Abstract
Background
Chronic gastritis, peptic ulcer disease, and gastric cancer have been shown to be related to infection with Helicobacter pylori (H. pylori). Two major virulence factors of H. pylori, CagA and VacA, have been associated with these sequelae of the infection. In this study, total DNA was isolated from gastric biopsy specimens to assess the cagA and vacA genotypes.
Results
Variations in H. pylori cagA EPIYA motifs and the mosaic structure of vacA s/m/i/d regions were analysed in 155 H. pylori-positive gastric biopsies from 71 individuals using PCR and sequencing. Analysis of a possible association between cagA and vacA genotypes and gastroduodenal pathogenesis was made by logistic regression analysis. We found that H. pylori strains with variation in the number of cagA EPIYA motif variants present in the same biopsy correlated with peptic ulcer, while occurrence of two or more EPIYA-C motifs was associated with atrophy in the gastric mucosa. No statistically significant relation between vacA genotypes and gastroduodenal pathogenesis was observed.
Conclusions
The results of this study indicate that cagA genotypes may be important determinants in the development of gastroduodenal sequelae of H. pylori infection. In contrast to other studies, vacA genotypes were not related to disease progression or outcome. In order to fully understand the relations between cagA, vacA and gastroduodenal pathogenesis, the mechanisms by which CagA and VacA act and interact need to be further investigated.
Similar content being viewed by others
Background
H. pylori is a microaerophilic, spiral shaped Gram-negative bacterium that chronically infects the gastric mucosa[1]. It is recognised as a human pathogen associated with chronic gastritis[1], peptic ulcer[2] and gastric cancer[3], the development of which are related to the virulence factors cytotoxin associated antigen (CagA)[4, 5] and vacuolating cytotoxin A (vacA)[6, 7]. It has been reported that CagA and VacA polymorphisms are associated with distinct pathological features in H. pylori infected adults with gastrointestinal diseases[8–14].
CagA has emerged as a major virulence factor for gastroduodenal disease severity, including an increased cancer risk[9, 15]. CagA is injected into epithelial cells mediated by a type IV secretion system[4, 16, 17]. In the host cell, CagA localises to the inner surface of the plasma membrane and becomes phosphorylated on specific tyrosine residues within repeating penta amino acid Glu-Pro-Ile-Tyr-Ala (EPIYA) motifs present at the C-terminus of the protein[18–20]. This part of the protein is encoded by the variable 3’-region of the cagA gene[4, 5, 21, 22] (Figure 1). Four different cagA EPIYA motifs have been defined according to the amino acid sequence that surrounds the EPIYA residues; EPIYA-A, -B, -C and -D[20, 22–25]. CagA toxins nearly always possess EPIYA-A and EPIYA-B, followed by varying numbers of EPIYA-C in Western-type isolates[22]. In East Asian-type of clinical H. pylori isolates, EPIYA-A and -B are, on the other hand, commonly followed by an EPIYA-D motif[24, 25]. It has been suggested that the considerable variation in number of repeating EPIYA-C motifs at the C-terminus of the protein may alter the biological activity of CagA in phosphorylation-dependent as well as phosphorylation-independent ways[20, 26]. It was suggested that the number of cagA EPIYA-C motifs and the tyrosine phosphorylation status of CagA are important risk factors for gastric cancer among Western strains[27]. This is also supported by a higher risk of cancer development in strains with a high degree of phosphorylation[28].
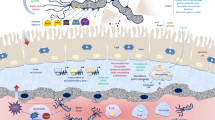
VacA induces vacuolisation in gastric epithelial cells by attaching to the cell membrane[29]. It also induces apoptosis in these cells via the mitochondrial pathway[30–33]. Initially, DNA sequence analysis revealed that the VacA protein has a mosaic structure comprising allelic variations in the signal (s) and mid region (m) (Figure 2), each having two different alleles (s1/s2, m1/m2) with different biological activities[6, 34]. The s and m regions have been associated with gastric cancer and the premalignant condition gastric mucosal atrophy[35, 36]. Recently, it was proposed that an intermediate (i) region, located between the s and m regions (Figure 2), is associated with gastric cancer[27, 37–40]. Similarly, a novel vacA gene deletion (d) region (Figure 2) has been described[36]. The d region is located between the vacA i and m regions, and involves a cleavage site crucial for the protein function and is associated with gastroduodenal diseases[36]. Amino-acid alterations in the repeated hydrophilic motif region (RHM), largely overlapping the d region of vacA, were previously shown not to be associated with any specific gastroduodenal disease[41].
