Abstract
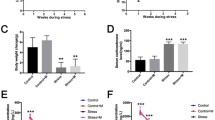
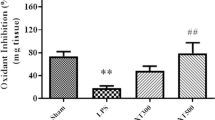
Lipopolysaccharide (LPS) — an endotoxin that is being extensively used in laboratory to mimic microbial infection that adversely affects male fertility. This study investigated the protective effects of melatonin on LPS-induced testicular nitro-oxidative stress, inflammation, and associated damages in the testes of male golden hamsters, Mesocricetus auratus. Hamsters were administered with melatonin and LPS for 7 days. Testes of LPS treated hamsters showed degenerative changes (appearance of vacuoles, exfoliation, and depletion of germ cells in the seminiferous tubules), adverse effects on spermatogenesis (sperm count and viability), and steroidogenesis (declined serum and testicular testosterone). Furthermore, LPS treatment decreased melatonin content, melatonin receptor (MT1), and antioxidant potential (catalase and SOD), and simultaneously increased nitro-oxidative stress (CRP, nitrate, TNFα). LPS upregulated NF-kB, COX-2, and iNOS expressions to increase testicular inflammatory load that resulted in the decrease of germ cell proliferation and survival, thus culminating into germ cell apoptosis as indicated by AO-EB staining and caspase-3 expression. Administration of melatonin with LPS showed improved testicular histoarchitecture, sperm parameters, and testosterone level. Melatonin increased testicular antioxidant status (SOD, catalase) to counteract the LPS-induced testicular ROS and thus reduced testicular nitro-oxidative stress. Furthermore, melatonin treatment upregulated testicular SIRT-1 expression to inhibit LPS-induced inflammatory proteins, i.e., NF-kB/COX-2/iNOS expression. The rescue effect of melatonin was further supported by increased germ cell survival (Bcl-2), proliferation (PCNA), and declined apoptosis (caspase-3). In conclusion, our result demonstrated that melatonin rescued testes from LPS-induced testicular nitro-oxidative stress, inflammation, and associated damages by upregulation of SIRT-1.








Similar content being viewed by others
References
Agarwal A, Mulgund A, Hamada A, Chyatte MR. A unique view on male infertility around the globe. Reprod Biol Endocrinol. 2015;13:37. https://doi.org/10.1186/s12958-015-0032-1.
Mima M, Greenwald D, Ohlander S. Environmental toxins and male fertility. Curr Urol Rep. 2018;19(7):50. https://doi.org/10.1007/s11934-018-0804-1.
Wang F, Liu W, Jiang Q, Gong M, Chen R, Wu H, et al. Lipopolysaccharide-induced testicular dysfunction and epididymitis in mice: a critical role of tumor necrosis factor alphadagger. Biol Reprod. 2019;100(3):849–61. https://doi.org/10.1093/biolre/ioy235.
Yang D, Wei Y, Lu Q, Qin D, Zhang M, Du X, et al. Melatonin alleviates LPS-induced endoplasmic reticulum stress and inflammation in spermatogonial stem cells. J Cell Physiol. 2020;236:3536–51. https://doi.org/10.1002/jcp.30088.
Chen YH, Xu DX, Wang JP, Wang H, Wei LZ, Sun MF, et al. Melatonin protects against lipopolysaccharide-induced intra-uterine fetal death and growth retardation in mice. J Pineal Res. 2006;40(1):40–7. https://doi.org/10.1111/j.1600-079X.2005.00274.x.
Shah SA, Khan M, Jo MH, Jo MG, Amin FU, Kim MO. Melatonin Stimulates the SIRT1/Nrf2 signaling pathway counteracting lipopolysaccharide (LPS)-induced oxidative stress to rescue postnatal rat brain. CNS Neurosci Ther. 2017;23(1):33–44. https://doi.org/10.1111/cns.12588.
Weidner W, Pilatz A, Diemer T, Schuppe HC, Rusz A, Wagenlehner F. Male urogenital infections: impact of infection and inflammation on ejaculate parameters. World J Urol. 2013;31(4):717–23. https://doi.org/10.1007/s00345-013-1082-7.
Ge L, Lin Z, Le G, Hou L, Mao X, Liu S, et al. Nontoxic-dose deoxynivalenol aggravates lipopolysaccharides-induced inflammation and tight junction disorder in IPEC-J2 cells through activation of NF-kappaB and LC3B. Food Chem Toxicol. 2020;145:111712. https://doi.org/10.1016/j.fct.2020.111712.
Cani PD, Amar J, Iglesias MA, Poggi M, Knauf C, Bastelica D, et al. Metabolic endotoxemia initiates obesity and insulin resistance. Diabetes. 2007;56(7):1761–72. https://doi.org/10.2337/db06-1491.
