Abstract
Background
The world’s population has increased faster than expected due to high fertility rates, with sub-Saharan Africa accounting for most of the increase. Modern contraceptive use is the best option to reduce the high fertility rate. There is limited information on the prevalence of modern contraception and its predictors in sub-Saharan Africa’s high-fertility countries. Therefore, this study aimed to assess the prevalence and predictors of modern contraception among reproductive-age women in high fertility countries in sub-Saharan Africa.
Methods
We used Demographic and Health Survey data sets from the top 10 high fertility countries in sub-Saharan Africa. Stata version 16.0 software was used to analyze the data, and all statistical analyses were completed after the data had been weighted. Multilevel binary logistic regression was performed to identify factors associated with modern contraceptive use. Adjusted odds ratio with a 95% confidence interval, and a p value < 0.05 was used to declare statistical significance.
Results
The prevalence of modern contraceptive use in all the countries considered in this study was 10.72% (95% CI 10.57, 10.87). In terms of the predictor variables, young aged women, those who had attended a primary or secondary level of formal education, women who received antenatal care follow up, women who reported distance to the health facility as not a big problem, and women from rich families were more likely to use modern contraceptives.
Conclusion
Only one in 10 women of reproductive age used modern contraceptive methods in high fertility countries in sub-Saharan Africa. To improve the use of modern contraceptives, governments and non-governmental organizations studied in the countries should intensify programs that focus on those women who are economically poor, those with no formal education, no media exposure, and those with no antenatal care follow up.
Similar content being viewed by others
Background
The availability of various modern contraceptive methods empowered women to take control of their bodies, sexuality, and decisions about whether or not to have children [1, 2]. This, however, is dependent on their social, cultural, or economic status, as well as the country in which they live [1, 3]. Modern contraception is an important mechanism for controlling high fertility and improving the physical and economic wellbeing of women and their families [4,5,6].
In the developing world, modern contraception prevents an estimated 308 million unintended pregnancies each year [3]. Additionally, modern contraceptives decreases maternal and infant mortality [9] and reduce the risk of acquiring sexually transmitted diseases [7]. Apart from these benefits, it also contributes to a healthy and productive family, food security, and sustainable development in low and middle-income countries [8, 9].
Despite the aforementioned purposes, globally, in 2019, among the 1.9 billion women of reproductive age, only 842 million are using modern contraceptive methods, with sub Saharan Africa (SSA) having the lowest prevalence [10, 11] and about 47 million women have an unmet need for modern contraceptives [12].
Population growth and fertility decisions in SSA were potentially influencing the depletion of common resources, like land and/or water. It may occur when parents place a high value on having more children to help in housework or farmwork, or when parents are unaware of the benefits of fewer children [13, 14]. Lack of adequate supply or availability is one reason for contraceptive use lags in SSA. In addition, when FP services are available, there is often low demand and low utilization [15].
Another negative externality is that gender division of labour, gender norms, access to and control over resources and decision making dimensions have been intricately linked to the utilization of family planning [16]. The ability of women to seek health services and visit health care facilities depends on their decision making autonomy [17]. Similarly, in African contexts, studies indicate that restrictions on women’s autonomy by limiting their involvement in decision-making and financial independence results in lower utilization of healthcare services [17,18,19]. Multiple barriers, such as a lack of trust in Western medicine and a desire to have large families, as well as low socioeconomic status and access to family planning clinics, influenced contraception use [20].
Although different interventions like improvement in access and uptake, integration of family planning services in primary health care facilities, and education have been made to reduce fertility in SSA [21, 22], the world bank’s 2021 report on the global fertility rate lists ten SSA countries as having high fertility rates above 5 [23], which is higher than the worldwide and African average of 2.47 and 4.44, respectively [23]. Niger (6.82), Somalia (5.98), Democratic Republic of the Congo (5.82), Mali (5.79), Chad (5.65), Angola (5.44), Burundi (5.32), Nigeria (5.32), Gambia (5.15), and Burkina Faso (5.11) have the highest fertility rates [23].
Even though the prevalence of modern contraception has increased from time to time [24], its utilization in SSA is still challenged by a weak health system [25, 26]. The family planning 2020 goal is highly ambitious and has made less progress than expected [21, 27]. The prevalence of modern contraception use in SSA countries is different across the regions [4, 28,29,30]. Increasing the use of modern contraceptives in sub-Saharan Africa is a multi-faceted problem [31], that requires adequate and sustainable policies to increase the uptake of modern contraception in the region [32, 33]. This can help to improve future programmatic and policy directions [29].