Schematic illustration of the H. pylori 26695 vacA gene. The amplified signal-sequence region (SS), intermediate-region (IR), deletion-region (DR) and mid region (MR) and the primers used (Table 2) are indicated in blue. s, i/d, m indicate amplicons generated and sequenced.
H. pylori cagA and vacA gene polymorphisms are well studied and it is assumed that these polymorphisms, alone or in concert, are associated in H. pylori associated pathogenesis[9, 10, 13, 42, 43]. However, some studies have reported a lack of association between H. pylori cagA and vacA gene polymorphisms and the severity or progression of H. pylori associated diseases[25, 44].
Statistical outcome is dependent on the population studied. We aimed to analyse a randomly selected population in South-eastern Sweden with regard to H. pylori cagA and vacA genotypes and sequelae using logistic regression analysis. By means of a previously described PCR-based strategy[45, 46] we assessed variations of cagA EPIYA and vacA s/m/i/d mosaic structure present in H. pylori DNA isolated from 155 fresh frozen (−80°C) gastric biopsy specimens.
Results
Presence of H. pylori DNA in the gastric biopsy specimens
Using MDA-DNA and 16S rDNA variables V3 region pyrosequencing analysis, the presence of H. pylori-DNA in all 155 biopsy specimens was confirmed.
Analysis of cagA EPIYA motifs
A total of 155 gastric biopsy specimens from 71 individuals were analysed for cagA EPIYA genotypes. In 92 biopsy specimens a single cagA amplicon was detected. DNA sequencing revealed the presence of different cagA EPIYA genotypes: EPIYA-AB in two, ABC in 56, ABCC in 29, and ABCCC, AC, ACC, AABC, AABCC in one biopsy each (Figure 3). In 37 biopsy specimens positive for the cagA EPIYA motif, two or more cagA amplicons were detected. Of these 37 specimens, the majority (19 specimens) were mixes between ABC and ABCC (Additional file1). From 26 biopsy DNA samples, no cagA EPIYA motif amplicons could be generated.
Summary of the various cagA EPIYA motif combinations based on amplicon sequencing. The large number of genotypes presented is due to biopsies having several motif combinations (multiple amplicons). For full information about EPIYA motifs in each biopsy, see Additional file1. N = number of strains.
Statistical analysis revealed that H. pylori strains with different number of cagA EPIYA motif variants present in the same biopsy was correlated to peptic ulcer development, OR = 2.77 (1.10-7.00). In the present study, peptic ulcer included four cases of duodenal ulcers, three pre-pyloric ulcers, two gastric ulcers and five cases of previously diagnosed ulcers of undefined origin (no data available).
Two or more cagA EPIYA-C motifs were associated with development of gastric atrophy, OR = 1.86 (1.05-3.30). In biopsies with mixed amplicons, the number of EPIYA-C was determined from the amplicon with the highest number of repeats. Gastritis was histologically classified according to the Sydney system, and atrophy of the gastric mucosa was graded from 1–3 (1 = mild, 2 = moderate, 3 = severe)[47]. For the purpose of the present study, moderate to severe atrophy of the gastric mucosa was classified as atrophic gastritis.
Statistical calculations were performed also in subgroups based on the location in the stomach (corpus, antrum). No differences were observed between the groups regarding their respective disease progression.
Analysis of cagE and cag-PAI empty-site
To detect deletions of cagA within cagPAI, a region surrounding cagA (cag-PAI empty site) was amplified, as well as the cagE gene (also located within the cag-PAI). Amplification of cagE was successful in 114 of the biopsies. Of the remaining 41 biopsies, only 19 successfully amplified the cag-PAI empty site region, indicating the presence of mutated primer target sites or absence of cagE.
Analysis of vacA s/i/d/m-region
Four regions of the vacA gene (s, m, i and d regions) were genotyped. PCR amplification and DNA sequence analysis in 155 H. pylori positive biopsy specimens revealed full information from all regions of vacA in 146 samples. Of the samples genotyped in the s region, the majority were of s1a (130) or s1b (19) genotype, while only three samples were s2 genotype. In the m region the distribution was more even, with 87 samples of m1 genotype and 64 samples of m2 genotype. DNA from 32 of the biopsies displayed a deletion of the d region (d2), while 115 isolates showed wild-type sequence (d1) in this region. The intermediate region is classified according to two different sequences, and may be of i1, i2, i1-i2 or i2-i1 genotype. In this material, 94 isolates were of i1 genotype, 24 isolates of i2 genotype and 31 isolates of i2-i1 genotype. None were of i1-i2 type.