Flegal KM, Kruszon-Moran D, Carroll MD, Fryar CD, Ogden CL. Trends in obesity among adults in the United States, 2005 to 2014. JAMA. 2016;315(21):2284–91. https://doi.org/10.1001/jama.2016.6458.
Fang H, Liu A, Chen X, Cheng W, Dirsch O, Dahmen U. The severity of LPS induced inflammatory injury is negatively associated with the functional liver mass after LPS injection in rat model. J Inflamm (Lond). 2018;15:21. https://doi.org/10.1186/s12950-018-0197-4.
Zhao J, Bi W, Xiao S, Lan X, Cheng X, Zhang J, et al. Neuroinflammation induced by lipopolysaccharide causes cognitive impairment in mice. Sci Rep. 2019;9(1):5790. https://doi.org/10.1038/s41598-019-42286-8.
Plotnikov EY, Brezgunova AA, Pevzner IB, Zorova LD, Manskikh VN, Popkov VA, et al. Mechanisms of LPS-induced acute kidney injury in neonatal and adult rats. Antioxidants (Basel). 2018;7(8). https://doi.org/10.3390/antiox7080105.
Li M, Wang S, Li X, Jiang L, Wang X, Kou R, et al. Diallyl sulfide protects against lipopolysaccharide/d-galactosamine-induced acute liver injury by inhibiting oxidative stress, inflammation and apoptosis in mice. Food Chem Toxicol. 2018;120:500–9. https://doi.org/10.1016/j.fct.2018.07.053.
Rao F, Tian H, Li W, Hung H, Sun F. Potential role of punicalagin against oxidative stress induced testicular damage. Asian J Androl. 2016;18(4):627–32. https://doi.org/10.4103/1008-682X.168792.
Smith LB, Walker WH. The regulation of spermatogenesis by androgens. Semin Cell Dev Biol. 2014;30:2–13. https://doi.org/10.1016/j.semcdb.2014.02.012.
Hong CY, Park JH, Ahn RS, Im SY, Choi HS, Soh J, et al. Molecular mechanism of suppression of testicular steroidogenesis by proinflammatory cytokine tumor necrosis factor alpha. Mol Cell Biol. 2004;24(7):2593–604. https://doi.org/10.1128/mcb.24.7.2593-2604.2004.
Chen X, Zhang C, Zhao M, Shi CE, Zhu RM, Wang H, et al. Melatonin alleviates lipopolysaccharide-induced hepatic SREBP-1c activation and lipid accumulation in mice. J Pineal Res. 2011;51(4):416–25. https://doi.org/10.1111/j.1600-079X.2011.00905.x.
Acuna-Castroviejo D, Escames G, Venegas C, Diaz-Casado ME, Lima-Cabello E, Lopez LC, et al. Extrapineal melatonin: sources, regulation, and potential functions. Cell Mol Life Sci. 2014;71(16):2997–3025. https://doi.org/10.1007/s00018-014-1579-2.
Tordjman S, Chokron S, Delorme R, Charrier A, Bellissant E, Jaafari N, et al. Melatonin: pharmacology, functions and therapeutic benefits. Curr Neuropharmacol. 2017;15(3):434–43. https://doi.org/10.2174/1570159X14666161228122115.
Tan DX, Manchester LC, Terron MP, Flores LJ, Reiter RJ. One molecule, many derivatives: a never-ending interaction of melatonin with reactive oxygen and nitrogen species? J Pineal Res. 2007;42(1):28–42. https://doi.org/10.1111/j.1600-079X.2006.00407.x.
Kumar J, Haldar C, Verma R. Fluoride compromises testicular redox sensor, gap junction protein, and metabolic status: amelioration by melatonin. Biol Trace Elem Res. 2019;196(2):552–64. https://doi.org/10.1007/s12011-019-01946-6.
Ren Z, He H, Zuo Z, Xu Z, Wei Z, Deng J. The role of different SIRT1-mediated signaling pathways in toxic injury. Cell Mol Biol Lett. 2019;24:36. https://doi.org/10.1186/s11658-019-0158-9.
Salakou S, Kardamakis D, Tsamandas AC, Zolota V, Apostolakis E, Tzelepi V, et al. Increased Bax/Bcl-2 ratio up-regulates caspase-3 and increases apoptosis in the thymus of patients with myasthenia gravis. In Vivo. 2007;21(1):123–32.
Kaur P, Kaur G, Bansal MP. Tertiary-butyl hydroperoxide induced oxidative stress and male reproductive activity in mice: role of transcription factor NF-kappaB and testicular antioxidant enzymes. Reprod Toxicol. 2006;22:479–84. https://doi.org/. https://doi.org/10.1016/j.reprotox.2006.03.017.
