Abstract
Background
Renal fibrosis is considered an irreversible pathological process and the ultimate common pathway for the development of all types of chronic kidney diseases and renal failure. Diosmin is a natural flavonoid glycoside that has antioxidant, anti-inflammatory, and antifibrotic activities. However, whether Diosmin protects kidneys by inhibiting renal fibrosis is unknown. We aimed to investigate the role of Diosmin in renal interstitial fibrosis and to explore the underlying mechanisms.
Methods
The UUO mouse model was established and gavaged with Diosmin (50 mg/kg·d and 100 mg/kg·d) for 14 days. HE staining, Masson staining, immunohistochemistry, western blotting and PCR were used to assess renal tissue injury and fibrosis. Elisa kits were used to detect the expression levels of IL-1β, IL-6, and TNF-α and the activity of SIRT3 in renal tissues. In addition, enrichment maps of RNA sequencing analyzed changes in signaling pathways. In vitro, human renal tubular epithelial cells (HK-2) were stimulated with TGF-β1 and then treated with diosmin (75 μM). The protein and mRNA expression levels of SIRT3 were detected in the cells. In addition, 3-TYP (selective inhibitor of SIRT3) and SIRT3 small interfering RNA (siRNA) were used to reduce SIRT3 levels in HK-2.
Results
Diosmin attenuated UUO-induced renal fibrosis and TGF-β1-induced HK-2 fibrosis. In addition, Diosmin reduced IL-1β, IL-6, and TNF-α levels in kidney tissues and supernatants of HK-2 medium. Interestingly, Diosmin administration increased the enzymatic activity of SIRT3 in UUO kidneys. In addition, Diosmin significantly increased mRNA and protein expression of SIRT3 in vitro and in vivo. Inhibition of SIRT3 expression using 3-TYP or SIRT3 siRNA abolished the anti-inflammatory effects of diosmin in HK-2 cells. Enrichment map analysis by RNA sequencing indicates that the nuclear factor-kappa B (NF-κB) signaling pathway was inhibited in the Diosmin intervention group. Furthermore, we found that TGF-β1 increased the nuclear expression of nuclear NF-κB p65 but had little significant effect on the total intracellular expression of NF-κB p65. Additionally, Diosmin reduced TGF-β1-caused NF-κB p65 nuclear translocation. Knockdown of SIRT3 expression by SIRT3 siRNA increased the nuclear expression of NF-κB p65 and abolished the inhibition effect of Diosmin in NF-κB p65 expression.
Conclusions
Diosmin reduces renal inflammation and fibrosis, which is contributed by inhibiting nuclear translocation of NF-κB P65 through activating SIRT3.
Similar content being viewed by others
Background
Worldwide mortality due to chronic kidney disease (CKD) has increased markedly over the past 25 years and continues to increase [1]. CKD has become a serious public-health problem that has caused great suffering and economic burden to people worldwide [2]. The multifaceted etiology of CKD encompasses various underlying factors, including diabetes, hypertension, inflammation, oxidative stress, and metabolic disorders [3]. However, efficacious drugs that can slow-down CKD progression are lacking. Studies have shown that the pathologic development of CKD involves progressive glomerulosclerosis, tubular constriction/dilation, death of tubular cells, and interstitial fibrosis. Among them, interstitial fibrosis [4] is a common pathway for almost all types of CKD to progress to end-stage renal disease. Renal fibrosis is now recognized as a major determinant of renal pathology [5]. Inflammation is often considered an important initial event in renal fibrosis [6,7,8]. Various physiologic injuries or inflammatory cytokines can trigger renal fibrosis in the initial stages and eventually cause end-stage renal disease. The sustained inflammatory response induces the release of cytokines and initiates various signaling pathways which, in turn, have a crucial role in enhanced myofibroblast activity and excessive accumulation of the extracellular matrix, and have an important pathologic basis for it [9]. Experimental studies [10, 11] have shown that use of specific anti-inflammatory measures in CKD has excellent antifibrotic and nephroprotective effects.
Silent information regulator 3 (SIRT3) belongs to a family of evolutionarily conserved deacetylases that mediate nuclear gene expression, metabolic control, the cell cycle, and cell proliferation [12, 13]. There is increasing evidence that SIRT3 plays an important part in the development of kidney disease. Increasing the expression and activity of SIRT3 can delay the development of kidney disease. Conversely, deficiency of SIRT3 leads to high levels of oxidative stress, increased chronic inflammation, mitochondrial dysfunction, and defective telomere instability [14, 15]. These cellular processes are involved in the progression of diseases such as diabetic nephropathy, renal fibrosis, and acute kidney injury, and strongly aggravate the pathologic damage to the kidney.
Diosmin is a glycosylated polyphenolic flavonoid found in Citrus aurantium (Citrus sinensis) and olive leaves (Olea europaea) [16,17,18]. Several clinical studies have demonstrated the anti-inflammatory potential of Diosmin [19, 20]. Diosmin can inhibite levels of TNF-α, IL-1β, and IL-6 while promoting IL-12 production in patients with chronic venous disease [19]. In preclinical studies, Diosmin has also shown a range of pharmacological activities including antioxidant, anti-inflammatory and anti-apoptotic [21]. Diosmin has been shown to attenuate paraquat-induced lung inflammation and fibrosis in mice by increasing glutathione levels and catalase activity and decreasing hydroxyproline levels and malondialdehyde levels [22]. Gerges et al. [23] demonstrated that Diosmin ameliorated inflammation, insulin resistance, and fibrosis in a rat model of non-alcoholic steatohepatitis. Furthermore, a preclinical study [24] showed that Diosmin regulates oxidative stress-mediated renal inflammation and apoptosis via the NF-kB pathway which, in turn, attenuates adriamycin-induced renal injury in rats. However, whether Diosmin provides protection against unilateral ureteral obstruction (UUO)-induced CKD by inhibiting renal inflammation and interstitial fibrosis is not known. We designed in vivo and in vitro experiments to determine the beneficial effects of Diosmin on ameliorating renal fibrosis and the underlying mechanisms involved.
