Abstract
Solitary neurofibroma is a rare benign non-odontogenic tumor. Particularly in the oral cavity, neurogenic tumors are rare, especially if they are malignant. Neurofibromas may present either as solitary lesions or as part of the generalised syndrome of neurofibromatosis or von Recklinghausen's disease of the skin. Clinically, oral neurofibromas usually appear as pediculated or sessile nodules, with slow growth and mostly without pain. The diagnosis can be confirmed by histological examination. Neurofibromas are immunopositive for the S-100 protein, indicating its neural origin. Treatment is surgical and the prognosis is excellent. For illustration a rare case of a solitary neurofibroma in the mandible is presented.
Similar content being viewed by others
Introduction
Neurogenic tumors are rare in the oral cavity, particularly so when malignant. Traumatic neuroma, although usually included with neurogenic tumors, is a reactive process rather than a true neoplasm [1]. In contrast, neurofibroma and schwannoma derive from nerve fibers, the perineurium, the endoneurium and the neurolemmomal cells [1]. Neurofibromas may present either as solitary lesions or as part of the generalised syndrome of neurofibromatosis or von Recklinghausen's disease of the skin [4–8]. Since the first description of solitary neurofibroma (neurilemmoma, schwannoma) of the oral cavity in 1954 by Bruce only few cases have been reported in the literature [2].
Epidemiology
Although neurofibroma represents one of the most common neurogenic tumors it is an uncommon intraoral tumor [3] like some other intraoral tumours [4]. Neurofibromas can be multiple or solitary. The tumor's most frequent location is the skin and its multiple appearance is highly associated with von Recklinghausen's disease and poliglandular syndrome MEN III [5–9]. It mainly appears in the third decade of life although occurrence between 10 months and 70 years old has been described. Any preference of sex is reported contradictorily [6]. There are no correlations reported with immunocompromising diseases [10].
Clinical features
Clinically, oral neurofibromas usually appear as pediculated or sessile nodule, with slow growth. They are usually painless, but pain or paresthesia may occur due to nervous compression. The most frequent location is the tongue, although they may occur at any site, especially on the palate, cheek mucosa and floor of the mouth [1, 11–14]. Even intraosseous location of the mandible has been described [15–18]. The definitive diagnosis is due to histological examination.
Pathohistological features
The macroscopic appearance of the oral neurofibroma is characterized by a whitish consistent mass with shiny surface. Microscopically the tumor is composed of an irregular pattern of proliferative spindle cells. The stroma is composed of collagen fibers and mucoid masses. Small axons all over the tumoral tissue are demonstrated with silver staining. Neurofibromas are immunopositive for the S-100 protein in 85 to 100% of the cases, indicating its neural origin [19–23].
Treatment and prognosis
Treatment of choice is surgical excision of the solitary lesions, trying to conserve the nerve from which the tumor originates [5]. Malignant transformation of solitary neurofibroma is extremely rare. Recurrence is also rare although some authors suggest higher rate of recurrence at head and neck location of solitary neurofibromas [24–28]. Therefore, the prognosis is quite excellent.
Case report
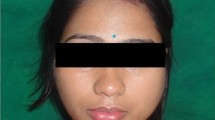
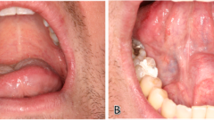
A 64-year-old male patient with a history of somewhat alcohol but no nicotine or any other diseases attended the department for Cranio- and Maxillofacial Surgery. Clinical examination revealed an exophytic tumor in the oral cavity extending all along the lingual aspect of the left mandible (fig. 1). Panoramic radiographs showed little to moderate interdental loss of bone between teeth 37 and 38 but no other abnormalities. Several biopsies from the oral cavity revealed a submucous benign mesenchymale proliferation with no signs of malignancy and thus, the tumor was completely excised under general anaesthesia (fig. 2, fig. 3). Surgical treatment also included extraction of teeth 37 and 38 and a modelling osteotomie. Immunohistochemical findings showed a solitary submucous neurofibroma with a predominate fibromatous component (fig. 4).