The genotypes of these regions were divided into three groups (Figure 4); group 1 contained 83 isolates of s1-d1-m1 genotype (regardless of i region), group 2 contained 30 isolates that were of d1-m2 genotypes (regardless of the s and i regions), and group 3 contained 32 isolates that were of d2 genotype (regardless of all other regions). Isolates that were indeterminate in one or more regions (n = 9) were excluded from this compilation.
In group 3, there were two isolates (6%) derived from peptic ulcer patients, while in group 1 and 2 there were 20 isolates (24%) and eight isolates (27%), respectively, originating from ulcer patients. The lower frequency of peptic ulcer observed in vacA s1d1m1 genotype compared to other genotypes was not statistically significant. Eight biopsies from group 1 (10%) and two biopsies from group 2 (7%) were derived from patients with atrophic gastritis, while in group three there was no subject with atrophic gastritis (not statistically significant).
Intraindividual variations of cagA EPIYA and vacA genotypes in corpus, antrum and duodenal bulb
In 51 of 71 individuals, biopsy specimens from all three locations of the stomach (corpus, antrum and duodenal bulb) were available for analysis. In 26 of these 51 subjects, the cagA and vacA genotypes were identical in all locations. Considering the remaining 25 subjects, 22 subjects differed with respect to the cagA EPIYA genotype, two with regard to the vacA (i) genotype, two considering the vacA (d) genotype and one with respect to the vacA (m) genotype, when comparing the locations for each subject (Additional file1).
Discussion
The results of several studies have indicated that there is an association between the cagA gene and gastric cancer[14, 27, 28, 48]. There are also reports showing an association between the vacA gene and gastroduodenal sequelae (e.g. peptic ulcer, atrophic gastritis) of H. pylori infection[36, 38–40].
Here we show that of the individuals with biopsies from all locationsns (corpus, antrum and duodenal bulb), 49% had different cagA EPIYA genotype between the three locations. There is a possibility that these individuals may have been infected with different strains on different occasions. However, it is perhaps more likely those H. pylori strains acquired genetic alterations in cagA after infection. Three recombination mechanisms have been detected in the cagA gene; homologous recombination between CM sequences, recombination between EPIYA sequences or between short similar sequences[49]. These recombination mechanisms, as well as mutations in the gene, may serve as a driving force for generating strain diversity in H. pylori, also called microevolution[50]. It is possible that infection with multiple H. pylori ancestral strains or alternatively, a single ancestral strain undergoing microevolution in the cagA gene giving rise to H. pylori subclones with different cagA EPIYA motif variants in the same biopsy specimen, may be more aggressive than a single ancestral strains acting alone. In an early study it has been suggested that the majority of Swedish clinical isolates of H. pylori from patients of higher age (>63 years old) represent single strain infections. However, in younger ages multiple strain infection may be more common[51]. Furthermore, it has been discussed that different subclones of each strain, some of which might be cagA-positive or -negative, may coexist, possibly colonising different areas of the stomach during different periods of life-long H pylori infection[51]. In this context, the aim of this study was to investigate a possible association between the presence of H. pylori cagA EPIYA motifs and disease outcome. We found an association between H. pylori DNA isolated from the same biopsy specimen and generating two or more cagA EPIYA motif variant amplicons and peptic ulcer OR = 2.77 (1.10-7.00).
Gastric atrophy was associated with two or more EPIYA-C motifs in the cagA gene of the biopsy (corpus and antrum only) H. pylori strains, OR = 1.86 (1.05-3.30). Previous studies have also found this correlation[14, 27] and it has been suggested that a higher number of EPIYA-C motifs enables a higher degree of phosphorylation, and, hence, increases the risk of gastric cancer and gastric intestinal metaplasia[28]. One explanatory mechanism in this aspect may be the interaction of CagA with the protein ASPP2, which normally activates p53 to induce apoptosis. CagA inhibits ASPP2, leading to an increased cell survival and enhanced transformation of the cell[48].
Other studies have shown an association of gastric cancer and atrophy to the s1 genotype[35], the s1m1 genotype[36], or the i1 genotype[27, 37–39]. In the present study, we detected a higher frequency of atrophy among the vacA s1d1m1 genotype than among other genotypes. However, none of these results were statistically significant, which could be due to small or unevenly distributed groups of samples (type II error).
Miernyk and co-workers observed an increased risk of developing peptic ulcer disease in s1m1 compared to s1m2/s2m2 vacA genotype[52]. Our study shows a tendency towards a similar association, although not statistically significant.
Conclusions
In summary, H. pylori strains with variation in the number of cagA EPIYA motif variants present in the same biopsy were associated with the occurrence of peptic ulcer. Similarly, two or more EPIYA-C motifs were associated with atrophy in the gastric mucosa. No statistically significant association between vacA genotypes and gastroduodenal pathogenesis was observed.