Zhao L, Liu H, Yue L, Zhang J, Li X, Wang B, et al. Melatonin attenuates early brain injury via the melatonin receptor/Sirt1/NF-kappaB signaling pathway following subarachnoid hemorrhage in mice. Mol Neurobiol. 2017;54(3):1612–21. https://doi.org/10.1007/s12035-016-9776-7.
Rato L, Alves MG, Silva BM, Sousa M, Oliveira PF. Sirtuins: novel players in male reproductive health. Curr Med Chem. 2016;23(11):1084–99. https://doi.org/10.2174/0929867323666160229114248.
Mukherjee A, Haldar C, Vishwas DK. Melatonin prevents dexamethasone-induced testicular oxidative stress and germ cell apoptosis in golden hamster, Mesocricetus auratus. J Androl 2014. 2014;47(8):920–31.
Miranda KM, Espey MG, Wink DA. A rapid, simple spectrophotometric method for simultaneous detection of nitrate and nitrite. Nitric Oxide. 2001;5(1):62–71. https://doi.org/10.1006/niox.2000.0319.
Kumar J, Verma R, Haldar C. Melatonin ameliorates Bisphenol S induced testicular damages by modulating Nrf-2/HO-1 and SIRT-1/FOXO-1 expressions. Environ Toxicol. 2020;64(1):97–102. https://doi.org/10.1002/tox.23045.
Patel SK, Singh S, Singh SK. Standardized extract of Bacopa monnieri (CDRI-08): effect on germ cell dynamics and possible mechanisms of its beneficial action on spermatogenesis and sperm quality in male mice. Biochem Biophys Res Commun. 2017;494(1-2):34–41. https://doi.org/10.1016/j.bbrc.2017.10.089.
Bradford MM. A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dyebinding. Anal Biochem. 1976;72:248–54. https://doi.org/10.1016/0003-2697(76)90527-3.
Tan DX, Manchester LC, Liu X, Rosales-Corral SA, Acuna-Castroviejo D, Reiter RJ. Mitochondria and chloroplasts as the original sites of melatonin synthesis: a hypothesis related to melatonin’s primary function and evolution in eukaryotes. J Pineal Res. 2013;54(2):127–38. https://doi.org/10.1111/jpi.12026.
Mukherjee A, Haldar C. Melatonin membrane receptor (MT1R) expression and nitro-oxidative stress in testis of golden hamster, Mesocricetus auratus: an age-dependent study. Exp Gerontol. 2015;69:211–20. https://doi.org/10.1016/j.exger.2015.06.022.
Fijak M, Pilatz A, Hedger MP, Nicolas N, Bhushan S, Michel V., Tung KSK, Schuppe HC. Meinhardt A (2018). Infectious, inflammatory and “autoimmune’ male factor infertility: how do rodent models inform clinical practice? Hum Reprod Update, 24(4), 416-441. doi:https://doi.org/10.1093/humupd/dmy009
Kumar J, Haldar C, Verma R. Effect of quinalphos on testes of long day seasonal breeder golden hamster. Mesocricetus auratus J of Sc Res. 2020;64(1):97–102. https://doi.org/10.37398/JSR.2020.640114.
Galano A, Tan DX, & Reiter RJ (2013) On the free radical scavenging activities of melatonin”s metabolites, AFMK and AMK. J Pineal Res, 54(3), 245-257. doi:https://doi.org/10.1111/jpi.12010
Aitken RJ, Roman SD. Antioxidant systems and oxidative stress in the testes. Oxidative Med Cell Longev. 2008;1(1):15–24. https://doi.org/10.4161/oxim.1.1.6843.
Wong EW, Cheng CY. Impacts of environmental toxicants on male reproductive dysfunction. Trends Pharmacol Sci. 2011;32(5):290–9. https://doi.org/10.1016/j.tips.2011.01.001.
Tak PP, Firestein GS. NF-kappaB: a key role in inflammatory diseases. J Clin Invest. 2001;107(1):7–11. https://doi.org/10.1172/JCI11830.
Zhang H, Sun SC. NF-kappaB in inflammation and renal diseases. Cell Biosci. 2015;5:63. https://doi.org/10.1186/s13578-015-0056-4.
Sproston NR, Ashworth JJ. Role of C-reactive protein at sites of inflammation and infection. Front Immunol. 2018;9:754. https://doi.org/10.3389/fimmu.2018.00754.
Volanakis JE. Human C-reactive protein: expression, structure, and function. Mol Immunol. 2001;38(2-3):189–97. https://doi.org/10.1016/s0161-5890(01)00042-6.
Du Clos TW, Mold C. C-reactive protein: an activator of innate immunity and a modulator of adaptive immunity. Immunol Res. 2004;30(3):261–77. https://doi.org/10.1385/IR:30:3:261.
