Abstract
Purpose
This study was planned to collect evidences of familial pertussis transmission to infants younger than 6 months of age. Understanding the dynamics of transmission of pertussis in families is essential to plan effective prevention strategies that could be integrated in pertussis control.
Methods
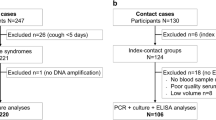
The seroprevalence of IgG antibodies to pertussis toxin (PT-IgG) and prolonged cough symptoms were evaluated in parents of 55 infants aged <6 months hospitalized for confirmed pertussis. Parents of 33 infants with lower respiratory tract infection (LRTI) and parents of 57 healthy infants admitted as outpatients for hip ultrasound examination (HE) were enrolled as controls.
Results
Parents of pertussis cases had PT-IgG levels significantly higher as compared to LRTI and HE parents. More than 40 % were compatible as transmitters of pertussis to their babies, since they had a level of PT-IgG ≥ 100 IU/ml, which is considered diagnostic for a recent pertussis episode. Based on serology, the percentage of pertussis cases that had at least one parent as source of infection was 49.1 %. When cough symptoms were taken into account, the percentage of parents putative transmitters of the infection to their infants increased to 56.4 %.
Conclusions
Parents are scarcely aware of the household transmission of pertussis to their newborns. Our study highlights the need to advise parents about the likelihood of transmission to the newborn and to be particularly aware of coughing symptoms in the household. Since infection can be asymptomatic, a serological survey of family members should also be considered.




Similar content being viewed by others
References
EUVAC-NET, Pertussis surveillance annual report 2009. http://www.euvac.net/graphics/euvac/pdf/pertussis_2009.pdf. Accessed 23 June 2016.
Zepp F, Heininger U, Mertsola J, Bernatowska E, Guiso N, Roord J, et al. Rationale for pertussis booster vaccination throughout life in Europe. Lancet Infect Dis. 2011;11:557–70.
Fedele G, Cassone A, Ausiello CM. T-cell immune responses to Bordetella pertussis infection and vaccination. Pathog Dis. 2015;7 (pii:ftv051).
Ausiello CM, Cassone A. Acellular pertussis vaccines and pertussis resurgence: revise or replace? MBio. 2014;10(5):e01339–14.
Locht C. Pertussis: where did we go wrong and what can we do about it? J Infect. 2016 (pii: S0163-4453(16)30047-0).
Mattoo S, Cherry JD. Molecular pathogenesis, epidemiology, and clinical manifestations of respiratory infections due to Bordetella pertussis and other Bordetella subspecies. Clin Microbiol Rev. 2005;18:326–82.
Melvin JA, Scheller EV, Miller JF, Cotter PA. Bordetella pertussis pathogenesis: current and future challenges. Nat Rev Microbiol. 2014;12:274–88.
Yaari E, Yafe-Zimerman Y, Schwartz SB, Slater PE, Shvartzman P, Andoren N, et al. Clinical manifestations of Bordetella pertussis infection in immunized children and young adults. Chest. 1999;115:1254–8.
Tozzi AE, Celentano LP, Ciofi degli Atti ML, Salmaso S. Diagnosis and management of pertussis. CMAJ. 2005;15(172):509–15.
Gonfiantini MV, Carloni E, Gesualdo F, Pandolfi E, Agricola E, Rizzuto E, et al. Epidemiology of pertussis in Italy: disease trends over the last century. Euro Surveill. 2014;19:20921.
Nelson JD. The changing epidemiology of pertussis in young infants. The role of adults as reservoirs of infection. Am J Dis Child. 1978;132:371–3.
Wendelboe AM, Van Rie A, Salmaso S, Englund JA. Duration of immunity against pertussis after natural infection or vaccination. Pediatr Infect Dis J. 2005;24:S58–61.
Althouse BM, Scarpino SV. Asymptomatic transmission and the resurgence of Bordetella pertussis. BMC Med. 2015;13:146.
de Greeff SC, Mooi FR, Westerhof A, Verbakel JM, Peeters MF, Heuvelman CJ, et al. Pertussis disease burden in the household: how to protect young infants. Clin Infect Dis. 2010;50:1339–45.
Wendelboe AM, Hudgens MG, Poole C, Van Rie A. Estimating the role of casual contact from the community in transmission of Bordetella pertussis to young infants. Emerg Themes Epidemiol. 2007;4:15.
Wiley KE, Zuo Y, Macartney KK, McIntyre PB. Sources of pertussis infection in young infants: a review of key evidence informing targeting of the cocoon strategy. Vaccine. 2013;31:618–25.
Giammanco A, Chiarini A, Maple PA, Andrews N, Pebody R, Gay N, et al. European Sero-Epidemiology Network: standardisation of the assay results for pertussis. Vaccine. 2003;22:112–20.
Hallander HO, Andersson M, Gustafsson L, Ljungman M, Netterlid E. Seroprevalence of pertussis antitoxin (anti-PT) in Sweden before and 10 years after the introduction of a universal childhood pertussis vaccination program. APMIS. 2009;117:912–22.
Palazzo R, Carollo M, Fedele G, Rizzo C, Rota MC, Giammanco A, et al. Evidence of increased circulation of Bordetella pertussis in the Italian adult population from seroprevalence data (2012-2013). J Med Microbiol. 2016 (Epub ahead of print ).