Methods
Study subjects and tissue collection
Frozen (−80°C) gastric biopsy specimens from a gastroscopic re-screening study in a randomly selected cohort of the population of Linköping, County of Östergötland, South-eastern Sweden, were used[53]. The study was approved by the local ethics committee in Linköping, Sweden (Dnr. 98007) and conducted in accordance with the Helsinki declaration. In the clinical setting, H. pylori status was classified as positive when more than one of the following occurred: H. pylori identified by light microscopic examination; a positive urease test on fresh biopsy specimen; an elevated level of H. pylori IgG antibodies in serum. Microscopic examination was performed by a single experienced pathologist who was blinded to the other data. Kappa analysis of the blinded repeat evaluation of the Sydney system scores of the biopsy sections from the antrum and corpus has been described by Redéen and co- workers[47]. From this cohort, a total of 155 biopsy specimens (61 corpus, 57 antrum and 37 from the duodenal bulb) from 71 individuals fulfilling the criteria for presence of H. pylori infection, were selected and homogenized (Table 1). In 51 individuals, biopsies from both the corpus and antrum were available (Table 1).
DNA was isolated from the homogenized tissue using an automated nucleic extractor M48 and MagAttract DNA Mini M48 kit following the manufacturer’s instruction (Qiagen, Hilden, Germany). The isolated DNA was enriched by whole genome amplification by means of multiple displacement amplification (MDA), using an Illustra GenomiPhi V2 DNA kit (GE-Healthcare, Uppsala, Sweden) according to standard protocols.
PCR amplification
Initially, the presence H. pylori DNA in the biopsy specimens were verified using 16S rDNA V3 region pyrosequencing analysis[54].
The cagA EPIYA motifs, located in the 3’-half of the cagA gene (Figure 1), were amplified using primer M13-CagA.EPIYA.SE and T7-CagA.EPIYA.AS (Figure 1; Table 2) The cagE gene and the cagA Pathogenicity Island (cag-PAI) empty site were amplified using primer M13-CagE.SE and CagE.AS, and primers M13(−21)_2.SE and T7_25.AS (Table 2), respectively.
VacA s/i/d/m region subtyping was accomplished by three single PCR amplification assays. The signal-sequence (SS) region was amplified using primer M13-SeqS.se and SeqS.as; the intermediate and deletion region (IR and DR) using primer M13-SeqVac.se and SeqVac.as; the midregion (MR) using primer M13-SeqM.se and VAG-R (Figure 2; Table 2), respectively
Amplification conditions used were identical in all assays as described previously[45]. Prior to sequencing, amplicons were analysed by automated capillary gel electrophoresis using a QIAxcel system and a QIAxcel DNA High Resolution kit (Qiagen, Hilden, Germany).
cagA EPIYA motif and vacA s/i/d/m-region sequence analysis
M13-tagged cagA EPIYA and vacA amplicons were sequenced using M13 uni (−21) sequencing primer and a customer sequencing service (Eurofins MWG Operon, Ebersberg, Germany). The obtained cagA and vacA sequences were aligned and compared with catalogued H. pylori 26695 [GenBank:AE000511, H. pylori J99 [GenBank:AE001439], H. pylori P12 [GeneBank:CP001217], H. pylori G27 [GenBank:CP001173], and H. pylori Shi470 [GeneBank:CP001072] sequences using the CLC DNA Workbench version 5.5[55]. Sequences were retrieved from the NCBI nucleotide database[56]. CagE and cag-PAI (empty-site) amplicon sizes were analysed by capillary gel electrophoresis only.
Statistical analysis
Binary logistic regression analysis of data was performed using Minitab 15 software. Statistical significance was assumed at P < 0.05. All statistical analyses presented here were significant according to Hosmer-Lemeshow (HL) goodness-of-fit test, with HL p values >0.05. In the logistic regression analysis and the GLM analysis, a 95% confidence interval including 1.0 was regarded as non-significant. Odds ratios with 95% confidence intervals (CI) were calculated to explore possible associations of individual genotypes to peptic ulcer or gastric atrophy. Age and sex were included as covariates. With regard to atrophy, data from duodenal biopsies were not included in the statistical analysis.
References
Marshall BJ, Warren JR: Unidentified curved bacilli in the stomach of patients with gastritis and peptic ulceration. Lancet. 1984, 1 (8390): 1311-1315.
Cover TL, Blaser MJ: Helicobacter pylori and gastroduodenal disease. Annu Rev Med. 1992, 43: 135-145. 10.1146/annurev.me.43.020192.001031.