Individual studies conducted in each country in Africa varied widely [7, 29, 34]. Despite recent study was tried to assess modern contraceptive in SSA [35], the study was restricted to adolescent girls and young women. All women of reproductive age (15–49 years) were included in this study, which makes it different from the previous study. Additionally, the former study was included 29 SSA countries. The current study, on the other hand, seeks to assess modern contraceptive utilization in the top ten high fertility SSA countries. Hence, it is essential to have a clear understanding of this issue in order to implement interventions that would curb population growth, improve the physical and economic wellbeing of women and their families.
Therefore, this study was intended to estimate the prevalence and factors associated with modern contraceptive use among reproductive-age women in high fertility sub-Saharan Africa countries using multilevel modelling based on the recent Demographic and Health surveys data. The findings of this study will eventually allow policymakers, program managers, non-governmental organizations, and other stakeholders involved in family planning to develop policies and programs for the regions based on the most recent evidence.
Methods
Study settings and data source
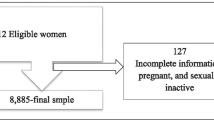
The study was a cross-sectional analysis of data from recent Demographic and Health Surveys (DHSs) conducted between January 2010 and December 2018 in nine countries in SSA. The DHS data are collected every 5 years in low-and middle-income countries using standardized, pre-tested, and validated questionnaires, and they follow a similar sampling, data collection, and coding procedure that allows for multi-country analysis. Niger, Democratic Republic Congo, Mali, Chad, Angola, Burundi, Nigeria, Gambia, and Burkina Faso were included in this study. These countries were selected because they are the top ten countries with high fertility rates in SSA, with fertility rates above 5.0, a higher value than the rate of 4.44 in SSA and 2.47 worldwide [23]. One country (Somalia) with no DHS data was excluded from the analysis. The data for these countries were obtained from the DHS program's official database, www.measuredhs.com, after permission was granted via an online request explaining the purpose of our study. We used the woman’s individual record (IR file) data set and extracted the outcome and explanatory variables. The DHS is a nationally representative household survey that uses face-to-face interviews on a wide range of population, health, nutrition tracking, and effect assessment measures. Respondents were selected using a two-stage stratified sampling technique. Enumeration Areas (EAs) were randomly selected in the first stage from the sampling frame (the frame are usually developed from the latest available national census), while households were selected by a systematic random sampling method from each cluster or EA in the second stage. Finally, interviews were conducted in selected households with target populations (women aged 15–49 and men aged 15–64). In this study, a total weighted sample of 159,014 married reproductive aged women who had given birth within the 5 years preceding the survey of each country were included. In addition, the reproductive aged women with missing values for the outcome variable were excluded from the study (Table 1).
Study variables
Outcome variable
The outcome variable of this study is modern contraceptive use. Modern contraceptive use is defined as the current use of modern methods, including pill, intrauterine device, injections, male condom, female condom, female sterilization, implant/Norplant, and emergency contraception. The outcome variable was dichotomized as yes, if the women uses the above modern methods and coded as “1”, and those who were not using any of the aforementioned methods, those using traditional methods and/or folkloric methods were considered as not using modern methods and coded as “0”) [35,36,37].
Explanatory variables
This study used the following individual and community-level variables; the individual level variables includes; age, marital status, educational status, occupation, household wealth index, media exposure, ANC visit, number of living children, place of delivery and decision making for using contraceptive methods. Whereas, residence, distance to the health facility, and community level poverty were considered under the community level variables [35, 38, 39].
Community level poverty was generated by aggregating the individual level factors at cluster level and categorized it as high if the proportion is ≥ 50% and low if the proportion is < 50% based on the national median value since the data was not normally distributed [40].
Data management and statistical analysis
Stata version 16 software was used for data analysis. We began by calculating the modern contraceptive use among married women in nine sub-Saharan African countries with high fertility rates. Secondly, we appended the dataset and this generated a total sample of 159,014 women. After appending, we compute v005/1,000,000 (Women’s individual sample weight/1,000,000) to ensure weighted representative of the DHS sample and get reliable estimates and standard errors before data analysis.
For this study, four models were fitted: the null model, which had no explanatory variables, model I, which had individual-level factors, model II, which had community-level factors. And model III, which had both individual and community-level components. Since the models were nested, the Intra-class Correlation Coefficient (ICC), Median Odds Ratio (MOR) and Likelihood Ratio test (LLR), deviance (-2LLR) values were used for model comparison and fitness, respectively. Model III was the best-fitted model since it had the lowest deviance. Variables with a p value less than 0.2 in bivariable were used for multivariable analysis. Finally, in the multivariable analysis, adjusted odds ratios with 95% confidence intervals and a p value of less than 0.05 were utilized to identify predictors of modern contraceptive use.
