Abstract
Background
Non-steroidal anti-inflammatory drugs have been shown to inhibit the development of induced neoplasms. Our previous research demonstrated that the cytotoxicity of sulindac against melanoma cells is comparable to dacarbazine, the drug used in chemotherapy. The aim of this study was to investigate the mechanism of sulindac cytotoxicity on COLO 829 and C32 cell lines.
Methods
The influence of sundilac on the activity of selected enzymes of the antioxidant system (superoxide dismutase (SOD), catalase (CAT), and glutathione peroxidase (GPx)) and the content of hydrogen peroxide as well as the level of proteins initiating (p53, Bax) and inhibiting (Bcl-2) apoptosis were measured in melanoma cells.
Results
In melanotic melanoma cells, sulindac increased the activity of SOD and the content of H2O2 but decreased the activity of CAT and GPx. The level of p53 and Bax proteins rose but the content of Bcl-2 protein was lowered. Similar results were observed for dacarbazine. In amelanotic melanoma cells, sulindac did not cause an increase in the activity of measured enzymes or any significant changes in the level of apoptotic proteins.
Conclusion
The cytotoxic effect of sulindac in the COLO 829 cell line is connected to disturbed redox homeostasis by changing the activity of SOD, CAT, GPx, and level of H2O2. Sulindac also induces apoptosis by changing the ratio of the pro-apoptotic/anti-apoptotic protein. The presented studies indicate the possibility of developing target therapy against melanotic melanoma using sulindac.
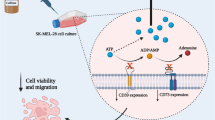
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
DNA damage may cause uncontrolled growth of cells leading to various types of cancer. Exposure to direct sunlight, especially ultraviolet light (UVB and UVA) induces the development of melanoma cells. A malignant neoplasm matures as a result of the neoplastic transformation of pigmented nevi or arises de novo in unchanged skin, mucous membranes, or the eyeball. Due to the aggressive course of the disease and the tendency to the occurrence of early and numerous metastases via the lymphatic system and bloodstream, melanoma is considered the most malignant type of skin and mucosa cancer [1, 2]. There are two basic types of melanoma, melanotic and amelanotic, of which the latter is not yet well understood. It is characterized by low melanin content and less cell differentiation, as well as a faster growth rate, greater malignancy, and worse prognosis than in the case of the melanotic variant [3, 4].
The basic method of treating melanoma is a surgical removal of the lesion. The scope of the procedure depends on the stage and location of the lesion as well as the clinical condition of the lymph nodes. Other methods, including chemotherapy, immunotherapy, targeted therapy, or radiation (phototherapy) are also often utilized [5]. Since 1975, dacarbazine has been used in chemotherapy mainly in stage IV metastatic malignant melanoma. Dacarbazine (Fig. 1) is a hydrophobic, phase-unspecific, pharmacologically inactive alkylating agent belonging to triazene. It has a short half-life and serious side effects [5]. Dacarbazine is considered the reference drug for evaluating new anti-melanoma compounds [6, 7].
The experimental and epidemiological studies conducted in recent years showed that non-steroidal anti-inflammatory drugs (NSAIDs) have anti-cancer properties [8,9,10,11,12]. The first indications of possible non-standard applications of COX inhibitors appeared in the 1980s. In experimental studies on animals, Pollard et al. [13] showed that chronic administration of indomethacin in laboratory rats with chemically induced colorectal cancer has a protective effect. The animals treated with indomethacin for several weeks had a significantly lower number and smaller size of tumors. The mechanism of NSAIDs’ anti-tumor activity is related, inter alia, to their inhibitory effect on tumor angiogenesis as well as the induction of apoptosis in neoplastic cells. Sulindac, acetylsalicylic acid, celecoxib, and indomethacin are NSAIDs often studied in the context of anti-tumor activity [5, 9, 14,15,16].