Parsonnet J, Friedman GD, Vandersteen DP, Chang Y, Vogelman JH, Orentreich N, Sibley RK: Helicobacter pylori infection and the risk of gastric carcinoma. N Engl J Med. 1991, 325 (16): 1127-1131. 10.1056/NEJM199110173251603.
Covacci A, Censini S, Bugnoli M, Petracca R, Burroni D, Macchia G, Massone A, Papini E, Xiang Z, Figura N, et al: Molecular characterization of the 128-kDa immunodominant antigen of Helicobacter pylori associated with cytotoxicity and duodenal ulcer. Proc Natl Acad Sci U S A. 1993, 90 (12): 5791-5795. 10.1073/pnas.90.12.5791.
Tummuru MK, Cover TL, Blaser MJ: Cloning and expression of a high-molecular-mass major antigen of Helicobacter pylori: evidence of linkage to cytotoxin production. Infect Immun. 1993, 61 (5): 1799-1809.
Cover TL, Tummuru MK, Cao P, Thompson SA, Blaser MJ: Divergence of genetic sequences for the vacuolating cytotoxin among Helicobacter pylori strains. J Biol Chem. 1994, 269 (14): 10566-10573.
Telford JL, Ghiara P, Dell'Orco M, Comanducci M, Burroni D, Bugnoli M, Tecce MF, Censini S, Covacci A, Xiang Z, et al: Gene structure of the Helicobacter pylori cytotoxin and evidence of its key role in gastric disease. J Exp Med. 1994, 179 (5): 1653-1658. 10.1084/jem.179.5.1653.
Gangwer KA, Shaffer CL, Suerbaum S, Lacy DB, Cover TL, Bordenstein SR: Molecular evolution of the Helicobacter pylori vacuolating toxin gene vacA. J Bacteriol. 2010, 192 (23): 6126-6135. 10.1128/JB.01081-10.
Jang S, Jones KR, Olsen CH, Joo YM, Yoo YJ, Chung IS, Cha JH, Merrell DS: Epidemiological link between gastric disease and polymorphisms in VacA and CagA. J Clin Microbiol. 2010, 48 (2): 559-567. 10.1128/JCM.01501-09.
Panayotopoulou EG, Sgouras DN, Papadakos KS, Petraki K, Breurec S, Michopoulos S, Mantzaris G, Papatheodoridis G, Mentis A, Archimandritis A: CagA and VacA polymorphisms are associated with distinct pathological features in Helicobacter pylori-infected adults with peptic ulcer and non-peptic ulcer disease. J Clin Microbiol. 2010, 48 (6): 2237-2239. 10.1128/JCM.00662-10.
Rudi J, Rudy A, Maiwald M, Kuck D, Sieg A, Stremmel W: Direct determination of Helicobacter pylori vacA genotypes and cagA gene in gastric biopsies and relationship to gastrointestinal diseases. Am J Gastroenterol. 1999, 94 (6): 1525-1531. 10.1111/j.1572-0241.1999.1138_a.x.
van Doorn LJ, Figueiredo C, Sanna R, Plaisier A, Schneeberger P, de Boer W, Quint W: Clinical relevance of the cagA, vacA, and iceA status of Helicobacter pylori. Gastroenterology. 1998, 115 (1): 58-66. 10.1016/S0016-5085(98)70365-8.
Xiang Z, Censini S, Bayeli PF, Telford JL, Figura N, Rappuoli R, Covacci A: Analysis of expression of CagA and VacA virulence factors in 43 strains of Helicobacter pylori reveals that clinical isolates can be divided into two major types and that CagA is not necessary for expression of the vacuolating cytotoxin. Infect Immun. 1995, 63 (1): 94-98.
Yamaoka Y, El-Zimaity HM, Gutierrez O, Figura N, Kim JG, Kodama T, Kashima K, Graham DY: Relationship between the cagA 3' repeat region of Helicobacter pylori, gastric histology, and susceptibility to low pH. Gastroenterology. 1999, 117 (2): 342-349. 10.1053/gast.1999.0029900342.
Blaser MJ, Perez-Perez GI, Kleanthous H, Cover TL, Peek RM, Chyou PH, Stemmermann GN, Nomura A: Infection with Helicobacter pylori strains possessing cagA is associated with an increased risk of developing adenocarcinoma of the stomach. Cancer Res. 1995, 55 (10): 2111-2115.
Akopyants NS, Clifton SW, Kersulyte D, Crabtree JE, Youree BE, Reece CA, Bukanov NO, Drazek ES, Roe BA, Berg DE: Analyses of the cag pathogenicity island of Helicobacter pylori. Mol Microbiol. 1998, 28 (1): 37-53.