In the presenting case the lesion occured at the lingual site of the left mandible presenting as painless pediculated exophytic tumor with slow growth. The localisation supports the lingual nerve as origin for the neurofibroma. The patient presented no signs of von Recklinghausen disease or poliglandular syndrome. Preoperative panoramic radiographs showed no serious abnormalities. Definitive diagnosis was based upon histological and inmunohistochemical findings. A clinical follow-up has been regularly performed for one year, there was no evidence of recurrence until now.
Consent statement
Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
References
Zachariades N, Mezitis M, Vairaktaris E, Triantafyllou D, Skoura-Kafoussia C, Konsolaki-Agouridaki E, Hadjiolou E, Papavassiliou D: Benign neurogenic tumors of the oral cavity. Int J Oral Maxillofac Surg. 1987, 16: 70-76. 10.1016/S0901-5027(87)80033-4.
Bruce KW: Solitary neurofibroma (neurilemmoma, schwannoma) of the oral cavity. Oral Surg Oral Med Oral Pathol. 1954, 7: 1150-1159. 10.1016/0030-4220(54)90307-2.
Boedeker CC, Ridder GJ, Kayser G, Schipper J, Maier W: Solitary neurofibroma of the maxillary sinus and pterygopalatine fossa. Otolaryngol Head Neck Surg. 2005, 133: 458-459. 10.1016/j.otohns.2005.01.006.
Handschel J, Herbst H, Brand B, Meyer U, Piffko J: Intraoral sebaceous carcinoma. Br J Oral Maxillofac Surg. 2003, 41: 84-87. 10.1016/S0266-4356(03)00036-6.
Alatli C, Oner B, Unur M, Erseven G: Solitary plexiform neurofibroma of the oral cavity A case report. Int J Oral Maxillofac Surg. 1996, 25: 379-380. 10.1016/S0901-5027(06)80036-6.
Gomez-Oliveira G, Fernandez-Alba Luengo J, Martin-Sastre R, Patino-Seijas B, Lopez-Cedrun-Cembranos JL: Plexiform neurofibroma of the cheek mucosa. A case report. Med Oral. 2004, 9: 263-267.
Badger GR: Solitary neurofibromatosis in the maxilla: report of oral findings. J Am Dent Assoc. 1980, 100: 213-214.
Che Z, Nam W, Park WS, Kim HJ, Cha IH, Kim HS, Yook JI, Kim J, Lee SH: Intraosseous nerve sheath tumors in the jaws. Yonsei Med J. 2006, 47: 264-270. 10.3349/ymj.2006.47.2.264.
Guneri EA, Akoglu E, Sutay S, Ceryan K, Sagol O, Pabuccuoglu U: Plexiform neurofibroma of the tongue: a case report of a child. Turk J Pediatr. 2006, 48: 155-158.
Meyer U, Kleinheinz J, Handschel J, Kruse-Losler B, Weingart D, Joos U: Oral findings in three different groups of immunocompromised patients. J Oral Pathol Med. 2000, 29: 153-158. 10.1034/j.1600-0714.2000.290402.x.
Richards D: Neurofibroma of the oral cavity. Br J Oral Surg. 1983, 21: 36-43. 10.1016/0007-117X(83)90029-X.
Shimoyama T, Kato T, Nasu D, Kaneko T, Horie N, Ide F: Solitary neurofibroma of the oral mucosa: a previously undescribed variant of neurofibroma. J Oral Sci. 2002, 44: 59-63.
Sinha R, Paul R, Sen I, Sikdar B: A solitary huge neurofibroma of the soft palate. J Laryngol Otol. 2002, 116: 637-638. 10.1258/00222150260171669.
Skouteris CA, Sotereanos GC: Solitary neurofibroma of the maxilla: report of a case. J Oral Maxillofac Surg. 1988, 46: 701-705. 10.1016/0278-2391(88)90117-6.
Vivek N, Manikandhan R, James PC, Rajeev R: Solitary intraosseous neurofibroma of mandible. Indian J Dent Res. 2006, 17: 135-138. 10.4103/0970-9290.29874.
Ueda M, Suzuki H, Kaneda T: Solitary intraosseous neurofibroma of the mandible: report of a case. Nagoya J Med Sci. 1993, 55: 97-101.