Sulindac (Fig. 1) is an indene analog of indomethacin, substituted indene acetic acid with a fluorine atom and sulfoxide group. It is used in the treatment of rheumatoid arthritis, ankylosing spondylitis, osteoarthritis, gout, and tendinitis [17]. In 1983, Waddell and Loughry [18] used sulindac in four patients with familial polyposis of the large intestine, achieving complete regression of the lesions after 1 year of treatment. Similar effects were observed after the 5 year treatment period. The key role of sulindac in the aforementioned clinical effect was confirmed by the fact that discontinuation of therapy was associated with the recurrence of the disease [19]. Over the years, the effectiveness of sulindac against various cancer lines has been proven in many experimental studies [9, 15, 20, 21]. Studies confirmed the inhibitory effect of sulindac on the NF-κB transcription factor in colon and breast cancer cells, leading to disturbance of the growth processes of neoplastic cells [15, 22]. Incubation of squamous cell carcinoma with sulindac induced apoptosis and inhibited tumor growth [23]. It was also reported that this drug downregulates Sp. transcription factors and Sp-regulated pro-oncogenic gene products [20] leading to the inhibition of cell cycle progression and induction of the apoptosis process caused by the accumulation of reactive oxygen species (ROS) in the cells. This is associated with the opening of mitochondrial channels, the release of cytochrome C, induction of p38 MAPK kinase, accumulation of pro-apoptotic proteins: p53, Bac, and Bax, and reduction in the level of the anti-apoptotic protein Bcl-2 [24]. The induction of pro-apoptotic NAG-1 protein under the influence of sulindac has also been demonstrated in studies carried out on ovarian cancer cells [25].
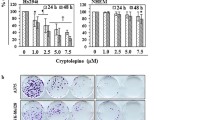
In our previous study [26], we demonstrated that the survival rate of melanotic (COLO 829) melanoma cells cultured in the presence of sulindac decreased with increasing drug concentration, and the effect was comparable to the reference drug, dacarbazine. Both tested drugs reduced the survival rate of amelanotic (C32) melanoma cells to a much lesser extent. For sulindac, 100 μM concentration exhibits the highest observed cytotoxic effect on COLO829 cells (decrease of cell viability to 53% of control). For C32 cells, sulindac did not affect viability.
This study’s aim is to investigate the cytotoxicity mechanism of sulindac on malignant melanoma cells. To determine the antioxidant potential and apoptosis induction of sulindac, the H2O2 content and activity of superoxide dismutase (SOD), catalase (CAT), and glutathione peroxide (GPx) were measured, as well as the content of apoptotic proteins: p53, Bcl-2, and Bax. The evaluation of the enzyme activities and protein levels in melanotic and amelanotic melanoma cells incubated with sulindac was compared with the reference drug, dacarbazine.
Materials and methods
Sulindac (S8139), dacarbazine (D2390), and amphotericin B (0.25 mg/ml) (A2942) were purchased from Sigma-Aldrich Inc. (USA). Growth medium RPMI 1604 with l-glutamate (L0495) and growth medium DMEM with l-glutamine (L0102) and glucose, as well as penicillin (P0018), streptomycin (S6501), and trypsin solutions (L0909) were purchased from Cytogen (Poland). Cell Proliferation Reagent I—WST-1 (11 644 807 001) was obtained from F. Hoffmann-La Roche AG.
Cell culture
Two malignant melanoma cell lines: melanotic (COLO 829) and amelanotic (C32) were purchased from ATCC. The quantitative composition of the basic culture medium for cells of the COLO829 line was: 500 ml of RMPI 1640, 55 ml of inactivated fetal bovine serum, 1 ml of solution of penicillin (10,000 U/ml) and streptomycin (10 mg/ml), 1 ml of amphotericin B solution (0.25 mg/ml). Quantitative composition of the basic culture medium for cells of the C32 line was: 500 ml of DMEM, 55 ml of inactivated fetal bovine serum, 1 ml of solution of penicillin (10,000 U/ml) and streptomycin (10 mg/ml), 1 ml of amphotericin B solution (0.25 mg/ml).
Measurements of SOD, CAT, and GPx activity in cancer cells
Superoxide dismutase activity in melanoma cells was determined using the SOD Assay Kit (706,002; Cayman Chemical). CAT activity was determined using the Catalase Assay Kit (707,002; Cayman Chemical). GPx activity was determined using the Glutathione Peroxidase Assay Kit (703,102; Cayman Chemical). Each test were performed five times with 1 × 105 cells/trial. COLO 829 melanotic melanoma cells and C32 amelanotic melanoma cells were treated with 10 µM, 50 µM, and 100 µM drug concentrations.
Determination of p53, Bcl-2, Bax proteins and H2O2 content in melanoma cells
Proteins’ content was determined in cell lysates by the modified Lowry method (sodium citrate was used), which uses a sensitive reaction of peptide bonds and aromatic amino acids with the phenolic reagent of Folin–Ciocalteu [27, 28].