Yamazaki S, Yamakawa A, Ito Y, Ohtani M, Higashi H, Hatakeyama M, Azuma T: The CagA protein of Helicobacter pylori is translocated into epithelial cells and binds to SHP-2 in human gastric mucosa. J Infect Dis. 2003, 187 (2): 334-337. 10.1086/367807.
Backert S, Moese S, Selbach M, Brinkmann V, Meyer TF: Phosphorylation of tyrosine 972 of the Helicobacter pylori CagA protein is essential for induction of a scattering phenotype in gastric epithelial cells. Mol Microbiol. 2001, 42 (3): 631-644.
Hatakeyama M: Helicobacter pylori CagA-a potential bacterial oncoprotein that functionally mimics the mammalian Gab family of adaptor proteins. Microbes Infect. 2003, 5 (2): 143-150. 10.1016/S1286-4579(02)00085-0.
Higashi H, Tsutsumi R, Fujita A, Yamazaki S, Asaka M, Azuma T, Hatakeyama M: Biological activity of the Helicobacter pylori virulence factor CagA is determined by variation in the tyrosine phosphorylation sites. Proc Natl Acad Sci U S A. 2002, 99 (22): 14428-14433. 10.1073/pnas.222375399.
Yamaoka Y, Kodama T, Kashima K, Graham DY, Sepulveda AR: Variants of the 3' region of the cagA gene in Helicobacter pylori isolates from patients with different H. pylori-associated diseases. J Clin Microbiol. 1998, 36 (8): 2258-2263.
Yamazaki S, Yamakawa A, Okuda T, Ohtani M, Suto H, Ito Y, Yamazaki Y, Keida Y, Higashi H, Hatakeyama M, et al: Distinct diversity of vacA, cagA, and cagE genes of Helicobacter pylori associated with peptic ulcer in Japan. J Clin Microbiol. 2005, 43 (8): 3906-3916. 10.1128/JCM.43.8.3906-3916.2005.
Jones KR, Joo YM, Jang S, Yoo YJ, Lee HS, Chung IS, Olsen CH, Whitmire JM, Merrell DS, Cha JH: Polymorphism in the CagA EPIYA motif impacts development of gastric cancer. J Clin Microbiol. 2009, 47 (4): 959-968. 10.1128/JCM.02330-08.
Panayotopoulou EG, Sgouras DN, Papadakos K, Kalliaropoulos A, Papatheodoridis G, Mentis AF, Archimandritis AJ: Strategy to characterize the number and type of repeating EPIYA phosphorylation motifs in the carboxyl terminus of CagA protein in Helicobacter pylori clinical isolates. J Clin Microbiol. 2007, 45 (2): 488-495. 10.1128/JCM.01616-06.
Sgouras DN, Panayotopoulou EG, Papadakos K, Martinez-Gonzalez B, Roumbani A, Panayiotou J, VanVliet-Constantinidou C, Mentis AF, Roma-Giannikou E: CagA and VacA polymorphisms do not correlate with severity of histopathological lesions in Helicobacter pylori-infected Greek children. J Clin Microbiol. 2009, 47 (8): 2426-2434. 10.1128/JCM.00159-09.
Costa AC, Figueiredo C, Touati E: Pathogenesis of Helicobacter pylori infection. Helicobacter. 2009, 14 (Suppl 1): 15-20.
Basso D, Zambon CF, Letley DP, Stranges A, Marchet A, Rhead JL, Schiavon S, Guariso G, Ceroti M, Nitti D, et al: Clinical relevance of Helicobacter pylori cagA and vacA gene polymorphisms. Gastroenterology. 2008, 135 (1): 91-99. 10.1053/j.gastro.2008.03.041.
Chuang CH, Yang HB, Sheu SM, Hung KH, Wu JJ, Cheng HC, Chang WL, Sheu BS: Helicobacter pylori with stronger intensity of CagA phosphorylation lead to an increased risk of gastric intestinal metaplasia and cancer. BMC Microbiol. 2011, 11: 121-10.1186/1471-2180-11-121.
Leunk RD, Johnson PT, David BC, Kraft WG, Morgan DR: Cytotoxic activity in broth-culture filtrates of Campylobacter pylori. J Med Microbiol. 1988, 26 (2): 93-99. 10.1099/00222615-26-2-93.
Blanke SR: Micro-managing the executioner: pathogen targeting of mitochondria. Trends Microbiol. 2005, 13 (2): 64-71. 10.1016/j.tim.2004.12.007.
Cover TL, Krishna US, Israel DA, Peek RM: Induction of gastric epithelial cell apoptosis by Helicobacter pylori vacuolating cytotoxin. Cancer Res. 2003, 63 (5): 951-957.