Apostolidis C, Anterriotis D, Rapidis AD, Angelopoulos AP: Solitary intraosseous neurofibroma of the inferior alveolar nerve: report of a case. J Oral Maxillofac Surg. 2001, 59: 232-235. 10.1053/joms.2001.20508.
Sigillo R, Rivera H, Nikitakis NG, Sauk JJ: Neurofibromatosis type 1: a clinicopathological study of the orofacial manifestations in 6 pediatric patients. Pediatr Dent. 2002, 24: 575-580.
Fisher DA, Chu P, McCalmont T: Solitary plexiform neurofibroma is not pathognomonic of von Recklinghausen's neurofibromatosis: a report of a case. Int J Dermatol. 1997, 36: 439-442.
Johnson MD, Glick AD, Davis BW: Immunohistochemical evaluation of Leu-7, myelin basic-protein, S100-protein, glial-fibrillary acidic-protein, and LN3 immunoreactivity in nerve sheath tumors and sarcomas. Arch Pathol Lab Med. 1988, 112: 155-160.
Weiss SW, Langloss JM, Enzinger FM: Value of S-100 protein in the diagnosis of soft tissue tumors with particular reference to benign and malignant Schwann cell tumors. Lab Invest. 1983, 49: 299-308.
Depprich R, Handschel J, Sebald W, Kubler NR, Wurzler KK: [Comparison of the osteogenic activity of bone morphogenetic protein (BMP) mutants]. Mund Kiefer Gesichtschir. 2005, 9: 363-368. 10.1007/s10006-005-0644-2.
Handschel JG, Depprich RA, Dirksen D, Runte C, Zimmermann A, Kubler NR: A prospective comparison of octyl-2-cyanoacrylate and suture in standardized facial wounds. Int J Oral Maxillofac Surg. 2006, 35: 318-323. 10.1016/j.ijom.2005.10.003.
Wise JB, Patel SG, Shah JP: Management issues in massive pediatric facial plexiform neurofibroma with neurofibromatosis type 1. Head Neck. 2002, 24: 207-211. 10.1002/hed.10001.
Polak M, Polak G, Brocheriou C, Vigneul J: Solitary neurofibroma of the mandible: case report and review of the literature. J Oral Maxillofac Surg. 1989, 47: 65-68. 10.1016/0278-2391(89)90127-4.
Takahama A, Leon JE, de Almeida OP, Kowalski LP: Nonlymphoid mesenchymal tumors of the parotid gland. Oral Oncol. 2008, 44: 970-974. 10.1016/j.oraloncology.2007.12.009.
Becelli R, Renzi G, Cerulli G, Saltarel A, Perugini M: Von Recklinghausen neurofibromatosis with palatal localization. Diagnostic and surgical problems in two clinical cases. Minerva Stomatol. 2002, 51: 391-397.
Meyer U, Wiesmann HP, Berr K, Kubler NR, Handschel J: Cell-based bone reconstruction therapies-principles of clinical approaches. Int J Oral Maxillofac Implants. 2006, 21: 899-906.
Author information
Authors and Affiliations
Corresponding author
Additional information
Competing interests
All authors disclaim any financial or non-financial interests or commercial associations that might pose or create a conflict of interest with information presented in this manuscript.
Authors' contributions
DS, JH, RD and NK made substantial contribution to the conception and design of the manuscript. PR carried out the pathohistological investigations and participated in creating this part of the manuscript.
All authors were involved in revising the manuscript critically and have given final approval of the version to be published.
Authors’ original submitted files for images
Below are the links to the authors’ original submitted files for images.
Rights and permissions
Open Access This article is published under license to BioMed Central Ltd. This is an Open Access article is distributed under the terms of the Creative Commons Attribution License ( https://creativecommons.org/licenses/by/2.0 ), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Depprich, R., Singh, D.D., Reinecke, P. et al. Solitary submucous neurofibroma of the mandible: review of the literature and report of a rare case. Head Face Med 5, 24 (2009). https://doi.org/10.1186/1746-160X-5-24
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/1746-160X-5-24