Materials and methods
Reagents
Diosmin (cat no.: HY-N0178) and 3-TYP (HY-108331) were purchased from MedChemExpress (Monmouth Junction, NJ, USA). Human proximal tubular epithelial (HK-2) cells were obtained from American Type Culture Collection (Manaszsas, VA, USA). Fetal bovine serum was sourced from MilliporeSigma (Burlington, MA, USA). Transforming growth factor-β1 (TGF-β1), primary antibodies α-smooth muscle actin (α-SMA), collagen I, NF-κB p65, glyceraldehyde 3-phosphate dehydrogenase (GAPDH)) and secondary rabbit-binding antibodies were purchased from Proteintech (Chicago, IL, USA). Lipofectamine™ 2000 Transfection Reagent (11668019) was from Thermo Fisher Scientific (Waltham, MA, USA). A reverse transcription kit and SYBR™ Green PCR master product was purchased from Vazyme (Nanjing, China).
Animals and experimental procedures
The protocol for animal experimentation was approved (LLSC20210354) by the Animal Care and Use Committee of Anhui Medical University (Hefei, China). The study was conducted in accordance with the Experimental Animal Administration regulations issued by the State Committee of Science and Technology of the People′ s Republic of China. All the procedures for the care of the mice were in accordance with the institutional guidelines for animal use in research. Renal fibrosis was induced by UUO surgery. UUO model is a classic and rapid model to simulate renal fibrosis [25]. In the UUO model, ligation of the ureter resulted in obstruction of the renal outflow tract on the ligation side, hydronephrosis with tubule dilation, and subsequent immune cell infiltration and fibrosis. Mechanical stretching of tubular epithelial cells leads to cell damage and death, which recruits large numbers of immune cells and causes an inflammatory response. The result is activation and proliferation of myofibroblasts. C57BL/6 mice (8 weeks; 20 ~ 25 g) were housed in SPF (Specific Pathogen Free) grade animal houses on an ad libitum diet at a temperature of 22–24 degrees Celsius and a humidity of approximately 60%. Mice were divided into four groups of five [22, 26]: sham operation (Sham), UUO, UUO + Dios-1 (Diosmin 50 mg/kg), and UUO + Dios-2 (Diosmin 100 mg/kg).
Diosmin was dissolved in dimethyl sulfoxide (0.5% v/v) and administered by gavage for 14 days after UUO surgery [27, 28]. Changes in bodyweight, food intake, and water intake were recorded every week. Mice were sacrificed by intraperitoneal injection of sodium pentobarbital (50 mg/kg). Serum was collected before mice were killed. Levels of alanine transaminase (ALT), aspartate transaminase (AST), alkaline phosphatase (ALP), blood urea nitrogen (BUN), and serum creatinine (Scr) were measured using an automated biochemical analyzer (Roche, Basel, Switzerland). Kidney tissue was fixed with 4% paraformaldehyde, embedded in paraffin, and sectioned to a thickness of 5 mm. Paraffin sections were stained with hematoxylin and eosin (H&E) or Masson's trichrome for morphology studies. Masson trichrome-stained fibrotic areas and positive areas were analyzed using ImageJ 1.47 (US National Institutes of Health, Bethesda, MD, USA).
RNA sequencing analysis
The mRNA of the kidneys was extracted and sent to Gene Denovo Technology Co., Ltd. for mRNA sequencing. Differential gene expression analysis was completed using the R package limma (version 3.44.3). The fold change (FC) of each gene was log2 transformed and further analyzed using the R package clusterProfiler (version 3.16.1). Then, gene set enrichment analysis of canonical pathways was conducted to find differentially regulated pathways.
Cell-viability assay
To assess cell viability, HK-2 cells were cultured at 1 × 104 cells per well in 96-well plates. After treatment with Diosmin for 3 h, they were incubated with 0.5 mg/mL of 3-(4,5-Dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide solution (100 μL/well) for 4 h. After washing with 1 × PBS, dimethyl sulfoxide (150 μL/well) was added to dissolve purple crystals. The absorbance of the sample was measured at 570 nm with a microplate reader (BioTek Instruments, Winooski, USA).
Small interfering RNA (siRNA) transfection
Human SIRT3-specific siRNA was synthesized by QingkeBio (Beijing, China). The target nucleotide sequence of the siRNA was CATCGATGGGCTTGAGAGA. HK-2 cells were added to a six-well plate at 2 × 104 cells/well. After cells had become attached, the medium was changed 1 h before transfection. Then, siRNA (50 nM) was transfected for 24 h using Lipofectamine 2000 (Thermo Fisher Scientific) according to manufacturer instructions.
Elisa
Elisa kits for interleukin (IL)-6 (RX203049M), IL-1β (RX203063M), and tumor necrosis factor (TNF)-α (RX202412M) were obtained from Quanzhou Ruixin Yijian Biotechnology (Quanzhou, China). Levels of IL-1β, IL-6, and TNF-α in kidney and the supernatant of HK-2 cell-culture medium were detected using Elisa kits according to standard protocols, respectively.
Assay to measure the activity of SIRT3
The activity of SIRT3 in mouse kidneys was measured by a SIRT3 enzyme activity detection kit (KL-SIRT3-Hu02, Shanghai, China). The activity of SIRT3 in specimens was measured by the double-antibody sandwich method. Results were obtained from three replicate experiments.
Western blotting
Western blotting was used to measure the protein expression in HK-2 cells or mouse kidney tissue after treatment (Part of the the blots were cut prior to hybridisation with antibodies during blotting). Antibody binding was detected using a western blotting detection kit (Thermo Fisher Scientific). Captured western blotting bands using an ultrasensitive multifunction imager (AI600RGB; General Electric, Boston, MA, USA). Bands were quantified with ImageJ and normalized to GAPDH expression.