Galmiche A, Rassow J, Doye A, Cagnol S, Chambard JC, Contamin S, de Thillot V, Just I, Ricci V, Solcia E, et al: The N-terminal 34 kDa fragment of Helicobacter pylori vacuolating cytotoxin targets mitochondria and induces cytochrome c release. EMBO J. 2000, 19 (23): 6361-6370. 10.1093/emboj/19.23.6361.
Yamasaki E, Wada A, Kumatori A, Nakagawa I, Funao J, Nakayama M, Hisatsune J, Kimura M, Moss J, Hirayama T: Helicobacter pylori vacuolating cytotoxin induces activation of the proapoptotic proteins Bax and Bak, leading to cytochrome c release and cell death, independent of vacuolation. J Biol Chem. 2006, 281 (16): 11250-11259. 10.1074/jbc.M509404200.
Atherton JC, Cao P, Peek RM, Tummuru MK, Blaser MJ, Cover TL: Mosaicism in vacuolating cytotoxin alleles of Helicobacter pylori, Association of specific vacA types with cytotoxin production and peptic ulceration. J Biol Chem. 1995, 270 (30): 17771-17777. 10.1074/jbc.270.30.17771.
Breurec S, Michel R, Seck A, Brisse S, Come D, Dieye FB, Garin B, Huerre M, Mbengue M, Fall C, et al: Clinical relevance of cagA and vacA gene polymorphisms in Helicobacter pylori isolates from Senegalese patients. Clin Microbiol Infect. 2011, 10.1111/j.1469-0691.2011.03524.x.
Ogiwara H, Sugimoto M, Ohno T, Vilaichone RK, Mahachai V, Graham DY, Yamaoka Y: Role of deletion located between the intermediate and middle regions of the Helicobacter pylori vacA gene in cases of gastroduodenal diseases. J Clin Microbiol. 2009, 47 (11): 3493-3500. 10.1128/JCM.00887-09.
Argent RH, Zhang Y, Atherton JC: Simple method for determination of the number of Helicobacter pylori CagA variable-region EPIYA tyrosine phosphorylation motifs by PCR. J Clin Microbiol. 2005, 43 (2): 791-795. 10.1128/JCM.43.2.791-795.2005.
Jones KR, Jang S, Chang JY, Kim J, Chung IS, Olsen CH, Merrell DS, Cha JH: Polymorphisms in the intermediate region of VacA impact Helicobacter pylori-induced disease development. J Clin Microbiol. 2011, 49 (1): 101-110. 10.1128/JCM.01782-10.
Rhead JL, Letley DP, Mohammadi M, Hussein N, Mohagheghi MA, Eshagh Hosseini M, Atherton JC: A new Helicobacter pylori vacuolating cytotoxin determinant, the intermediate region, is associated with gastric cancer. Gastroenterology. 2007, 133 (3): 926-936. 10.1053/j.gastro.2007.06.056.
Sheu SM, Hung KH, Sheu BS, Yang HB, Wu JJ: Association of nonsynonymous substitutions in the intermediate region of the vacA gene of Helicobacter pylori with gastric diseases in Taiwan. J Clin Microbiol. 2009, 47 (1): 249-251. 10.1128/JCM.01651-08.
Ito Y, Azuma T, Ito S, Suto H, Miyaji H, Yamazaki Y, Kohli Y, Kuriyama M: Full-length sequence analysis of the vacA gene from cytotoxic and noncytotoxic Helicobacter pylori. J Infect Dis. 1998, 178 (5): 1391-1398. 10.1086/314435.
Akada JK, Aoki H, Torigoe Y, Kitagawa T, Kurazono H, Hoshida H, Nishikawa J, Terai S, Matsuzaki M, Hirayama T, et al: Helicobacter pylori CagA inhibits endocytosis of cytotoxin VacA in host cells. Dis Model Mech. 2010, 3 (9–10): 605-617.
Oldani A, Cormont M, Hofman V, Chiozzi V, Oregioni O, Canonici A, Sciullo A, Sommi P, Fabbri A, Ricci V, et al: Helicobacter pylori counteracts the apoptotic action of its VacA toxin by injecting the CagA protein into gastric epithelial cells. PLoS Pathog. 2009, 5 (10): e1000603-10.1371/journal.ppat.1000603.
Acosta N, Quiroga A, Delgado P, Bravo MM, Jaramillo C: Helicobacter pylori CagA protein polymorphisms and their lack of association with pathogenesis. World J Gastroenterol. 2010, 16 (31): 3936-3943. 10.3748/wjg.v16.i31.3936.
