Abstract
Introduction
Uric acid (UA), the final product of purine catabolism, may be associated with an increased risk of cardiovascular disease.
Aim
The aim of this meta-analysis of randomized placebo-controlled trials was to evaluate whether lowering serum UA (SUA) levels with allopurinol is associated with improved flow-mediated dilation (FMD), a validated marker of early vascular damage.
Methods
A literature search was carried out from inception until 20 June 2017. Meta-analysis was performed using an inverse variance-weighted, random-effects model with standardized mean difference (SMD) as the effect size estimate.
Results
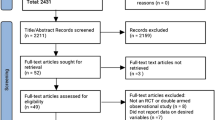
Meta-analysis of data from the ten eligible randomized controlled trials (RCTs), with 670 subjects, suggested a significant increase in FMD following allopurinol treatment (weighted mean difference [WMD] 1.79%, 95% confidence interval [CI] 1.01–2.56, p < 0.001; I 2: 86.77%). The effect size was robust and remained significant after omission of each single study. Subgroup analyses of RCTs based on the administered dose or duration of treatment did not reveal any significant impact of these variables on FMD change. Nor was a significant association found between allopurinol-induced changes in SUA levels and FMD (slope 0.46, p = 0.253), whereas baseline FMD significantly influenced the degree of FMD improvement following allopurinol treatment (slope 0.52, p = 0.022). Nitroglycerin-mediated dilation was not altered by allopurinol treatment (WMD 0.88%, 95% CI − 1.15–2.91, p = 0.395; I 2: 80.88%).
Conclusion
This meta-analysis of available RCTs suggests a significant benefit from allopurinol intake in increasing FMD in humans, independent of its effect on SUA levels.







Similar content being viewed by others
References
Hyndman D, Liu S, Miner JN. Urate handling in the human body. Curr Rheumatol Rep. 2016;18(6):34.
Maiuolo J, Oppedisano F, Gratteri S, Muscoli C, Mollace V. Regulation of uric acid metabolism and excretion. Int J Cardiol. 2016;213:8–14.
Katsiki N, Karagiannis A, Athyros VG, Mikhailidis DP. Hyperuricaemia: more than just a cause of gout? J Cardiovasc Med. 2013;14:397–402.
Feig DI, Kang DH, Johnson RJ. Uric acid and cardiovascular risk. N Engl J Med. 2008;359:1811–21.
Borghi C. Uric acid as a cross-over between rheumatology and cardiovascular disease. Curr Med Res Opin. 2013;29(Suppl 3):1–2.
Shi Y, Evans JE, Rock KL. Molecular identification of a danger signal that alerts the immune system to dying cells. Nature. 2003;425:516–21.
Netea MG, Kullberg BJ, Blok WL, Netea RT, van der Meer JW. The role of hyperuricemia in the increased cytokine production after lipopolysaccharide challenge in neutropenic mice. Blood. 1997;89:577–82.
Erdogan D, Gullu H, Caliskan M, Yildirim E, Bilgi M, Yildirim E, et al. Relationship of serum uric acid to measures of endothelial function and atherosclerosis in healthy adults. Int J Clin Pract. 2005;59:1276–82.
Cicero AF, Salvi P, D’Addato S, Rosticci M. Borghi C for the Brisighella Heart Study group. Association between serum uric acid, hypertension, vascular stiffness and subclinical atherosclerosis: data from the Brisighella Heart Study. J Hypertens. 2014;32:57–64.
Borghi C, Cicero AFG. Serum uric acid and cardiometabolic disease: another brick in the wall? Hypertension. 2017;69(6):1011–3.
Borghi C, Cicero AF. Cardiometabolic risks and obesity in the young. N Engl J Med. 2016;374(6):591–2.
Wang Y, Hu JW, Lv YB, Chu C, Wang KK, Zheng WL, Cao YM, et al. The role of uric acid in hypertension of adolescents, prehypertension and salt sensitivity of blood pressure. Med Sci Monit. 2017;23:790–5.
Kivity S, Kopel E, Maor E, Abu-Bachar F, Segev S, Abu-Bachar F, Segev S, Sidi Y, Olchovsky D. Association of serum uric acid and cardiovascular disease in healthy adults. Am J Cardiol. 2013;111:1146–51.
Vlachopoulos C, Xaplanteris P, Aboyans V, Brodmann M, Cífková R, Cosentino F, De Carlo M, et al. The role of vascular biomarkers for primary and secondary prevention. A position paper from the European Society of Cardiology Working Group on peripheral circulation: endorsed by the Association for Research into Arterial Structure and Physiology (ARTERY) Society. Atherosclerosis. 2015;241(2):507–32.
Flammer AJ, Anderson T, Celermajer DS, Creager MA, Deanfield J, Ganz P, Hamburg NM, et al. The assessment of endothelial function: from research into clinical practice. Circulation. 2012;126(6):753–67.