Ethical approval and consent to participate
The study does not involve the collection of information from subjects. Consent to respondents is not applicable since the data set used in this study is freely available and possible to download from the link: https://dhsprogram.com/data/available-datasets.cfm. All the methods were conducted according to the Helsinki declarations. The data is available without respondents identifications. Approval was sought from MEASURE DHS/ICF International and permission was granted for this use.
Results
Prevalence of modern contraceptive use
Modern contraceptive use in all the countries was 10.72% (95% CI 10.57, 10.87), with Mali recording the highest prevalence of 15.42%, while Chad had the lowest prevalence of 4.84% (Fig. 1).
Background characteristics of the respondents
A total of 159,014 weighted samples of reproductive age women in high fertility countries in SSA were included. Nearly sixty-four percent of women were from rural areas. Regarding education, 44.80% of the women had no formal education, while 22.13% had primary-level education. In terms of wealth status, 17.88% of the women fell in the poorest quintile, and 23.06% were in the richest categories (Table 2).
Random effect analysis
In the empty model, the values of Intra Class Correlation (ICC = 0.096) and Median Odds Ratio (MOR = 13.9) imply the presence of community-level variability of modern contraceptive use. Around 10% of the variation in modern contraceptive use is attributed to ICC. In the empty model, the presence of heterogeneity of modern contraceptive use between clusters is indicated by the MOR with a value of 13.9. It indicates that if we randomly select reproductive age women (15–49), a woman at the cluster with higher modern contraceptive use had around 13.9 times higher odds of modern contraceptive use than a woman at cluster with lower modern contraceptive use. Model III had the lowest deviance value (3501.5), and hence it was selected as the best-fitted model (Table 3).
Obstetric characteristics of women
Nearly ninety percent of the women had antenatal care visits. Three-fourths (73.80%) of the respondents gave birth in the health facility. Regarding decision making for using contraceptive methods, 62% had joint decisions with husbands; the majority of the women (88.1%) knew about modern contraceptive methods (Table 4).
Factors associated with the use of modern contraceptive methods
The odds of modern contraceptive use among women aged 15–24 and 25–34 years were 1.56 (95% CI 1.34–1.81) and 1.24 (95% CI 1.13–1.38) times higher than those aged 35–49 years, respectively. Women who had secondary/higher education and primary education had 3.30 (95% CI 2.92–3.73), and 1.36 (95% CI 1.22–1.52) times higher odds of modern contraceptive use, respectively as compared to those who did not attend formal education (no education). The category of women from households with the rich wealth index had 1.32 (95% CI 1.16–1.51) times higher odds of modern contraceptive use than those from poor households. The odds of modern contraceptive use was 1.68 (95% CI 1.51–1.86) times higher among women who had media exposure compared to no media exposure. The odds of modern contraceptive use was 1.33 (95% CI 1.1–1.6) times higher among those who had antenatal care compared to those who did not have antenatal care. The odds of modern contraceptive use was 1.17(95% CI 1.07–1.29) times higher among those women who reported distance to the health facility as not a big problem compared with their counterparts (Table 5).
Discussion
This study aimed to investigate the prevalence and predictors of modern contraceptive use among reproductive-age women in high fertility countries in SSA. It was found that one in ten (10.72%) reproductive age women in these countries used modern contraception, with Chad having the lowest prevalence of 4.84%. The study findings revealed that age, level of education, wealth index, media exposure, ANC follow-up, and perceived distance to the health facilities were identified as the predictive factors of modern contraceptive use.
The prevalence of modern contraceptive use among reproductive-age women in the current study is lower than a study conducted in SSA [35]. The possible justification for the discrepancy might be the difference in study population and setting, in which the previous study was conducted in SSA among adolescent girls and young women but the current study is among all reproductive age women. As older age included in the study, the prevalence might be underestimated because getting older may make women believe they will not be able to become pregnant and, consequently, not use contraceptives. Additionally, the previous study was conducted in all SSA countries, whereas the current study is focused on the top ten high fertility countries. The study was also lower than studies conducted in Ethiopia [41,42,43,44], Nigeria [45, 46], Burundi [47], and Uganda [48]. The lower prevalence of modern contraceptive use in the current study compared with the previous studies could be explained by the difference in study settings, in which the current study used the top 10 high fertility SSA countries. In contrast, the previous studies were conducted at the individual countries. In addition, this discrepancy might also result from the socio-cultural differences between countries, which may have a dramatic effect on contraceptive use.
