesiological departments and special care units in order to ensure comparable levels of knowledge between different study sites.
-
2.
Environmental orientation support: the hospital environment will be adapted to the special needs of the patients. The decline of sensory function in older adults often leads to additional psychosocial stress, and is exacerbated by cognitive impairment. To address these issues, appropriate posters and signage will be placed on the wards, and in patients’ rooms and restrooms. Tools for temporal and situational orientation will be made available; for example, whiteboards with personal information, date, season, and year, as well as analog clocks that can be seen from the bed. Moreover, appropriate tools to prevent falls will be provided, such as anti-sliding socks. Special boxes for glasses, hearing aids, and dentures, as well as sleeping masks and ear plugs will be within reach of the patients at all times.
-
3.
Preadmission phase: the trained staff will implement some nonpharmacological preventive interventions in this phase, including informative talks and written recommendations for patients, and instructive contacts with the referring doctors regarding the age-appropriateness of prescribed medications and interventions.
-
4.
“Best practice” multimodal intervention: participants at the respective centers will receive perioperative and postoperative multimodal delirium prevention and care management between 8 a.m. and 8 p.m. on 7 days of the week, modified according to best practice models such as the Hospital Elder Life Program (HELP) [26], “The old patient in the surgery room” [22], or the Care of Confused Hospitalised Older Persons (CHOPs) [27]. Psychogeriatric nurses and one physician who have received 900 additional minutes of “delirium champion” training will form a multiprofessional consultation–liaison-like intervention team that will contact the patients and address their special needs daily. They will facilitate the implementation of the treatments advised in international delirium prevention guidelines [17, 23]: adaptation of surgery and anesthesia, medication and pain treatment appropriate for the patients’ age, pain monitoring, avoidance of movement restrictions such as catheters or infusions, and avoidance of benzodiazepines and anticholinergic drugs. These specialists will prescribe meaningful individualized daily activities for preventing delirium, defined in six modules: reorientation, cognitive activation, mobilization, meal companionship, clinical diagnostics and operation room attendance, and nonpharmacological sleep promotion and anxiety reduction. A team of nurses’ aides or volunteers (mostly gap-year social work volunteers) will carry out these activities, as well as chaperone patients during the diagnostic procedures, and in the operating and recovery rooms. They will receive 40 h of theoretical and practical training on the modules, and will be available daily in two shifts of 12 h per day.
-
5.
Patients and their family members will be advised individually about delirium risk and prevention, and will receive information materials (leaflets, posters, etc.) about delirium and the care service. Moreover, family members will provide individual information about the patient, facilitating individualized care and communication, and will be advised to support some individualized delirium prevention activities.
Given the patient-centered care research implementation goal of this study, the outcomes of patients undergoing the intervention will be compared to the outcomes of patients receiving treatment as usual (TAU) provided by the centers before the randomized start of the intervention.
Patient group involvement and staff involvement has been implemented in an earlier version of this intervention approach adapting the HELP (Hospital Elderly Life Program) structure (see [18]). In addition, we will implement focus groups at the general practitioner level post hospital stay to further evaluate patients’ perception of the intervention itself.
Adherence to intervention
The training modules are expected to play a fundamental role in improving adherence to the intervention protocols. They will be supplemented by additional talks, case discussions, and a web-based knowledge base providing webinars, training videos, and so forth. Moreover, a support system for the intervention teams will be established comprising an email service and a telephone hotline, as well as a data pool on a project server. Modules prescribed by the intervention team will be monitored, and the time span of the intervention will be daily documented. Furthermore, adherence to the manuals and “prescription checklists” will be tested by unannounced visits to every site.
Adverse events
Adverse events and serious adverse events (SAEs) will be recorded and documented. Falls, strokes, infections, and other severe perioperative complications (death, reoperation, pneumonia, sepsis) are to be expected in this patient group independently of the intervention, while SAEs related to the intervention are expected to be very rare. An example of a study-related SAE could be, for instance, a patient’s fall during early mobilization by the delirium companion during the active intervention phase. The feasibility of the project and the occurrence of SAEs will be assessed every 3 months by the REDMB, who will also carry out audits every year. In the case of substantial differences between the SAEs in the different groups, this will be discussed by the REDBM.
Withdrawal
The criteria for discontinuing the intervention for a participant will be death; or study withdrawal requested by the patient, guardian, or authorized relative; or (re)operation of more than 1 h (cut-to-suture time) during the first perioperative week, given that in this case a delirium or POCD cannot be precisely assigned to the first operation; or malignancy surgery with prognosis under 15 months, neoadjuvant chemotherapy, brain radiotherapy, or primary metastasis surgery for pancreas or bronchial cancer.
Outcome assessment
The assessment of all the outcomes will always be performed by trained assessors, who will be blinded for the intervention. Specifically, delirium raters will be told that the data will be used for validating a delirium risk score. Staff will be instructed not to reveal the nature of the intervention to these assessors.
The primary outcome will be delirium prevalence. It will be measured by daily delirium screening (I-Confusion Assessment Method-based scoring system for delirium severity (I-CAM)/CAM-S)) [28, 29] over 7 days after surgery and after 2 and 6 months, the Nursing Delirium Screening Scale (NuDESC) [30] (days 2 and 6 after surgery), a chart review at discharge applying the DSM-V delirium criteria as a reference standard [31], and the clinical evaluation.
The CAM [32], with its four-step diagnostic algorithm, is a widely used screening test for assessing delirium. Originally developed from the DSM-III-R, it is now predominantly used for delirium screening and research according to the DSM-IV and DSM-V criteria. It has been operationalized and translated into German [33], and then revealed a high sensitivity of 0.77 in a cohort of geriatric patients with a high prevalence dementia, and a specificity of 0.96–1.00 with excellent inter-rater reliability (Cohen’s κ = 0.95 (CI 0.74–1.0) for the algorithm, single item’s κ values varied between 0.5 and 1).
The I-CAM (I for ICD-10) [28] extends the German version of the original CAM adding abnormal psychomotor activity, to allow taking also the ICD-10 delirium diagnosis as a reference standard and assessing the motor delirium subtypes as well. The CAM-S [29] is a CAM-based scoring system for assessing delirium severity and was operationalized for use with the German version of the I-CAM. As the CAM might be confounded by the fluctuating nature of delirium, we use a chart-based review [31] filled out by trained medical staff at discharge to evaluate for fluctuations in sleep–wake rhythm or psychomotor activity indicating delirium.
The NuDESC is a five-item scale based on nurses’ observations assessing disorientation, inappropriate behavior and communication, hallucinations, and psychomotor retardation over a 24-h period. For the German version of the NuDESC, in a sample of patients after elective surgery, a sensitivity of 0.98, a specificity of 0.92, and an inter-rater reliability of 0.83 were observed [34].
