Abstract
Objective
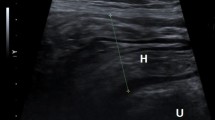
Ultrasonography (US) is a non-invasive, non-ionizing radiation modality highly successful at diagnosing inguinal hernia. The aim of this study is to demonstrate the accuracy of ultrasound in evaluating defects of fascia in inguinal hernias and compare with surgical findings.
Material and methods
A total of 33 patients with a sonographic diagnosis of an inguinal hernia are included to study. After US, all patients underwent a blinded surgery and the surgical findings are compared with the US results.
Results
The sensitivity of US was found to be 100% and 80% for indirect and direct types, respectively. The mean size of the defect was found to be 22 mm (max: 70 mm, min: 6 mm) with US; and 27 mm (max: 50 mm, min: 4 mm) at surgery. The size of defects at US and in surgery were correlated with each other (p = 0.001).


Similar content being viewed by others
References
Burkhardt JH, Arshanskiy Y, Munson JL, Scholz FJ (2011) Diagnosis of inguinal region hernias with axial CT: the lateral crescent sign and other key findings. Radiographics 31(2):E1–E12
Robinson A, Light D, Kasim A, Nice C (2013) A systematic review and meta-analysis of the role of radiology in the diagnosis of occult inguinal hernia. Surg Endosc 27(1):11–18
Arend CF (2013) Static and dynamic sonography for diagnosis of abdominal wall hernias. J Ultrasound Med 32(7):1251–1259
van den Berg JC (2002) Inguinal hernias: MRI and ultrasound. Semin Ultrasound CT MR 23(2):156–173
Duarte BHF, Iamarino APM, Gabor S, Favaro ML, Juliano Y, Novo NF et al (2019) Accuracy of the ultrasound examination in patients with inguinal hernia. Rev Col Bras Cir 46(2):2108
Jansen CJ, Yielder PC (2018) Evaluation of hernia of the male inguinal canal: sonographic method. J Med Radiat Sci 65(2):163–168
Bradley M, Morgan D, Pentlow B, Roe A (2003) The groin hernia—an ultrasound diagnosis? Ann R Coll Surg Engl 85(3):178–180
Simons MP, Aufenacker T, Bay-Nielsen M, Bouillot JL, Campanelli G, Conze J et al (2009) European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia 13(4):343–403
van den Berg JC, de Valois JC, Go PM, Rosenbusch G (1999) Detection of groin hernia with physical examination, ultrasound, and MRI compared with laparoscopic findings. Invest Radiol 34(12):739–743
Kim B, Robinson P, Modi H, Gupta H, Horgan K, Achuthan R (2015) Evaluation of the usage and influence of groin ultrasound in primary and secondary healthcare settings. Hernia 19(3):367–371
Matthews RD, Neumayer L (2008) Inguinal hernia in the 21st century: an evidence-based review. Curr Probl Surg 45(4):261–312
Piga E, Zetner D, Andresen K, Rosenberg J (2020) Imaging modalities for inguinal hernia diagnosis: a systematic review. Hernia 24(5):917–926
Babkova IV, Bozhko VV (1999) Ultrasound assessment in diagnosis of uncomplicated inguinal hernia. Khirurgiia (Mosk) 2:46–50
Li B, Qin C, Yu J, Gong D, Nie X, Li G et al (2021) Totally endoscopic sublay (TES) repair for lateral abdominal wall hernias: technique and first results. Hernia 25(2):523–533
Funding
The authors declared that this study has received no financial support.
Author information
Authors and Affiliations
Contributions
Concept: MAG; Design: MAG, MTK; Supervision: AKB, Funding: MAG, AKB; Materials: MAG, AKB; Data Collection and/or Processing: MAG, AKB; Analysis and/or Interpretation: AKB, MTK; Literature Review: MTK; Writer: MAG, AKB, MTK; Critical Review: MTK.
Corresponding author
Ethics declarations
Conflict of interest
No conflict of interest was declared by the authors.
Ethical approval
This study was approved by Health Sciences University Kartal Dr Lütfi Kırdar City Hospital Institutional Ethics Committee (Protocol number: 514/196/1- 24.02.2021).
Informed consent
Written informed consent was obtained from patient who participated in this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gök, M.A., Büyüközsoy, A.K. & Kafadar, M.T. The sensitivity of ultrasound in the clinical diagnosis of inguinal hernias in adults: a comparative study. J Ultrasound 25, 655–658 (2022). https://doi.org/10.1007/s40477-021-00641-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40477-021-00641-4