Quantitative PCR
Total RNA was extracted from HK-2 cells or mice kidney tissue using TRIzol® Reagent. Complementary-DNA was synthesized by Hiscript Q RT SuperMix and used for a qPCR (+ gDNA wiper) reverse transcriptase kit (Vazyme). Real-time PCR was undertaken on primers, the sequences of which are shown in Table 1. Messenger (m)RNA expression of the corresponding samples was normalized with GAPDH mRNA.
Statistical analyses
Values are the mean ± SEM. Quantitative data were tested for normality. Two-tailed unpaired t-test and one-way ANOVA were used to compare differences between two groups and multiple groups, respectively. Prism 9.0 (GraphPad, San Diego, CA, USA) was used for statistical analyses. p < 0.05 was designated significant.
Results
Diosmin attenuates UUO-induced renal injury and inflammation
To assess the potential impact of Diosmin on renal injury, we examined tissue staining, renal function, and the expression of inflammatory cytokines in four groups of mice. H&E staining showed diffuse infiltration of inflammatory cells, degeneration and necrosis of renal tubular epithelial cells, and renal tubular dilatation in the kidney tissue of UUO mice (Fig. 1A). Diosmin treatment improved renal histologic damages significantly. Inflammatory cytokine levels were subsequently measured in the kidneys and blood of mice. Enzyme-linked immunosorbent assay showed that Diosmin inhibited the levels of IL-1β, IL-6 and TNF-α in the kidneys of mice in the UUO group (Fig. 1F-H). Furthermore, staining with Masson trichrome suggested that Diosmin could attenuate UUO-induced hyperplasia of interstitial collagen fibers significantly in the fibrotic kidneys of mice (Fig. 1A, D). There was no significant difference in Scr, BUN (Fig. 1B, C), and the kidney weight: bodyweight ratio (Fig. S1) among the four groups. In addition, Diosmin had no significant effect on serum levels of ALT, AST, or ALP (Fig. S2).
Diosmin attenuates UUO-induced renal injury and inflammation. A Representative images of HE staining and Masson staining of kidney tissue. B Scr and (C) BUN values for the different groups. D Quantification of Masson staining-positive areas. E Detection of protein expression levels of IL-6, (F) IL-1β and (G) TNF-α in the serum using Elisa. *p < 0.05, and ***p < 0.001 versus the Sham group; &&p < 0.01, and &&&p < 0.001 versus the UUO group; #p < 0.05, ##p < 0.01; ns = no significance; Scr = serum creatinine; BUN = blood urea nitrogen; Scale bar = 100 μm. Dios-1 = Diosmin 50 mg/kg; Dios-2 = Diosmin 100 mg
Diosmin inhibits the UUO-induced collagen deposition and fibrosis
Sustained activation of inflammatory cytokines caused by UUO leads to the conversion of fibroblasts in the renal interstitium into myofibroblasts. The latter secrete collagen fibers that are non-degradable, which leads to the accumulation and deposition of large amounts of extracellular matrix collagen, thereby destroying the renal tissue structure. To assess the potential impact of Diosmin on renal fibrosis, we examined renal fibrosis markers in four groups of mice. Immunohistochemical staining showed a significant increase in protein expression of collagen I and a-SMA in the kidneys of mice in the UUO group (Fig. 2A). Whereas Diosmin treatment inhibited the expression of fibrosis-marking proteins. In addition, Western blotting also proved consistent results (Fig. 2B-D). RT-qPCR showed that the levels of collagen I and a-SMA mRNA were suppressed after D intervention (Fig. 2E, F). These results indicated that Diosmin alleviated UUO-induced kidney injury, collagen production, and renal fibrosis in mice.
Diosmin inhibits the UUO-induced collagen deposition and fibrosis. A Representative images of collagen I and α-SMA IHC staining. B Representative western blot analysis of collagen I and α-SMA. C Quantitative analysis of collagen I and D α-SMA. E The mRNA expression levels of collagen I and F α-SMA in the left kidney of mice. ***p < 0.0001 versus the Sham group; &&p < 0.01, and &&&p < 0.001 versus the UUO group; #p < 0.05, ##p < 0.01 and ###p < 0.001; ns = no significance; Scale bar = 100 μm. Dios-1 = Diosmin 50 mg/kg; Dios-2 = Diosmin 100 mg/kg
Diosmin inhibits TGF-β1 induced inflammation and fibrosis in HK-2 cells
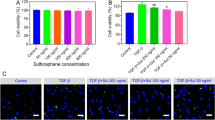
We further investigated the anti-fibrotic effect of Diosmin on human renal tubular epithelial (HK-2) cells. Diosmin treatment (0, 1, 5, 10, 25, 50, and 75 μM) of HK-2 cells did not produce a significant inhibitory effect on their viability (Fig. 3A). Cell viability was inhibited slightly at a Diosmin concentration of 100 μM. Therefore, we chose to treat cells with Diosmin at a concentration of 75 μM. HK-2 cells treated with TGF-β1 (5 ng/mL) increased the mRNA and protein expression of collagen I and α-SMA. Diosmin inhibited the transcription and translation the protein expression of α-SMA and collagen I in HK-2 cells stimulated by TGF-β1 (Fig. 3B-F). Consistent with the in vivo results, Diosmin inhibited secretion of IL-1β, IL-6, and TNF-α in HK-2 cell supernatants following TGF-β1 stimulation (Fig. 3G-I). Taken together, Diosmin attenuated fibrosis and inflammation in HK-2 cells under TGF-β1 stimulation.