The secondary outcomes will be: delirium duration as described in the primary outcome assessment; prevalence of POCD 2 and 6 months after surgery; and persistence of POCD after 12 months. The prevalence of POCD will be measured by the following neuropsychological test battery: the Montreal Cognitive Assessment (MoCA) [35], the digit span backwards [36], the Trail Making Test A and B (TMT A and B) [37], and cognitive performance measured with the continuous nonstandardized test values of these scales. A cognitive deficit is defined as the presence of a test value of ≤ 0.5 standard deviations, normalized for age, gender, and education, in one of these test procedures.
The MoCA is a brief cognitive screening test for assessing cognitive impairment among older people. The test assesses multiple cognitive domains including visuospatial ability, executive functions, memory, attention, language, abstraction, and orientation. The MoCA has high sensitivity (0.90) and specificity (0.87) to detect individuals with mild cognitive impairment and distinguish them from cognitively intact older people [35] and is available in three parallel versions.
The digit span backwards is commonly used to assess working memory capacity. Participants are required to recall a sequence of spoken digits in reverse order. For people older than 70 years, the digit span backwards had a test–retest reliability > 0.60 and an internal consistency of 0.882 [38].
The TMT is a widely used instrument in neuropsychological assessment that measures the speed of scanning and visuomotor tracking, divided attention, and cognitive flexibility [36]. The test consists of two parts, A and B. TMT A requires an individual to draw lines sequentially connecting consecutive numbers from 1 to 25. TMT B involves drawing a similar line, connecting an ascending sequence of numbers and letters in an alternating manner. In a sample of healthy older adults, Part A had a test–retest reliability of 0.78 and Part B of 0.73, and Part A an inter-rater reliability of 0.99 and Part B of 0.93 [39]. In a sample of elderly volunteers, Part B had a sensitivity of 0.63 for cognitive dysfunction, 0.72 for dementia, and 0.77 for AD, and a specificity of 0.89 [40].
For baseline assessment, the following variables will be evaluated. Basic sociodemographic patient information to be collected includes age, gender, weight, height, dominant hand, marital status, immigrant background, educational level, occupation, living arrangements, nicotine consumption, alcohol consumption, falls, and statutory level of care dependency. The self-reported subjective memory impairment (SMI) will be assessed, for which subjects will be asked “Do you feel that your memory is getting worse?” (no; yes; I don’t know). If the patient answers yes, the patient will then be asked whether he or she is worried about this (no; yes, that worries me; yes, that worries me very much; I don’t know, no answer) [41]. The personal medical history, including comorbidities, is to be quantified by the expanded version of the Charlson’s comorbidity Index (CCI) [42]. The patient’s preoperative physical status will be assessed by the American Society of Anesthesiologists Physical Status classification (ASA) [43]. The risk of stroke will be estimated with the CHA2DS2-VASc score (Congestive heart failure/left ventricular dysfunction, Hypertension, Age > 75, Diabetes, Stroke/transient ischemic attack/thromboembolism, Vascular disease, Age 65–74, Sex category) [44]. Laboratory results (hemoglobin, sodium, creatinine, total amount of protein, C-reactive protein), the history of delirium in the past, and a neurological examination will be recorded. The grip strength as a frailty marker will be measured with the Jamar® Hydraulic Hand Dynamometer. Hearing and visual integrity will be tested by the whisper and visual acuity tests [45]. Functional mobility and risk of falls will be investigated by the Timed Up and Go Test (TUG) [46]. Anxiety and depression will be assessed by the Patient Health Questionnaire (PHQ-4) [47]. The health-related quality of life will be measured by the EuroQol five dimensions questionnaire (EQ-5D-5 L) [48, 49] (this version includes five levels of severity in each of the existing five EQ-5D dimensions) and by the 12-Item Short Form Survey (SF-12) [50, 51]. Nutritional status will be assessed by the Mini Nutritional Assessment Short Form (MNA-SF) [52, 53]. Functional status will be evaluated with the Hamburg Classification Manual [54] version of the Barthel Index [55]. Frailty will be analyzed with the Clinical Frailty Scale of the Canadian Study of Health and Aging (CSHA Clinical Frailty Scale) [56]. Pain will be measured by the Numerical Rating Scale of Pain (NRS Pain) [57]. Sleeping behavior will be investigated by the Pittsburgh Sleep Quality Index—Basic (PSQI-Basic), a four-item version of the PSQI [58]. Sleep apnea will be screened for by the STOP-BANG questionnaire (Stop-BANG) [59]. Olfactory function will be scrutinized by the Sniffin’ Sticks 12 version [60]. Cognitive decline will be assessed by the very short version (seven items) of the Informant Questionnaire on Cognitive Decline in the Elderly (IQCODE) [61]. The subjective burden of the family caregivers will be measured by the German Zarit Burden interview (G-ZBI) [62, 63]. Classification as a geriatric patient, will be assessed with the Geriatric-Check using the geriatric concept of Baden-Württemberg (GC) [45]. Finally, the patient’s medications will be recorded, including the type, dose, and frequency of administration.
For planned analysis, the following variables are currently anticipated: anxiety and depression will be evaluated with the PHQ-4 questionnaire, the health-related quality of life with the EQ-5D-5 L questionnaire and the SF-12 survey, the nutrition status with the MNA-SF, the functional status with the Barthel Index, and the frailty with the CSHA Clinical Frailty Scale and hand grip. The duration and extent of use of physical restraints and patient care attendants will also be assessed. Moreover, the relevant aspects of behavior in daily life will be assessed by the Nurses’ Observation Scale for Geriatric Patients (NOSGER II) [64, 65], the presence of cognitive decline will be assessed by IQCODE evidenced by relatives, and the subjective burden of family caregivers by G-ZBI. The timelines are summarized in Fig. 3.
Standard Protocol Items: Recommendations for Interventional Trials figure of enrollment, intervention, and assessments. CSHA Clinical Frailty Scale of the Canadian Study of Health and Aging, EQ-5D-5L EuroQol five dimensions questionnaire, G-ZBI German Zarit Burden interview, I-CAM-S I-Confusion Assessment Method-based scoring system for delirium severity, IQCODE Informant Questionnaire on Cognitive Decline in the Elderly, MNA-SF Mini Nutritional Assessment Short Form, MoCA Montreal-Cognitive Assessment, NOSGER II Nurses’ Observation Scale for Geriatric Patients, NRS Pain Numerical Rating Scale of Pain, NuDESC Nursing Delirium Screening Scale, PHQ-4 Patient Health Questionnaire, PSQI (Basic) Pittsburgh Sleep Quality Index (Basic), RASS Richmond Agitation–Sedation Scale, SF-12 12-Item Short Form Survey, SMI subjective memory impairment, TMT Trail Making Test, V1/V2/V3 parallel versions of the MoCA, STOP BANG Sleep Apnea Questionnaire (snoring, tiredness, observed apnea, blood presure, body mass index, age, neck circunference, gender)
For planned validity assessment of postoperative delirium, the validity of the I-CAM-S and NuDESC vs the Richmond Agitation-Sedation Scale (RASS) [66] and vs chart review will be evaluated. The RASS is a simple observational scale that quantifies the level of consciousness, assessing both sedation and agitation.