In this study, respondents aged 15–24 and 25–34 years old were more likely to use modern contraceptive methods than older age groups. It is consistent with the studies conducted in Ethiopia [49], Mali [50], Pakistan [51], and Bangladesh [52], which indicate that the proportion of women using modern contraceptive methods increases until it reaches its peak in the 30–34 age group. The possible explanation might be that women in the 15–24 and 25–34 age group is the time most women engaged in different activities such as attending school, income generation to fulfil their needs; as a result, they want to postpone their birth. Hence, to achieve their plan, they prefer to use contraceptives. On the other hand, getting older may make women believe they will not be able to become pregnant, which may lower the utilization of modern contraceptives [41, 53].
Another important factor that significantly influenced contraceptive use in this study was education. Women with primary and secondary/higher education were 1.36 and 3.30 times more likely to use modern contraceptives than women without formal education, respectively. The finding of this study is in agreement with those of studies conducted in low and middle-income countries [54, 55]. The possible reason might be women with formal education have better exposure to contraceptives through media and other ways of exposure, which improves access to contraceptive alternatives and helps them to understand the health benefits of the contraceptive in reducing fertility, unintended pregnancy, unsafe abortion, and other maternal and child problems [54, 56]. In addition, educated women have greater autonomy in decision-making regarding contraceptive use and need [56, 57]. These suggest that educating women will be one way to improve the use of modern contraception in these high fertility countries in SSA.
The likelihood of modern contraceptive use among women from households with rich wealth quintile was higher than those from households with poor wealth quintile. This finding is supported by studies done in developing countries [58]. The reason might be that women from rich households can be able to deal with the cost barrier associated with access to contraceptive use compared to those from poor households since they can overcome both the direct and indirect costs associated with contraceptive uptake [59]. Another possible reason could be that as an income increases, exposure to different information and financial accessibility of services will be improved. Which means that their income strongly influences their decision to visit the health facility, since the higher the socio economic status the better their health because of households’ increased ability to purchase health services [60, 61].
In this study, women who had media exposure were more likely to use modern contraceptives as compared to their counterparts. The finding is consistent with the evidence from other SSA countries like Ghana [62], Mali [63], and Nigeria [64], where exposure to mass media has a substantial positive effect on contraceptive use and intended future use of contraception. The reason for this might be that women exposed to media might have a better understanding of contraception, which can bring a positive change in their attitude toward contraception [64, 65]. As a result, considering mass media exposure as a predictor of modern contraceptive use, as well as using the media to raise awareness and share information, may be very important [66].
Another factor that predicts modern contraceptive use found in our study was ANC utilization; this is congruent with a population-based survey done in Kenya and Zambia [67], where women who had ANC follow up during pregnancy had higher odds of using modern contraceptives than their counterparts. This could be due to health care providers providing information during ANC follow up about family planning helps the mothers to agree and practice contraceptive use after delivery [68]. This suggests intervention on ANC attendant women is an effective strategy to increase modern contraceptive use.
Furthermore, the odds of modern contraceptive use among women who perceived distance to the health facility as not a big problem was higher than those women who perceived distance from the health facility as a big problem. This is in line with the studies conducted in Ethiopia [69] and Turkey [70]. The possible explanation could be that women who perceive distance as not a big problem are more likely to receive the recommended maternal health care services [71]. Furthermore, previous research has found that distance to health care facilities is a significant deterrent for women seeking health care [72, 73].
Public health implications
Due to the high fertility rate, sub-Saharan Africa has contributed most of the world’s unexpected population growth. Modern contraception plays a crucial role in helping to regulate population growth, and to improve the physical and economic wellbeing of women and their families. However, in sub-Saharan African countries with high fertility, nine out of ten reproductive-age women did not use modern contraception. Thus, thousands of reproductive age women are not using any modern contraceptives. In turn, this can lead to an increase in unwanted or mistimed pregnancy rates, and sexually transmitted infections such as HIV/AIDS may be contracted as well. In order to combat the problem, nongovernmental organizations and policymakers should promote the use of modern contraception more widely in the region.
Strengths and limitations
The main strength of this study was that it used nationally representative survey data and focused on high fertility countries in SSA. In addition, the DHS uses validated instruments in its appraisals of datasets along with the large sample size and well-designed procedures, such as training field enumerators and employing well-tested methods for data collection. However, since the surveys are cross-sectional, causality cannot be established for the findings. Moreover, the difference in the survey years may affect the comparability of the results since the modernization may have an impact on modern contraceptive utilization in more recent surveys compared to older ones. It is helpful to know what percentage of the “not married” women (which could involve women who are never married, divorced, separated, or cohabiting) are sexually active. However, such information is unavailable in the DHS data. Finally, it is important to note that some socio-cultural factors such as religion, which have direct or indirect effects on contraceptives use were not included.