Diosmin reduces TGF-β1 induced inflammation and fibrosis in HK-2 cells. A MTT assay detects the toxicity of Diosmin on HK-2 cells. B The mRNA expression levels of collagen I and (C) α-SMA. D Representative western blot analysis of collagen I and α-SMA. E Quantitative analysis of collagen I and (F) α-SMA. G The levels of IL-6, (H) IL-1β and (I) TNF-α in the supernatant. *p < 0.05, and ***p < 0.001 versus the control (DMSO) group; &p < 0.05, &&p < 0.01, and &&&p < 0.001 versus the TGF-β1 group; ns = no significance; Ctrl = control; Dios = 75uM
Diosmin increases SIRT3 expression in vivo and in vitro
We found that protein expression of SIRT3 was significantly reduced in the kidneys of the UUO group, while Diosmin was able to partially restore SIRT3 expression (Fig. 4A). Western blotting also indicated consistent results (Fig. 4E, F). Therefore, we further explored the effect of Diosmin on SIRT3 activity. UUO treatment decreased SIRT3 activity in kidney, whereas Diosmin increased SIRT3 activity significantly in the fibrotic kidneys (Fig. 4B). Furthermore, the effect of Diosmin on SIRT3 expression was examined in vivo and in vitro. Treatment with UUO and TGF-β1 decreased the protein and mRNA expression of SIRT3 in kidney tissue and HK-2 cells, but intervention with Diosmin reversed this phenomenon (Fig. 4C, D). Thus, Diosmin increased SIRT3 expression and activity.
Diosmin increases SIRT3 expression in vivo and in vitro. A Representative images of SIRT3 IHC staining. B The enzyme activity of SIRT3 in left kidney of different groups of mice. C The mRNA expression levels of SIRT3 in the left kidney and (D) HK-2. (E) Representative western blot analysis and (F) quantitative analysis in the HK-2. **p < 0.01, and ***p < 0.001 versus the Sham or the control (DMSO) group; &p < 0.05, &&p < 0.01, and &&&p < 0.001 versus UUO or TGF-β1 group; ###p < 0.001; ns = no significance; Ctrl = control; Dios = 75uM; Dios-1 = Diosmin 50 mg/kg; Dios-2 = Diosmin 100 mg/kg
Deletion of SIRT3 eliminates the anti-inflammatory effects of Diosmin
We treated HK-2 cells with SIRT3 siRNA or 3YTP (SIRT3-selective inhibitor) and investigated the regulation of SIRT3 in the anti-inflammatory effect of Diosmin. Western blotting was used to detect transfection efficiency (Fig. 5A, B). SIRT3 siRNA significantly attenuated the inhibitory effect of Diosmin on inflammation in TGF-β1-induced HK-2 cells (Fig. 5C-E). Furthermore, identical results were obtained using 3-TYP (Fig. 5F-H). However, 3-TYP alone had no detectable effect on levels of inflammatory cytokines compared with controls. In addition, the 3-TYP + TGF-β1 group and SIRT3 siRNA + TGF-β1 significantly increased the levels of inflammatory cytokines compared with those using 3-TYP alone or SIRT3 siRNA alone, thereby indicating that 3-TYP or SIRT3 siRNA was effective only in pathologic conditions.
Deletion of SIRT3 eliminates the anti-inflammatory effects of Diosmin. A, B Western blotting for the transfection efficiency. C-E The effect of SIRT3 SiRNA on the secretion of IL-1β, IL-6, and TNF-α regulated by Diosmin in the supernatant of the culture medium of HK-2 cells. F-H The effect of 3-TYP (SIRT3 selective inhibitor) on the secretion of IL-1β, IL-6, and TNF-α regulated by Diosmin in the supernatant of the culture medium of HK-2 cells. **p < 0.01, and ***p < 0.001 versus the control (DMSO) group; &p < 0.05, &&p < 0.01, and &&&p < 0.001 versus the TGF-β1 alone group; #p < 0.05, ##p < 0.01 and ###p < 0.001 versus the Dios + TGF-β1 group; $$$p < 0.001 versus the SIRT3 siRNA alone group; ns = no significanc
Diosmin ameliorates renal fibrosis by regulating SIRT3-mediated NF-κB p65 nuclear translocation
To further explore the mechanism of Diosmin inhibition of fibrosis, we analyzed the differentially expressed genes in the kidneys of mice from UUO and Diosmin intervention groups using RNA sequencing (RNA-seq). We found that the NF-κB signaling pathway was significantly down-regulated after Diosmin intervention compared to UUO mice (Fig. 6A). Hence, we investigated how SIRT3 regulates inflammation by focusing on the NF-κB signaling pathway in stimulated HK-2 cells. TGF-β1 significantly increased the nuclear expression of NF-κB p65 in HK-2 cells. However, TGF-β1 and Diosmin had no significant effect on the total expression of NF-κB p65 in HK-2 cells (Fig. 6B-D). Diosmin inhibited the nuclear expression of NF-κB p65 in HK-2 cells. After knockdown of SIRT3 expression, the inhibitory effect of Diosmin on NF-κB p65 was attenuated significantly. Taken together, SIRT3 mediates Diosmin-induced anti-fibrotic effects by reducing the nuclear expression of NF-κB p65 in HK-2 cells after treatment (Fig. 7).