Hydrogen peroxide content was determined using the OxiSelect™ Hydrogen Peroxide Assay Kit (STA-844), purchased from Cell Biolabs. Proteins p53, Bcl-2, and Bax in melanoma cells were determined by enzyme immunoassay using the following assays: human p53 ELISA (RAF082R; BioVendor), human Bcl-2 ELISA (RAF005R; BioVendor), Bax human ELISA kit (502,006,852; Enzo). Each test was performed three or four times with 2.5 × 105 cells/trial.
Statistical analysis
Mean values and standard deviations (SD) were calculated. After checking whether the distribution of results in individual groups is consistent with the normal distribution and whether the variances of comparable groups meet the assumption of homogeneity (Brown–Forsythe test), a one-way ANOVA and Dunnett’s test were used. The results were considered statistically significant at p < 0.05. GraphPadPrism 6.01 software was used to calculate the variability values.
Results
The effect of sulindac and dacarbazine on the antioxidant potential of melanotic and amelanotic melanoma cells
The effect of sulindac and dacarbazine on the antioxidant potential of melanoma cells was measured by the activity of three enzymes: superoxide dismutase (SOD), catalase (CAT), and glutathione peroxidase (GPx) as well as by the content of hydrogen peroxide in the presence of the drugs in various concentrations. The measurements of enzyme activity were performed by a spectrophotometric method using cell lysates obtained after 24 h incubation of melanoma cells in the presence of the tested drugs.
Superoxide dismutase (SOD) activity
Superoxide dismutase activity increased in melanoma cells in presence of sulindac proportional to the concentration in comparison to the control (Fig. 2). In melanotic melanoma cells incubated with 100 µM sulindac solution, the enzyme activity increased by 41.4 ± 8.7%, similar to the reference drug, dacarbazine, for which the activity increases by 37 ± 5.7%. In the case of amelanotic melanoma cells incubated in sulindac solution, the SOD activity did not change, whereas dacarbazine caused higher SOD activity than in the control sample. The effect of dacarbazine on amelanotic cells is much smaller than on melanotic melanoma cells. (sulindac: COLO 829 F3,16 = 54, p < 0.0001; C32 F3,20 = 2.1, p = 0.1377; dacarbazine: COLO 829 F3,16 = 50, p < 0.0001).
Superoxide dismutase (SOD) activity in COLO 829 melanotic and C32 amelanotic melanoma cells grown in the presence of dacarbazine and sulindac; SOD Assay Kit. One-way ANOVA followed by Dunnet’s test. The data are shown as a percentage of SOD activity to control, mean ± SD, n = 5, *p < 0.05, **p < 0.01. Circles represent individual data points. More details are included in Tables 1S and 2S in the Supplementary materials
Catalase (CAT) activity
In the presence of sulindac, the catalase activity decreased proportionally to the concentration in melanotic melanoma cells (Fig. 3) but no changes were observed for amelanotic cells. In contrast to dacarbazine, which caused a lowering of CAT activity in both types of melanoma cells. (sulindac: COLO 829 F3,16 = 38, p < 0.0001; C32 F3,20 = 0.3, p = 0.8219; dacarbazine: COLO 829 F3,16 = 18, p < 0.0001; C32 F3,20 = 10, p = 0.0002.)
Catalase (CAT) activity in COLO 829 melanotic and C32 amelanotic melanoma cells grown in the presence of dacarbazine and sulindac; Catalase Assay Kit. One-way ANOVA followed by Dunnet’s test. The data are shown as a percentage of catalase activity to control, mean ± SD, n = 3, *p < 0.05, **p < 0.01. Circles represent individual data points. More details are included in Tables 3S and 4S in the Supplementary materials
Glutathione peroxidase (GPx) activity
Sulindac and dacarbazine caused a similar effect of glutathione peroxide activity in melanotic melanoma cells. Sulindac did not affect the GPx activity of glutathione peroxidase in amelanotic melanoma cells, while dacarbazine caused a decrease in its activity compared to the control (Fig. 4). In amelanotic melanoma cells, sulindac at all tested concentrations did not cause statistically significant changes, while with increasing dacarbazine concentration, GPx activity in the tested cells decreased; however, the decrease was smaller than for melanotic melanoma cells. (sulindac: COLO 829 F3,16 = 33, p < 0.0001; C32 F3,20 = 0.97, p = 0.4258; dacarbazine: COLO 829 F3,16 = 29, p < 0.0001; C32 F3,20 = 17, p < 0.0001.)