Ridker PM, Rifai N, Rose L, Buring JE, Cook NR. Comparison of C-reactive protein and low-density lipoprotein cholesterol levels in the prediction of first cardiovascular events. N Engl J Med. 2002;347(20):1557–65. https://doi.org/10.1056/NEJMoa021993.
van den Berg R, Haenen GR, van den Berg H, Bast A. Transcription factor NF-kappaB as a potential biomarker for oxidative stress. Br J Nutr. 2001;86(Suppl 1):S121–7. https://doi.org/10.1079/bjn2001340.
De SK, Chen HL, Pace JL, Hunt JS, Terranova PF, Enders GC. Expression of tumor necrosis factor-alpha in mouse spermatogenic cells. Endocrinology. 1993;133(1):389–96. https://doi.org/10.1210/endo.133.1.8319585.
Doshi SB, Khullar K, Sharma RK, Agarwal A. Role of reactive nitrogen species in male infertility. Reprod Biol Endocrinol. 2012;10:109. https://doi.org/10.1186/1477-7827-10-109.
Reiter RJ, Tan DX, Fuentes-Broto L. Melatonin: a multitasking molecule. Prog Brain Res. 2010;181:127–51. https://doi.org/10.1016/S0079-6123(08)81008-4.
Chang HC, Guarente L. SIRT1 and other sirtuins in metabolism. Trends Endocrinol Metab. 2014;25(3):138–45. https://doi.org/10.1016/j.tem.2013.12.001.
Lin J, Handschin C, Spiegelman BM. Metabolic control through the PGC-1 family of transcription coactivators. Cell Metab. 2005;1(6):361–70. https://doi.org/10.1016/j.cmet.2005.05.004.
Jones AW, Yao Z, Vicencio JM, Karkucinska-Wieckowska A, Szabadkai G. PGC-1 family coactivators and cell fate: roles in cancer, neurodegeneration, cardiovascular disease and retrograde mitochondria-nucleus signalling. Mitochondrion. 2012;12(1):86–99. https://doi.org/10.1016/j.mito.2011.09.009.
Richburg JH. The relevance of spontaneous- and chemically-induced alterations in testicular germ cell apoptosis to toxicology. Toxicol Lett. 2000;112-113:79–86. https://doi.org/10.1016/s0378-4274(99)00253-2.
Tousson E, Ali EM, Ibrahim W, Mansour MA. Proliferating cell nuclear antigen as a molecular biomarker for spermatogenesis in PTU-induced hypothyroidism of rats. Reprod Sci. 2011;18(7):679–86. https://doi.org/10.1177/1933719110395401.
Wang Q, Zhao XF, Ji YL, Wang H, Liu P, Zhang C, et al. Mitochondrial signaling pathway is also involved in bisphenol A induced germ cell apoptosis in testes. Toxicol Lett. 2010;199(2):129–35. https://doi.org/10.1016/j.toxlet.2010.08.014.
Kajihara T, Okagaki R, Ishihara O. LPS-induced transient testicular dysfunction accompanied by apoptosis of testicular germ cells in mice. Med Mol Morphol. 2006;39(4):203–8. https://doi.org/10.1007/s00795-006-0334-7.
Radogna F, Cristofanon S, Paternoster L, D’Alessio M, De Nicola M, Cerella C, et al. Melatonin antagonizes the intrinsic pathway of apoptosis via mitochondrial targeting of Bcl-2. J Pineal Res. 2008;44(3):316–25. https://doi.org/10.1111/j.1600-079X.2007.00532.x.
Acknowledgements
The authors gratefully acknowledge the qRT-PCR facility of the ISLS, BHU. Prof. Chandana Haldar is thankful to UGC, New Delhi, for award BSR faculty fellowship. We are thankful to Prof. Muniyandi Singaravel and Dr. Ajit Singh, Department of Zoology, BHU for extending their lab facilities. The instrument subsidiary award from the Alexander von Humboldt Foundation, Bonn, Germany to Prof. Chandana Haldar is gratefully acknowledged.
Funding
The authors received financial support from the Council of Scientific and Industrial Research (CSIR), New Delhi, Government of India, through a Senior Research Fellowship to Mr. Jitendra Kumar (grant scheme number: 09/013/(0709)/2017-EMR-I). The authors also received a research grant from the University Grants Commission, New Delhi, India, through CAS (Center of Advance Study) in the Department of Zoology, BHU.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kumar, J., Haldar, C. & Verma, R. Melatonin Ameliorates LPS-Induced Testicular Nitro-oxidative Stress (iNOS/TNFα) and Inflammation (NF-kB/COX-2) via Modulation of SIRT-1. Reprod. Sci. 28, 3417–3430 (2021). https://doi.org/10.1007/s43032-021-00597-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43032-021-00597-0