Diosmin ameliorates renal fibrosis by regulating SIRT3-mediated NF-κB p65 nuclear translocation. A The enrichment plot of NF-κB signaling pathway. B Representative western blot analysis of the expression of total NF-κB P65 and nuclear NF-κB p65 in HK-2 cells. C Quantitative analysis of total NF-κB p65 and (D) nuclear NF-κB p65. ***p < 0.001 versus the control (DMSO) group; &&&p < 0.001 versus the TGF-β1 alone group; ###p < 0.001 versus the Dios + TGF-β1 group; ns = no significance; WCL = whole cell; NE = nucleus; t-NF-κB p65 = total NF-κB p65
Schema of the underlying mechanism anti-inflammatory effect of Diosmin in renal fibrosis. Diosmin performs promotes the expression and activity of SIRT3, then inhibits nuclear translocation of NF-κB p65 to reduce inflammatory cytokines (TNF-α, IL-6, and IL-1β) levels. Therefore, Diosmin exerts the anti-fibrotic effect. Altogether, Diosmin attenuates renal fibrosis mainly by suppressing NF-κB p65-inflammation pathway, which is dependent on induction of SIRT3 expression
Discussion
Anti-inflammatory therapy is an effective strategy for treating fibrosis [29, 30]. We demonstrated that Diosmin prevented UUO- or TGF-β1-induced renal fibrosis mainly by inhibiting inflammation. Decreased levels of inflammatory cytokines were documented. In particular, SIRT3 was involved in the anti-inflammatory effect of Diosmin-induced renal fibrosis. Diosmin promoted SIRT3 expression, and deletion of SIRT3 abolished the inhibitory effect of Diosmin upon inflammation. Interestingly, SIRT3 was involved in the regulation of nuclear expression of NF-κB p65, and silencing SIRT3 expression increased the nuclear expression of NF-κB p65 in HK-2 cells. Thus, our data clearly demonstrate that anti-inflammatory effects against Diosmin-induced renal fibrosis can be promoted by regulating SIRT3-mediated nuclear NF-κB p65 expression.
Renal fibrosis is considered to be an inflammation-related disease [31, 32]. Inflammatory cells secrete many inflammatory cytokines and further infiltrate renal tissue, making the kidney in an “inflammatory microenvironment”. Without efficacious treatment, persistent inflammatory stimulation can further aggravate irreversible kidney damage. NF-κB p65 is a key regulator mediating the regulation of inflammation. Phosphorylation and nuclear translocation of p65 are the main modes of activation of the NF-kB pathway. Therefore, p65-nuclear localization sequence is often used to reflect the expression of active p65. Several studies have shown that regulation of nuclear NF-κB p65 expression can control inflammation effectively [33,34,35]. Studies have reported that Liuweiwuling tablets can alleviate bile-duct ligation-induced liver fibrosis mainly by inhibiting the expression of the inflammatory cytokines IL-1β1, TNF-α, and IL-6 [36]. The anti-hepatic-fibrosis effect of the novel oridonin analog CYD0618 is accomplished mainly by blockade of the nuclear translocation of NF-κB p65 and preventing the phosphorylation of the NF-κB inhibitory protein IκBα [37]. Recently, Chen et al. [37] found that, in a carbon tetrachloride-induced model of liver fibrosis in rats, increased expression of SIRT3 attenuated inflammation and fibrosis by inhibiting NF-κB p65 nuclear translocation. Consistent with the results of other studies, our results indicated that TGF-β1 increased the expression of nuclear NF-κB p65, whereas Diosmin decreased the expression of nuclear NF-κB p65 significantly. Therefore, the anti-inflammatory effect of Diosmin is also dependent upon NF-κB.
SIRT3 is a promising target for treatment of inflammation-related diseases [38, 39]. Kurundkar et al. [40] reported that SIRT3 expression was reduced significantly in mouse lungs upon activation of the NLR family pyrin domain during lipopolysaccharide-induced acute lung injury. Activation of SIRT3 with vinferin reduced activation of the NLRP3 inflammasome and production of inflammatory cytokines, and attenuated lung-tissue damage. However, the protection mentioned above was abolished in SIRT3-knockout mice [40]. Zhang et al. [41] demonstrated that melatonin could exhibit anti-inflammatory, anti-oxidative stress, and anti-apoptotic renoprotective effects via activation of SIRT3 in models of acute renal failure in vivo and in vitro. Wu et al. [42] showed that Rhein has antioxidant capacity and anti-fibrosis effects in a model of chronic kidney disease because it can activate the SIRT3/Fxo3α signaling pathway. Palomer et al. [43] found that SIRT3-knockout mice developed myocardial inflammation and fibrosis. In contrast, SIRT3 overexpression in the cardiomyocytes of neonatal rats prevented (at least in part) TNF-α-induced inflammatory responses and attenuated fibrotic responses. We found that UUO or TGF-β1 decreased the activity and expression of SIRT3 significantly, while increasing the secretion of inflammatory cytokines and the expression of NF-κB p65 in activated hematopoietic stem cells. In addition, SIRT3 overexpression reduced the expression of NF-κB p65, suggesting that SIRT3 mediates the regulation of TGF-β1-induced inflammation mainly by regulating the expression of NF-κB p65 during renal fibrosis, data which are consistent with the results of other reports [44, 45]. Therefore, our data suggest that SIRT3 may be a potential therapeutic target of inflammation-related diseases such as renal fibrosis. In the absence of TGF-β1 stimulation, 3-TYP alone or SIRT3 siRNA alone did not have a significant effect on the secretion of inflammatory cytokines, but they significantly promoted secretion of inflammatory cytokines. This phenomenon may be due to TGF-β1 stimulation leading to the formation of some pathologic microenvironments characterized by excessive secretion of inflammatory cytokines, whereas SIRT3 siRNA or 3-TYP exerted their effects only in such pathologic microenvironments. SIRT3 siRNA or 3-TYP enhanced TGF-β1-induced secretion of inflammatory cytokines.
As a flavonoid compound, Diosmin has anti-inflammatory, anti-oxidative stress, anti-fibrotic, and other effects [21,22,23]. Tahir et al. [46] found that Diosmin could protect against ethanol-induced liver injury by attenuating the inflammatory response and regulating activation of TNF-α and NF-κB. Yang et al. created a mouse model of renal ischemia by non-traumatic microvascular clipping of the left renal pedicle combined with resection of the right renal pedicle. After perfusion, Diosmin treatment inhibited nuclear NF-κB and mitochondrial apoptotic pathways and activated the Nrf2/HO-1 pathway to protect the kidneys [47]. Fattori et al. [48] applied Diosmin to block NF-κB activation in the treatment of lipopolysaccharide-induced inflammatory pain and peritonitis in mice. We found that Diosmin can suppress the level of inflammation and inhibit the progression of renal fibrosis by upregulating the expression of SIRT3.