Glutathione peroxidase (GPx) activity in COLO 829 melanotic and C32 amelanotic melanoma cells grown in the presence of dacarbazine and sulindac expressed; Glutathione Peroxidase Assay Kit. One-way ANOVA followed by Dunnet’s test. The data are shown as a percentage of glutathione peroxide activity to control, mean ± SD, n = 3, *p < 0.05, **p < 0.01. Circles represent individual data points. More details are included in Tables 5S and 6S in the Supplementary materials
Hydrogen peroxide content
The impact of sulindac and dacarbazine on the content of H2O2 in melanoma cells was also measured (Fig. 5). Hydrogen peroxide levels in melanotic melanoma cells in the presence of sulindac increased compared to the control sample. In the case of incubation of cells with dacarbazine solutions, even the lowest used concentration caused a statistically significant increase in the content of H2O2 higher than incubation with sulindac. In amelanotic melanoma cells, sulindac did not influence the level of hydrogen peroxide. On the other hand, dacarbazine caused smaller changes than in melanotic melanoma cells. (sulindac: COLO 829 F3,20 = 116, p < 0.0001; C32 F3,20 = 0.55, p = 0.6524; dacarbazine: COLO 829 F3,16 = 71, p < 0.0001; C32 F3,20 = 96, p < 0.0001.)
Hydrogen peroxide content in COLO 829 melanotic and C32 amelanotic melanoma cells grown in the presence of dacarbazine and sulindac; OxiSelectTM Hydrogen Peroxide Assay Kit. One-way ANOVA followed by Dunnet's test. The data are shown as a percentage of H2O2 content to control, mean ± SD, n = 3, *p < 0.05, **p < 0.01. Circles represent individual data points. More details are included in Tables 7S and 8S in the Supplementary materials
Effect of sulindac on the expression of apoptotic proteins in melanoma cells
The influence of sulindac and dacarbazine on their ability to initiate the process of apoptosis in malignant melanoma cells was measured by the content of p53, Bcl-2, and Bax proteins in the presence of the drugs in various concentrations. The protein content level in melanotic and amelanotic melanoma cells was determined in cell lysates after 24 h incubation with the drug.
Protein p53 content
Incubation of melanotic melanoma cells with various concentrations of sulindac increased the p53 protein content compared to the control sample (Fig. 6). A similar dependence was seen in the case of dacarbazine; increasing the drug dose increased the p53 protein content. On the other hand, the influence of the studied drugs on the p53 protein content in C32 cells was much smaller and the effect was only observed for the highest concentration of 100 μM. (sulindac: COLO 829 F3,12 = 71, p < 0.0001; C32 F3,12 = 17, p = 0.0001; dacarbazine: COLO 829 F3,12 = 66, p < 0.0001; C32 F3,20 = 33, p < 0.0001.)
p53 protein content in COLO 829 melanotic and C32 amelanotic melanoma cells grown in the presence of dacarbazine and sulindac; Human p53 ELISA (Biovendor) Kit. One-way ANOVA followed by Dunnet’s test. The data are shown as a percentage of p53 protein content to control, mean ± SD, n = 4, *p < 0.05, **p < 0.01. Circles represent individual data points. More details are included in Tables 9S and 10S in supporting information.
Bcl-2 protein content
The Bcl-2 protein content was affected by sulindac in COLO 829 cells decreasing its amount in the sample (Fig. 7). A much larger decrease was noted for the incubation of these cells with dacarbazine. In amelanotic cells, the trend was the opposite, the content of Bcl-2 protein increased in the cells for both drugs. (sulindac: COLO 829 F3,12 = 20, p < 0.0001; C32 F3,12 = 221, p < 0.0001; dacarbazine: COLO 829 F3,12 = 134, p < 0.0001; C32 F3,12 = 123, p < 0.0001).