For analysis of delirium severity, the duration and extent of restraints and one-to-one supervision requirements will be used, in addition to the CAM-S score.
For process analysis, acceptance and feasibility will be evaluated by qualitative assessment using focus groups formed by members of the geriatric centers.
For planned health-economic analyses, the initial hospital costs and the costs per delirium of two centers (Tübingen and Stuttgart) will be assessed. Moreover, for the patients whose health insurance is AOK Baden-Württemberg (Germany), health and care insurance expenditures and utilization will be assessed, in particular regarding hospital care, outpatient care, medication, rehabilitation, and nursing care. For a precise evaluation of the costs, the expense for training and staff carrying out the intervention will be included in the analyses.
Timelines
The study started in November 2017, and the recruitment phase will last until April 2019.
There will be three follow-up examinations after 2, 6, and 12 months, with the last planned for April 2020. We plan to complete the evaluations and cost analyses by December 2020.
From the patient’s perspective, the study will start with a preadmission screening (T0, at most 3 weeks before admission) (see Fig. 3). Admission (T1) will be followed by surgery and then daily delirium screening for 7 days (T2–T8) during hospitalization. A final discharge assessment (T9) will take place 1–8 days after surgery. If, at this point, the patient is considered to suffer from delirium, then delirium screening and monitoring will continue for another 2 weeks, so long as the patient remains hospitalized in the center. The discharge examination (T9) will take place, at the latest, 3 weeks after the elective surgery, with the participation of a physician who will note any postoperative complications. Follow-up assessments will be performed after 2 months (T10), 6 months (T11), and 12 months (T12). Moreover, the patient’s relatives will be asked at T12 about their care burden using the G-ZBI, and the cognitive state of the patient will be assessed using the IQCODE instrument. If a patient is unable or unwilling to go to the regional center for any follow-up assessment, the local PAWEL team will offer the assessment either at some hospital closer to the patient or at the patient’s general physician’s practice. If the patient is not able to go to any of these places, a team member will assess the patient at the patient’s home. Finally, if the patient refuses this option, he or she will be asked for a telephone interview.
Sample size
The power analysis for the primary outcome of delirium prevalence assumes a reduction in the outcome from 25% to 15% [20] as a result of the intervention. A conventional analysis to detect differences in proportions (delirium rate) between the intervention and control groups, using Fisher’s exact test, results in a total of 514 patients with a 1:1 randomization, given a power of 1 – β = 0.80 and an α error of 5%. Using the adjustment form proposed by Woertman et al. [67] with five crosspoints in a stepped-wedge design, with a maximum of 50 patients per cluster per period and an intracluster correlation of 0.01, leads to a correction factor for the stepped-wedge design of KF = 2.63, and therefore a number of 514 × 2.63 = 1351 patients. Assuming a dropout rate of 15%, this leads to a total requirement for about 750 patients per arm. The minimum number of clusters is given by the ratio of the total number of patients to the product between the number of crossing points and the patients per cluster per period, and is 15.
For the secondary outcomes, a reduction of the persistent cognitive deficit from 20% to 10% results in 428 patients using the conventional analysis with Fisher’s exact test and a 1:1 randomization, a power of 1 – β = 0.80, and an α error of 5%, which after the design correction leads to a requirement of 1079 patients.
Thus, the planned sample size is of at most 1500 patients (see Fig. 1 with the numbers per period). Furthermore, relatives of the patients will be asked about the burden of caring and the cognitive status of the patients.
Recruitment
The study takes place in Germany in the state of Baden-Württemberg. The study will be performed in university hospitals in Tübingen, Freiburg, and Ulm, and in tertiary care hospitals (one in Stuttgart and two in Karlsruhe). In total, five medical centers (one per city) with 12 surgical departments (three in Stuttgart and Tübingen, and two at the other centers) are included. To balance the surgical subspecialties per center, recruitment is restricted to a maximum of 2/3 from one of the following surgical subspecialties: orthopedics, vessels and cardiac, or abdominal. We intend to maintain this ratio for every center and for every 12-week interval of the study.
Patient recruitment will be carried out by a medical specialist. Study staff, including doctors and scientists, will provide the necessary information and obtain the written informed consent from the patients, and whenever possible also from one relative (to assess the caregiver burden and the cognitive status of the patient).
The medical directors and the managers of anesthesia and nursing at the hospitals included in the study have provided a letter of intent expressing their interest in introducing and evaluating preventive procedures, and their willingness to recruit the necessary number of patients. Hence, the recruiting objective is realistic. However, if a department fails to meet its recruitment target (17 patients for the departments in Stuttgart and Tübingen, 25 patients for the others) during one period, concrete and binding measures will be taken to reach the planned number of patients. In this case, the center will commit either to increase the recruitment in its departments or to include another surgical department. If several departments do not reach their target, then the five recruitment blocks, each lasting 3 months, will be extended to 4 months, adding 33% more time to recruit. In this case, for the patients recruited during the last period of the project, the POCD assessments would be completed after 6 months instead of after 12 months.
Randomization
Randomization will take place at the cluster level (k = 5 clusters) using a computer-generated sequence. Five months before starting the intervention in a given center, that center and the training team in Stuttgart will be informed about the allocation to prepare for the training and to form the intervention teams. Otherwise, randomization allocation will only be known to the consortium leader and the scientific staff at the University of Potsdam, who will implement the random sequence generation.
Data management
The collection of the clinical data during all stages of the study (preadmission, admission and postoperatively) will be performed exclusively by authorized staff of the study sites, using electronic Case Report Forms (eCRFs) via the web-based electronic data capture (EDC) system secuTrial® from interActive Systems GmbH. The access to the secuTrial® platform is protected by an authentication process, and the transmission of data between the study centers and the secuTrial® server is protected by a secure connection using Secure Sockets Layer (SSL) encryption. All collected data will be checked for reliability and validity every 3 months. Data access will be granted initially to project and data management and consortium leaders. All the data from scales and neuropsychological tests, as well as the clinical data and the data for the health-economic analysis, will be stored in a pseudonymized fashion. After the end of the study, all paper and electronic documents will be stored for at least 10 years more.
Statistical analysis
For the primary outcome, logistic regression analyses with cluster adjustment are planned.
For the secondary outcomes, the changes in the medication and the care burden of the patients’ relatives, we plan analyses using mixed linear and logistic regression models, with fixed and random factors for estimating heterogeneity over clusters [68].
Subgroup analyses for specific patient groups (e.g., patients with cardiac surgery regarding cognitive status or patients with brief hospital stays/brief surgeries) are planned.