Monstein HJ, Karlsson A, Ryberg A, Borch K: Application of PCR amplicon sequencing using a single primer pair in PCR amplification to assess variations in Helicobacter pylori CagA EPIYA tyrosine phosphorylation motifs. BMC Res Notes. 2010, 3: 35-10.1186/1756-0500-3-35.
Ryberg A, Borch K, Sun YQ, Monstein HJ: Concurrent genotyping of Helicobacter pylori virulence genes and human cytokine SNP sites using whole genome amplified DNA derived from minute amounts of gastric biopsy specimen DNA. BMC Microbiol. 2008, 8: 175-10.1186/1471-2180-8-175.
Redeen S, Petersson F, Kechagias S, Mardh E, Borch K: Natural history of chronic gastritis in a population-based cohort. Scand J Gastroenterol. 2010, 45 (5): 540-549. 10.3109/00365521003624151.
Buti L, Spooner E, Van der Veen AG, Rappuoli R, Covacci A, Ploegh HL: Helicobacter pylori cytotoxin-associated gene A (CagA) subverts the apoptosis-stimulating protein of p53 (ASPP2) tumor suppressor pathway of the host. Proc Natl Acad Sci U S A. 2011, 108 (22): 9238-9243. 10.1073/pnas.1106200108.
Furuta Y, Yahara K, Hatakeyama M, Kobayashi I: Evolution of cagA oncogene of Helicobacter pylori through recombination. PLoS One. 2011, 6 (8): e23499-10.1371/journal.pone.0023499.
Kraft C, Suerbaum S: Mutation and recombination in Helicobacter pylori: mechanisms and role in generating strain diversity. Int J Med Microbiol. 2005, 295 (5): 299-305. 10.1016/j.ijmm.2005.06.002.
Enroth H, Nyren O, Engstrand L: One stomach-one strain: does Helicobacter pylori strain variation influence disease outcome?. Dig Dis Sci. 1999, 44 (1): 102-107. 10.1023/A:1026658301825.
Miernyk K, Morris J, Bruden D, McMahon B, Hurlburt D, Sacco F, Parkinson A, Hennessy T, Bruce M: Characterization of Helicobacter pylori cagA and vacA Genotypes among Alaskans and Their Correlation with Clinical Disease. J Clin Microbiol. 2011, 49 (9): 3114-3121. 10.1128/JCM.00469-11.
Borch K, Jonsson KA, Petersson F, Redeen S, Mardh S, Franzen LE: Prevalence of gastroduodenitis and Helicobacter pylori infection in a general population sample: relations to symptomatology and life-style. Dig Dis Sci. 2000, 45 (7): 1322-1329. 10.1023/A:1005547802121.
Monstein HJ, Olsson C, Nilsson I, Grahn N, Benoni C, Ahrne S: Multiple displacement amplification of DNA from human colon and rectum biopsies: bacterial profiling and identification of Helicobacter pylori-DNA by means of 16S rDNA-based TTGE and pyrosequencing analysis. J Microbiol Methods. 2005, 63 (3): 239-247. 10.1016/j.mimet.2005.03.012.
CLC bio. [http://wwwclcbiocom]
NCBI-Entrez Nucleotide. [http://wwwncbinlmnihgov/nucleotide]
Acknowledgements
The study was supported by grants from the Research Council in the South-East of Sweden (FORSS, the ALF program, the committee for medical R&D, and the Molecular Biology program at Clinical Microbiology, Laboratory Medicine Centre-DC, University Hospital, Linköping, Sweden. We are grateful to Statistician Olle Eriksson, PhD, for statistical calculations and advice.
Author information
Authors and Affiliations
Corresponding author
Additional information
Competing interests
The authors declare that they have no competing interests.
Authors’ contributions
AK, AR, KB and HJM participated in the conception, design and data interpretation and drafting of the manuscript. AK, AR, MND performed the practical molecular biology procedures. KB collected and selected the biopsy specimens. All authors have been involved in drafting of the manuscript and approved the final version.
Electronic supplementary material
Authors’ original submitted files for images
Below are the links to the authors’ original submitted files for images.
Rights and permissions
Open Access This article is published under license to BioMed Central Ltd. This is an Open Access article is distributed under the terms of the Creative Commons Attribution License ( https://creativecommons.org/licenses/by/2.0 ), which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
About this article
Cite this article
Karlsson, A., Ryberg, A., Dehnoei, M.N. et al. Association between cagA and vacA genotypes and pathogenesis in a Helicobacter pylori infected population from South-eastern Sweden. BMC Microbiol 12, 129 (2012). https://doi.org/10.1186/1471-2180-12-129
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/1471-2180-12-129