Bcl-2 protein content in COLO 829 melanotic and C32 amelanotic melanoma cells grown in the presence of dacarbazine and sulindac; Human Bcl-2 ELISA (Biovendor) Kit. One-way ANOVA followed by Dunnet’s test. The data are shown as a percentage of Bcl-2 protein content to control, mean ± SD, n = 4, *p < 0.05, **p < 0.01. Circles represent individual data points. More details are included in Tables 11S and 12S in the Supplementary materials
Bax protein content
Both tested drugs slightly affected the Bax protein content in melanotic and amelanotic cells (Fig. 8). Only in the case of the highest concentration (100 µM), significant increase was observed compared to the control sample. Incubation of amelanotic cells with sulindac and dacarbazine caused a similar effect. (sulindac: COLO 829 F3,12 = 4.9, p = 0.0183; C32 F3,12 = 2.3, p = 0.1278; dacarbazine: COLO 829 F3,12 = 8.5, p = 0.0027; C32 F3,12 = 5.8, p = 0.0107.)
Bax protein content in COLO 829 melanotic and C32 amelanotic melanoma cells grown in the presence of dacarbazine and sulindac; Bax (human) ELISA Kit (Enzo). One-way ANOVA followed by Dunnet's test. The data are shown as a percentage of Bax protein content to control, mean ± SD, n = 4, *p < 0.05, **p < 0.01. Circles represent individual data points. More details are included in Tables 13S and 14S in the Supplementary materials
Discussion
There is a limited selection of cytostatics in systemic therapy; additionally, melanoma cells are highly resistant to most known treatments. The prognosis of patients diagnosed with melanoma is lowered, due to high resistance to the induction of apoptosis [29]. Therefore, constant efforts to develop new methods of treatment should be made. According to numerous studies, NSAIDs exhibit clinically significant anti-cancer properties, among others is sulindac [8,9,10,11,12].
In this article, we attempt to determine the mechanism of the cytotoxic mechanism of sulindac. For this purpose, the influence of the tested drug, in various concentrations, on the activity of antioxidant enzymes (SOD, CAT, and GPx) and the amount of hydrogen peroxide, as well as the content of proteins stimulating (p53, Bax) and inhibiting (Bcl-2) the apoptosis process in COLO 829 melanotic and C32 amelanotic cell lines were measured. The anti-melanoma properties of sulindac were compared with the effects of the reference drug, dacarbazine. Dacarbazine is the most commonly used drug in clinical practice during chemotherapy. The rate of response to this drug is approximately 20% [30].
Our studies showed that in COLO 829 melanotic cell line, the activity of SOD and H2O2 content increased with increasing concentration of sulindac as opposed to the activity of CAT and GPx. The content of p53 protein increased, unlike the level of Bcl-2 and Bax proteins. A stronger effect was observed when cells were incubated with dacarbazine. In C32 amelanotic cell lines, the activity of measured enzymes and the content of H2O2 as well as the level of selected proteins significantly changed neither in presence of sulindac nor dacarbazine.
The research was inspired by our previous studies, where we proved that sulindac decreases the survival rate of melanotic (COLO 829) melanoma cells and to a much lesser extent, amelanotic (C32) melanoma cells. Sulindac was much more cytotoxic to the melanotic melanoma cells of the COLO 829 line than to the amelanotic melanoma cells of the C32 line. The survival of melanoma cells was decreasing proportionally to the concentrations of sulindac. It should also be noticed that sulindac had a slightly higher cytotoxicity to melanotic melanoma cells than the reference drug, dacarbazine [26].
The cytotoxicity mechanism of sulindac was investigated by the activity of antioxidant enzymes—SOD, CAT, and GPx. Those enzymes regulate the reactive oxygen species content in the cell, changes in their activity may cause cell damage, induce apoptosis, and reduce cell proliferation [31]. The activity of antioxidant enzymes has a large influence on the treatment of many diseases, including cancer. Verm et al. [32] investigated the sulindac influence on the activity of antioxidant enzymes in rat lung cells affected by fibrosis caused by bleomycin administration. In the cells incubated with sulindac, the activity of antioxidant enzymes increases enhancing the antioxidant defence of the cells against bleomycin.
The cytotoxicity is also related to apoptosis induction. Therefore, the content of three proteins was measured—p53, Bcl-2, and Bax. The p53 protein is a transcription factor responsible for the regulation of the cell cycle and, in particular, for the activation of DNA repair and the induction of apoptosis [33]. It is inactive in the cell until the appearance of various types of stress factors, such as heat, oxidative stress, or pathological conditions associated with the genetic instability of cells and further with the development of cancer. Activation of p53 involves the phosphorylation of one of several specific Ser/Thr residues within the N-terminal or C-terminal domain of the protein due to the presence of several kinase enzymes that interact with p53 in response to a physiological imbalance in the body. When DNA repair fails, p53 initiates cell apoptosis by increasing Bax expression and mitochondrial release of cytochrome C and AIF (apoptosis-inducing factor), while reducing the concentration of Bcl-2 responsible for inhibiting the secretion of these factors [34].