Diosmin may increase SIRT3 expression and activity through multiple pathways. However, exactly how Diosmin regulates SIRT3 is not known. Our research team will further explore the potential mechanisms. Furthermore, to investigate further the role of SIRT3 in Diosmin-induced anti-fibrotic effects, we will use SIRT3-knockout mice in future studies. The Smad protein [49, 50] has been studied widely as a transcription factor and key intracellular effector of TGF-β1. Smad4 and Smad3 are pro-fibrotic, whereas Smad2 and Smad7 protect against fibrosis [51, 52]. As a key mediator in the pathogenesis of renal fibrosis, TGF-β1 can activate Smad-dependent and non-dependent pathways to express its biological activity. Therefore, we will explore the function of TGF-β1/Smad signaling in Diosmin-induced renal fibrosis in future studies.
However, it is important to acknowledge certain limitations in our study. First, our research primarily focused on preclinical models, and the transition to clinical studies in human subjects is warranted to confirm the safety and efficacy of Diosmin in a real-world setting. Second, while our investigation provides insights into the mechanism of action of Diosmin, additional in-depth studies are needed to elucidate the complete signaling pathways involved. Furthermore, a more comprehensive assessment of the potential adverse effects and side effects of Diosmin should be undertaken as part of future research, considering its translational potential.
Conclusions
Diosmin was found to attenuate renal fibrosis mainly by inhibiting inflammation. The anti-inflammatory effect of Diosmin was dependent on SIRT3-mediated nuclear expression of NF-κB p65. Our results provide new insights into the molecular mechanisms by which Diosmin regulates inflammation-related diseases and could be a natural candidate for the treatment of renal fibrosis.
Availability of data and materials
The data in this study are available from the corresponding author request.
References
Eckardt KU, Coresh J, Devuyst O, Johnson RJ, Köttgen A, Levey AS, Levin A. Evolving importance of kidney disease: from subspecialty to global health burden. Lancet (London, England). 2013;382(9887):158–69.
Lv JC, Zhang LX. Prevalence and disease burden of chronic kidney disease. Adv Exp Med Biol. 2019;1165:3–15.
Eckardt KU, Delgado C, Heerspink HJL, Pecoits-Filho R, Ricardo AC, Stengel B, Tonelli M, Cheung M, Jadoul M, Winkelmayer WC, et al. Trends and perspectives for improving quality of chronic kidney disease care: conclusions from a Kidney Disease: Improving Global Outcomes (KDIGO) Controversies Conference. Kidney Int. 2023;104(5):888–903.
de Cos M, Xipell M, García-Herrera A, Lledo GM, Guillen E, Blasco M, Espinosa G, Cervera R, Quintana LF. Assessing and counteracting fibrosis is a cornerstone of the treatment of CKD secondary to systemic and renal limited autoimmune disorders. Autoimmun Rev. 2022;21(3):103014.
Roccatello D, Lan HY, Sciascia S, Sethi S, Fornoni A, Glassock R: From inflammation to renal fibrosis: a one-way road in autoimmunity?. Autoimmun Rev. 2023:103466. Published Online October 15 2023.
Gu YY, Liu XS, Huang XR, Yu XQ, Lan HY. TGF-β in renal fibrosis: triumphs and challenges. Future Med Chem. 2020;12(9):853–66.
Yan H, Xu J, Xu Z, Yang B, Luo P, He Q. Defining therapeutic targets for renal fibrosis: exploiting the biology of pathogenesis. Biomed Pharmacother. 2021;143:112115.
Wu W, Wang X, Yu X, Lan HY. Smad3 signatures in renal inflammation and fibrosis. Int J Biol Sci. 2022;18(7):2795–806.
Lv W, Booz GW, Wang Y, Fan F, Roman RJ. Inflammation and renal fibrosis: recent developments on key signaling molecules as potential therapeutic targets. Eur J Pharmacol. 2018;820:65–76.
Liao Y, Tan RZ, Li JC, Liu TT, Zhong X, Yan Y, Yang JK, Lin X, Fan JM, Wang L. Isoliquiritigenin Attenuates UUO-Induced Renal Inflammation and Fibrosis by Inhibiting Mincle/Syk/NF-Kappa B Signaling Pathway. Drug Des Dev Ther. 2020;14:1455–68.
Li S, Lin Q, Shao X, Mou S, Gu L, Wang L, Zhang Z, Shen J, Zhou Y, Qi C, et al. NLRP3 inflammasome inhibition attenuates cisplatin-induced renal fibrosis by decreasing oxidative stress and inflammation. Exp Cell Res. 2019;383(1):111488.
Wang Q, Xu J, Li X, Liu Z, Han Y, Xu X, Li X, Tang Y, Liu Y, Yu T, et al. Sirt3 modulate renal ischemia-reperfusion injury through enhancing mitochondrial fusion and activating the ERK-OPA1 signaling pathway. J Cell Physiol. 2019;234(12):23495–506.
Tan C, Gu J, Li T, Chen H, Liu K, Liu M, Zhang H, Xiao X. Inhibition of aerobic glycolysis alleviates sepsis-induced acute kidney injury by promoting lactate/Sirtuin 3/AMPK-regulated autophagy. Int J Mol Med. 2021;47(3):19.
Zhang Q, Liu X, Li N, Zhang J, Yang J, Bu P. Sirtuin 3 deficiency aggravates contrast-induced acute kidney injury. J Transl Med. 2018;16(1):313.
Srivastava SP, Li J, Kitada M, Fujita H, Yamada Y, Goodwin JE, Kanasaki K, Koya D. SIRT3 deficiency leads to induction of abnormal glycolysis in diabetic kidney with fibrosis. Cell Death Dis. 2018;9(10):997.
Buddhan R, Manoharan S. Diosmin reduces cell viability of A431 skin cancer cells through apoptotic induction. J Cancer Res Ther. 2017;13(3):471–6.