Moher D, Liberati A, Tetzlaff J. Altman DG; PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009;339:b2535.
Higgins JPT, Green S. Handbook for systematic reviews of interventions. Version 5.0.2 ed. London: The Cochrane Collaboration; 2009
Borenstein M, Higgins JP. Comprehensive Meta-analysis and subgroups. Prev Sci. 2013;14(2):134–43.
Sutton AJ, Abrams KR, Jones DR, Sheldon TA, Song F. Methods for meta-analysis in medical research. Chichester: Wiley; 2000.
Bucher HC, Guyatt GH, Griffith LE, Walter SD. The results of direct and indirect treatment comparisons in meta-analysis of randomized controlled trials. J Clin Epidemiol. 1997;50(6):683–91.
Duval STR. Trim and fill: a simple funnel-plot-based method of testing and adjusting for publication bias in meta-analysis. Biometrics. 2000;56(2):455–63.
El Solh AA, Saliba R, Bosinski T, Grant BJ, Berbary E, Miller N. Allopurinol improves endothelial function in sleep apnoea: a randomised controlled study. Eur Respir J. 2006;27(5):997–1002.
Yiginer O, Ozcelik F, Inanc T, Aparci M, Ozmen N, Cingozbay BY, Kardesoglu E, Suleymanoglu S, Sener G, Cebeci BS. Allopurinol improves endothelial function and reduces oxidant-inflammatory enzyme of myeloperoxidase in metabolic syndrome. Clin Res Cardiol. 2008;97(5):334–40.
Kao MP, Ang DS, Gandy SJ, Nadir MA, Houston JG, Lang CC, Struthers AD. Allopurinol benefits left ventricular mass and endothelial dysfunction in chronic kidney disease. J Am Soc Nephrol. 2011;22(7):1382–9.
Jalal DI, Decker E, Perrenoud L, Nowak KL, Bispham N, Mehta T, Smits G, You Z, Seals D, Chonchol M, Johnson RJ. Vascular function and uric acid-lowering in stage 3 CKD. J Am Soc Nephrol. 2017;28(3):943–52.
Dogan A, Yarlioglues M, Kaya MG, Karadag Z, Dogan S, Ardic I, Dogdu O, Kilinc Y, Zencir C, Akpek M, Ozdogru I, Oguzhan A, Kalay N. Effect of long-term and high-dose allopurinol therapy on endothelial function in normotensive diabetic patients. Blood Press. 2011;20(3):182–7.
Szwejkowski BR, Gandy SJ, Rekhraj S, Houston JG, Lang CC, Morris AD, George J, Struthers AD. Allopurinol reduces left ventricular mass in patients with type 2 diabetes and left ventricular hypertrophy. J Am Coll Cardiol. 2013;62(24):2284–93.
Rajendra NS, Ireland S, George J, Belch JJ, Lang CC, Struthers AD. Mechanistic insights into the therapeutic use of high-dose allopurinol in angina pectoris. J Am Coll Cardiol. 2011;58(8):820–8.
Rekhraj S, Gandy SJ, Szwejkowski BR, Nadir MA, Noman A, Houston JG, Lang CC, George J, Struthers AD. High-dose allopurinol reduces left ventricular mass in patients with ischemic heart disease. J Am Coll Cardiol. 2013;61(9):926–32.
Tousoulis D, Andreou I, Tsiatas M, Miliou A, Tentolouris C, Siasos G, Papageorgiou N, Papadimitriou CA, Dimopoulos MA, Stefanadis C. Effects of rosuvastatin and allopurinol on circulating endothelial progenitor cells in patients with congestive heart failure: the impact of inflammatory process and oxidative stress. Atherosclerosis. 2011;214(1):151–7.
Robertson AJ, Struthers AD. A randomized controlled trial of allopurinol in patients with peripheral arterial disease. Can J Cardiol. 2016;32(2):190–6.
Wang Y, Bao X. Effects of uric acid on endothelial dysfunction in early chronic kidney disease and its mechanisms. Eur J Med Res. 2013;18:26.
Kanbay M, Segal M, Afsar B, Kang DH, Rodriguez-Iturbe B, Johnson RJ. The role of uric acid in the pathogenesis of human cardiovascular disease. Heart. 2013;99:759–66.
Kang DH, Park SK, Lee IK, Johnson RJ. Uric acid-induced C-reactive protein expression: implication on cell proliferation and nitric oxide production of human vascular cells. J Am Soc Nephrol. 2005;16:3553–62.
Yu MA, Sánchez-Lozada LG, Johnson RJ, Kang DH. Oxidative stress with an activation of the renin-angiotensin system in human vascular endothelial cells as a novel mechanism of uric acid-induced endothelial dysfunction. J Hypertens. 2010;28:1234–42.
Choi HY, Kim SH, Choi AR, Kim SG, Kim H, Lee JE, Kim HJ, Park HC. Hyperuricemia and risk of increased arterial stiffness in healthy women based on health screening in Korean population. PLoS One. 2017;12(6):e0180406.