For planned validity assessments of postoperative delirium, the validity of the I-CAM-S and NuDESC vs the RASS will be evaluated as screening tools for postoperative delirium. Diagnostic test performance of the tools will be evaluated by receiver operating characteristics (ROC) analysis.
Missing data (due to nonadherence of a department or a particular patient) will be documented. We will apply mixed-effect models, which handle the missing data without using any imputation method. Mixed-effect models assume that the missing data are missing at random (MAR); that is, when the probability that an outcome is missing is related to some other fully observable variable in the model, but not to the variable with the missing value itself [69].
Regarding the health-economic evaluation, a micro-costing analysis will be carried out using data from the clinical administration of two hospitals (Tübingen and Stuttgart). Moreover, for the patients insured by a specific health insurance (AOK Baden-Württemberg) who consent, the health and care insurance costs of the 12 months before and after surgery will be calculated using a difference-in-difference approach [70]. In this case, the target parameter is the cost per avoided POCD. The cost-effectiveness of the intervention will be calculated comparing the costs of the intervention group and the control group. In addition, quality-adjusted life years (QALYs) will then be calculated using data from the EQ-5D-5 L form about health-related quality of life, and applied for calculating the incremental cost-effectiveness. When possible, subgroup analyses will be carried out, for example, by age or gender, to determine whether cost-effectiveness is different in the corresponding groups. Sensitivity analyses will also be performed. The evaluation will be carried out following the recommendations of the “Good practice secondary data analysis” (GPS).
Dissemination policy
Publications about the results of the trial will be submitted to international journals after being approved by the project committee. Use of professional writers will not take place, and authorship eligibility criteria are specified in the trial contract and comply with International Committee of Medical Journal Editors (ICMJE) statements [71].
An analysis of the perioperative patient pathway will be developed as an outcome of the project. The goal of this analysis is to adapt the intervention to everyday care routine and to facilitate its subsequent implementation. To this end, doctors and other members of the geriatric centers will meet in 10 focus groups of 10 participants each. They will discuss exploratory questions about the needs and sensitivity to delirium and POCD, the knowledge about delirium, dementia, and depression, and other aspects of the study. To ensure the implementation of the results, they will be disseminated through workshops: at a training course; at the annual update on dementia (in cooperation with the medical association of Baden-Württemberg); and at the day of general medicine of the Institute of General Medicine and Interprofessional Care in Tübingen. A main result of the project will be a care pathway including information tools (e.g., flyers) and training modules for doctors and doctors’ assistants.
Ethics
This is an intervention study in which existing guidelines and recommendations will be implemented, including the S3 guideline of the German Society for Anesthesiology and Intensive Care Medicine (Deutsche Gesellschaft für Anästhesie und Intensivmedizin (DGAI)), the S3 guideline of the Working Group in Geriatric Traumatology (Arbeitsgemeinschaft Alterstraumatologie (AG Alterstraumatologie)) of the German Association of Trauma Surgery (Deutsche Gesellschaft für Unfallchirurgie (DGU)), the guidelines of the National Institute for Clinical Excellence (NICE), the guidelines of the American Geriatrics Society (AGS), and the guidelines of the Difficult Airway Society (DAS). Ethics approval according to the occupational regulations (Berufsordnung (BO)) has been obtained for all centers. All relevant changes will be communicated to the scientific advisory board, the Regional Ethics and Data Monitoring Board (REDMB), the relevant institutional review boards (IRBs), and the clinical trial registry. Given that there are no extra risks, the usual health insurance or civil liability will cover the risks of the trial, and there will be no additional medical liability insurance for the study. For the additional outpatient assessments, patients and their relatives will be covered by travel insurance.
In the preadmission assessments, it is to be expected that approximately 40% of the examined patients will have slight or severe cognitive impairment [72]. However, this does not necessarily restrict their capacity to consent or their legal capacity. Following Kim and Caine [73], we consider that this only occurs when transitioning to a more severe dementia (MMSE < 19). For those patients, the possible damage would be the self-stigmatization as a dementia-endangered person, but the benefit of the intervention would prevail because of its stipulated reduction of delirium and POCD.
On the other hand, if a previously unrecognized severe cognitive disorder was found, the patient probably could not consent, requiring consent from a substitute decision-maker.
Discussion
This study has several strong features. The study will determine the perioperative delirium prevalence, measured with I-CAM-S, for the first time in a large multicenter German sample. Despite its high prevalence and consequences, delirium is often underdiagnosed in hospitalized older adults. In particular, this is the case for hypoactive delirium because patients with this syndrome are often not disruptive [8]. To tackle this issue, we will use the five-item I-CAM, a useful diagnostic and screening tool for ICD-10 delirium that includes abnormal psychomotor activity and is sensitive for the detection of hypoactive delirium [28].
In addition, we will use a complementary chart review [31] to ascertain the detection of delirium beyond the established sensitivity and specificity of the I-CAM. While we cannot exclude disruptions of blinding of outcome assessors in this complex trial, we nevertheless attempted to ensure blinding of the assessors as much as was feasible in this trial.
Another advantage of the study is the development of a multisector, individualized, multiprofessional and multimodal delirium and POCD prevention program. There is now strong evidence indicating that such multicomponent interventions can prevent delirium in hospitalized patients, and indicating the importance of adequate training of the involved staff [16].
Another strength of the study is the design as a stepped-wedge cluster randomized controlled trial, which allows modeling of effects within and between sites of the delirium prevention and management program. Such evidence is of higher quality than results obtained from nonrandomized studies [74]. In addition, by using a stepped-wedge design, the intervention will be made available to all clusters by the end of the trial [75], avoiding the controversial situation in which control groups have no intervention.
The study will also investigate whether the intervention is cost-effective, so that the improvement of quality of life does not involve higher costs, and the care needs are lower than without the intervention. Given that delirium is highly multifactorial and is linked to many other common geriatric syndromes, it is expected that improving its diagnosis and treatment will be a very practical and effective strategy to improve outcomes, decrease costs, and raise the quality of the healthcare system wide [14].
Finally, the results of the study are intended to be a milestone for new German guidelines for the prevention and management of delirium in surgery, and for dealing with the frequent and insufficiently diagnosed POCD. In this way, the results of an elective operation will be better, the patient safety and quality of life will be improved, and the long-term risk of dementia will be minimized. Furthermore, from an economic perspective, diagnosing cognitive deficits early and minimizing POD and POCD should be beneficial for patients, caregivers, hospitals, and healthcare insurances.
Trial status
Recruitment commenced in November 2017.