Campanero MA, Escolar M, Perez G, Garcia-Quetglas E, Sadaba B, Azanza JR. Simultaneous determination of diosmin and diosmetin in human plasma by ion trap liquid chromatography-atmospheric pressure chemical ionization tandem mass spectrometry: application to a clinical pharmacokinetic study. J Pharm Biomed Anal. 2010;51(4):875–81.
Gerges SH, Wahdan SA, Elsherbiny DA, El-Demerdash E. Pharmacology of Diosmin, a citrus flavone glycoside: an updated review. Eur J Drug Metab Pharmacokinet. 2022;47(1):1–18.
Feldo M, Wójciak M, Dresler S, Sowa P, Płachno BJ, Samborski D, Sowa I. Effect of Diosmin on selected parameters of oxygen homeostasis. Int J Mol Sci. 2023;24(16):12917.
Siennicka A, Kłysz M, Adamska M, Chełstowski K, Biskupski A, Jastrzębska M. Assessment of platelet reactivity and inflammatory markers in coronary artery bypass graft patients treated with acetylsalicylic acid with flavonoid supplementation. Molecules (Basel, Switzerland). 2021;26(24):7486.
Zheng Y, Zhang R, Shi W, Li L, Liu H, Chen Z, Wu L. Metabolism and pharmacological activities of the natural health-benefiting compound diosmin. Food Funct. 2020;11(10):8472–92.
Mirzaee S, Mansouri E, Shirani M, Zeinvand-Lorestani M, Khodayar MJ. Diosmin ameliorative effects on oxidative stress and fibrosis in paraquat-induced lung injury in mice. Environ Sci Pollut Res Int. 2019;26(36):36468–77.
Gerges SH, Wahdan SA, Elsherbiny DA, El-Demerdash E. Diosmin ameliorates inflammation, insulin resistance, and fibrosis in an experimental model of non-alcoholic steatohepatitis in rats. Toxicol Appl Pharmacol. 2020;401:115101.
AlAsmari AF, Alharbi M, Alqahtani F, Alasmari F, AlSwayyed M, Alzarea SI, Al-Alallah IA, Alghamdi A, Hakami HM, Alyousef MK, et al. Diosmin alleviates doxorubicin-induced liver injury via modulation of oxidative stress-mediated hepatic inflammation and apoptosis via NfkB and MAPK pathway: a preclinical study. Antioxidants (Basel, Switzerland). 2021;10(12):1998.
Nørregaard R, Mutsaers HAM, Frøkiær J, Kwon TH. Obstructive nephropathy and molecular pathophysiology of renal interstitial fibrosis. Physiol Rev. 2023;103(4):2827–72.
Ali FEM, Bakr AG, Abo-Youssef AM, Azouz AA, Hemeida RAM. Targeting Keap-1/Nrf-2 pathway and cytoglobin as a potential protective mechanism of diosmin and pentoxifylline against cholestatic liver cirrhosis. Life Sci. 2018;207:50–60.
Makled MN, El-Kashef DH. Saroglitazar attenuates renal fibrosis induced by unilateral ureteral obstruction via inhibiting TGF-β/Smad signaling pathway. Life Sci. 2020;253:117729.
Shin KC, Nam HK, Oh DK. Hydrolysis of flavanone glycosides by β-glucosidase from Pyrococcus furiosus and its application to the production of flavanone aglycones from citrus extracts. J Agric Food Chem. 2013;61(47):11532–40.
Zhang J, Yang A, Wu Y, Guan W, Xiong B, Peng X, Wei X, Chen C, Liu Z. Stachydrine ameliorates carbon tetrachloride-induced hepatic fibrosis by inhibiting inflammation, oxidative stress and regulating MMPs/TIMPs system in rats. Biomed Pharmacother. 2018;97:1586–94.
Sha M, Gao Y, Deng C, Wan Y, Zhuang Y, Hu X, Wang Y. Therapeutic effects of AdipoRon on liver inflammation and fibrosis induced by CCl(4) in mice. Int Immunopharmacol. 2020;79:106157.
Pan Z, Yang K, Wang H, Xiao Y, Zhang M, Yu X, Xu T, Bai T, Zhu H. MFAP4 deficiency alleviates renal fibrosis through inhibition of NF-κB and TGF-β/Smad signaling pathways. FASEB J. 2020;34(11):14250–63.
Qi R, Wang J, Jiang Y, Qiu Y, Xu M, Rong R, Zhu T. Snai1-induced partial epithelial-mesenchymal transition orchestrates p53–p21-mediated G2/M arrest in the progression of renal fibrosis via NF-κB-mediated inflammation. Cell Death Dis. 2021;12(1):44.
Xu Z, Zhang M, Wang Y, Chen R, Xu S, Sun X, Yang Y, Lin Z, Wang S, Huang H. Gentiopicroside ameliorates diabetic renal tubulointerstitial fibrosis via inhibiting the AT1R/CK2/NF-κB pathway. Front Pharmacol. 2022;13:848915.
Li H, Duann P, Li Z, Zhou X, Ma J, Rovin BH, Lin PH. The cell membrane repair protein MG53 modulates transcription factor NF-κB signaling to control kidney fibrosis. Kidney Int. 2022;101(1):119–30.
Song Z, Zhu M, Wu J, Yu T, Chen Y, Ye X, Li S, Xu N. Fucoidans from Cucumaria frondosa ameliorate renal interstitial fibrosis via inhibition of the PI3K/Akt/NF-κB signaling pathway. Food Funct. 2022;13(3):1168–79.
Liu H, Dong F, Li G, Niu M, Zhang C, Han Y, He L, Yin P, Wang B, Sang X, et al. Liuweiwuling tablets attenuate BDL-induced hepatic fibrosis via modulation of TGF-β/Smad and NF-κB signaling pathways. J Ethnopharmacol. 2018;210:232–41.