Conclusion
Only one in ten reproductive-age women used modern contraceptive methods in high fertility countries in sub-Saharan Africa, with Chad having the lowest prevalence. Age, educational status, wealth index, antenatal care follow-up, mass media exposure, and distance to the health facilities were the predictors for utilization of modern contraceptives. Therefore, governmental and non-governmental organizations should increase programs that improve these factors when designing interventions, especially in high fertility countries in SSA, to address the problem of low contraceptive use.
Availability of data and materials
Data for this study were sourced from Demographic and Health surveys (DHS) and available here: http://dhsprogram.com/data/available-datasets.cfm.
Abbreviations
- AOR:
-
Adjusted odds ratio
- CI:
-
Confidence interval
- DHS:
-
Demographic and health survey
- ICC:
-
Intra-class correlation coefficient
- MOR:
-
Median odds ratio
- PCV:
-
Proportional change in variance
- SD:
-
Standard deviation
- SSA:
-
Sub-Saharan Africa
- WHO:
-
World Health Organization
References
Schaapveld A. vdVIKf: investing in contraception and maternal and newborn health knowledge file. Report. 2017.
Hubacher D, Trussell J. A definition of modern contraceptive methods. Contraception. 2015;92(5):420–1.
Darroch JE, Sully E, Biddlecom A. Adding it up: investing in contraception and maternal and newborn health, 2017—supplementary tables. New York: The Guttmacher Institute; 2017.
Ahinkorah BO. Predictors of unmet need for contraception among adolescent girls and young women in selected high fertility countries in sub-Saharan Africa: a multilevel mixed effects analysis. PLoS ONE. 2020;15(8): e0236352.
Darroch JE, Singh S. Trends in contraceptive need and use in developing countries in 2003, 2008, and 2012: an analysis of national surveys. Lancet. 2013;381(9879):1756–62.
Odimegwu CO, Akinyemi JO, Banjo OO, Olamijuwon E, Amoo EO. Fertility, family size preference and contraceptive use in sub-Saharan Africa: 1990–2014. Afr J Reprod Health. 2018;22(4):44–53.
Boohene E, Tsodzai J, Hardee-Cleaveland K, Weir S, Janowitz B. Fertility and contraceptive use among young adults in Harare Zimbabwe. Stud Fam plan. 1991;22(4):264–71.
Juarez F, Gayet C, Mejia-Pailles G. Factors associated with unmet need for contraception in Mexico: evidence from the national survey of demographic dynamics 2014. BMC Public Health. 2018;18(1):1–8.
Bahamondes L, Peloggia A. Modern contraceptives in sub-Saharan African countries. Lancet Glob Health. 2019;7(7):e819–20.
Kantorová V, Wheldon MC, Ueffing P, Dasgupta AN. Estimating progress towards meeting women’s contraceptive needs in 185 countries: a Bayesian hierarchical modelling study. PLoS Med. 2020;17(2): e1003026.
Biddlecom A. Population division department of economic and social affairs United Nations Secretariat New York. 2018;1–2
Darroch JE, Sedgh G, Ball H. Contraceptive technologies: responding to women’s needs. New York Guttmacher Inst. 2011;201(1):1–51.
Bongaarts J. Can family planning programs reduce high desired family size in sub-Saharan Africa? Int Perspect Sex Reprod Health. 2011;37(4):209–16.
Bongaarts J. Trends in fertility and fertility preferences in sub-Saharan Africa: the roles of education and family planning programs. Genus. 2020;76(1):1–15.
The economic rationale for investing in family planning in Sub-Saharan Africa: MAY 10, 2016 availabe at: https://blogs.worldbank.org
Bloom SS, Wypij D, Das Gupta M. Dimensions of women’s autonomy and the influence on maternal health care utilization in a north Indian city. Demography. 2001;38(1):67–78.
Tiruneh FN, Chuang K-Y, Chuang Y-C. Women’s autonomy and maternal healthcare service utilization in Ethiopia. BMC Health Serv Res. 2017;17(1):1–12.
Chima V. Women autonomy and maternal healthcare services utilization among young ever-married women in Nigeria. Int J Nurs Midwifery. 2018;10(6):62–73.