Xing D, Wirsing von König CH, Newland P, Riffelmann M, Meade BD, Corbel M, et al. Characterization of reference materials for human antiserum to pertussis antigens by an international collaborative study. Clin Vaccine Immunol. 2009;16:303–11.
Hallander HO, Ljungman M, Storsaeter J, Gustafsson L. Kinetics and sensitivity of ELISA IgG pertussis antitoxin after infection and vaccination with Bordetella pertussis in young children. APMIS. 2009;117:797–807.
Guiso N, Berbers G, Fry NK, He Q, Riffelmann M, Wirsing von König CH, EU Pertstrain group. What to do and what not to do in serological diagnosis of pertussis: recommendations from EU reference laboratories. Eur J Clin Microbiol Infect Dis. 2011;30:307–12.
ECDC, 2012 Guidance and protocol for the serological diagnosis of human infection with Bordetella pertussis. http://ecdc.europa.eu/en/publications/Publications/bordetella-pertussis-guidance-protocol-serological-diagnosis.pdf. Accessed 23 June 2016.
Italian Ministry of Health http://www.salute.gov.it/portale/documentazione/p6_2_8_3_1.jsp?lingua=italiano&id=20. Accessed 5 Aug 2016.
The Italian Vaccine Coverage Survey Working Group. Childhood vaccination coverage in Italy: results of a seven-region survey. Bull World Health Org. 1994;72:885–95.
Bisgard KM, Pascual FB, Ehresmann KR, Miller CA, Cianfrini C, Jennings CE, et al. Infant pertussis: who was the source? Pediatr Infect Dis J. 2004;23:985–9.
Elliott E, McIntyre P, Ridley G, Morris A, Massie J, McEniery J, et al. National study of infants hospitalized with pertussis in the acellular vaccine era. Pediatr Infect Dis J. 2004;23:246–52.
Long SS, Welkon CJ, Clark JL. Widespread silent transmission of pertussis in families: antibody correlates of infection and symptomatology. J Infect Dis. 1990;161:480–6.
Ward JI, Cherry JD, Chang SJ, Partridge S, Keitel W, Edwards K, et al. Bordetella Pertussis infections in vaccinated and unvaccinated adolescents and adults, as assessed in a national prospective randomized Acellular Pertussis Vaccine Trial (APERT). Clin Infect Dis. 2006;43:151–7.
Crowcroft NS, Booy R, Harrison T, Spicer L, Britto J, Mok Q, et al. Severe and unrecognised: pertussis in UK infants. Arch Dis Child. 2003;88:802–6 erratum in: Arch Dis Child. 2006;91:453.
Warfel JM, Zimmerman LI, Merkel TJ. Acellular pertussis vaccines protect against disease but fail to prevent infection and transmission in a nonhuman primate model. Proc Natl Acad Sci USA. 2014;111:787–92.
Storsaeter J, Hallander H, Farrington CP, Olin P, Möllby R, Miller E. Secondary analyses of the efficacy of two acellular pertussis vaccines evaluated in a Swedish phase III trial. Vaccine. 1990;8:457–61.
Von Linstow ML, Pontoppidan PL, König C-HW, Cherry JD, Hogh B. Evidence of Bordetella pertussis infection in vaccinated 1-year-old Danish children. Eur J Pediatr. 2010;169:1119–22.
Dabrera G, Amirthalingam G, Andrews N, Campbell H, Ribeiro S, Kara E, et al. A case-control study to estimate the effectiveness of maternal pertussis vaccination in protecting newborn infants in England and Wales, 2012–2013. Clin Infect Dis. 2015;60:333–7.
van den Biggelaar AH, Poolman JT. Predicting future trends in the burden of pertussis in the 21st century: implications for infant pertussis and the success of maternal immunization. Expert Rev Vaccines. 2016;15:69–80.
Acknowledgments
This work was supported by Grants from the Italian Ministry of Health, RF-2010-2317709.
The Pertussis Study Group Pasqualina Leone, Ilaria Schiavoni, Gabriele Buttinelli (Department of Infectious, Parasitic and Immuno-mediated Disease, Istituto Superiore di Sanità, Rome, Italy); Michaela Veronika Gonfiantini, Eleonora Agricola, Luisa Russo, Beatrice Ferretti, Ilaria Campagna (Multifactorial Disease and Complex Phenotype Research Area, Bambino Gesù Children’s Hospital, Rome, Italy); Valentina Marcellini (Immunology Area, B-cell physiopathology Unit, Bambino Gesù Children Hospital, Rome, Italy); Carlo Concato (Virology Unit, Bambino Gesù Children’s Hospital, Rome, Italy); Antonella Frassanito, Raffaella Nenna, Greta Di Mattia (Department of Pediatrics, Sapienza University of Rome, Rome, Italy); Caterina Rizzo (National Centre for Epidemiology Surveillance and Health Promotion, Istituto Superiore di Sanità, Rome, Italy).
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Fedele, G., Carollo, M., Palazzo, R. et al. Parents as source of pertussis transmission in hospitalized young infants. Infection 45, 171–178 (2017). https://doi.org/10.1007/s15010-016-0943-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s15010-016-0943-6