Cicero AF, Rosticci M, Bove M, Fogacci F, Giovannini M, Urso R, D’Addato S. Borghi C; Brisighella Heart Study Group. Serum uric acid change and modification of blood pressure and fasting plasma glucose in an overall healthy population sample: data from the Brisighella heart study. Ann Med. 2017;49(4):275–82.
Riesterer L, Jaques R. The anti-inflammatory action of a xanthine oxidase inhibitor (allopurinol). Pharmacology. 1969;2(5):288–94.
Muir SW, Harrow C, Dawson J, Lees KR, Weir CJ, Sattar N, Walters MR. Allopurinol use yields potentially beneficial effects on inflammatory indices in those with recent ischemic stroke: a randomized, double-blind, placebo-controlled trial. Stroke. 2008;39(12):3303–7.
Daskalopoulou SS, Tzovaras V, Mikhailidis DP, Elisaf M. Effect on serum uric acid levels of drugs prescribed for indications other than treating hyperuricaemia. Curr Pharm Des. 2005;11(32):4161–75.
Matsuzawa Y, Kwon TG, Lennon RJ, Lerman LO, Lerman A. Prognostic value of flow-mediated vasodilation in brachial artery and fingertip artery for cardiovascular events: a systematic review and meta-analysis. J Am Heart Assoc. 2015;4(11):e002270.
Singh JA, Cleveland J. Allopurinol and the risk of ventricular arrhythmias in the elderly: a study using US Medicare data. BMC Med. 2017;15(1):59.
MacIsaac RL, Salatzki J, Higgins P, Walters MR, Padmanabhan S, Dominiczak AF, Touyz RM, Dawson J. Allopurinol and cardiovascular outcomes in adults with hypertension. Hypertension. 2016;67(3):535–40.
de Abajo FJ, Gil MJ, Rodríguez A, García-Poza P, Álvarez A, Bryant V, García-Rodríguez LA. Allopurinol use and risk of non-fatal acute myocardial infarction. Heart. 2015;101(9):679–85.
Grimaldi-Bensouda L, Alpérovitch A, Aubrun E, Danchin N, Rossignol M, Abenhaim L, Richette P, PGRx MI Group. Impact of allopurinol on risk of myocardial infarction. Ann Rheum Dis. 2015;74(5):836–42.
Bove M, Cicero AF, Veronesi M, Borghi C. An evidence-based review on urate-lowering treatments: implications for optimal treatment of chronic hyperuricemia. Vasc Health Risk Manag. 2017;13:23–8.
Tsuruta Y, Kikuchi K, Tsuruta Y, Sasaki Y, Moriyama T, Itabashi M, Takei T, et al. Febuxostat improves endothelial function in hemodialysis patients with hyperuricemia: a randomized controlled study. Hemodial Int. 2015;19(4):514–20.
Lytvyn Y, Har R, Locke A, Lai V, Fong D, Advani A, Perkins BA, Cherney DZI. Renal and vascular effects of uric acid lowering in normouricemic patients with uncomplicated type 1 diabetes. Diabetes. 2017;66(7):1939–49.
Zhang L, Gong D, Li S, Zhou X. Meta-analysis of the effects of statin therapy on endothelial function in patients with diabetes mellitus. Atherosclerosis. 2012;223(1):78–85.
Masoura C, Pitsavos C, Aznaouridis K, Skoumas I, Vlachopoulos C, Stefanadis C. Arterial endothelial function and wall thickness in familial hypercholesterolemia and familial combined hyperlipidemia and the effect of statins. A systematic review and meta-analysis. Atherosclerosis. 2011;214(1):129–38.
Author information
Authors and Affiliations
Contributions
AFGC, MP, MB and AS conceived and designed the work and contributed to the drafting of the manuscript. Arrigo F.G. Cicero and Matteo Pirro performed the searches and extracted data. Amirhossein Sahebkar performed the statistical analysis. GFWa, DPM and MB contributed to the interpretation of the work and revised the manuscript critically for important intellectual content. All authors approved the final manuscript and agree to be held accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflicts of interest
Prof. Watts has received honoraria for advisory boards and lectures from Amgen, Sanofi, Regeneron, Kowa and MSD. Prof. Banach has served on the speaker’s bureau and as an advisory board member for Amgen, Sanofi, Aventis and Lilly. Prof. Mikhailidis has given talks and attended conferences sponsored by MSD, Libytec and AstraZeneca. No professional writer was involved in the preparation of this meta-analysis.
Funding
This meta-analysis was written independently; no company or institution supported it financially.
Rights and permissions
About this article
Cite this article
Cicero, A.F.G., Pirro, M., Watts, G.F. et al. Effects of Allopurinol on Endothelial Function: A Systematic Review and Meta-Analysis of Randomized Placebo-Controlled Trials. Drugs 78, 99–109 (2018). https://doi.org/10.1007/s40265-017-0839-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40265-017-0839-5