Abbreviations
- AE:
-
Adverse event
- AG:
-
Arbeitsgemeinschaft (working group)
- AGS:
-
American Geriatrics Society
- AOK:
-
Allgemeine Ortskrankenkasse (public health insurance company)
- ASA:
-
American Society of Anesthesiologists Physical Status classification
- BO:
-
Berufsordnung (Professional Code of Conduct)
- CAM-S:
-
CAM-based scoring system for assessing delirium severity
- CCI:
-
Charlson’s comorbidity index
- CHA2DS2-VASc:
-
Congestive heart failure/left ventricular dysfunction, Hypertension, Age > 75, Diabetes, Stroke/transient ischemic attack/thromboembolism, Vascular disease, Age 65–74, Sex category
- CHOPs:
-
Care of Confused Hospitalised Older Persons
- CSHAClinical Frailty Scale:
-
Clinical Frailty Scale of the Canadian Study of Health and Aging
- DAS:
-
Difficult Airway Society
- DGAI:
-
Deutsche Gesellschaft für Anästhesie und Intensivmedizin (German Society for Anesthesiology and Intensive Care Medicine)
- DGU:
-
Deutsche Gesellschaft für Unfallchirurgie (German Association of Trauma Surgery)
- eCRF:
-
Electronic Case Report Form
- EDC:
-
Electronic data capture
- EQ-5D-5 L:
-
EuroQol five dimensions questionnaire
- G-BA:
-
Gemeinsame Bundesausschuss (Federal Joint Committee)
- GC:
-
Geriatric-Check
- GPS:
-
Good practice secondary data analysis
- G-ZBI:
-
German Zarit Burden interview
- HELP:
-
Hospital Elder Life Program
- I-CAM:
-
I-Confusion Assessment Method
- ICMJE:
-
International Committee of Medical Journal Editors
- IQCODE:
-
Informant Questionnaire on Cognitive Decline in the Elderly
- IRBs:
-
Institutional review boards
- MAR:
-
Missing at random
- MMSE:
-
Mini Mental State Examination
- MNA-SF:
-
Mini Nutritional Assessment Short Form
- MoCA:
-
Montreal Cognitive Assessment
- NICE:
-
National Institute for Clinical Excellence
- NOSGER II:
-
Nurses’ Observation Scale for Geriatric Patients
- NRS Pain:
-
Numerical Rating Scale of Pain
- NuDESC:
-
Nursing Delirium Screening Scale
- POCD:
-
Postoperative cognitive dysfunction
- POD:
-
Postoperative delirium
- PSQI-Basic:
-
Pittsburgh Sleep Quality Index—Basic
- QALY:
-
Quality-adjusted life year
- RASS:
-
Richmond Agitation–Sedation Scale
- REDMB:
-
Regional Ethics and Data Monitoring Board
- ROC:
-
Receiver operating characteristics
- SAE:
-
Serious adverse event
- SF-12:
-
12-Item Short Form Survey
- SMI:
-
Subjective memory impairment
- SPIRIT:
-
Standard Protocol Items: Recommendations for Interventional Trials
- Stop-BANG:
-
STOP-BANG questionnaire
- TAU:
-
Treatment as usual
- TMT A and B:
-
Trail Making Test A and B
- TUG:
-
Timed Up and Go
References
Witlox J, Eurelings LS, de Jonghe JF, Kalisvaart KJ, Eikelenboom P, Van Gool WA. Delirium in elderly patients and the risk of postdischarge mortality, institutionalization, and dementia: a meta-analysis. JAMA. 2010;304(4):443–51.
Guenther U, Riedel L, Radtke FM. Patients prone for postoperative delirium: preoperative assessment, perioperative prophylaxis, postoperative treatment. Curr Opin Anaesthesiol. 2016;29(3):384–90.
Brown CH, Morrissey C, Ono M, Yenokyan G, Selnes OA, Walston J, et al. Impaired olfaction and risk of delirium or cognitive decline after cardiac surgery. J Am Geriatr Soc. 2015;63(1):16–23.
Todd O, Gellrich L, Maclullich A, Driessen M, Thomas C, Kreisel S. Sleep disruption at home as an independent risk factor for postoperative delirium. JAGS J Am Geriatr Soc. 2017;65(5):949–57.
Patel J, Baldwin J, Bunting P, Laha S. The effect of a multicomponent multidisciplinary bundle of interventions on sleep and delirium in medical and surgical intensive care patients. Anaesthesia. 2014;69(6):540–9.
Hagen K, Ehlis AC, Haeussinger FB, Beeretz S, Kromer GV, Heinzel S, et al. The relation of SMI and the VSEP in a risk sample for neurodegenerative disorders. J Neural Transm (Vienna). 2015;122(8):1167–74.
Jessen F, Wolfsgruber S, Wiese B, Bickel H, Mösch E, Kaduszkiewicz H, et al. AD dementia risk in late MCI, in early MCI, and in subjective memory impairment. Alzheimers Dement. 2014;10(1):76–83.
Monk TG, Price CC. Postoperative cognitive disorders. Curr Opin Crit Care. 2011;17(4):376–81.
Rundshagen I. Postoperative cognitive dysfunction. Dtsch Arztebl Int. 2014;111(8):119–25.
Fong TG, Davis D, Growdon ME, Albuquerque A, Inouye SK. The interface between delirium and dementia in elderly adults. Lancet Neurol. 2015;14(8):823–32.
Visser L, Prent A, van der Laan MJ, van Leeuwen BL, Izaks GJ, Zeebregts CJ, et al. Predicting postoperative delirium after vascular surgical procedures. J Vasc Sur. 2015;62(1):183–9.
Pretto M, Spirig R, Milisen K, Degeest S, Regazzoni P, Hasemann W. Effects of an interdisciplinary nurse-led Delirium Prevention and Management Program (DPMP) on nursing workload: a pilot study. Int J Nurs Stud. 2009;46(6):804–12.
Gleason LJ, Schmitt EM, Kosar CM, Tabloski P, Saczynski JS, Robinson T, et al. Effect of delirium and other major complications on outcomes after elective surgery in older adults. JAMA surg. 2015;150(12):1134–40.
Inouye SH, Westendorp RGJ, Saczynski JS. Delirium in older people. Lancet. 2014;383(9920):911–22.
Reston JT, Schoelles KM. In-facility delirium prevention programs as a patient safety strategy: a systematic review. Ann Intern Med. 2013;158(5 Pt 2):375–80.
Siddiqi N, Harrison JK, Clegg A, Teale EA, Young J, Taylor J, et al. Interventions for preventing delirium in hospitalised non-ICU patients. Cochrane Database Syst Rev. 2016;3:CD005563.
Inouye SK, Robinson T, Blaum C, Busby-Whitehead J, Boustani M, Chalian A, et al. Postoperative delirium in older adults: best practice statement from the American Geriatrics Society. J Am Coll Surg. 2015;220(2):136–48.
Bringemeier J, Thomas C, Guhra M, Kreisel S. HELP zur Vermeidung von Delirien. Psych Up2date. 2015;9(03):137–48.