Ameyaw EK, Tanle A, Kissah-Korsah K, Amo-Adjei J. Women’s health decision-making autonomy and skilled birth attendance in Ghana. Int J Reprod Med. 2016. https://doi.org/10.1155/2016/6569514.
Ackerson K, Zielinski R. Factors influencing use of family planning in women living in crisis affected areas of sub-Saharan Africa: a review of the literature. Midwifery. 2017;54:35–60.
Aliyu AA: Family planning services in Africa: the successes and challenges. Fam Plan. 2018;69.
Shapiro D, Tambashe BO. The impact of women’s employment and education on contraceptive use and abortion in Kinshasa, Zaire. Stud Fam Plan. 1994;25:96–110.
African countries with the highest fertility rate | Statista https://worldpopulationreview.com/countries/total-fertility-rate. cited on December 8, 2021.
Emina JB, Chirwa T, Kandala N-B. Trend in the use of modern contraception in sub-Saharan Africa: Does women’s education matter? Contraception. 2014;90(2):154–61.
Tsui AO, Brown W, Li Q. Contraceptive practice in sub-Saharan Africa. Popul and Dev Rev. 2017;43(Suppl Suppl 1):166.
Mbizvo MT, Phillips SJ. Family planning: choices and challenges for developing countries. Best Pract Res Clin Obstet Gynaecol. 2014;28(6):931–43.
Ahmed S, Choi Y, Rimon JG, Alzouma S, Gichangi P, Guiella G, Kayembe P, Kibira SP, Makumbi F, OlaOlorun F. Trends in contraceptive prevalence rates in sub-Saharan Africa since the 2012 London summit on family planning: results from repeated cross-sectional surveys. Lancet Glob Health. 2019;7(7):e904–11.
Derso T, Biks GA, Yitayal M, Ayele TA, Alemu K, Demissie GD, Wolde HF, Dellie E, Azale T, Misganaw B. Prevalence and determinants of modern contraceptive utilization among rural lactating mothers: findings from the primary health care project in two northwest Ethiopian districts. BMC Womens Health. 2020;20(1):1–6.
Namasivayam A, Lovell S, Namutamba S, Schluter PJ. Predictors of modern contraceptive use among women and men in Uganda: a population-level analysis. BMJ Open. 2020;10(2): e034675.
Bolarinwa OA, Tessema ZT, Frimpong JB, Seidu A-A, Ahinkorah BO. Spatial distribution and factors associated with modern contraceptive use among women of reproductive age in Nigeria: a multilevel analysis. PLoS ONE. 2021;16(12): e0258844.
Blackstone SR, Nwaozuru U, Iwelunmor J. Factors influencing contraceptive use in sub-Saharan Africa: a systematic review. Int Q Community Health Educ. 2017;37(2):79–91.
Adedze M, Osei-Yeboah R. Underuse of modern contraception in sub-Saharan Africa: Are there implications for sustainable development and climate change? A review of the literature. Eur J Contracept Reprod Health Care. 2019;24(4):314–8.
Toffolutti V, Ma H, Menichelli G, Berlot E, Mencarini L, Aassve A. How the internet increases modern contraception uptake: evidence from eight sub-Saharan African countries. BMJ Glob Health. 2020;5(11): e002616.
Chikandiwa A, Burgess E, Otwombe K, Chimoyi L. Use of contraceptives, high risk births and under-five mortality in Sub Saharan Africa: evidence from Kenyan (2014) and Zimbabwean (2011) demographic health surveys. BMC Womens Health. 2018;18(1):1–13.
Ahinkorah BO. Predictors of modern contraceptive use among adolescent girls and young women in sub-Saharan Africa: a mixed effects multilevel analysis of data from 29 demographic and health surveys. Contracept Reprod Med. 2020;5(1):1–12.
Ahinkorah BO, Hagan JE Jr, Seidu A-A, Sambah F, Adoboi F, Schack T, Budu E. Female adolescents’ reproductive health decision-making capacity and contraceptive use in sub-Saharan Africa: What does the future hold? PLoS ONE. 2020;15(7): e0235601.
Ahinkorah BO, Budu E, Aboagye RG, Agbaglo E, Arthur-Holmes F, Adu C, Archer AG, Aderoju YBG, Seidu A-A. Factors associated with modern contraceptive use among women with no fertility intention in sub-Saharan Africa: evidence from cross-sectional surveys of 29 countries. Contracept Reprod Med. 2021;6(1):1–13.
Namasivayam A, Lovell S, Namutamba S, Schluter PJ. Improved contraceptive use among women and men in Uganda between 1995–2016: a repeated cross-sectional population study. PLoS ONE. 2019;14(7): e0219963.