Raisova et al. [35] proved that the mutual quantitative ratio of Bax and Bcl-2 proteins determines the initiation of the apoptosis process in melanoma cells of the M186 and M221 lines. For the ratio < 1 of Bax/Bcl-2 in the analyzed cells, the proliferative processes had the advantage over apoptosis. On the other hand, the increase in the Bax/Bcl-2 ratio above the > 1 value was associated with the increased sensitivity of the tested cells to the induction of the apoptosis process. In addition, the cited studies have shown that the p53 protein by attaching to the Bax protein promotes its oligomerization, which intensifies the process of apoptosis, and the occurrence of mutations within p53 reduces the intensity of this process in melanoma cells. Similar conclusions were drawn from studies by Faião-Flores et al. [36] who assessed the effect of the curcumin analog DM1 on the survival of murine melanoma cells of the B16F10 line. They recognized that the resistance of melanoma to apoptosis is one of its most important properties and that the effectiveness of anti-cancer therapy depends on the possibility of its suppression. Using the DM1 compound, scientists were able to obtain a Bax/Bcl-2 ratio of 1.1, and when DM1 was used simultaneously with dacarbazine − 1.26. Comparing these results with those obtained in this study, it can be seen that the Bax/Bcl-2 ratio obtained as a result of sulindac incubation with COLO 829 cells is much higher − 1.64 (for the highest concentration used). In turn, the Bax/Bcl-2 ratio obtained for the amelanotic line was 0.49 for sulindac and dacarbazine was 0.64. The ratio decreases with increasing p53 protein content, which confirms that the p53 protein is the basic inhibitor of the proliferation of damaged cells and the multiplication of DNA errors, and the ratio of Bax to Bcl-2 ultimately determines their survival or death.
The increased expression of Bcl-2, and more precisely the unfavorable ratio of the pro-apoptotic Bax protein to the anti-apoptotic Bcl-2 protein, determines the high resistance of this tumor to chemotherapy. Therefore, in our studies, to evaluate the effect of sulindac on the content of pro- and anti-apoptotic proteins in malignant melanoma cells, the changes in the ratio of pro- and anti-apoptotic proteins from the Bcl-2 family were observed.
The obtained results for the amelanotic line confirmed the proposed mechanism. The slight cytotoxic effect of sulindac concerning C32 cells is a consequence of the production of a large amount of Bcl-2 protein in response to the action of the drug, inhibiting the initiation of the apoptosis process, and lack of influence on the level of the pro-apoptotic protein Bax. The reference drug, in contrast to sulindac, at the highest concentration used, slightly increases the content of Bax protein and to a lesser extent increases the content of Bcl-2 protein compared to the control sample. The differences in the content of pro- and anti-apoptotic proteins may explain the higher cytotoxicity of dacarbazine against C32 amelanotic melanoma cells in comparison to sulindac.
Summarizing the obtained results, sulindac cytotoxic activity against COLO 829 melanotic melanoma cells, comparable to the reference drug, dacarbazine, is related to the induction of oxidative stress in cancer cells and the stimulation of the apoptosis process. Results may suggest that apoptosis is initiated as a result of damage to cell structures caused by reactive oxygen species. Sulindac increases the level of pro-apoptotic proteins in COLO 829 melanotic melanoma cells in contrast to C32 cells. The obtained results are the basis for further research on sulindac's influence on melanotic melanoma cells, which may be used in the future to develop new targeted therapy against melanotic melanoma cells.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Abbreviations
- SOD:
-
Superoxide dismutase,
- CAT:
-
Catalase
- GPx:
-
Glutathione peroxidase
- H2O2 :
-
Hydrogen peroxide
- COX:
-
Cyclooxygenase
- NSAIDs:
-
Non-steroidal anti-inflammatory drugs
- ROS:
-
Reactive oxygen species
- p53:
-
Tumor protein p53 or transformation-related protein 53
- Bax:
-
Pro-apoptotic protein of the Bcl-2 family (Bcl-2-associated X protein)
- Bcl-2:
-
B-cell lymphoma 2 protein, member of pro- and anti-apoptotic proteins
References
Situm M, Buljan M, Kolić M, Vučić M. Melanomam - clinical, dermatoscopic, and histopathological morphological characteristics. Acta Dermatovenerol Croat. 2014;22:1–12.