Zhang H, Lu Y, Liu M, Zou Z, Wang L, Xu FY, et al. Strategies for prevention of postoperative delirium: a systematic review and meta-analysis of randomized trials. Crit Care. 2013;17(2):R47.
Hshieh TT, Yue J, Oh E, Puelle M, Dowal S, Travison T, et al. Effectiveness of multicomponent nonpharmacological delirium interventions: a meta-analysis. JAMA Intern Med. 2015;175(4):512–20.
Yang FM, Inouye SK, Fearing MA, Kiely DK, Marcantonio ER, Jones RN. Participation in activity and risk for incident delirium. J Am Geriatr Soc. 2008;56(8):1479–84.
Gurlit S, Möllmann M. How to prevent perioperative delirium in the elderly? Z Gerontol Geriatr und Geriatrie. 2008;41(6):447–52.
Barr J, Fraser GL, Puntillo K, Ely EW, Gélinas C, Dasta JF, et al. Clinical practice guidelines for the management of pain, agitation, and delirium in adult patients in the intensive care unit. Crit Care Med. 2013;41(1):263–306.
Chan AW, Tetzlaff JM, Altman DG, Dickersin K, Moher D. SPIRIT 2013: new guidance for content of clinical trial protocols. Lancet. 2013;381(9861):91–2.
Chan AW, Tetzlaff JM, Gøtzsche PC, Altman DG, Mann H, Berlin JA, et al. SPIRIT 2013 explanation and elaboration: guidance for protocols of clinical trials. BMJ. 2013;346:e7586.
Inouye SK, Bogardus ST Jr, Baker DI, Leo-Summers L, Cooney LM Jr. The Hospital Elder Life Program: a model of care to prevent cognitive and functional decline in older hospitalized patients. Hospital Elder Life Program. J Am Geriatr Soc. 2000;48(12):1697–706.
Caplan GA, Kurrle SE, Cumming A. Appropriate care for older people with cognitive impairment in hospital. Med J Aust. 2016;205(10):Suppl:12–5.
Thomas C, Kreisel SH, Oster P, Driessen M, Arolt V, Inouye SK. Diagnosing delirium in older hospitalized adults with dementia: adapting the confusion assessment method to international classification of diseases, tenth revision, diagnostic criteria. J Am Geriatr Soc. 2012;60(8):1471–7.
Inouye SK, Kosar CM, Tommet D, Schmitt EM, Puelle MR, Saczynski JS, et al. The CAM-S: development and validation of a new scoring system for delirium severity in 2 cohorts. Ann Intern Med. 2014;160(8):526–33.
Gaudreau JD, Gagnon P, Harel F, Tremblay A, Roy MA. Fast, systematic, and continuous delirium assessment in hospitalized patients: the nursing delirium screening scale. J Pain Symptom Manag. 2005;29(4):368–75.
Inouye SK, Leo-Summers L, Zhang Y, Bogardus ST Jr, Leslie DL, Agostini JV. A chart-based method for identification of delirium: validation compared with interviewer ratings using the confusion assessment method. J Am Geriatr Soc. 2005;53(2):312–8.
Inouye SK, van Dyck CH, Alessi CA, Balkin S, Siegal AP, Horwitz RI. Clarifying confusion: the Confusion Assessment Method. A new method for detection of delirium. Ann Intern Med. 1990;113(12):941–8.
Hestermann U, Backenstrass M, Gekle I, Hack M, Mundt C, Oster P, et al. Validation of a German version of the Confusion Assessment Method for delirium detection in a sample of acute geriatric patients with a high prevalence of dementia. Psychopathology. 2009;42(4):270–6.
Radtke FM, Franck M, Schust S, Boehme L, Pascher A, Bail HJ, et al. A comparison of three scores to screen for delirium on the surgical ward. World J Surg. 2010;34(3):487–94.
Nasreddine ZS, Phillips NA, Bédirian V, Charbonneau S, Whitehead V, Collin I, et al. The Montreal Cognitive Assessment, MoCA: a brief screening tool for mild cognitive impairment. J Am Geriatr Soc. 2005;53(4):695–9.
Lezak MD, Howieson DB, Loring D. Orientation and attention. In: Lezak MD, Howieson DB, Loring D, editors. Neuropsychological assessment. 4th ed. New York: Oxford University Press; 2004. p. 337–74.
AITB. Army Individual Test Battery. Manual of directions and scoring. Washington, DC: War Department, Adjutant General’s Office; 1944.
Waters GS, Caplan D. The reliability and stability of verbal working memory measures. Behav Res Methods Instrum Comput. 2003;35(4):550–64.
Cangoz B, Karakoc E, Selekler K. Trail Making Test: normative data for Turkish elderly population by age, sex and education. J Neurol Sci. 2009;283(1–2):73–8.
Rasmusson XD, Zonderman AB, Kawas C, Resnick SM. Effects of age and dementia on the Trail Making Test. Clin Neuropsychol. 1998;12(2):169–78.
Geerlings MI, Jonker C, Bouter LM, Adèr HJ, Schmand B. Association between memory complaints and incident Alzheimer’s disease in elderly people with normal baseline cognition. Am J Psychiatry. 1999;156(4):531–7.
Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40(5):373–83.
Wolters U, Wolf T, Stützer H, Schröder T. ASA classification and perioperative variables as predictors of postoperative outcome. Br J Anaesth. 1996;77(2):217–22.
Lip GY, Nieuwlaat R, Pisters R, Lane DA, Crijns HJ. Refining clinical risk stratification for predicting stroke and thromboembolism in atrial fibrillation using a novel risk factor-based approach: the euro heart survey on atrial fibrillation. Chest. 2010;137(2):263–72.
Ministerium für Soziales und Integration Baden-Württemberg. Aktualisierter Anhang zum Geriatriekonzept Baden-Württemberg 2014. Ministerium für Soziales und Integration Baden-Württemberg 2016. https://sozialministerium.baden-wuerttemberg.de/fileadmin/redaktion/m-sm/intern/downloads/Publikationen/Geriatriekonzept_2014_Anhang_2016.pdf. Accessed 1 Jan 2018.
Podsiadlo D, Richardson S. The timed “Up and Go” test: a test of basic functional mobility for frail elderly persons. J Am Geriatr Soc. 1991;39(2):142–8.
Kroenke K, Spitzer RL, Williams JB, Löwe B. An ultra-brief screening scale for anxiety and depression: the PHQ-4. Psychosomatics. 2009;50(6):613–21.
Herdman M, Gudex C, Lloyd A, Janssen MF, Kind P, Parkin D, et al. Development and preliminary testing of the new five-level version of EQ-5D (EQ-5D-5L). Qual Life Res. 2011;20(10):1727–36.
Hinz A, Kohlmann T, Stöbel-Richter Y, Zenger M, Brähler E. The quality of life questionnaire EQ-5D-5L: psychometric properties and normative values for the general German population. Qual Life Res. 2014;23(2):443–7.