Solanke BL, Oyinlola FF, Oyeleye OJ, Ilesanmi BB. Maternal and community factors associated with unmet contraceptive need among childbearing women in Northern Nigeria. Contracept Reprod Med. 2019;4(1):1–12.
Liyew AM, Teshale AB. Individual and community level factors associated with anemia among lactating mothers in Ethiopia using data from Ethiopian demographic and health survey, 2016; a multilevel analysis. BMC Public Health. 2020;20(1):1–11.
Debebe S, Limenih MA, Biadgo B. Modern contraceptive methods utilization and associated factors among reproductive aged women in rural Dembia District, northwest Ethiopia: community based cross-sectional study. Int J Reprod BioMed. 2017;15(6):367.
Belda SS, Haile MT, Melku AT, Tololu AK. Modern contraceptive utilization and associated factors among married pastoralist women in Bale eco-region, Bale Zone, South East Ethiopia. BMC Health Serv Res. 2017;17(1):1–12.
Gebre MN, Edossa ZK. Modern contraceptive utilization and associated factors among reproductive-age women in Ethiopia: evidence from 2016 Ethiopia demographic and health survey. BMC Womens Health. 2020;20(1):1–14.
Sorato MM. Assessment of modern contraceptive method utilization and associated factors among women of reproductive age group in Arba Minch town, SNNPR Ethiopia. EC Gynaecol. 2017;6:36–53.
Igbodekwe FC, Oladimeji O, Oladimeji KE, Adeoye IA, Akpa OM, Lawson L. Utilisation of modern contraceptive among women of childbearing age in resource constraint setting: evidence from 2008 national demographic and health survey in Nigeria. J Health Sci. 2014;4(3):72–8.
NPCI. International. Nigeria Demographic and Health Survey 2013. In: Abuja, Nigeria, and Rockville, Maryland, USA: National Population Commission. 2014.
Nkunzimana E, Ndoreraho A, Nyandwi J. Uptake of modern contraceptive methods among Burundian women and associated factors: analysis of demographic and health survey data, Burundi 2016–2017. East Afr Health Res J. 2021;5(1):75.
Rutaremwa G, Kabagenyi A, Wandera SO, Jhamba T, Akiror E, Nviiri HL. Predictors of modern contraceptive use during the postpartum period among women in Uganda: a population-based cross sectional study. BMC Public Health. 2015;15(1):1–9.
Tekelab T, Melka AS, Wirtu D. Predictors of modern contraceptive methods use among married women of reproductive age groups in Western Ethiopia: a community based cross-sectional study. BMC Womens Health. 2015;15(1):1–8.
Kaggwa EB, Diop N, Storey JD. The role of individual and community normative factors: a multilevel analysis of contraceptive use among women in union in Mali. Int Fam Plan Perspect. 2008. https://doi.org/10.1363/3407908.
Qazi HA, Hashmi A, Raza SA, Soomro JA, Ghauri A. Contraceptive methods and factors associated with modern contraceptive in use. 2010.
Thorvaldsen G, Islam R. Family planning knowledge and current use of contraception among the Mru indigenous women in Bangladesh: a multivariate analysis. 2012.
Zimmerman LA, Bell SO, Li Q, Morzenti A, Anglewicz P, Tsui AO, Group PPI. Individual, community and service environment factors associated with modern contraceptive use in five sub-Saharan African countries: a multilevel, multinomial analysis using geographically linked data from PMA2020. PloS one. 2019;14(6):e0218157.
Mutumba M, Wekesa E, Stephenson R. Community influences on modern contraceptive use among young women in low and middle-income countries: a cross-sectional multi-country analysis. BMC Public Health. 2018;18(1):1–9.
Remez L, Woog V, Mhloyi M. Sexual and reproductive health needs of adolescents in Zimbabwe. Issues Brief (Alan Guttmacher Inst). 2014;3:1–8.
Alemayehu GA, Fekadu A, Yitayal M, Kebede Y, Abebe SM, Ayele TA, Gizaw Z, Wubeshet M, Muchie KF, Gelagay AA. Prevalence and determinants of contraceptive utilization among married women at Dabat and demographic surveillance system site health, northwest Ethiopia. BMC Womens Health. 2018;18(1):1–7.
Ezenwaka U, Mbachu C, Ezumah N, Eze I, Agu C, Agu I, Onwujekwe O. Exploring factors constraining utilization of contraceptive services among adolescents in Southeast Nigeria: an application of the socio-ecological model. BMC Public Health. 2020;20(1):1–11.