Cummins CB, Wang X, Xu J, Hughes BD, Ding Y, Chen H, Zhou J, Radhakrishnan RS. Antifibrosis effect of novel oridonin analog cyd0618 via suppression of the NF-κB pathway. J Surg Res. 2018;232:283–92.
Dikalova AE, Pandey A, Xiao L, Arslanbaeva L, Sidorova T, Lopez MG, Billings FTT, Verdin E, Auwerx J, Harrison DG, et al. Mitochondrial deacetylase Sirt3 reduces vascular dysfunction and hypertension while Sirt3 depletion in essential hypertension is linked to vascular inflammation and oxidative stress. Circ Res. 2020;126(4):439–52.
Wang Z, Li Y, Wang Y, Zhao K, Chi Y, Wang B. Pyrroloquinoline quinine protects HK-2 cells against high glucose-induced oxidative stress and apoptosis through Sirt3 and PI3K/Akt/FoxO3a signaling pathway. Biochem Biophys Res Commun. 2019;508(2):398–404.
Kurundkar D, Kurundkar AR, Bone NB, Becker EJ Jr, Liu W, Chacko B, Darley-Usmar V, Zmijewski JW, Thannickal VJ. SIRT3 diminishes inflammation and mitigates endotoxin-induced acute lung injury. JCI insight. 2019;4(1):e120722.
Zhang C, Suo M, Liu L, Qi Y, Zhang C, Xie L, Zheng X, Ma C, Li J, Yang J, et al. Melatonin alleviates contrast-induced acute kidney injury by activation of Sirt3. Oxid Med Cell Longev. 2021;2021:6668887.
Wu X, Liu M, Wei G, Guan Y, Duan J, Xi M, Wang J. Renal protection of rhein against 5/6 nephrectomied-induced chronic kidney disease: role of SIRT3-FOXO3α signalling pathway. J Pharm Pharmacol. 2020;72(5):699–708.
Palomer X, Román-Azcona MS, Pizarro-Delgado J, Planavila A, Villarroya F, Valenzuela-Alcaraz B, Crispi F, Sepúlveda-Martínez Á, Miguel-Escalada I, Ferrer J, et al. SIRT3-mediated inhibition of FOS through histone H3 deacetylation prevents cardiac fibrosis and inflammation. Signal Transduct Target Ther. 2020;5(1):14.
Chen Y, Zhang F, Wang D, Li L, Si H, Wang C, Liu J, Chen Y, Cheng J, Lu Y. Mesenchymal stem cells attenuate diabetic lung fibrosis via adjusting Sirt3-mediated stress responses in rats. Oxid Med Cell Longev. 2020;2020:8076105.
Chen C, Gu J, Wang J, Wu Y, Yang A, Chen T, Zhou T, Liu Z. Physcion 8-O-β-glucopyranoside ameliorates liver fibrosis through inflammation inhibition by regulating SIRT3-mediated NF-κB P65 nuclear expression. Int Immunopharmacol. 2021;90:107206.
Tahir M, Rehman MU, Lateef A, Khan R, Khan AQ, Qamar W, Ali F, O’Hamiza O, Sultana S. Diosmin protects against ethanol-induced hepatic injury via alleviation of inflammation and regulation of TNF-α and NF-κB activation. Alcohol (Fayetteville, NY). 2013;47(2):131–9.
Yang K, Li WF, Yu JF, Yi C, Huang WF. Diosmetin protects against ischemia/reperfusion-induced acute kidney injury in mice. J Surg Res. 2017;214:69–78.
Fattori V, Rasquel-Oliveira FS, Artero NA, Ferraz CR, Borghi SM, Casagrande R, Verri WA Jr. Diosmin treats lipopolysaccharide-induced inflammatory pain and peritonitis by blocking NF-κB activation in mice. J Nat Prod. 2020;83(4):1018–26.
Isaka Y. Targeting TGF-β signaling in kidney fibrosis. Int J Mol Sci. 2018;19(9):2532.
Rauchman M, Griggs D. Emerging strategies to disrupt the central TGF-β axis in kidney fibrosis. Transl Res. 2019;209:90–104.
Hu HH, Chen DQ, Wang YN, Feng YL, Cao G, Vaziri ND, Zhao YY. New insights into TGF-β/Smad signaling in tissue fibrosis. Chem Biol Interact. 2018;292:76–83.
Walton KL, Johnson KE, Harrison CA. Targeting TGF-β mediated SMAD signaling for the prevention of fibrosis. Front Pharmacol. 2017;8:461.
Acknowledgements
We thank all authors for their contributions and support.
Funding
This work was supported by a grant from the Natural Science Foundation of Anhui Province (2008085MH244), Postgraduate Innovation Research, Practice Program of Anhui Medical University (YJS20230032), and Health Research Program of Anhui (AHWJ2022b072).
Author information
Authors and Affiliations
Contributions
Wen-Man Zhao and Xun-Liang Li: Conceptualization, Methodology, Investigation, Data curation, Writing – original draft. Zhi-Juan Wang: Investigation, Data curation. Yuyu Zhu: Investigation, Data curation. Rui Shi: Software. Jian-Ping Xiao: Methodology, Project administration. De-Guang Wang: Review, Resources, Supervision, Project administration, Funding acquisition. All authors read the manuscript critically and approved the final version for submission.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The protocol for experimentation was approved (LLSC20210354) by the Animal Care and Use Committee of Anhui Medical University (Hefei, China). The manuscript report is in conformity with the ARRIVAL guidelines for the reporting of animal experiments.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1:
Figure S1. The kidney weight / bodyweight between the four groups of mice. Figure S2. Serum ALT, AST, and ALP levels in four groups of mice.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Zhao, WM., Li, XL., Zhu, Y. et al. Diosmin ameliorates renal fibrosis through inhibition of inflammation by regulating SIRT3-mediated NF-κB p65 nuclear translocation. BMC Complement Med Ther 24, 29 (2024). https://doi.org/10.1186/s12906-023-04330-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12906-023-04330-z