Ware JE Jr, Kosinski M, Keller SD. A 12-Item Short-Form Health Survey: construction of scales and preliminary tests of reliability and validity. Med Care. 1996;34(3):220–33.
Gandek B, Ware JE, Aaronson NK, Apolone G, Bjorner JB, Brazier JE, et al. Cross-validation of item selection and scoring for the SF-12 Health Survey in nine countries: results from the IQOLA Project. J Clin Epidemiol. 1998;51(11):1171–8.
Rubenstein LZ, Harker JO, Salvà A, Guigoz Y, Vellas B. Screening for undernutrition in geriatric practice: developing the Short-Form Mini-Nutritional Assessment (MNA-SF). J Gerontol A Biol Sci Med Sci. 2001;56(6):M366–72.
Kaiser M, Bauer JM, Ramsch C, Uter W, Guigoz Y, Cederholm T, et al. Validation of the Mini Nutritional Assessment Short-Form (MNA®-SF): a practical tool for identification of nutritional status. J Nutr Health Aging. 2009;13(9):782–8.
Lübke N, Meinck M, von Renteln-Kruse W. Der Barthel-Index in der Geriatrie. Eine Kontextanalyse zum Hamburger Einstufungsmanual. Z Gerontol Geriatr. 2004;37(4):316–26.
Mahoney FI, Barthel D. Functional evaluation: the Barthel Index. Md State Med J. 1965;14:61–5.
Rockwood K, Song X, MacKnight C, Bergman H, Hogan DB, McDowell I, et al. A global clinical measure of fitness and frailty in elderly people. CMAJ. 2005;173(5):489–95.
Hawker GA, Mian S, Kendzerska T, French M. Measures of adult pain: Visual Analog Scale for Pain (VAS Pain), Numeric Rating Scale for Pain (NRS Pain), McGill Pain Questionnaire (MPQ), Short-Form McGill Pain Questionnaire (SF-MPQ), Chronic Pain Grade Scale (CPGS), Short Form-36 Bodily Pain Scale (SF-36 BPS), and Measure of Intermittent and Constant Osteoarthritis Pain (ICOAP). Arthritis Care Res. 2011;63(Suppl 11):240–52.
Buysse DJ, Reynolds CF, Monk TH, Berman SR, Kupfer DJ. The Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res. 1989;28(2):193–213.
Chung F, Yegneswaran B, Liao P. STOP questionnaire: a tool to screen patients for obstructive sleep apnea. Anesthesiology. 2008;108(5):812–21.
Kobal G, Hummel TH, Sekinger B, Barz S, Roscher S, Wolf S. “Sniffin'sticks”: screening of olfactory performance. HNO. 1996;34(4):222–6.
Ehrensperger MM, Berres M, Taylor KI, Monsch AU. Screening properties of the German IQCODE with a two-year time frame in MCI and early Alzheimer's disease. Int Psychogeriatr. 2010;22(1):91–100.
Zarit SH, Reever KE, Bach-Peterson J. Relatives of the impaired elderly: correlates of feelings of burden. Gerontologist. 1980;20(6):649–55.
Braun M, Scholz U, Hornung R, Martin M. The burden of spousal caregiving: a preliminary psychometric evaluation of the German version of the Zarit Burden Interview. Aging Ment Health. 2010;14(2):159–67.
Brunner C, Spiegel R. Eine Validierungsstudie mit der NOSGER (Nurses’ Observation Scale for Geriatric Patients), einem neuen Beurteilungsinstrument für die Psychogeriatrie. Z Klin Psychol. 1990;19(3):211–29.
Spiegel R, Brunner C, Ermini-Fünfschilling D, Monsch A, Notter M, Puxty J, et al. A New Behavioral Assessment Scale for Geriatric Out-and In-Patients: the NOSGER (Nurses’ Observation Scale for Geriatric Patients). J Am Geriatr Soc. 1991;39(4):339–47.
Sessler CN, Gosnell MS, Grap MJ, Brophy GM, O'neal PV, Keane KA, et al. The Richmond Agitation-Sedation Scale: validity and reliability in adult intensive care unit patients. Am J Respir Crit Care Med. 2002;166(10):1338–44.
Woertman W, de Hoop E, Moerbeek M, Zuidema SU, Gerritsen DL, Teerenstra S. Stepped wedge designs could reduce the required sample size in cluster randomized trials. J Clin Epidemiol. 2013;66(7):752–8.
Rapp MA, Mell T, Majic T, Treusch Y, Nordheim J, Niemann-Mirmehdi M, et al. Agitation in nursing home residents with dementia (VIDEANT trial): effects of a cluster-randomized, controlled, guideline implementation trial. J Am Med Dir Assoc. 2013;14(9):690–5.
Garcia TP, Marder K. Statistical approaches to longitudinal data analysis in neurodegenerative diseases: Huntington's disease as a model. Curr Neurol Neurosci Rep. 2017;17(2):14.
van Asselt AD, van Mastrigt GA, Dirksen CD, Arntz A, Severens JL, Kessels AG. How to deal with cost differences at baseline. PharmacoEconomics. 2009;27(6):519–28.
International Committee of Medical Journal Editors. Defining the role of authors and contributors. http://www.icmje.org/recommendations/browse/roles-and-responsibilities/defining-the-role-of-authors-and-contributors.html. Accessed 1 May 2018.
Hendlmeier I, Bickel H, Hessler JB, Weber J, Junge MN, Leonhardt S, et al. Demenzsensible Versorgungsangebote im Allgemeinkrankenhaus: Repräsentative Ergebnisse aus der General Hospital Study (GHoSt) [Dementia friendly care services in general hospitals: Representative results of the general hospital study (GHoSt)]. Z Gerontol Geriatr. 2018;51(5):509–16.
Kim SY, Caine ED. Utility and limits of the mini mental state examination in evaluating consent capacity in Alzheimer's disease. Psychiatr Serv. 2002;53(10):1322–4.
Hargreaves JR, Copas AJ, Beard E, Osrin D, Lewis JJ, Davey C, et al. Five questions to consider before conducting a stepped wedge trial. Trials. 2015;16:350.
Grayling MJ, Wason JM, Mander AP. Stepped wedge cluster randomized controlled trial designs: a review of reporting quality and design features. Trials. 2017;18(1):33.