Gwatkin DR, Rutstein S, Johnson K, Suliman E, Wagstaff A, Amouzou A. Socio-economic differences in health, nutrition, and population within developing countries. Washington, DC: World Bank; 2007. p. 287.
Hulme J, Dunn S, Guilbert E, Soon J, Norman W. Barriers and facilitators to family planning access in Canada. Healthc Policy. 2015;10(3):48.
Alaba OO, Olubusoye OE, Olaomi J. Spatial pattern and determinants of unmet need of family planning in Nigeria. South Afr Fam Pract. 2015;57(5):306–12.
Kâ MM. Micro-econometric analysis of the determinants of socio-economic in the use of basic health services in Senegal. Afr Sci J. 2022;3(12):001–001.
Appiah F, Seidu A-A, Ahinkorah BO, Baatiema L, Ameyaw EK. Trends and determinants of contraceptive use among female adolescents in Ghana: analysis of 2003–2014 demographic and health surveys. SSM Popul Health. 2020;10: 100554.
Zamawe CO, Banda M, Dube AN. The impact of a community driven mass media campaign on the utilisation of maternal health care services in rural Malawi. BMC Pregnancy Childbirth. 2016;16(1):1–8.
Ajaero CK, Odimegwu C, Ajaero ID, Nwachukwu CA. Access to mass media messages, and use of family planning in Nigeria: a spatio-demographic analysis from the 2013 DHS. BMC Public Health. 2016;16(1):1–10.
Retherford RD, Mishra VK. Media exposure increases contraceptive use. 1997.
Ghosh R, Mozumdar A, Chattopadhyay A, Acharya R. Mass media exposure and use of reversible modern contraceptives among married women in India: an analysis of the NFHS 2015–16 data. PLoS ONE. 2021;16(7): e0254400.
Do M, Hotchkiss D. Relationships between antenatal and postnatal care and post-partum modern contraceptive use: evidence from population surveys in Kenya and Zambia. BMC Health Serv Res. 2013;13(1):1–14.
Coomson JI, Manu A. Determinants of modern contraceptive use among postpartum women in two health facilities in urban Ghana: a cross-sectional study. Contracept Reprod Med. 2019;4(1):1–11.
Shiferaw S, Spigt M, Seme A, Amogne A, Skrøvseth S, Desta S, Radloff S, Tsui A, GeertJan D. Does proximity of women to facilities with better choice of contraceptives affect their contraceptive utilization in rural Ethiopia? PLoS ONE. 2017;12(11): e0187311.
Sato R, Rohr J, Huber-Krum S, Esmer Y, Okçuoğlu BA, Karadon D, Shah I, Canning D. Effect of distance to health facilities and access to contraceptive services among urban Turkish women. Eur J Contracept Reprod Health Care. 2021. https://doi.org/10.1080/13625187.2021.1906412.
Tanou M, Kamiya Y. Assessing the impact of geographical access to health facilities on maternal healthcare utilization: evidence from the Burkina Faso demographic and health survey 2010. BMC Public Health. 2019;19(1):1–8.
Baird MB, Smith CM, DeBacco KM. Perspectives of northern Ugandan health providers about the effect of cultural beliefs and practices on birth outcomes. Health Care Women Int. 2015;36(11):1208–23.
Anastasi E, Borchert M, Campbell OM, Sondorp E, Kaducu F, Hill O, Okeng D, Odong VN, Lange IL. Losing women along the path to safe motherhood: Why is there such a gap between women’s use of antenatal care and skilled birth attendance? A mixed methods study in northern Uganda. BMC Pregnancy Childbirth. 2015;15(1):1–15.
Acknowledgements
Our thanks were forwarded to the MEASURE DHS program for permitting us to obtain and use the data set for analysis.
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
WDN and DBA conceived the study, WDN, DBA, and HBE extract, analyzed, and interpreted the data. All the author’s drafted the first manuscript and write up the final manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical approval and consent to participate
The study does not involve the collection of information from subjects. Consent to respondents is not applicable since the data set used in this study is freely available and possible to download from the link: https://dhsprogram.com/data/available-datasets.cfm. All the methods were conducted according to the Helsinki declarations. The data is available without respondents identifications. Approval was sought from MEASURE DHS/ICF International and permission was granted for this use.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Negash, W.D., Eshetu, H.B. & Asmamaw, D.B. Predictors of modern contraceptive use among reproductive age women in high fertility countries in sub-Saharan Africa: evidence from demographic and health surveys. BMC Women's Health 22, 520 (2022). https://doi.org/10.1186/s12905-022-02121-1
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12905-022-02121-1