Rastrelli M, Alaibac M, Stramare R, Chiarion Sileni V, Montesco MC, Vecchiato A, et al. Melanoma m (zero): diagnosis and therapy. ISRN Dermatol. 2013;2013:616170.
Teixeira TF, Gentile LB, da Silva TC, Mennecier G, Chaible LM, Cogliati B, et al. Cell proliferation and expression of connexins differ in melanotic and amelanotic canine oral melanomas. Vet Res Commun. 2014;38:29–38.
Koch SE, Lange JR. Amelanotic melanoma: the great masquerader. J Am Acad Dermatol. 2000;42:731–4.
Wang H, Tran TT, Duong KT, Nguyen T, Le UM. Options of therapeutics and novel delivery systems of drugs for the treatment of melanoma. Mol Pharm. 2022;19:4487–505.
Al-Badr AA, Alodhaib MM. Chapter Four—Dacarbazine. In: Brittain HG, editor. Profiles of drug substances. Excipients and related methodology: Academic Press; 2016. p. 323–77.
Serrone L, Zeuli M, Sega FM, Cognetti F. Dacarbazine-based chemotherapy for metastatic melanoma: 30 year experience overview. J Exp Clin Cancer Res. 2000;19:21–34.
Cuzick J, Otto F, Baron JA, Brown PH, Burn J, Greenwald P, et al. Aspirin and non-steroidal anti-inflammatory drugs for cancer prevention: an international consensus statement. Lancet Oncol. 2009;10:501–7.
Piazza GA, Keeton AB, Tinsley HN, Whitt JD, Gary BD, Mathew B, et al. NSAIDs: old drugs reveal new anticancer targets. Pharm (Basel). 2010;3:1652–67.
Djavid AR, Stonesifer C, Fullerton BT, Wang SW, Tartaro MA, Kwinta BD, et al. Etiologies of melanoma development and prevention measures: a review of the current evidence. Cancers (Basel). 2021;13:4914.
Curiel-Lewandrowski C, Swetter SM, Einspahr JG, Hsu CH, Nagle R, Sagerman P, et al. Randomized, double-blind, placebo-controlled trial of sulindac in individuals at risk for melanoma: evaluation of potential chemopreventive activity. Cancer. 2012;118:5848–56.
Ma Y, Yu P, Lin S, Li Q, Fang Z, Huang Z. The association between nonsteroidal anti-inflammatory drugs and skin cancer: different responses in American and European populations. Pharmacol Res. 2020;152:104499.
Pollard M, Luckert PH, Schmidt MA. The suppressive effect of piroxicam on autochthonous intestinal tumors in the rat. Cancer Lett. 1983;21:57–61.
Rezania MA, Eghtedari A, Taha MF, Ardekani AM, Javeri A. A novel role for aspirin in enhancing the reprogramming function of miR-302/367 cluster and breast tumor suppression. J Cell Biochem. 2022;123:1077–90.
Loveridge CJ, MacDonald AD, Thoms HC, Dunlop MG, Stark LA. The proapoptotic effects of sulindac, sulindac sulfone and indomethacin are mediated by nucleolar translocation of the RelA(p65) subunit of NF-kappaB. Oncogene. 2008;27:2648–55.
Yin T, Wang G, Ye T, Wang Y. Sulindac, a non-steroidal anti-inflammatory drug, mediates breast cancer inhibition as an immune modulator. Sci Rep. 2016;6:19534.
Davies NM, Watson MS. Clinical Pharmacokinetics of Sulindac. Clin Pharmacokinet. 1997;32:437–59.
Waddell WR, Loughry RW. Sulindac for polyposis of the colon. J Surg Oncol. 1983;24:83–7.
Waddell WR, Ganser GF, Cerise EJ, Loughry RW. Sulindac for polyposis of the colon. Am J Surg. 1989;157:175–9.
Bock JM, Menon SG, Goswami PC, Sinclair LL, Bedford NS, Jackson RE, et al. Differential activity of sulindac metabolites against squamous cell carcinoma of the head and neck is mediated by p21waf1/cip1 induction and cell cycle inhibition. Cancer Biol Ther. 2007;6:30–9.