Acknowledgements
The following people are instrumental in data acquisition at the sites: University Hospital Tübingen, Tübingen, Germany—Andreas Kirschniak (Department of Visceral Surgery); Marvin Metzner, Oksana Forkavets, Christian Mychajliw, Susanne Yuki Schneider, Rita Binder, Annette Schroth, Marlen Brachthäuser, and Cindy Boden (Department of Psychiatry and Psychotherapy); Andrea Albrecht (Nursing Department); and Laura Bertram (Institute for General Practice and Interprofessional Care). Klinikum Stuttgart, Stuttgart, Germany—Thomas Hupp (Department of Vascular Surgery and Vascular Medicine and Transplant Surgery); Joerg Koeninger (Department of General, Visceral, Thoracic and Transplant Surgery); Christian Knop (Department of Trauma Surgery and Orthopaedics); Christian Humke (Department of Urological and Transplant Surgery); Oliver Ganslandt (Department of Neurosurgery and Spine Surgery); Katrin Markgräfe-Weisser, Irina Tkacenko, Kathrin Wunder, Peter Stark, Robert Gerz, Larissa Nürk, Janosch Fox, Lorenz Sutter and Maike Kleine-Katthöfer (Department of Old Age Psychiatry and Psychotherapy); Stefan Blumenrode (Psychiatric Nurses‘ Qualification Institute); Carola Bruns, Juliane Spank, Sarah Weller, and Eva Mennig (Department of Old Age Psychiatry and Psychotherapy) contributed to the development of the different training curricula for all staff, intervention teams, and nurses’ aides. University of Freiburg, Freiburg, Germany—Norbert P. Südkamp and Gunnar Ochs (Department of Orthopedics and Trauma Surgery); Stefan Fichtner-Feigl (Department of General and Visceral Surgery); Hartmut Bürkle (Department of Anesthesiology and Critical Care); Markus Martin (Department of Neurology and Neurophysiology); Jonas Hoch, Marina Gimbel, Anna Groß, and Damian Sommer (Medical Center). University Hospital Ulm, Ulm, Germany—Christoph Leinert, Cynthia Vázquez, and Jill Holbrook (Department of Neurology); Cornelia Ribeill (Department for Orthopedics); Udo Wihlenda (Nursing Department); Marius Sabau and Natalie Waldherr (Department of Cardiothoracic and Vascular Surgery); Dhayana Dallmeier, Clara Dettlinger, and Patrick Frey (Agaplesion Bethesda Clinic, Geriatric Medicine, Ulm University and Geriatric Center Ulm); and Helene Maucher (University and Rehabilitation Hospital Ulm). Karlsruhe, Germany—Jan Gerhardus, Zvjezdana Peric, Julia Pieloth, Saifullah Abubaker, Naser Ghaffari, Christine Neuber, and Adel Yunes (Helios Clinic for Heart Surgery); Natalie Dodkiewicz, Janine Kistner, and Elke Wächter (Geriatric Center Karlsruhe, ViDia Christian Clinics Karlsruhe). AOK Baden-Württemberg, Stuttgart, Germany—Julia Frankenhauser-Mannuß and Julia Pick.
Members of the international advisory board provided input to the study design: Ulf Günther (Department of Anesthesiology, Intensive Care Medicine, and Pain Therapy, University Hospital Oldenburg, Oldenburg, Germany), George A. Kuchel (University of Connecticut Center on Aging, Farmington, Connecticut, USA), Susan Kurrle (Health Care of Older People, Faculty of Medicine, University of Sidney, Sidney, Australia), and Yoanna Skrobik (Department of Medicine, McGill University, Montreal, Quebec, Canada).
PAWEL study group members and collaborators who contributed to this article: University Hospital Tübingen—Florian Metzger (Department of Psychiatry and Psychotherapy); Andreas Straub (Department of Anesthesiology); Tobias Krüger (Department of Heart Surgery); Felix Bausenhart (Department of Orthopedics); and Petra Renz (Nursing Department). Klinikum Stuttgart, Stuttgart, Germany—Andreas Walther (Department of Anaesthesiology and Intensive Care, Katharinenhospital); Carola Bruns, Juliane Spank, and Patricia Sabbah (Department of Old Age Psychiatry and Psychotherapy). University of Potsdam, Potsdam, Germany—Andreas Häusler, Bernd Förstner, and Susanne Schulze (Department of Social and Preventive Medicine). University of Freiburg, Freiburg, Germany—Christoph Maurer and Markus Martin (Department of Neurology and Neurophysiology); Bernhard Heimbach and Sebastian Voigt-Radloff (Center for Geriatric Medicine and Gerontology (ZGGF). University Hospital Ulm, Ulm, Germany—Heiko Reichel (Department for Orthopedics); Andreas Liebold (Department of Cardiothoracic and Vascular Surgery); Olivia Küster (Department of Neurology); and Simone Brefka (Agaplesion Bethesda Clinic, Geriatric Medicine, Ulm University and Geriatric Center Ulm). Karlsruhe, Germany—Stephan Kirschner (Department of Orthopaedics, ViDia Christian Clinics); Nina Stober (Geriatric Center Karlsruhe, ViDia); and Uwe Mehlhorn (Helios Clinic for Cardiac Surgery, Karlsruhe). University Duisburg-Essen, Essen, Germany—Jürgen Wasem and Anja Neumann (Institute for Health Care Management and Research).
Funding
This study is funded by the Innovationsfonds (Fund of the Federal Joint Committee, Gemeinsame Bundesausschuss, G-BA), who had no role in the design of the study and will have no role during its execution, or in the analyses of the data, or in the decision to submit any results. The authors acknowledge the support of the Deutsche Forschungsgemeinschaft and Open Access Publishing Fund of University of Potsdam.
Availability of data and materials
The participant-level data set cannot be made publicly available due to German data protection rules and regulations. The statistical code can be made available upon request.
Author information
Authors and Affiliations
Consortia
Contributions
CT, GWE, and MAR designed the multicenter trial. CT developed the multimodal, multiprofessional intervention. SK, MD, CAFvA, JB-S, and YS contributed significantly to the trial formation. AS, FD, SW, FK, CAFvA, MD, MAR, LOC, JB-S, SJ, HS, BM, and RA specified outcomes and interventions. AS wrote the first draft of the manuscript, followed by extensive revision by CT. All authors contributed to and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
This study was approved by the Ethics Commission of the Faculty of Medicine of the Eberhard-Karls University and University Hospital Tübingen with number 517/2017BO1 on October 12, 2017, and by the Ethics Commission of the University of Potsdam with number 38/2017 on December 11, 2017. The study was registered on the German Clinical Trials Register (number DRKS00013311, https://www.drks.de/drks_web/navigate.do?navigationId=trial.HTML&TRIAL_ID=DRKS00013311) on November 10, 2017.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Additional file
Additional file 1:
SPIRIT checklist: recommended items to address in a clinical trial protocol and related documents. (DOCX 56 kb)
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Sánchez, A., Thomas, C., Deeken, F. et al. Patient safety, cost-effectiveness, and quality of life: reduction of delirium risk and postoperative cognitive dysfunction after elective procedures in older adults—study protocol for a stepped-wedge cluster randomized trial (PAWEL Study). Trials 20, 71 (2019). https://doi.org/10.1186/s13063-018-3148-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s13063-018-3148-8