Abstract
Background
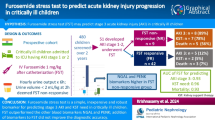
Acute kidney injury (AKI) is a major cause of morbidity and mortality in critically ill children. The aim of this paper was to describe the prevalence and course of AKI in critically ill children and to compare different AKI classification criteria.
Methods
We conducted a retrospective observational study in our multi-disciplinary Pediatric Intensive Care Unit (ICU) from January 2015 to December 2018. All patients from birth to 16 years of age who were admitted to the pediatric ICU were included. The Kidney Disease Improving Global Outcomes (KDIGO) definition was considered as the reference standard. We compared the incidence data assessed by KDIGO, pediatric risk, injury, failure, loss of kidney function and end- stage renal disease (pRIFLE) and pediatric reference change value optimised for AKI (pROCK).
Results
Out of 7505 patients, 9.2% developed AKI by KDIGO criteria. The majority (59.8%) presented with stage 1 AKI. Recovery from AKI was observed in 70.4% of patients within 7 days from diagnosis. Both pRIFLE and pROCK were less sensitive compared to KDIGO criteria for the classification of AKI. Patients who met all three—KDIGO, pRIFLE and pROCK criteria had a high mortality rate (35.0%).
Conclusion
Close to one in ten patients admitted to the pediatric ICU met AKI criteria according to KDIGO. In about 30% of patients, AKI persisted beyond 7 days. Follow-up of patients with persistent kidney function reduction at hospital discharge is needed to reveal the long-term morbidity due to AKI in the pediatric ICU.
Graphic abstract



Similar content being viewed by others
Availability of data and materials
All data generated or analyzed during this study are included in this published article and its supplementary material.
References
Kaddourah A, Basu RK, Bagshaw SM et al (2017) Epidemiology of acute kidney injury in critically ill children and young adults. N Engl J Med 376:11–20
Kari JA, Alhasan KA, Shalaby MA et al (2018) Outcome of pediatric acute kidney injury: a multicenter prospective cohort study. Pediatr Nephrol 33:335–340
Kidney disease: Improving global outcomes (KDIGO) Acute Kidney Injury Work Group (2012) KDIGO clinical practice guideline for acute kidney injury. Kidney Int Suppl 2:1–138
Akcan-Arikan A, Zappitelli M, Loftis LL et al (2007) Modified RIFLE criteria in critically ill children with acute kidney injury. Kidney Int 71:1028–1035
Xu X, Nie S, Zhang A et al (2018) A new criterion for pediatric AKI based on the reference change value of serum creatinine. J Am Soc Nephrol 29(9):2432–2442
Hessey E, Morissette G, Lacroix J et al (2018) Healthcare utilization after acute kidney injury in the pediatric intensive care unit. Clin J Am Soc Nephrol 13:685–692
Coca SG, Yusuf B, Shlipak MG, Garg AX, Parikh CR (2009) Long-term risk of mortality and other adverse outcomes after acute kidney injury: a systematic review and meta-analysis. Am J Kidney Dis 53:961–973
Chawla LS, Bellomo R, Bihorac A, Goldstein SL, Siew ED, Bagshaw SM, Bittleman D, Cruz D, Endre Z, Fitzgerald RL, Forni L, Kane-Gill SL, Hoste E, Koyner J, Liu KD, Macedo E, Mehta R, Murray P, Nadim M, Ostermann M, Palevsky PM, Pannu N, Rosner M, Wald R, Zarbock A, Ronco C, Kellum JA (2017) Acute disease quality initiative workgroup 16. Acute kidney disease and renal recovery: consensus report of the acute disease quality initiative (ADQI) 16 workgroup. Nat Rev Nephrol 13:241–257
Macedo E, Cerda J, Hingorani S, Hou J, Bagga A, Burdmann EA, Rocco M, Mehta R (2018) Recognition and management of acute kidney injury in children: the ISN 0by25 Global Snapshot study. PLoS ONE 13(5):e0196586
Hessey E, Ali R, Dorais M, Morissette G, Pizzi M, Rink N et al (2017) Renal function follow-up and renal recovery after acute kidney injury in critically ill children. Pediatr Crit Care Med 18(8):733–740
Mammen C, Abbas AA, Skippen P, Nadel H, Levine D, Collet JP, Matsell DG (2012) Long-term risk of CKD in children surviving episodes of acute kidney injury in the intensive care unit: a prospective cohort study. Am J Kidney Dis 59(4):523–530
Raman S, Tai CW, le Marsney R, Schibler A, Gibbons K, Schlapbach LJ (2020) Prediction of acute kidney injury on admission to pediatric intensive care. Pediatr Crit Care Med 21(9):811–819
Boer DP, De Rijke YB, Hop WC et al (2010) Reference values for serum creatinine in children younger than 1 year of age. Pediatr Nephrol 25:2107–2113
Ceriotti F, Boyd JC, Klein G et al (2008) Reference intervals for serum creatinine concentrations: assessment of available data for global application. Clin Chem 54:559–566
Slater A, Shann F, McEniery J et al (2003) The ANZPIC Registry diagnostic codes: a system for coding reasons for admitting children to intensive care. Intensive Care Med 29:271–277
Australia and New Zealand Intensive Care Society (2020) Australian and New Zealand Paediatric Intensive Care (ANZPIC) Diagnostic Codes. https://www.anzics.com.au/wp-content/uploads/2019/07/ANZPICR-Diagnostic-Codes.pdf. Assessed 1 Dec 2020
Ping Kirk AH, Sng QW, Zhang LQ, Ming Wong JJ, Puthucheary J, Lee JH (2018) Characteristics and outcomes of long-stay patients in the pediatric intensive care unit. J Pediatr Intensive Care 7(1):1–6
James MT, Bhatt M, Pannu N, Tonelli M (2020) Long-term outcomes of acute kidney injury and strategies for improved care. Nat Rev Nephrol 16:193–205
Lebel A, Teoh CW, Zappitelli M (2020) Long-term complications of acute kidney injury in children. Curr Opin Pediatr 32(3):367–375
Sutherland SM, Brynes JJ, Kothari M, Longhurst CA, Dutta S, Garcia P, Goldstein SL (2015) AKI in hospitalized children: comparing the pRIFLE, AKIN and KDIGO definitions. Clin J Am Soc Nephrol 10(4):554–561
Luo X, Jiang L, Du B et al (2014) A comparison of different diagnostic criteria of acute kidney injury in critically ill patients. Crit Care 18:R144
Acknowledgements
We thank the pediatric ICU Metavision data management team for their help with data extraction for this study. Special thanks to Endrias Ergetu (Paediatric Critical Care Research Group, Child Health Research Centre, The University of Queensland, Queensland, Australia) for his help with the digital artwork.
Funding
LJS is supported by a Practitioner Fellowship of the National Health and Medical Research Council of Australia and New Zealand, and by the Children`s Hospital Foundation, Brisbane, Australia.
Author information
Authors and Affiliations
Contributions
CWT and SR verified the data extraction codes, analyzed the data and wrote the first draft of the article. KG and SR checked accuracy of data analysis. CWT, AS, LJS and SR contributed to design of the study, interpretation of findings and manuscript writing. All authors read and approved the final manuscript except AS who was unfortunately very ill.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethics approval
Ethics approval was obtained from Children’s Health Queensland HREC (HREC/17/QRCH/287). A waiver of consent for access to patient records was granted.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tai, C.W., Gibbons, K., Schibler, A. et al. Acute kidney injury: epidemiology and course in critically ill children. J Nephrol 35, 559–565 (2022). https://doi.org/10.1007/s40620-021-01071-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-021-01071-5