Han A, Song Z, Tong C, Hu D, Bi X, Augenlicht LH, et al. Sulindac suppresses beta-catenin expression in human cancer cells. Eur J Pharmacol. 2008;583:26–31.
Williams JL, Ji P, Ouyang N, Liu X, Rigas B. NO-donating aspirin inhibits the activation of NF-kappaB in human cancer cell lines and Min mice. Carcinogenesis. 2008;29:390–7.
Scheper MA, Nikitakis NG, Chaisuparat R, Montaner S, Sauk JJ. Sulindac induces Apoptosis and Inhibits Tumor Growth In Vivo in head and neck squamous cell Carcinoma. Neoplasia. 2007;9:192–9.
Seo SK, Lee HC, Woo SH, Jin HO, Yoo DH, Lee SJ, et al. Sulindac-derived reactive oxygen species induce apoptosis of human multiple myeloma cells via p38 mitogen activated protein kinase-induced mitochondrial dysfunction. Apoptosis Int J Prog Cell Death. 2007;12:195–209.
Jakubowska-Mućka A, Sieńko J, Świtaj T, Gołąb J, Lasek W. Antitumor effects of sulindac in ovarian cell cultures. Ginekol Pol. 2011;82:195–9.
Miliński M, Delijewski M, Rok J, Wrześniok D, Beberok A, Chełmecka E, et al. The pivotal effeckt of sulindac on melanin-containing cancer cells. Acta Pol Pharm. 2017;74:1681–9.
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ. Protein measurement with the Folin phenol reagent. J Biol Chem. 1951;193:265–75.
Ji TH. Interference by detergents, chelating agents, and buffers with the Lowry protein determination. Anal Biochem. 1973;52:517–21.
Rutkowski P, Świtaj T, Szacht M, Krzakowski M, Wysocki PJ, Nasierowska-Guttmejer A, et al. Czerniaki skóry-zasady postępowania diagnostyczno-terapeutycznego w 2016 roku. Dermatol Rev Przeglad Dermatol. 2016;103(6):501–16.
Koprowska K, Czyż M. Dacarbazine, a chemotherapeutic against metastatic melanoma and a reference drug for new treatment modalities. Postepy Hig Med Dosw (Online). 2011;65:734–51.
Woźniak A, Drewa G, Woźniak B, Schachtschabel DO, Mila-Kierzenkowska C, Drewa T, et al. The effect of antitumor drugs on oxidative stress in B16 and S91 melanoma cells in vitro. Med Sci Monit. 2005;11:29.
Verma R, Brahmankar M, Kushwah L, Suresh B. Evaluating the inhibitory potential of sulindac against the bleomycin-induced pulmonary fibrosis in wistar rats. Environ Toxicol Pharmacol. 2013;36:769–78.
Stanczyk M, Majsterek I. Apoptoza-cel ukierunkowanej terapii przeciwnowotworowej. Postępy Biologii Komórki. 2008;35:467–84.
Łabedzka K, Grzanka A, Izdebska M. Mitochondria and cell death. Postepy Hig Med Dosw (Online). 2006;60:439–46.
Raisova M, Hossini AM, Eberle J, Riebeling C, Wieder T, Sturm I, et al. The Bax/Bcl-2 ratio determines the susceptibility of human melanoma cells to CD95/Fas-mediated apoptosis. J Invest Dermatol. 2001;117:333–40.
Faião-Flores F, Quincoces Suarez JA, Fruet AC, Maria-Engler SS, Pardi PC, Maria DA. Curcumin analog DM-1 in monotherapy or combinatory treatment with dacarbazine as a strategy to inhibit in vivo melanoma progression. PLoS ONE. 2015;10:e0118702.
Funding
This research was funded by the Medical University of Silesia in Katowice, grant number PCN-1–013/K/2/F.
Author information
Authors and Affiliations
Contributions
MM: conceptualization, methodology, formal analysis, writing—original draft preparation; MS: writing—original draft preparation, visualization, writing—review; JR: data curation, methodology, formal analysis, writing—review and editing; AB: writing—review and editing; DW: writing—review and editing, supervision, and funding acquisition.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Miliński, M., Staś, M., Rok, J. et al. The effect of sulindac on redox homeostasis and apoptosis-related proteins in melanotic and amelanotic cells. Pharmacol. Rep 75, 995–1004 (2023). https://doi.org/10.1007/s43440-023-00493-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43440-023-00493-1